Research Article Open Access
Osteopathia Striata with Concomitant Fibroblastic Osteosarcoma of the Femur. A Potential Malignant Risk?
Oana C. Rafael1*, Leonard Kahn1, Gerald Rosen2 and Mohamed Aziz11Pathology, North Shore LIJ - Hofstra School of Medicine, Lake Success, NY, USA
2Oncology, NYU Langone Medical Cente, New York, NY, USA
- *Corresponding Author:
- Oana C. Rafael
Hofstra North Shore-LIJ School of Medicine 6 Ohio Drive (Suite 202) Lake Success, NY 11042, USA
Tel: 516-304-7209
Fax: 516-304-7269
E-mail: orafael@nshs.edu
Received Date: December 18, 2015; Accepted Date: December 29, 2015; Published Date: December 31, 2015
Citation: Rafael OC, Kahn L, Rosen G, Aziz M (2015) Osteopathia Striata with Concomitant Fibroblastic Osteosarcoma of the Femur. A Potential Malignant Risk? J Orthop Oncol 1:104. doi:10.4172/2472-016X.1000104
Copyright: © 2015 Rafael OC, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Orthopedic Oncology
Abstract
We report a case of a 33-year old female with an unusual presentation of high-grade osteosarcoma superimposed on osteopathia striata. Few cases of malignancy arising in sclerosing bone dysplasia have been reported in literature. Of the few reported ones, osteosarcoma was associated with melorheostosis in two cases, with osteopoikilosis in the one case, and with combined melorheostosis and osteopathia striata in one case. To the best of our knowledge the current case is the first one of a high-grade osteosarcoma arising from isolated osteopathia striata, not combined with other forms of sclerosing bone dysplasia.
Introduction
Osteopathia striata is an uncommon sclerosing bone dysplasia that remains mostly asymptomatic. First described by Voorhoeve in 1924 [1], it is characterized by linear streaks of altered bone density in the metaphyses and diaphyses of long bones, pelvis, and scapulae, thought to arise from disturbances in the endochondral bone formation. Initially thought to be an autosomal dominant disorder, recent molecular analysis confirmed an X-linked dominant inheritance, with germline mutations of the WTX gene, causing osteopathia striata congenita with cranial sclerosis [2]. The radiologic findings of osteopathia striata are characteristic, suggesting the diagnosis; however, the molecular analysis can confirm it .
Here we report an unusual case of high-grade osteosarcoma likely arising from osteopathia striata. We review the literature and attempt to clarify questions of potential malignant risk associated with sclerosing bone dysplasia. To our knowledge, only one case of osteosarcoma arising in a background of osteopathia striata combined with melorheostosis has been reported in literature, but none of osteosarcoma arising from isolated osteopathia striata.
Case Report
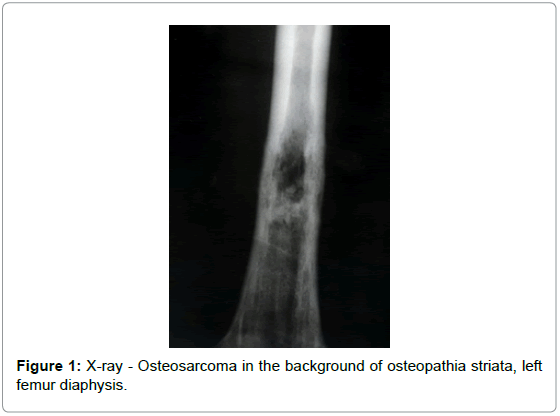
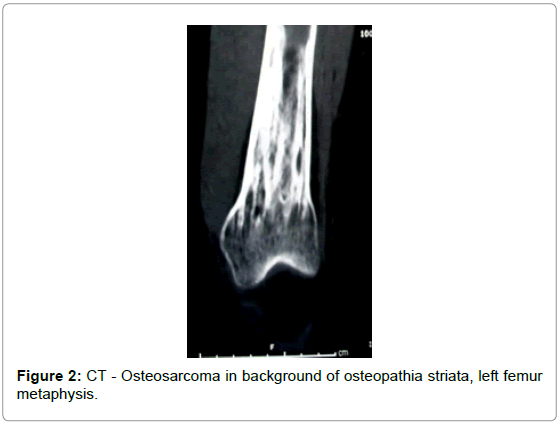
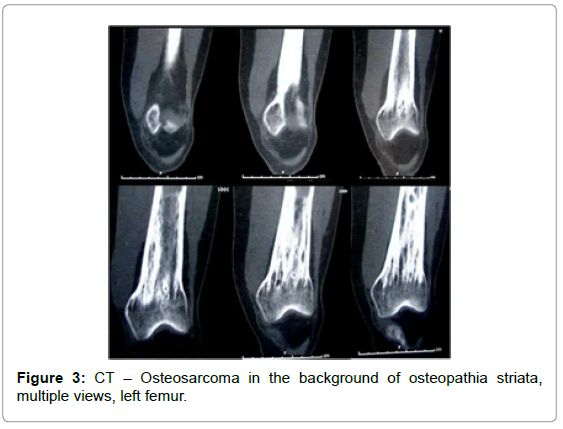
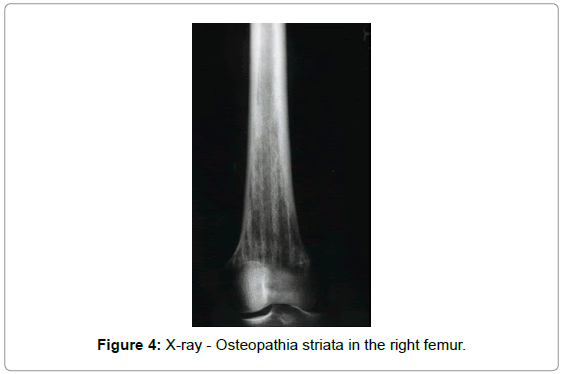
A 33-year-old woman presented with pain in the left thigh. Imaging revealed a diaphyseal soft tissue mass superimposed on a previously undetected benign sclerotic condition of the left femur, in the background of sclerosis (Figure 1). Endosteal scalloping was present in the femoral diaphysis, suggesting a slowly growing process, possibly a malignant transformation taking place in an otherwise benign bone condition. The distal femoral metaphysis and the proximal tibia showed radiographic changes consistent with osteopathia striata (Figures 2 and 3). Radiographic characteristics consistent with osteopathia striata were also appreciated in the patient’s contralateral lower extremity (right femur, tibia, and fibula - Figure 4). Abnormality in the left ileosacral region was also noted.
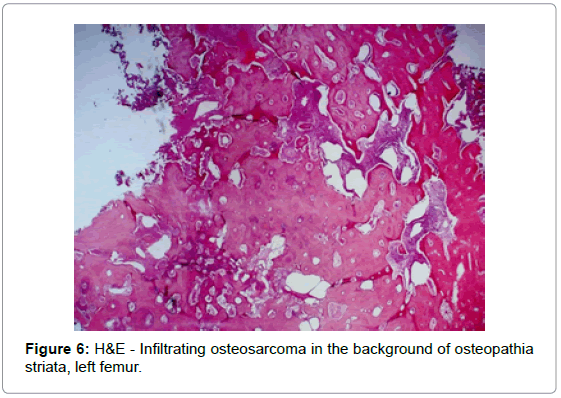
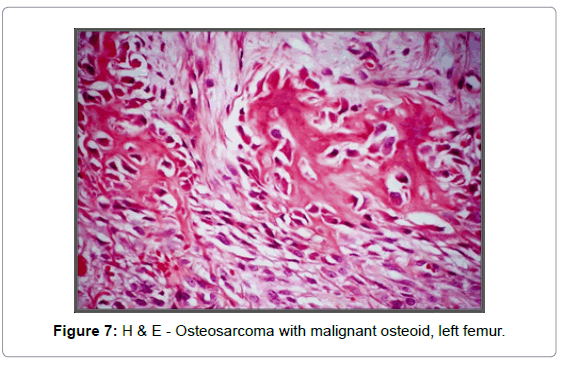
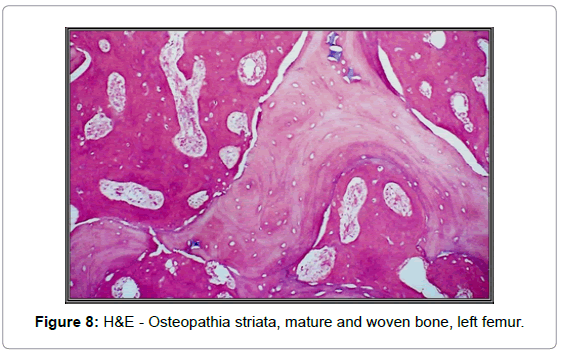
A needle biopsy of the diaphyseal soft tissue mass indicated malignancy; an 8-cm mass was removed during a subsequent extraarticular surgery with diaphyseal allograft placement (Figure 5). Decalcified sections of the tumor with bone revealed abundant malignant osteoid formation in a high-grade osteosarcoma of the femoral diaphysis, with prominent fibroblastic features, in a background of extensive sclerosing bone dysplasia, prominent cement lines, and focal marrow fibrosis, consistent with osteopathia striata (Figures 6-8). Areas of woven bone were also present on polarized light examination (Figure 9). Many areas of osteosarcoma displayed features morphologically indistinguishable from leiomyosarcoma. Immunohistochemical markers were negative for desmin, actin, CD- 34, S-100, and wide spectrum keratins. The soft tissue portion of the tumor showed foci of malignant osteoid formation.
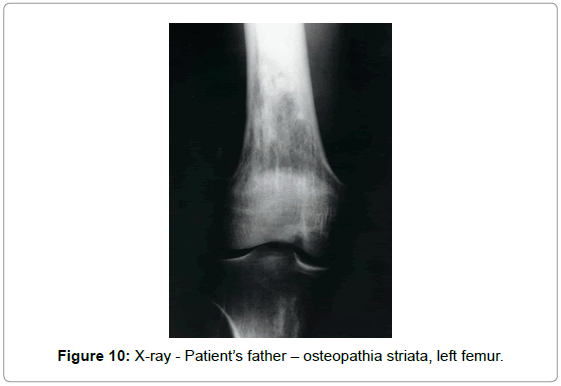
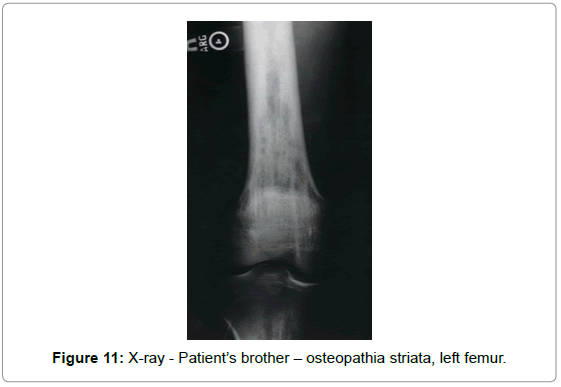
Postoperative imaging showed characteristics of osteopathia striata in the residual distal femoral and proximal tibial metaphyses. Radiographs in four other family members (father, mother, brother and daughter) showed changes consistent with osteopathia striata in father and brother (Figures 10 and 11).
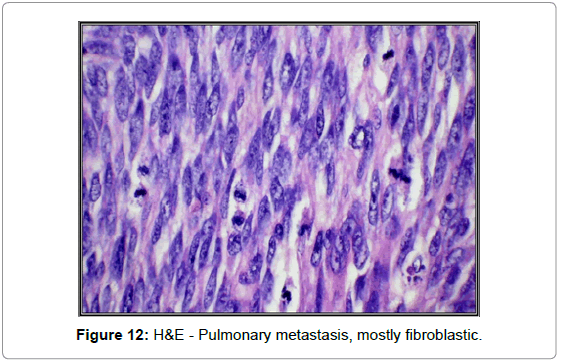
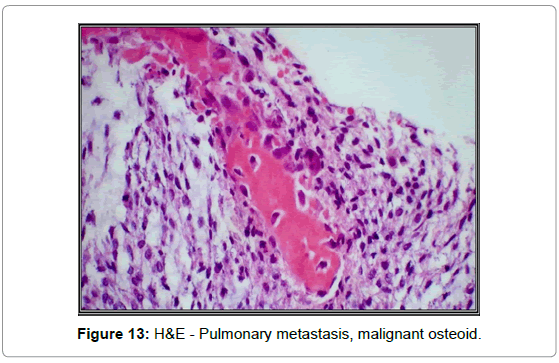
Patient underwent post-operative chemotherapy; however, six months after the treatment initiation a 6-cm mass was found in the left upper lobe of the lung with pleural seeding. Biopsies of the lung nodule, left chest wall, pericardium, and pleura showed metastatic high-grade spindle/pleomorphic sarcoma with focal malignant osteoid formation, all histomorphologically similar to the original femoral osteosarcoma (Figures 12 and 13).
The patient succumbed to disease nine months after the initial diagnosis.
Discussion
Osteopathia striata is a rare sclerosing bone dysplasia with characteristic radiographic features including longitudinal sclerotic striations of long bones. Sclerosing bone dysplasia comprises of a unique set of skeletal abnormalities with a wide range of radiologic, clinical, and genetic characteristics. The hereditary dysplasia includes osteopetrosis, pyknodysostosis (Maroteaux-Lamy disease), osteopoikilosis, osteopathia striata (Voorhoeve disease), progressive diaphyseal dysplasia (Camurati-Engelmann disease), hereditary multiple diaphyseal sclerosis (Ribbing disease), and hyperostosis corticalis generalisata (endosteal hyperostoses). Each disorder represents disruption in the bone ossification pathway. Some of these entities have similar genetic pathways, possibly representing phenotypic variants of the same disease. The nonhereditary dysplasia includes intramedullary osteosclerosis, melorheostosis (Leri disease) and overlapping syndromes [3].
Osteopathia striata is viewed as presence of disturbances in development associated with the process of enchondral bone formation. Although referred to as an autosomal dominant, some studies suggested an X-linked inheritance. Most cases were reported in association with cranial sclerosis, which was lacking in our patient. Osteopathia striata is often a marker of other disorders, particularly associated with focal dermal hypoplasia (Goltz-Gorlin syndrome or Goltz syndrome) [4].
More recently, an association with cranial sclerosis with and without cranial nerve dysfunction has been described [5]. Males with osteopathia striata with cranial sclerosis show mutations of the AMER1 gene located on the long arm of the X chromosome; they don’t usually survive and the survival is associated with various internal organs malformations [6]. Other clinical associations include skin abnormalities, mucosal papillomas, eye, renal, and dental anomalies. Therapy is mainly symptomatic, directed at relieving pain.
To the best of our knowledge the current case is the first one of a high-grade osteosarcoma arising from isolated osteopathia striata, not combined with other forms of sclerosing bone dysplasia. Few cases of malignancy arising in sclerosing bone dysplasia have been reported in literature. Of the few reported ones, osteosarcoma was associated with melorheostosis in two cases [7,8], with osteopoikilosis in the third case [9], and with combined melorheostosis and osteopathia striata in the fourth case [10].
Our case illustrates an unusual concurrent osteopathia striata and osteosarcoma in a female, emphasizing the various clinical associations of this disorder. When osteopathia striata is diagnosed, other abnormalities such as cranial osteosclerosis and internal anomalies should be looked for. In addition, family members should be screened for the presence of this skeletal abnormality, as demonstrated in our case. A close monitoring might be beneficial for patients since osteosarcoma might develop. With more cases of simultaneous osteopathia striata and osteosarcoma to be reported in the future, a better understanding of the optimal follow-up and management in these patients will emerge.
References
- Voorhoeve N (1924) L'imageradiologique non encore decrited'uneanomalie du squelette. Ses rapports avec la dyschondroplasie et l'osteopathiacondensansdisseminata. ActaRadiol 3: 407-427.
- Jenkins ZA, van Kogelenberg M, Morgan T, Jeffs A, Fukuzawa R, et al. (2009) Germline mutations in WTX cause a sclerosing skeletal dysplasia but do not predispose to tumorigenesis. Nature Genet 41: 95-100.
- Böstman OM, Holmström T, Riska EB (1987) Osteosarcoma arising in a melorheostotic femur. A case report. J Bone Joint Surg Am 69: 1232-1237.
- Murphy M, Kearns S, Cavanagh M, O’Connell D, Hurson B (2003) Occurrence of osteosarcoma in a melorheostotic femur. Ir Med J 96: 55-56.
- Mindell ER, Northup CS, Douglass Jr HO (1978) Osteosarcoma associated with osteopoikilosis. J Bone Joint Surg Am 60: 406-408.
- Brennan DD, Bruzzi JF, Thakore H, O’Keane JC, Eustace S (2002) Osteosarcoma arising in a femur with melorheostosis and osteopathiastriata. Skeletal Radiol 31: 471-474.
- http://ghr.nlm.nih.gov/condition/focal-dermal-hypoplasia#synonyms Accessed December 2015.
- http://ghr.nlm.nih.gov/gene/AMER1 Accessed December 2015.
- Ward LM, Rauch F, Travers R, Roy M, Montes J, et al. (2004) Osteopathia striata with cranial sclerosis: clinical, radiological, and bone histological findings in an adolescent girl.Am J Med Genet A 129: 8-12.
- Ihde LL, Forrester DM, Gottsegen CJ, Masih S, Patel DB, et al. (2011) Sclerosing bone dysplasias: review and differentiation from other causes of osteosclerosis. RadioGraphics 31: 1865-1882.
Relevant Topics
- 3D Printing in Limb-Sparing Surgery
- Adamantinoma
- Aneurysmal Bone Cysts
- Chondrosarcoma
- Chordomas
- Cryosurgery
- Enchondroma
- Ewing’s Sarcoma
- Fibrous Dysplasia
- Giant Cell Tumor of Bone
- Immunotherapy for Osteosarcoma
- Liquid Biopsy in Orthopedic Oncology
- Malignant Osteoid
- Metastatic Bone Cancer
- Molecular Profiling of Bone Tumors
- Multilobular Tumour of Bone
- Orthopaedic Oncology
- Osteocartilaginous Exostosis
- Osteochondrodysplasia
- Osteoma
- Osteonecrosis
- Osteosarcoma
- Primary Bone Tumors
- Sarcoma
- Secondary Bone Tumours
- Targeted Therapy in Bone Sarcomas
- Tumours of Bone
Recommended Journals
Article Tools
Article Usage
- Total views: 12669
- [From(publication date):
December-2015 - Aug 18, 2025] - Breakdown by view type
- HTML page views : 11675
- PDF downloads : 994