Research Article Open Access
Oral Squamous Cell Carcinoma in Moroccan Population: A Cartographic Study
Saliha Chbicheb, Narjiss Akerzoul* and Wafaa El Wady
Faculty of Dentistry of Rabat, Mohammed V University, Rabat, Morocco
- *Corresponding Author:
- Narjiss Akerzoul
Faculty of Dentistry of Rabat
Mohammed V University, Rabat, Morocco
Tel: +2126 69 10 53 25
E-mail: narjissakerzoul87@gmail.com
Received September 09, 2015; Accepted September 18, 2015; Published November 16, 2015
Citation: Chbicheb S, Akerzoul N, El Wady W (2015) Oral Squamous Cell Carcinoma in Moroccan Population: A Cartographic Study. Cosmetol & Oro Facial Surg 1:102. doi:10.4172/jcofs.1000102
Copyright: © 2015 Chbicheb S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Cosmetology & Oro Facial Surgery
Abstract
Purposes: Study the epidemiological and histopathological profile of the oral cancers in Adult patients in many Oncologic Centers and Hospitals in Morocco. Our aim is to define the importance of Oral Cancer, and also to describe the oral cancers in adult patients, theirs frequences and theirs histopathological characteristics. Materials and methods: This is a cartographic study review of patients with oral cavity cancers who viewed the ENT department at the Specialized Hospital of Rabat, the Instruction Military Mohammed V Hospital (IMMVH) of Rabat, and other Oncologic Centers in various cities of the Kingdom of Morocco, during the period from January 2005 to December 2012. We did collect 1453 cases. The collected information was recorded on a pre-operation plug. Results: In our study, patients whose age is above 40 years were the age bracket most affected by the oral cancer with 91.3%, while patients whose age is less than 40 years old represented only 8.7% of the cases affected by the oral cavity cancer. In our study, males accounted for 63% of all cases. The pattern associated with the tumor was the most reported in 64% of cases, including the swelling and ulceration. For the histological type of the tumor in our sample, Oral Squamous Cell Carcinoma (OSCC) was the most dominant histological type in 78% of cases. The predominant consultation period was later 6 months with 57%, according to our sample. Tobacco was the most dominant risk factor with 41% of all cases. In our sample 76.6% of patients had as a major promoting factor a poor oral health status, and prolonged sun exposure was mentioned in 13.3% of cases. Conclusion: Our results correlate well with previously published clinicopathological data on comparable studies, which is important when considering the applicability of results from biomarker studies performed on this material compared to other retrospective studies, and vice versa.
Keywords
Oral squamous cell carcinoma; Oral cavity
Introduction
Oral cancer, with an annual incidence of over 300,000 cases, is reported to be the eighth most common cancer globally [1,2]. Incidence and mortality as a result of oral cancer are higher in developing countries when compared to developed countries [2,3]. According to the latest World Health Organization (WHO) data recorded in 2010, the death rate due to oral cancer in the North Africa is reported to be approximately 2 in 100,000, which is much lower than that in India and in the United States [4]. Squamous cell carcinoma of the head and neck (HNSCC) is primarily a disease of older adults, occurring most frequently in patients older than age 45. Epidemiological studies over last 20 years have shown a steady rise in the incidence of these cancers in younger adults (age 18–45 years), especially in cancers of the oropharynx and oral cavity [1,2]. The predilection for these particular subsites vs. other sites such as the larynx or the hypopharynx remains unclear. Likewise, the aetiology for early onset of these neoplasms is not well understood. Squamous cell carcinomas (SCCs) of the lip and oral cavity comprise 90 to 95% of all oral malignancies. Hidden regional metastasis in oral squamous cell carcinoma (OSCC) is prevalent in at least 30% of cases [5]. Clinical examination alone is proven to be unreliable in detecting such regional metastasis. Identification of regional metastasis and early intervention could decrease mortality rates. Improved diagnostic modalities are required not only to detect regional disease but also to decrease postoperative morbidity and mortality. This study aims to determine the prevalence of Oral Squamous Cell Carcinoma in the Moroccan population, to correlate cases of OSCC with age, gender, site, grade, and clinical presentation [4,5].
Materials and Methods
This is a cartographic study review of patients with oral cavity cancers who viewed the ENT department at the Specialized Hospital of Rabat, the ENT department at the Instruction Military Mohammed V Hospital (IMMVH) of Rabat, the Oncologic Centers of Agadir, Marrakech, Casablanca, Oujda, Fes, the Private Oncologic Clinic of Casablanca, the Al Azhar Nakhil Clinic of Rabat, the Moulay Abdellah Hospital, during the period from January 2005 to December 2012. We did collect 1453 patients consultation records and files. Only 1327 cases were selected. The collected information was recorded on a preoperation plug. In the absence of records of some patients, it was based on the department computerized database. Were excluded from the study all patients with pathological examination which did not allow to define the nature of cancer, patients with cancer in the nasopharynx, maxillary sinus and the parotid gland, patients having a cancer other than cancers of the oral cavity; and patients with benign tumors of the oral cavity.
Analysis of the results was performed using the software Statistic Package for Social Science (SPSS Version 13.0) for Windows. The implementation of graphics was done with Excel 2007 software. Quantitative variables were expressed as mean ± standard deviation. Categorical variables were expressed as effective and valid percentage (%).
The comparison of categorical variables was performed using the “chi.”2 Test. The difference is considered statistically significant when the p value is strictly less than 0.05.
Results
In our study males accounted for 63% of all cases. The median age was 60 years for men and 64 years for women. Our results were similar to those found in the cancer center Sidi Mohammed Ben Abdellah in Rabat in 2011 when men represented 60.3% and the oncology center in Fez in 2012, where men represented 68% of cases. In Oncology Centers in Marrakech and Agadir in 2012, male prevalence was 56%, while female one was 44%. The pattern associated with the tumor was the most reported in 64% of cases, including the swelling and ulceration. The predominant consultation period was later 6 months with 57%, according to our sample.
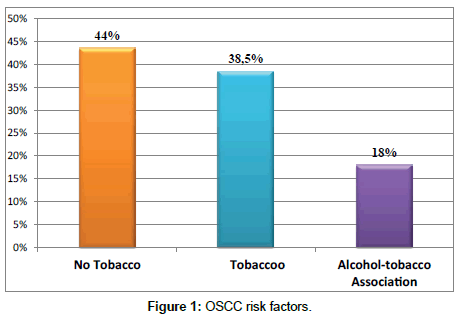
Tobacco was the most dominant risk factor which accounts for 41%. In our study, chronic smoking was mentioned in 38.5% of cases; (Figure 1) 18% was alcoholo-smoking. According to collected clinical information, the most common clinical form was the ulcerative burgeoning form with 55%, the budding form comes in second place with 25% of patients.
Concerning the location of the tumor, the lips were the most affected seat in 37% of cases (upper lip represented 21.62% of all cases of lip cancer), the second location was the tongue with 17% of cases.
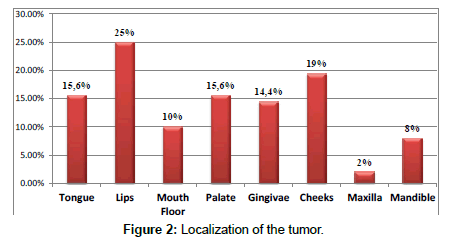
In our study, the lips represented the most common tumor location, with 25% of cases with 64.4% for the lower lip, tongue represented 15.6% (Figure 2). The study in Oncology Center of Fez (2012) also noted a predominence in the lips with 37%, followed by the tongue with an incidence of 17%. The study conducted at the Oncology Center of Oujda (2012) mentioned a common location for the lips and tongue with a rate of 26.9% each.
For tumor size, T4 size dominated in the vast majority of patients with 47%, while T2 size was observed in only 27% of cases.
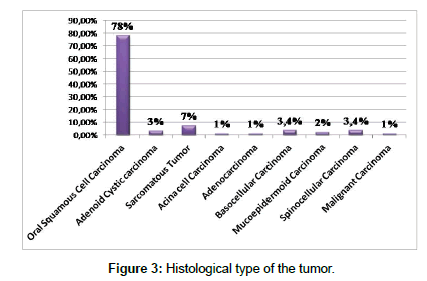
For the histological type of the tumor in our sample, Squamous Cell Carcinoma was the most dominant histological type in 78% of cases, (Figure 3) followed by basal cell carcinoma with 14% of cases. Compared to these results, the studies in Oncology Centers in Marrakech and Agadir also reported a high prevalence of Squamous Cell Carcinoma with 80.2% in Marrakech and 87% in Agadir.
In terms of staging, our study was local tumor extension in 64.4% of cases, and locoregional in 32%. Patients who have distant metastases constituted 6.7% of all cases. These results are comparable to those found in the Oncology Center of Fez in 2012, where the study found a local extension in 66%, locoregional in 50%, and metastasis in 4%. In Oncology Center of Casablanca in 2011, the extension was locoregional in 51%.
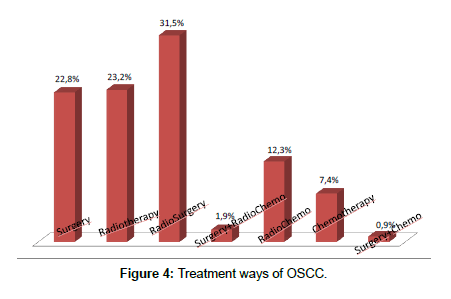
Treatment was based on surgery alone with a rate of 52%, followed by surgery and radiotherapy combination with 33% of cases (Figure 4).
Regarding followed patients, treatment was favorable in 56% of cases, 35% had tumor recurrence, 6% developed metastases, and 2% were dead. The study in Oujda Oncology Center (2012), reported that 40.5% of the cases responded to treatment and in 20% of cases, there’s been a recurrence.
Discussion
The OSCC is a malignant neoplasm, multifactorial and considered the highest incidence among all oral cancers. Just as other carcinomas, the risk of oral squamous cell carcinoma increases with age, especially in men. Through a cartographic study of cases of this tumor, it was possible to compare the results with the current literature, confirming that the impact in terms of gender, age and anatomical location, remains the same over the years [1,2].
Our results were similar to those reported in the literature. The authors reported that the frequency of cancers of the oral cavity is 2.5% of all cancers and 30% of cancers of the superior aerodigestive tract [3].
Male predominance is observed. But the feminine curve is clearly ancestry none that she exceeded the male curve according to some authors especially in sub-Saharan African countries. Beyond that there is still a male predominance in the Moroccan population. Although this male prevalence is overwhelming, Gauzéran et al. in 2007 noted among the European population that feminine curve is now clear descent due to the significant increase in smoking among women [3,4].
The most found location remains the tongue. Tumors of the lips, floor of the mouth and palate are also common. In literature, SCC is by far the most dominant histological type in cancers of the oral cavity. Chouaïb et al. reported 21.9% in the tongue and 14.3% in the palate. He also reported a predominance of Squamous Cell Carcinoma with 90.5% and 73.1% of cases. According to Lezy et al. 90% of cancers of the oral mucosa are Squamous Cell Carcinomas pretty differentiated, the others being mainly salivary. Lymphomas, sarcomas and melanomas remain very rare. In most cases, the average time between the first symptom and diagnosis is less than six months in our study [5-7].
Some authors confirmed that the first metastasis is located in the cervical lymph nodes. Pulmonary localization comes in second place with a rate of 30% regardless of the location of the primary cancer, what justifies setting a full extension sheet up in search of synchronous localization of oral cancer [7]. Most experts believe that oral cancer is a multifactorial disease, and many well-established risk factors have been identified. Tobacco use is universally regarded as the single biggest risk factor. About 80% of OSCC patients have a history of smoking tobacco and a person’s risk of developing OSCC increases with heavier daily use and longer duration of use [6,7]. Due to the lack of relative risk data regarding OSCC, the risk of head and neck SCC for cigarette smokers is estimated to be 10-fold over that of people who have never smoked cigarettes. Our results were similar to those found in Rabat Oncology Center in 2011, where the study found the notion of smoking in 35.3% of cases. In the Casablanca Oncology Center in 2011, we found that chronic cigarette smoking was accounted in 56%.
Smokeless tobacco (chewing tobacco, moist snuff and dry snuff) has also been implicated in OSCC. Recent epidemiologic studies have found that smokeless tobacco users are about twice as likely to develop OSCC as those who have never used. It should be noted that dry snuff, which is used most often in the southern U.S, appears to be more dangerous than moist snuff or chewing tobacco. Current literature indicates that the association between OSCC and smokeless tobacco is not as strong as the relationship between OSCC and tobacco smoking. According to the latest report from the National Academy of Medicine, tobacco is the leading cause of cancer with a rate estimated at 27% in men and 6% in women. It is also at the dawn of this century, the source of 33% of cancer deaths in men and 10% women [7-9]
Excessive alcohol consumption is another important risk factor for OSCC. While it is unclear whether alcohol abuse alone can cause cancer, the risk of alcohol and tobacco in combination is well established [4,7].
Regarding occupational factors in our study, they are strongly suspected in cancer genesis, but their identification is difficult because of their frequent association with tobacco and alcohol. These factors include formaldehyde, asbestos, synthetic mineral fibers, welding fumes, polycyclic aromatic hydrocarbons, and wood dust. The International Center for Research on Cancer notes that variations between countries are very important. This reflects the degree of exposure of the population of each region to the risk factors and the variation of environmental, nutritional, and genetic factors. All authors agreed that tobacco intoxication and ethyl impregnation are often associated. Their effects on the risk of oral cancer are multiplicative. The carcinogenic role of cannabis, bad oral hygiene, the prosthetic irritation remain controversial [8-12]
The treatment of OSCCs may consist on surgery, radiation and/or chemotherapy. Surgery may include a neck dissection if regional lymph node metastasis is suspected [13]. A lymph node with metastatic OSCC will usually be enlarged, firm and non-tender. About 20% of patients with SCC of the oral cavity have cervical lymph node metastases at the time of diagnosis. SCC of the oropharynx is prone to earlier metastasis, with 50% of patients having involved cervical lymph nodes when diagnosed [14-16]. This highlights the importance of a thorough head and neck exam as a component of the oral cancer screening process [16].
The precise treatment regimen that a given patient receives depends largely on the location and stage of their disease. Staging is a quantification of the size and metastatic spread of a tumor. This determination is carried out by running imaging tests such as X-Ray, CT, MRI and PET scans. The TNM protocol is the preferred method of staging OSCCs, where T indicates the size of the primary tumor, N stands for involvement of local lymph nodes and M for distant (below the clavicles) metastasis. Once each of these factors is evaluated, a stage of I, II, III or IV is assigned to the cancer, with stage IV having the worst prognosis. In general, surgery is the initial treatment for SCCs of the oral cavity, which may be followed by radiation, chemotherapy or both. Oropharyngeal SCCs are usually treated by a combination of radiation and chemotherapy [16-18]. New therapeutic regimens continue to be developed with the aim of maximizing the desired effect on cancer cells while minimizing patient morbidity and thus improving survival and quality of life. Examples of these new techniques include intensity modulated radiation therapy, induction chemotherapy and new drugs that target specific components of cancer cells (targeted therapy). Clinical trials are constantly being conducted to evaluate the utility of promising new therapies [16,18].
The prognosis for patients with OSCC varies based on stage and other factors. Chouaib’s study in 2010, noted 27.5% of recurrences, and survival at 5 years was favorable for cancers of the lips, while a worse prognosis was observed with gum cancer. According to the most recent epidemiologic data available, the overall 5-year survival rate for OSCC is around 60% [19,20].
Conclusion
Despite advances in the treatment and understanding of the underlying molecular mechanisms involved in the pathogenesis of oral cancer, survival rates have improved significantly.
Our results correlate well with previously published clinicopathological data on comparable studies, which is important when considering the applicability of results from biomarker studies performed on this material compared to other retrospective and cartographic studies, and vice versa.
References
- Slotman GJ, Swaminathan AP, Rush BF Jr (1983) Head and neck cancer in a youngage group: high incidence in black patients.Head Neck Surg 5: 293-298.
- Sarkaria JN, Harari PM (1994) Oral tongue cancer in youngadultslessthan 40 years of age: rationale for aggressivetherapy.Head Neck 16: 107-111.
- Gilroy JS, Morris CG, Amdur RJ, Mendenhall WM (2005) Impact of youngage on prognosis for head and neck cancer: amatched-pair analysis.Head Neck 27: 269-273.
- Islami F, Fedirko V, Tramacere I, Bagnardi V, Jenab M, et al. (2011) Alcoholdrinking and esophagealsquamouscellcarcinomawith focus on light-drinkers and never-smokers: asystematicreview and meta-analysis.Int J Cancer 129: 2473-2484.
- Rosenblatt KA, Daling JR, Chen C, Sherman KJ, Schwartz SM (2004) Marijuana use and risk of oral squamouscellcarcinoma.Cancer Res 64: 4049-4054.
- Patel SC, Carpenter WR, Tyree S, Couch ME, Weissler M, et al. (2011) Increasing incidence of oral tonguesquamouscellcarcinoma in young white women, age 18 to 44 years.J Clin Oncol 29: 1488-1494.
- Lipkin A, Miller RH, Woodson GE (1985) Squamouscellcarcinoma of the oral cavity, pharynx, and larynx in youngadults.Laryngoscope 95: 790-793.
- Alvarez-Ame´zaga J, Barbier-Herrero L, Pijoan-Zubizarreta JI, Marti´n-Rodri´guez JC, Romo-Simo´n L et al. (2007)Diagnostic efficacy of sentinelnodebiopsy in oral squamouscellcarcinoma. Cohortstudy and meta-analysis. Med Oral Patol Oral CirBucal 12: E235-43.
- O¨ nem E, Alpo¨z E, Gu¨neri P, U¨ nal T, Boyacioglu H. (2010) Oral lesiondiagnosisdilemma: correlationbetweenclinical and histologicaldiagnosis. A samplestudy. SU DishekFakDerg 19: 40-6.
- Fierro-Garibay C, Almendros-Marques N, Berini-Aytes L, Gay- Escoda C. (2011) Prevalence of biopsies oral lesions in a departmentof oral surgery.J Clin Exp Dent 3: e73-7.
- El-Naaj IA, Leiser Y, Shveis M, Sabo E, Peled M (2011) Incidence of oral cancer occultmetastasis and survival of T1-T2N0 oral cancer patients.J Oral MaxillofacSurg 69: 2674-2679.
- Llewellyn CD, Johnson NW, Warnakulasuriya KA (2004) Riskfactors for oral cancer in newlydiagnosed patients aged 45 years and younger: a case-control study in SouthernEngland.J Oral Pathol Med 33: 525-532.
- Soudry E, Preis M, Hod R, Hamzany Y, Hadar T, et al. (2010) Squamouscellcarcinoma of the oral tongue in patients youngerthan 30 years: clinicopathologicfeatures and outcome.Clin Otolaryngol 35: 307-312.
- Bernier J, Domenge C, Ozsahin M, Matuszewska K, Lefèbvre JL, et al. (2004) Postoperative irradiation with or without concomitant chemotherapy for locallyadvancedhead and neck cancer.N Engl J Med 350: 1945-1952.
- Furness S, Glenny AM, Worthington HV, Pavitt S, Oliver S, et al. (2012) Interventions for the treatment of oral cavity and oropharyngeal cancer: chemotherapy. Cochrane DatabaseSystRev4: CD006386
- Kies MS, Boatright DH, Li G, Blumenschein G, El-Naggar AK, et al. (2012) Phase II trial of induction chemotherapyfollowed by surgery for squamouscellcarcinoma of the oral tongue in youngadults.Head Neck 34: 1255-1262.
- Licitra L, Grandi C, Guzzo M, Mariani L, Lo Vullo S, et al. (2003) Primarychemotherapy in resectable oral cavitysquamouscell cancer: arandomizedcontrolled trial.J Clin Oncol 21: 327-333.
- Haddad R, O’Neill A, Rabinowits G, Tishler R, Khuri F, et al. (2013) Induction chemotherapyfollowed by concurrent chemoradiotherapy (sequentialchemoradiotherapy) versus concurrent chemoradiotherapyalone in locallyadvancedhead and neck cancer (PARADIGM): arandomised phase 3 trial. Lancet Oncol14: 257-264.
- Malicki J (2012) The importance of accuratetreatment planning, delivery, and dose verification.RepPractOncolRadiother 17: 63-65.
- Chen AM, Zahra T, Daly ME, Farwell DG, Luu Q, (2015) et al. Definitive radiation therapywithoutchemotherapy for human papillomavirus-positive head and neck cancer. Head Neck 35: 1652-6.
Relevant Topics
- Blepharoplasty
- Bone Anchored Hearing Aids
- Chemical peel
- Cleft Surgery
- Congenital Craniofacial Malformations
- Cosmetic Facial Surgery
- Craniofacial Surgery
- Dental Orofacial Surgery
- Dentoalveolar Surgery
- Head and Neck Reconstruction
- Injectable Cosmetic Treatments
- Lip Reconstruction
- Mandibular Nerve Surgery
- Maxfax Surgery
- Maxillofacial Surgery
- Neck Liposuction
- Oral and Maxillofacial Surgery
- Oral Surgery Surgeon
- Orofacial Surgery Braces
- Pediatric Maxillofacial Surgery
- Rhytidectomy
- Sleep Apnea Orofacial Surgery
- Temporomandibular Joint Disorders
- Upper Jaw Surgery
Recommended Journals
Article Tools
Article Usage
- Total views: 11232
- [From(publication date):
December-2015 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 10282
- PDF downloads : 950