LemierreГўВ?В?s Syndrome in an Adult: A Case Review
Published Date: 05-Apr-2014 DOI: 10.4172/2161-119X.1000167
Abstract
Lemierre’s syndrome (postanginal septicaemia/human necrobacillosis) was first defined and described in 1936 by Lemierre, a French Physician and Professor in Microbiology, although the first case report of human necrobacillosis was published in 1900 by Courmont and Cade [1,2]. Lemierre’s syndrome has come to be known as the “forgotten” disease, as very few cases have been reported since the introduction and widespread use of antibiotics [3,4]. In the preantibiotic era, Lemierre’s Syndrome was associated with a mortality rate of approximately 90% [1]. Currently, the associated mortality rate is estimated to range from 5% to 10% [5-7]. Since 1974, less than 100 cases have been reported [8,9]. This can be explained by the fact that more throat infections received early treatment with the widespread use of antibiotics, leading to the decrease in the incidence of Lemierre’s disease. The syndrome is characterised by a recent history of oropharyngitis with persistent fevers, followed by septic thrombophlebitis of the internal jugular vein and dissemination of the infection to multiple sites distant to the pharynx [10]. Fusobacterium species are responsible in most cases. It affects previously healthy adolescents and young adults.
Introduction
Lemierre’s syndrome (postanginal septicaemia/human necrobacillosis) was first defined and described in 1936 by Lemierre, a French Physician and Professor in Microbiology, although the first case report of human necrobacillosis was published in 1900 by Courmont and Cade [1,2]. Lemierre’s syndrome has come to be known as the “forgotten” disease, as very few cases have been reported since the introduction and widespread use of antibiotics [3,4]. In the preantibiotic era, Lemierre’s Syndrome was associated with a mortality rate of approximately 90% [1]. Currently, the associated mortality rate is estimated to range from 5% to 10% [5-7]. Since 1974, less than 100 cases have been reported [8,9]. This can be explained by the fact that more throat infections received early treatment with the widespread use of antibiotics, leading to the decrease in the incidence of Lemierre’s disease. The syndrome is characterised by a recent history of oropharyngitis with persistent fevers, followed by septic thrombophlebitis of the internal jugular vein and dissemination of the infection to multiple sites distant to the pharynx [10]. Fusobacterium species are responsible in most cases. It affects previously healthy adolescents and young adults.
Case Report
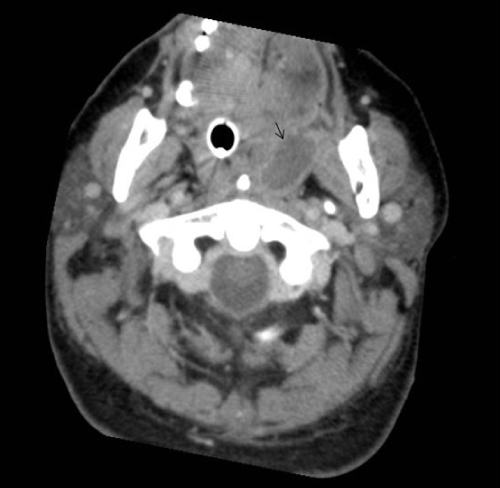
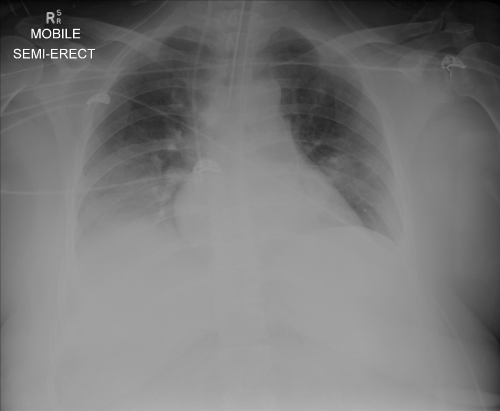
A previously healthy 44 year old female was seen in the Emergency Department with a 3 day history of progressively worsening sore throat predominantly to the left with associated fevers and vomiting. She deteriorated rapidly over the last 24 hours before presenting to the hospital, with significant odynophagia, vomiting and dehydration. On examination, she was febrile (39.8°C), hypotensive (92/50 mm of Hg) and tachycardic (142 beats per minute). Throat examination revealed an erythematous left tonsil pushed medially. On examination of the neck, there was associated tender cervical lymphadenopathy. Lung fields were clear on auscultation. Abdominal examination did not reveal any organomegaly or tenderness. Investigations at the time of admission showed White Cell Count (WCC) 29.0×109 L with a platelet count of 37/mm3, International Normalised Ratio (INR) of 2.2, C-Reactive Protein (CRP) of 211 along with deranged liver and kidney function tests. Initial chest radiography revealed normal lung fields. She required acute resuscitation and intensive care admission. She underwent a Computerised Tomography (CT) of the neck with contrast which revealed a collection in the left peritonsillar region (Figure 1). Drainage of the peritonsilllar abscess was deferred due to coagulopathy. She rapidly deteriorated despite intravenous antibiotics and developed coagulopathy, acute renal failure, encephalopathy, respiratory failure and bilateral pleural effusions (Figure 2). She required inotropic support, mechanical ventilation and dialysis. Intravenous antibiotic therapy included Lincomycin and Meropenem with blood cultures pending. Blood cultures grew Fusobacterium necrophorum (subspecies not identified), sensitive to Penicillin and Metronidazole. Antibiotics were changed accordingly to Piperacillin-Tazobactam and Metronidazole. A diagnosis of Lemierre’s syndrome was made. The left peritonsillar abscess was drained on the sixth day of admission after the reversal of coagulopathy with fresh frozen plasma. An improvement in her condition was noted and she was successfully extubated on the ninth day after admission. She was discharged home on thirteenth day on a week’s course of Amoxycillin-Clavulanic acid. She has remained asymptomatic and well since discharge. She was followed up in Ear, Nose and Throat (ENT) outpatient clinics 2 months later but did not require any further treatment.
Discussion
Fusobacterium necrophorum is a gram-negative anaerobe responsible for Lemierre`s syndrome in 90% cases and has been detected in 10% of all acute sore throats and 21% of all recurring sore throats with the remainder caused by group A streptococci or viruses [11,12]. F. necrophorum is conventionally thought to be a part of the normal flora of the pharynx, gastrointestinal tract, and female genital tract but there is no convincing evidence of the same [12]. It can invade as a primary pathogen due to its ability to produce lipopolysaccharide endotoxin, leukocidin, and haemolysin [13]. It has been shown to release bradykinin and activate the intrinsic pathway of coagulation by activating the contact system through direct binding of high molecular weight kininogen and factor XI, respectively [14]. Bacteroides, Streptococcus, Peptostreptococcus and Eikenella are other organisms that have been isolated from the patients with Lemierre’s syndrome [10,15]. Palatine tonsils and peritonsillar tissue are the prime sources of infection. The infection may spread to involve the parapharyngeal space leading to secondary thrombophlebitis of the tonsillar veins, which can propagate thrombus formation to the internal jugular vein [6,9,16].
The patients present with a history of a recent sore throat within the last week with high grade temperatures ranging between 39-41 degrees often followed by a rigor [1,17,18]. At the time of presentation, the throat may vary from a normal looking oropharynx to a severe exudative tonsillitis or peritonsillitis [9,12,19]. Neck pain, stiffness and cervical lymphadenopathy are often present due to the development of thrombus in the Internal Jugular Vein (IJV). Sometimes, this may have concomitant trismus, otalgia and dysphagia [20]. Local septic complications include peritonsillar abscess, internal jugular vein thrombosis, parapharyngeal abscess and paratracheal abscess [21,22].
Evidence of internal jugular vein thrombosis is radiologically evident either by ultrasonography or CT, in approximately 30-70% of the patients [6,13]. The thrombus releases septic emboli leading to metastatic infections. The most commonly involved organs are the lungs. There may be associated pleural effusion, empyema, bilateral pulmonary infiltrates or multiple cavitating lesions [23-26]. A rather rapid progression of lung lesions and pleural effusion is noted in these patients despite antibiotic therapy. Pneumatocoeles, pneumothorax and adult respiratory distress syndrome are uncommon complications [26-29]. Bearing in mind the aggressive nature of disease progression and severity of septicaemic illness, acute respiratory distress syndrome is noted in only a very small subset of those diagnosed, with less than 10% requiring mechanical ventilation [30]. Septic arthritis, osteomyelitis, pericarditis, hepatic abscesses are other metastatic manifestations. The spleen, skin, kidneys, brain and soft tissue may rarely be involved [24,31,32]. There may be associated splenomegaly, hepatomegaly and jaundice. Liver function tests are deranged in 49% of the patients with hyperbilirubinaemia [33]. Blood picture reveals leucocytosis in most cases with thrombocytopenia in some. Renal involvement may result in renal insufficiency with haematuria, pyuria, proteinuria and uraemia [5,34-36]. Activation of the intrinsic pathway of coagulation can lead to coagulopathy and disseminated intravascular coagulation [14].
A high degree of suspicion is required to aid in the diagnosis. The diagnosis is usually not reached until the blood culture results are available which may take at least 48 hours and sometimes up to 7 days. Radiological studies especially contrast enhanced CT can confirm clinical suspicions. The images reveal distended veins with enhancement of the vessel walls, intramural filling defects and adjacent soft tissue swelling [37]. Local complications like peritonsillar abscess are also visualised on CT. Doppler ultrasound, Magnetic Resonance Angiography (MRA), gallium scan and radionuclide venography may sometimes be required. CT and plain chest radiographs are used to look for lung involvement. An ultrasound examination of the abdomen may be undertaken when hepatic or splenic abscesses are suspected [37-41].
Intravenous antibiotics are the mainstay of treatment. Slow improvement in the clinical picture despite appropriate antibiotics therapy may be noted. Majority of the patients treated with antibiotics in a timely manner show a favourable outcome. Poorer outcomes are seen with delayed treatment. Fusobacterium necrophorum is found to be sensitive to beta-lactam antibiotics, metronidazole, clindamycin and third generation cephalosporins [13,34,42]. Due to a high probability of a co-infection by another bacterium, monotherapy is not advised for the treatment of Lemierre’s syndrome. Patients should be treated with penicillin combined with a beta-lactamase inhibitor such as clavulanic acid or with metronidazole for a total of 6 weeks [5,6,15,43]. Clindamycin can be given as a single agent. Surgical excision and ligation of the IJV is rarely required and reserved for patients with ongoing sepsis and septic embolization resulting in repetitive embolic manifestations [6,9,15,44].
The role of anticoagulation in the treatment of Lemierre’s syndrome remains controversial. Heparin use in these patients may shorten the course of the disease and the need of surgical intervention [45]. Patients may be anticoagulated for possible early clot dissolution but should be easily reversible if the need for surgical intervention arises. It needs to be kept in mind that these patients are usually coagulopathic and hence the presence of thrombophilia should be used as a guide to the need of anticoagulation. Sigmoid sinus thrombosis is an indication that warrants anticoagulation [19,25,46,47]. The recommended anticoagulation regime, if indicated should include one week of intravenous heparin followed by 3 months of oral warfarin [19,47]. Hyperbaric oxygen has also been used with some evidence to support a favourable and rapid improvement in patients’ condition [48].
Conclusion
Pharyngitis with associated clinical picture of IJV thrombophlebitis, sepsis or septic emboli should raise the possibility of Lemierre’s syndrome in the treating clinician’s mind leading to appropriate treatment and investigations. Early recognition of the syndrome is vital for prompt and appropriate therapy as blood cultures may take several days. Bearing in mind, the clinical suspicion of Lemierre’s syndrome, patients presenting with pharyngitis and associated high grade fevers, should undergo a careful and thorough examination of the neck and blood cultures as part of the initial workup. Mortality and morbidity is low if diagnosed and treated early.
References
- Lemierre A (1936) On certain septicaemias due to anaerobic organisms. Lancet 1:701ГўвӮ¬вҖң703.
- Courmont P, Cade A (1900) Sur une septico-pyohemie de lГўвӮ¬в„ўhomme simulant la peste et causeГӮВҙe parun streptobacille anaerobie. Arch Med Exp Anat Pathol 12:393ГўвӮ¬вҖң418.
- Shah SA, Ghani R (2005) Lemierre's syndrome: a forgotten complication of oropharyngeal infection. J Ayub Med Coll Abbottabad 17: 30-33.
- Koay CB, Heyworth T, Burden P (1995) Lemierre syndrome--a forgotten complication of acute tonsillitis. J Laryngol Otol 109: 657-661.
- Chirinos JA, Lichtstein DM, Garcia J, Tamariz LJ (2002) The evolution of Lemierre syndrome: report of 2 cases and review of the literature. Medicine (Baltimore) 81: 458-465.
- Ianniello F, Ferri E, Pinzani A (1998) [Septic thrombophlebitis of the internal jugular vein due to Fusobacterium necrophorum (Lemierre's syndrome): case report and review of literature]. Acta Otorhinolaryngol Ital 18: 332-337.
- Sherer Y, Mishal J (2003) The changing face of Lemierre's syndrome. Isr Med Assoc J 5: 819-820.
- Singhal A, Kerstein MD (2001) Lemierre's syndrome. South Med J 94: 886-887.
- Subirana Pozo FX1, Serra Carreras J, Lorente Guerrero J, Crego de Pablos F, GarcГғВӯa LГғВіpez M, et al. (2001) [Lemiere's syndrome. Thrombophlebitis of the internal jugular vein induced by oropharyngeal lesion. A case report]. An Otorrinolaringol Ibero Am 28: 419-430.
- Sinave CP, Hardy GJ, Fardy PW (1989) The Lemierre syndrome: suppurative thrombophlebitis of the internal jugular vein secondary to oropharyngeal infection. Medicine (Baltimore) 68: 85-94.
- Aliyu SH, Marriott RK, Curran MD, Parmar S, Bentley N, et al. (2004) Real-time PCR investigation into the importance of Fusobacterium necrophorum as a cause of acute pharyngitis in general practice. J Med Microbiol 53: 1029-1035.
- Batty A, Wren MW, Gal M (2005) Fusobacterium necrophorum as the cause of recurrent sore throat: comparison of isolates from persistent sore throat syndrome and Lemierre's disease. J Infect 51: 299-306.
- Riordan T (2007) Human infection with Fusobacterium necrophorum (Necrobacillosis), with a focus on Lemierre's syndrome. Clin Microbiol Rev 20: 622-659.
- Holm K, Frick IM, BjГғВ¶rck L, Rasmussen M (2011) Activation of the contact system at the surface of Fusobacterium necrophorum represents a possible virulence mechanism in LemiГғВЁrre's syndrome. Infect Immun 79: 3284-3290.
- Puymirat E, Biais M, Camou F, LefГғВЁvre J, Guisset O, et al. (2008) A Lemierre syndrome variant caused by Staphylococcus aureus. Am J Emerg Med 26: 380.
- Benhayoun M, Llor J, Van-Den-Abbeele T, Elmaleh M, Mariani P, et al. (2003) [Bilateral jugular thrombosis in Lemierre syndrome]. Arch Pediatr 10: 1071-1074.
- de Lima JE Jr, Levin M (2003) Lemierre's syndrome: post-anginal septicemia. Pediatr Radiol 33: 281-283.
- Lacaze O, Bocquel V, Fournel P, Emonot A (2000) [Lemierre syndrome: clinical and radiological characteristics of a rare disease]. Rev Mal Respir 17: 1105-1106.
- Nakamura S, Sadoshima S, Doi Y, Yoshioka M, Yamashita S, et al. (2000) Internal jugular vein thrombosis, Lemierre's syndrome; oropharyngeal infection with antibiotic and anticoagulation therapy--a case report. Angiology 51: 173-177.
- Clarke MG, Kennedy NJ, Kennedy K (2003) Serious consequences of a sore throat. Ann R Coll Surg Engl 85: 242-244.
- Cosgrove EF, Colodny SM, Pesce RR (1993) Adult respiratory distress syndrome as a complication of postanginal sepsis. Chest 103: 1628-1629.
- MГғВёller K, Dreijer B (1997) Post-anginal sepsis (Lemierre's disease): a persistent challenge. Presentation of 4 cases. Scand J Infect Dis 29: 191-194.
- Gormus N, Durgut K, Ozergin U, Odev K, Solak H (2004) Lemierre's syndrome associated with septic pulmonary embolism: a case report. Ann Vasc Surg 18: 243-245.
- Riordon T, Wilson M (2003) Lemierre`s Syndrome: more than a historical curiosa: Postgradmed J: 328-334.
- Razonable RR, Rahman AE, Wilson WR (2003) Lemierre syndrome variant: necrobacillosis associated with inferior vena cava thrombosis and pulmonary abscesses after trauma-induced leg abscess. Mayo Clin Proc 78: 1153-1156.
- Cook RJ, Ashton RW, Aughenbaugh GL, Ryu JH (2005) Septic pulmonary embolism: presenting features and clinical course of 14 patients. Chest 128: 162-166.
- Smith SA (1999) Respiratory failure as a complication of pharyngitis: Lemierre's syndrome. Pediatr Emerg Care 15: 402-403.
- Schmid T, Miskin H, Schlesinger Y, Argaman Z, Kleid D (2005) Respiratory failure and hypercoagulability in a toddler with Lemierre's syndrome. Pediatrics 115: e620-622.
- Fiesseler FW, Richman PB, Riggs RL (2001) Pharyngitis followed by hypoxia and sepsis: Lemierre syndrome. Am J Emerg Med 19: 320-322.
- Sasaki Y, Iwata H, Kinoshita M, Sumiya M (2000) [Lemierre syndrome with extensive cervical venous thrombosis and multiple pulmonary embolisms]. Nihon Naika Gakkai Zasshi 89: 2174-2176.
- Bentham JR, Pollard AJ, Milford CA, Anslow P, Pike MG (2004) Cerebral infarct and meningitis secondary to Lemierre's syndrome. Pediatr Neurol 30: 281-283.
- Singaporewalla RM, Clarke MJ, Krishnan PU, Tan DE (2006). Is this a variant of Lemierre's syndrome? Singapore Med J. 47(12):1092ГўвӮ¬вҖң1095.
- Hagelskjaer LH, Prag J, Malczynski J, Kristensen JH (1998) Incidence and clinical epidemiology of necrobacillosis, including Lemierre's syndrome, in Denmark 1990-1995. Eur J Clin Microbiol Infect Dis 17: 561-565.
- Brazier JS (2006) Human infections with Fusobacterium necrophorum. Anaerobe 12: 165-172.
- Wilson P, Tierney L (2005) Lemierre syndrome caused by Streptococcus pyogenes. Clin Infect Dis 41: 1208-1209.
- Kuduvalli PM, Jukka CM, Stallwood M, Battersby C, Neal T, et al. (2005) Fusobacterium necrophorum-induced sepsis: an unusual case of Lemierre's syndrome. Acta Anaesthesiol Scand 49: 572-575.
- Lai YJ, Lirng JF, Chang FC, Luo CB, Teng MM, et al. (2004) Computed tomographic findings in Lemierre syndrome. J Chin Med Assoc 67: 419-421.
- Perrin MA, Jankowski A, Righini C, Boubagra K, Coulomb M, et al. (2007) [Imaging findings in Lemierre syndrome]. J Radiol 88: 65-68.
- Lai C, Vummidi DR (2004) Images in clinical medicine. Lemierre's Syndrome. N Engl J Med 350: e14.
- Auber AE, Mancuso PA (2000) Lemierre syndrome: magnetic resonance imaging and computed tomographic appearance. Mil Med 165: 638-640.
- Chiu O, Erbay SH, Bhadelia RA (2007) Lemierre's syndrome revisited: case report and imaging findings. Australas Radiol 51 Suppl: B196-198.
- Hagelskjaer Kristensen L, Prag J (2000) Human necrobacillosis, with emphasis on Lemierre's syndrome. Clin Infect Dis 31: 524-532.
- Syed MI, Baring D, Addidle M, Murray C, Adams C (2007). "Lemierre syndrome: two cases and a review". The Laryngoscope (The American Laryngological, Rhinological & Otological Society; Lippincott Williams & Wilkins 117: 1605ГўвӮ¬вҖң1610.
- Morris P, O'Sullivan E, Choo M, Barry C, Thompson CJ (2006) A rare cause of sepsis in an 18 year old. Lemierre's syndrome with external jugular vein thrombosis. Ir Med J 99: 24.
- Hoehn KS (2005) Lemierre's syndrome: the controversy of anticoagulation. Pediatrics 115: 1415-1416.
- Blaise S, Colombe B, Millet C, Poulain C, Bosseray A, et al. (2005) [Jugular thrombosis with fever: what about Lemierre syndrome?]. J Mal Vasc 30: 231-232.
- Repanos C, Chadha NK, Griffiths MV (2006) Sigmoid sinus thrombosis secondary to Lemierre's syndrome. Ear Nose Throat J 85: 98-101.
- Hodgson R, Emig M, Pisarello J (2003) Hyperbaric oxygen (HBO2) in the treatment of Lemierre syndrome. Undersea Hyperb Med 30: 87-91.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 15138
- [From(publication date): 5-2014 - Aug 30, 2025]
- Breakdown by view type
- HTML page views: 10452
- PDF downloads: 4686