Research Article Open Access
Metrological Assessment of Infrared Tympanic Thermometers: A Safety Measure
| Ana Luisa Silva1, Claudia Pereira1, Sílvia Moutinho1, Cecilia Rodrigues2, Idalina Beirao2 and Humberto S Machado3* | |
| 1Quality Management, Quality Department, Hospital Port Center, EPE, Porto, Portugal | |
| 2Clinical Governance, Quality Department, Hospital Port Center, EPE, Porto, Portugal | |
| 3Anesthesiology Department, Hospital Port Center, EPE, Porto, Portugal | |
| *Corresponding Author : | Humberto S Machado Anesthesiology Department, Hospital Port Center EPE, Porto, Portugal Tel: 351-935848475 E-mail: hjs.machado@gmail.com |
| Received date: Feb 24, 2016; Accepted date: Apr 01, 2016; Published date: Apr 07, 2016 | |
| Citation: Silva AL, Pereira C, Moutinho S, Rodrigues C, Machado HS, et al. (2016) Metrological Assessment of Infrared Tympanic Thermometers: A Safety Measure. J Preg Child Health 3:240. doi:10.4172/2376-127X.1000240 | |
| Copyright: © 2016 Silva AL, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Pregnancy and Child Health
Abstract
Background: There are different temperature readings in different body sites that are estimated values of the core temperature. The IR tympanic thermometers measure the thermal radiation of the tympanic membrane. These devices are often considered the best non-invasive and most accurate technique to measure body temperature. The incorrect use and the features of the IR tympanic thermometers may lead to significant errors in temperature readings. A metrological approach allows the analysis of the accuracy of the IR tympanic thermometers when compared to a standard electronic device. The main purpose of this study was to assess the measuring errors of the infrared (IR) tympanic thermometers over time and to decide the best time interval between metrological assessments. Methods: The metrological control of IR tympanic thermometers (n=125 used in adult and n=21 in paediatric patients) was based on the comparison with a thermal imaging black body device. An acceptance criterion (AC) of ±0.2°C was considered for metrological control. Results: 93.90% of the errors of low temperature readings (32°C) and 94.24% of the errors of high temperature readings (40°C) were within the acceptance criterion (±0,2°C). Results show 6% of the errors out of specifications. The maximum and minimum errors were +2.5°C and –0.8°C and +0.8°C and -5.2°C for low and high temperatures, respectively. For high temperatures the errors decrease gradually over time unlike to the observed regarding the low temperatures. Conclusions: The variability of errors might be device related; nevertheless it does not preclude its reliability. Significant errors were not found. The accuracy of the IR tympanic thermometers improved over time for high temperatures. Regular metrological assessments are needed to identify errors and assure a good performance of the IR tympanic thermometers.
| Keywords |
| Infrared tympanic thermometers; Metrological assessment; Safety; Body temperature; Hypothermia; Hyperthermia; Hyperpyrexia |
| Introduction |
| The measurement of body temperature is essential in health care as temperature is considered a vital sign [1]. The normal body temperature (37°C) and fever (≥38°C) are standard values, even though the body temperature is generally accepted as a range rather than a fixed temperature [2,3]. Hyperthermia occurs whenever body temperature exceeds the normal temperature values and hyperpyrexia is considered when temperature values are greater than 41°C. |
| Hypothermia is defined as temperature values less than 35°C, whilst severe hypothermia is less than 32°C [4,5]. Some authors even consider that hypothermia may vary between 32°C to 34°C for mild hypothermia, 28°C to 32°C for moderate and <28°C for severe hypothermia [6]. On the other hand, for neonates (normal temperatures within 36.5°C and 37.4°C) hypothermia range considered was 36°C to 36.4°C (mild), 32°C to 35,9°C (moderate) and <32°C (severe) [7]. |
| The human body gives different temperature readings in different sites of the body such as rectal, oral, tympanic and axillar temperatures that are estimated values of the core temperature in the central pulmonary artery. The hypothalamus regulates body temperature according to the core temperature [1,8]. In fact, core temperature can only be measured invasively (often using a pulmonary artery catheter connected to a thermistor) which is possible only for intensive care units [2]. Therefore the best non-invasive thermometer to be used in clinical practice should be the one that presents temperature readings similar to the temperature in the central pulmonary artery. |
| The core temperature is the highest body temperature. Rectal temperature is about 0,3°C and 0,5°C higher than oral [9] and axillar [10] readings respectively and temperature adjustments are considered in modern devices by the manufacturers. Some authors demonstrated that rectal temperature readings are frequently incorrect due to the poor blood supply in the rectum and little heat losses [8,11,12]. Additionally, a previous study [13] confirmed that tympanic temperature tracked the core temperature at central pulmonary artery better than rectal temperature [14]. |
| IR tympanic thermometers measure the thermal radiation of tympanic membrane. As tympanic membrane and hypothalamus share the arterial blood supply, IR tympanic thermometers might be the best non-invasive thermometers to be used in clinical practice [1,14-19]. |
| Nevertheless the tympanic temperature measured is a mix of the heat from the tympanic membrane and the ear inner surfaces [20] as the probe is placed away from tympanic membrane about 1,5 cm [1]. The adjustment of tympanic temperature to the other sites of the body temperatures depends on the algorithm defined by manufacturers [20]. |
| IR tympanic thermometers have some advantages namely the ease of use, speed, improved hygiene, non-invasive measurements and large patient approval [2,14]. However, a rigorous hygiene and a proper technique are essential for the accuracy of these thermometers [1,14]. Regarding the user technique, the temperature readings may vary depending on the placement of the probe i.e., when the angle between the ideal direction and the observation direction is large (>80°) [9,12,18,21]. |
| Temperature measurements often exhibit high patient variability mostly due to human body inherent factors as the normal thermoregulation, the gender, age and the site of measurement. In addition, regarding the tympanic and axillary temperatures, individual variability in temperature has been observed between the right and left sites [1,10,14,19]. |
| Metrological assessments do not consider erroneous measurements related to the human body factors or the user technique since the metrological assessment of thermometers is performed with a standard device instead of patients. This standard device measures the errors of the IR tympanic thermometers and makes automatic adjustments so that the error is minimized, ideally to an error equal to zero. |
| Traditionally, in many cases measurement uncertainties are acceptable for routine clinical work and experienced health professionals usually disregard apparently erroneous measurements. However due to modern measurement systems it is becoming more difficult to detect malfunction or measurement errors in modern electronic devices. |
| The factors named previously introduce important errors which might significantly influence the assessment of the health condition of the individual, leading, for instance, to the incorrect diagnosis of fever, hypothermia or hyperthermia. |
| Some clinical departments in CHP, EPE are hesitant in using IR tympanic thermometers owing to the previously mentioned uncertainties associated to the quality of the measurements. |
| Therefore, the aim of our study was to assess the measuring errors of the IR tympanic thermometers in order to conclude about the safety of using this type of devices in clinical practice, and to analyse the evolution of the error over time in order to decide about the best time interval to be considered between metrological assessments. |
| This study’s relevance to clinical practice is based on the fact that body temperature is a vital sign regularly monitored. The identification of the errors of the body temperature measurements is essential to the correct diagnosis of patient condition. Significant errors of temperature measurements may lead to clinical misjudgementsregarding the assumption of hypothermia, hyperthermia or hyperpyrexia. |
| Methods |
| Study sample |
| All IR tympanic thermometers used in CHP for adults and children were identified resulting in a total of 152 thermometers. From these, 6 thermometers that presented malfunctions (e.g., malfunctions in battery or display) were disregard and not included in our study. Therefore 146 IR tympanic thermometers of the same type were studied (from which 125 thermometers are used in adult wards and outpatient departments and 21 thermometers are used in paediatric departments). The sample of 146 thermometers allowed a set of 295 effective measurements (corresponding to 52 thermometers verified once, 42 thermometers verified twice, 49 thermometers verified three times and 3 thermometers verified four times). |
| Technical and metrological data |
| Technical and metrological data were collected and considered in the analysis of the equipment. The main technical and metrological data of IR tympanic thermometers are summarized in Table 1. |
| The annual plan for metrological assessment of all IR tympanic thermometers predicted quarterly interventions since the control of these thermometers should be done regularly and in short periods of time as a preventive measure. |
| The assessment of the IR tympanic thermometers was performed by comparison with a stable thermal imaging black body device of high emissivity. The black body device used to assess CHP thermometers has the following characteristics: |
| Operates in the measuring range with an overall uncertainty of ± 0,2°C (and the international standard [22] requires that the radiation temperature of the black body is calibrated with a maximum uncertainty of 0,07°C) has a reference platinum resistance thermometer traceable to a national standard body has a conical shape cavity and their inner surfaces are black to achieve an emissivity equal or greater than 0,95. This device is annually tested by the manufacturer as well as calibrated by an accredited entity for this purpose. |
| Metrological assessment |
| Steps |
| Turn on the black body and allow it to warm up and stabilize according to the manufacturer’s instructions Check to make sure the probe lens of the infrared thermometer was clean. Attach the probe cover before testing Testing requires inserting the test thermometer into the aperture of black body device, recording the reading of low and high temperatures Repeat the previous step three times: the measured error corresponds to the average of the errors of three temperature readings. These three readings are performed for low and high temperatures Keep a record of the test, including: Date of testing; Name of the CHP department; Serial number of the thermometer; Serial number of black body device; The test thermometer readings; The reference thermometer readings; The measured error; The actions taken (if any) Label IR tympanic thermometers according to the results compliant or not compliant. The temperature is read at low and high temperature points 32.0°C and 40,0°C. The error of test thermometers is calculated using the equation |
| Error test reading-reference reading |
| Whenever AC ≥ error, the IR tympanic thermometer is accepted. If the IR tympanic thermometer exceeds the AC the thermometer returns to the manufacturer for adjustment or replacement. After metrological assessment of all IR tympanic thermometers the error of each set of measurements was analysed. |
| Results |
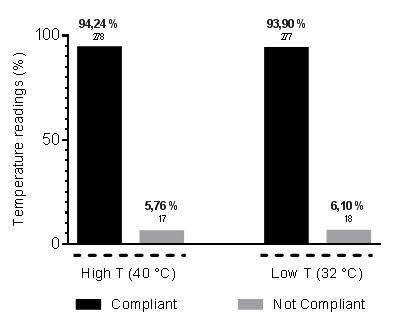
| Metrological assessment of IR tympanic thermometers showed that the errors of 93,90% of temperature readings at low temperature points (32°C) were within the acceptance criterion (±0,2°C), demonstrating that 6,10 % of readings were out of specification (Figure 1). |
| Similarly for high temperatures (40°C), the results showed that the errors of 94,24% of temperature readings were within the acceptance criterion (±0,2°C) and 5,76% of readings were out of specification (Figure 1). |
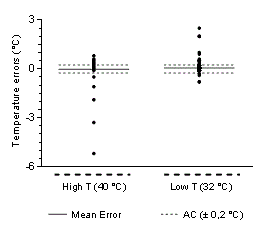
| Figure 2 shows the scattering of the measured errors for low and high temperatures, with a higher amount of the errors around the zero value for both temperatures (Table 2). |
| In addition, presents the mean error (±SD) for compliant and not compliant readings. |
| The analysis of the not compliant readings (errors > AC) showed that errors are mainly higher than +0,2°C for low temperatures and lower than -0,2°C for high temperatures (Figure 2). |
| The maximum and minimum errors of the not compliant readings were +2,5°C and –0,8°C for low temperatures and +0,8°C and -5,2°C for high temperatures. The minimum temperature registered was 31,2°C and the maximum was 40,8°C. |
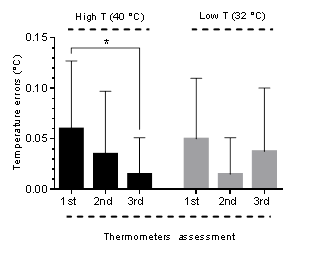
| To study the measured errors over time, only compliant IR tympanic thermometers verified three times in an overall six month time period were analysed (40 thermometers used in adults). Figure 3 shows the evolution of the errors between the first, second and third assessments, (matching the first, third and sixth month). |
| Analysing Figure 3 it is possible to notice that the errors decrease gradually over time for high temperatures. On the contrary, for low temperatures the errors decrease from the first to the second assessment and increase from the second to the third assessment. The statistic test One-way ANOVA was used to compare the errors over time and statistic significant differences were only verified for high temperatures between the first and the third assessment (p < 0,01). |
| Discussion |
| The current study shows that IR tympanic thermometers are suitable to measure body temperature in clinical practice in CHP. Our findings match previously published results, regarding adults and children that compare temperatures in numerous sites of the body and using different devices [14-18]. However, to our knowledge this study is the first attempt to assess the performance of IR tympanic thermometers in clinical practice using a metrological approach. |
| Our results demonstrated that the errors of the IR tympanic thermometers are mostly within the AC (≤±0,2°C). In fact, approximately 94% of the IR tympanic thermometers were considered accurate to measure body temperature and safe. |
| Nevertheless, 6% of the errors found for low and high temperatures are out of specification. In addition, we consider that the variability observed in this 6% of the measurements do not have relevant impact in clinical practice. In fact, only one measurement (that is not significant) led to a severe temperature alteration from 40,8°C to 34,8°C which was enough to change hyperthermia into hypothermia. As metrological assessments did not consider erroneous measurements associated to the user technique or human body factors, this study also confirmed that a large variation of the errors is related to the features and the operation of the IR tympanic thermometers. |
| Neonatology departments were not included in our study as in CHP IR tympanic thermometers are not used in neonates. For that reason, the metrological assessment of the thermometers and their accuracy analysis was likewise performed for the thermometers used in adults and paediatric departments. A consistent accuracy or inaccuracy of the IR tympanic thermometers over time was not possible to conclude [23-31]. |
| In fact, at high temperatures, it was verified a decrease of the errors over time. Although, even supposing that this result is related to the automatic adjustment of the IR tympanic thermometers, we remain assuming that the evolution of the errors might be influenced by the continued use of these thermometers in the clinical practice. Therefore, it was not possible to conclude about the evolution of the error over time, as well as the best time interval to perform the metrological assessments. A possible explanation for our results is the small sample size and the short time period of the study that are recognized limitations of this work. Future work is needed to validate our findings where improvements in the evolution of the error over time are desirable. |
| Conclusions |
| IR tympanic thermometers are easy and safe to use. The variability of errors might be device related, but this does not preclude its reliability to measure tympanic temperatures. Improvement in accuracy over time in high temperature readings should not exclude regular metrological assessment of these devices. |
| References |
|
Tables and Figures at a glance
| Table 1 | Table 2 |
Figures at a glance
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 |
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 11867
- [From(publication date):
April-2016 - Aug 18, 2025] - Breakdown by view type
- HTML page views : 10821
- PDF downloads : 1046
