Onodi Cell Mucocele: Case Report
Received: 11-Aug-2014 / Accepted Date: 09-Oct-2014 / Published Date: 16-Oct-2014 DOI: 10.4172/2161-119X.1000176
Abstract
Onodi cells represent a type of posterior ethmoid cells in the sphenoid sinus; here, Pneumatisation occurs as a result of posterolateral. In the case reported, a 37-year-old Male patient was referred to our clinic with complaints of approximately 4-5 years of Headaches, nasal congestion and snoring. Paranasal sinus computed tomography (CT) scans showed left isodense lesions exhibiting the isolated Onodi cell. Surgery was planned to remove the Onodi cell mucocele using the endoscopic approach. The Lesion had expanded to completely fill the Onodi cell; lesion was totally removed by Aspiration. Fifteen months postoperatively, the patient underwent CT, and Onodi cells with completely normal aeration were observed. Onodi cells, the optic nerve and the internal carotid artery are in close proximity to one another, and therefore the existence Of Onodi cells are important information. Therefore, elucidating the detailed anatomy of the paranasal sinuses and the recognition of variations amongst them will facilitate accurate diagnosis of patients, as well as physicians’ management of complications which may occur.
Introduction
Various anatomical variations can be seen in the paranasal sinuses [1]. The Onodi cell has been defined as a posterior ethmoid cell that has pneumatized laterally and superiorly to the sphenoid sinus. Onodi cells are positioned in the lateral direction, close to the optic nerve and internal carotid artery. It is important to identificate the onodi cell because of its relationship with vital adjacent structures [2-3]. In some cases, Onodi cells may cross through the optical nerve. Optic nerve dehiscence often accompanies the Onodi cell. The optic nerve can be damaged during the natural course of the disease in this region; moreover, there is also a possibility that it can be damaged during surgical procedures [4-9].
Paranasal sinus mucoceles are caused by the obstruction in the ductus of mucous glands. Mucoceles are expansile lesions and can cause erosion on the paranasal sinus walls. Mucoceles are often caused by inflammation of the sinus ostium. However trauma, tumors, polyposis and surgical manipulations can cause mucoceles. Sinus mucoceles are most frequently seen in the frontal sinus however sphenoid sinus is a rare location for mucoceles [9].
This article presents a rare case of an Onodi cell mucocele and data from the literature are reviewed.
Case Presentation
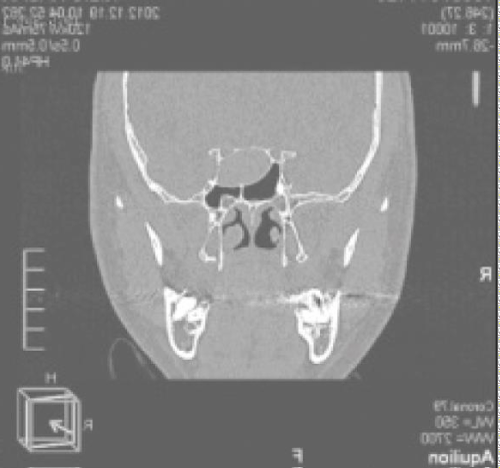
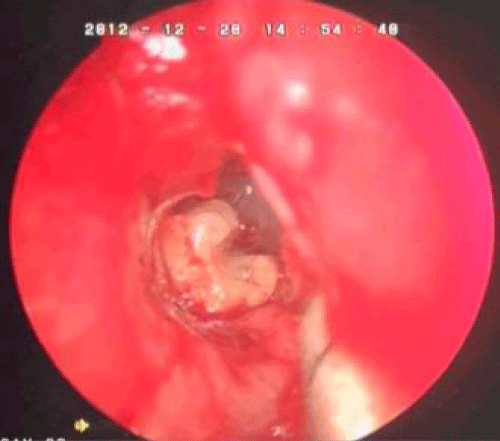
A 37-year-old male patient was referred to our clinic with the complaints of headache that for 4–5 years, nasal obstruction and snoring. Anterior rhinoscopy revealed that the nasal septum was deviated to the right side and compensatory left turbinate hypertrophy was present. Paranasal sinus Computed Tomography (CT) showed that an isodense lesion of the Onodi cell on the left side (Figure 1). There was no evidence of expansion or destruction of the bony structure. Surgery was planned to remove the Onodi cell pathology using the navigation assisted endoscopic approach. Surgery was performed under general anesthesia. Topical and infiltration anesthesia was performed. Basis of the Onodi cell was found approximately 1.5 cm superior of the left choana. When Onodi cell was opened, the entire sinus was filled with a dirty white lesion surrounded by a thick wall (Figure 2). The contents of the mucocele were totally removed by aspiration and the cell was marsipualized.
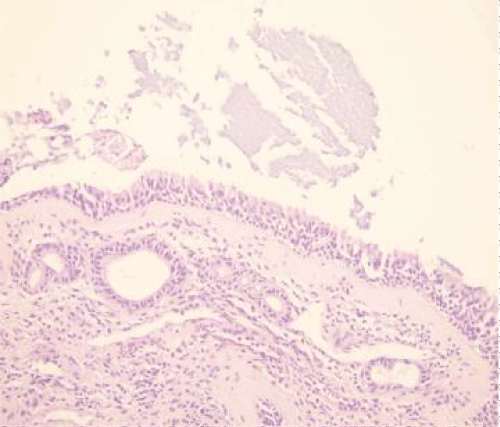
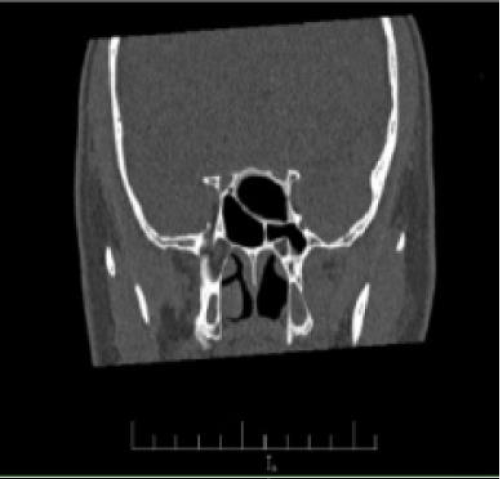
The removed lesion was sent for pathological examination. The medial wall of the optic canal was observed as an intact ridge. The patient did not develop any complications during the postoperative followup. Through microscopic examination, mucocele was diagnosed. Microscopically, the cystic cavity was filled with mucinous material and the cavity wall lined with benign respiratory mucosa including a mild, chronically inflammatory infiltrate, subepithelial hyalinization and telangiectatic vascular structures (Figure 3). One year follow up after the operation paranasal sinus CT showed no recurrence or residual disease (Figure 4). Informed consent was obtained from the patient.
Discussion
The importance of the close relationship between posterior ethmoid cells and the optic nerve was first introduced by Adolf Onodi in 1904 [2]. The reported incidence of Onodi cells ranges from 8% to 14% on the basis of CT and radiological findings [1-3]. However, this ratio was found to be 60% in cadaver studies [10]. Onodi cells are often close to the optic nerve or the internal carotid artery. Sometimes, these cells can even cross directly through the optic nerve. Optic nerve injury during endoscopic sinus surgery is a rare complication. Moreover, the presence of anatomical variations such as Onodi cell may play a role in the development of this complication. However, preoperative or intraoperative recognition of the Onodi cell reduces the likelihood of injury to the optic nerve [3].
Paranasal sinus mucoceles most commonly occur at the age of 30-60 years. Frontal sinus is most frequently affected (65%), followed by the ethmoid sinus (25%) and maxillary sinus (10%) [11]. Sphenoid sinus and Onodi cell mucocele are considered to be very rare. They often do not show clinical signs. However, some patients may have non-specific symptoms such as headache. Sometimes, a decrease in visual acuity may even be the first presenting symptom. Indeed, in our case, the patient experienced headache, nasal congestion and snoring symptoms, but had no other complaints.
In the diagnosis of the mucocele, CT and Magnetic Resonance Imaging (MRI) are useful. On CT, affected paranasal sinus is completely opacified and expanded. Density is variable depending on the hydration degree of the content. Thinning and erosion of adjacent bony wall can be detected on CT. On the other hand, the MRI signal intensity is very variable depends on the proportions of mucus, protein and water. Mucoceles can be seen hypointense on T1-weighted images and hyperintense on T2-weighted images. In advanced cases, expension and compression to surrounding tissues can be observed [12]. Definitive diagnosis is made through cytology and/or biopsies. In our case, the lesion was limited to Onodi cell without bony destruction. After the CT scan, patients were operated on with the initial diagnosis of mucocele. During the operation, it was found that Onodi cell was filled with a yellow-white lesion. Onodi cell was marsipualized. Histopathological examination of the removed material was reported as mucocele (Figure 3). Surgery is the first treatment modalities for paranasal sinus mucoceles. Antibiotic treatment is necessary if there is muco-pyelocele. In our case, an Onodi cell mucocele was detected without any complications. Endoscopic sinus surgery was performed after 10 days antibiotic treatment.
Conclusion
Onodi cell shows the close anatomical relationship with the optic nerve and internal carotid artery. Onodi cell mucoceles are rare but they may cause vision loss which can lead to medical emergencies. Therefore, it is necessary to carry out detailed investigation of the anatomy of the paranasal sinuses and recognize possible variations. This will result in accurate diagnosis of patients, and allow physicians to plan for and manage any complications that may arise. In our case, an Onodi cell mucocele was detected and successfully treated with endoscopic sinus surgery without any complications.
References
- Stammberger HR, Kennedy DW; Anatomic Terminology Group (1995) Paranasalsinuses:anatomic terminology and nomenclature. Ann OtolRhinolLaryngolSuppl 167: 7-16.
- Onodi A (1904) Die Sehstorungen und ErblindungnasalenUrsprunges, bedingtdurchErkrank-ungen der hinterenNebenhohlen. Z Augenheilkd12:23-46.
- Driben JS , Bolger WE, Robles HA, Cable B, Zinreich SJ (1998) The reliability of computerized tomographic detection of the Onodi (Sphenoethmoid) cell. Am J Rhinol 12: 105-111.
- Fukuda Y, Chikamatsu K, Ninomiya H, Yasuoka Y, Miyashita M, et al. (2006) Mucocele in an Onodi cell with simultaneous bilateral visual disturbance.AurisNasus Larynx 33: 199-202.
- Kitagawa K, Hayasaka S, Shimizu K, Nagaki Y (2003) Optic neuropathy produced by a compressed mucocele in an Onodi cell. Am J Ophthalmol 135: 253-254.
- Yoshida K, Wataya T, Yamagata S (2005) Mucocele in an Onodi cell responsible for acute optic neuropathy. Br J Neurosurg 19: 55-56.
- Toh ST, Lee JC (2007) Onodi cell mucocele: rare cause of optic compressive neuropathy. Arch Otolaryngol Head Neck Surg 133: 1153-1156.
- Ogata Y, Okinaka Y, Takahashi M (1998) Isolated mucocele in an Onodi cell. ORL J OtorhinolaryngolRelat Spec 60: 349-352.
- Lim SA, Sitoh YY, Lim TC, Lee JC (2008) Clinics in diagnostic imaging (120). Right rhinogenic optic neuritis secondary to mucocoele of the Onodi cell. Singapore Med J 49: 84-87.
- Thanaviratananich S, Chaisiwamongkol K, Kraitrakul S, Tangsawad W (2003) The prevalence of an Onodi cell in adult Thai cadavers. Ear Nose Throat J 82: 200-204.
- Lund VJ, Henderson B, Song Y (1993) Involvement of cytokines and vascular adhesion receptors in the pathology of fronto-ethmoidalmucocoeles.ActaOtolaryngol 113: 540-546.
- Lim CC, Dillon WP, McDermott MW (1999) Mucocele involving the anterior clinoid process: MR and CT findings. AJNR Am J Neuroradiol 20: 287-290.
Citation: Bilici S, Huq GE, Sunter AV, Yigit O, Yıldız M (2014) Onodi Cell Mucocele: Case Report. Otolaryngology 4:176. DOI: 10.4172/2161-119X.1000176
Copyright: © 2014 Bilici S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 16516
- [From(publication date): 10-2014 - Jul 04, 2025]
- Breakdown by view type
- HTML page views: 11893
- PDF downloads: 4623