Review Article Open Access
Pharmacology of Marijuana
Thersilla Oberbarnscheidt1* and Norman S Miller2
1Central Michigan University, Houghton Avenue, USA
2CEO of Health Advocates PLLC, East Lansing, MI, Clinical Professor of Psychiatry, Department of Psychiatry, Medical College of George, Augusta University, Augusta, Georgia, USA
- *Corresponding Author:
- Thersilla Oberbarnscheidt
Resident, Central Michigan University
Houghton Avenue, USA
E-mail: Thersilla.oberbarnscheidt@cmich.edu
Received date: November 21, 2016; Accepted date: December 02, 2016; Published date: December 09, 2016
Citation: Oberbarnscheidt T, Miller NS (2016) Pharmacology of Marijuana. J Addict Res Ther S11:012. doi:10.4172/2155-6105.1000S11-012
Copyright: © 2016 Oberbarnscheidt T, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Addiction Research & Therapy
Abstract
The following review of literature regarding the pharmacology of marijuana is intended to demonstrate its mental and physical pharmacological effects. "Marijuana" refers specifically to the dried leaves and flowering tops or "herbal cannabis”, the natural form of cannabis as derived from the plant Cannabis sativa. Another term for marijuana is the word cannabis or hemp.
Keywords
Marijuana; Toxic effects; Patient; Cannabis.
Introduction
Marijuana consists of more than 421 components and 60 pharmacologically active cannabinoids. The two best-described cannabinoids are THC and cannabidiol (CBD). Most of the other compounds are not yet understood and their mental and physical effects are unknown [1-3].
Marijuana is highly lipophilic which leads to its storage in adipose tissue, liver, muscle and spleen and redistributed into the users blood stream long after ingestion. Because of the persistence in the body, marijuana can cause highly potent mental, physical and toxic effects in the users that are hard to control or predict [2].
In addition, Marijuana causes dependence, tolerance and addiction. The attempt to discontinue its use causes withdrawal symptoms consisting of: anxiety, depression, decreased appetite, headaches, insomnia, irritability, muscle tension, nausea, nightmares and unpleasant vivid dreams [4,5].
Chemistry of Marijuana
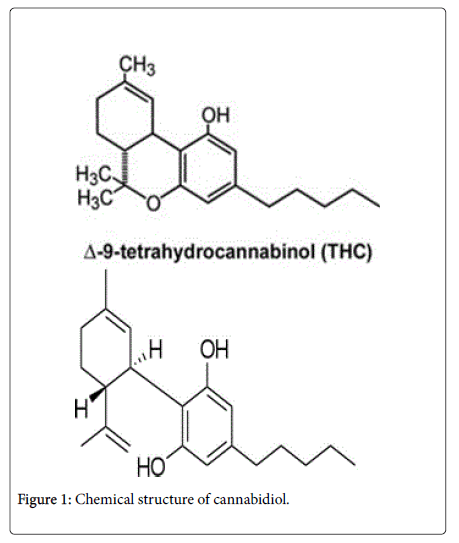
Marijuana, as used in the general population for smoked consumption, is an extract of the plant Cannabis sativa (Indian hemp). It consists of more than 421 components and more than 60 pharmacologically active cannabinoids. The two most well described cannabinoids in marijuana are delta9-tetrahydrocannabinol (THC) and cannabidiol (CBD) [1,3]. CBD does not produce any of the psychoactive responses and appears to block some of the effects of THC by acting as an antagonist at the cannabinoid receptors [2,6,7].
THC has a tri-cyclic 21-carbon structure without nitrogen and with 2 chiral centers in transfiguration. THC is volatile viscous oil with high lipid solubility and low water solubility and a pKa of 10.6. The primary active metabolite of THC is 11-hydroxy-delta-tetrahydrocannabinol (11-OH-THC) and the primary inactive metabolite is 11-nor-9- carboxy-delta-9-tetrahydrocannabinol (THC-COOH) [2] (Figure 1).
Marijuana Cultivation
Marijuana is a plant that grows best in temperatures of about 20°C or 68°F but the plant has a characteristic of being “flexible” meaning it can potentially grow in extreme conditions. The typical growing regions are anywhere within the 35 degrees of the equator. Typical growing regions include Mexico, Nepal, Northern India, many parts of Africa, Afghanistan, the United States and Australia. Marijuana can also be planted in homes and it is therefore possible to plant marijuana almost anywhere in the world. Seeds for Marijuana can be easily shipped by mail and are mostly from warmer climate countries with twelve hours or more of sunlight a day.
The duration of the growth of the plant depends of the conditions and can vary from 8 weeks to more than 7 month, the average growth being 3-4 month for indoor growers. After the harvest process the flower buds need to be dried for 3-10 days [8-10].
Natural Form
Marijuana is dried material from the Cannabis sativa plant, from leaves, stems and flower buds, and consists THC, Cannabidiol and other cannabinoids. “Medical marijuana” as defined by state laws is available in herbal form utilizing dried parts of the cannabis plant (only in some states), and essentially the same form that is sold illicitly. THC is the active ingredient sought after for its psychoactive effects [2,5].
In the last decades Marijuana has become significantly more potent and consequently, more dangerous. The average THC content in confiscated cannabis in 1990 was around 3.7 percent for marijuana and 7.5 percent for sinsemilla, which is higher potency marijuana from a specially tended female plant. Compared to these numbers, the contents changed towards the more potent form, with averaging 9.6 percent for marijuana and 16 percent for sinsemilla [11]. Also newer forms of marijuana are available with higher contents of THC that contain THC-rich hash oil. The average marijuana sold on streets currently contains 50 percent THC with samples exceeding 80 percent [12].
Synthetic Forms
A synthetic version of THC is available per prescription Marinol (Dronabinol), or as newer synthetic form of THC, Cesamet (Nabilone) [1,4,13]. Synthetic THC does not have the same effect as the “natural” cannabis. Natural cannabis cannot be synthesized yet due to its unknown compounds. The potent synthetic cannabinoids have different chemical qualities and are more water-soluble than THC and can therefore also be administered intravenously [2,14].
Another form, currently being tested in the US is Epidiolex, a CBDbased liquid medication that is tested for childhood epilepsies, Dravet syndrome and Lennox-Gastaut syndrome [4].
Semi-Synthetic Forms
A combination of THC and cannabidiol is only available outside of the US under the name Sativex (Nabiximols). It is available as a peppermint-flavoured spray. It is a so-called “whole plant” extract, includes THC and CBD at a ratio of 1:1. It stems directly from the cannabis plant and is not synthetic, yet it undergoes an extensive processing regimen [15]. THC and CBD represent approximately 70 percent of the product, with 5 percent from other cannabinoids and the remainder being terpenoids, flavonoids, sterols, alkanes, and other chemicals [15].
Mechanism of Action
Marijuana’s main sites of action are in the brain and the spinal cord. It binds to two types of G-protein-coupled receptors, CB1 and CB2. CB1 receptors are predominantly expressed in the brain and located in the basal ganglia, cerebellum, hippocampus, association cortices, spinal cord and peripheral nerves [4,7,16,17]. Through antagonistic effects on the CB1 receptor, marijuana induces its mental and behavioral effects. By acting on CB1 receptor, marijuana alters the user’s perceptions and mood and disturbs memory function and learning and leads to impaired judgment. Additional central effects of marijuana are a disruption of psychomotor behavior, psychosis and loss of time perception as well as impairment in movement coordination [5,7,18]. Because of these perceptual aberrations, marijuana was originally classified as an hallucinogen.
Marijuana over-activates the endo cannabinoid system, also known as "the body’s own cannabinoid system" causing addiction and a major part of the behavioral abnormalities [6,17,18].
The anti-emetic effects are mostly mediated through antagonism at the 5-HT3 receptors [1,19].
The CB2 receptors are mainly found in the peripheral tissues on cells in the immune system, the hematopoietic systems and in the spleen. These receptors may play a role in the immune-suppressive activity of cannabis [4,16,17].
Both cannabinoid receptors, CB1 and CB2, are G-protein coupled and become activated through inhibition of the adenylate-cyclase. The activation of these receptors cause an inhibition of the release of the neurotransmitters acetylcholine and glutamate while indirectly affecting y-aminobutyric acid, N-methyl-D-aspartate, opioid and serotonin receptors. The cannabinoid receptors are predominantly located presynaptic rather than postsynaptic which means that cannabinoids modulate the neurotransmitter releases [18].
Recent studies have shown that marijuana decreases the sensitivity to dopamine in the reward center in the brain, mainly the region in the mesolimbic dopamine system. Dopamine neurons are located in the midbrain and dopamine is the neurotransmitter responsible for the brain’s pleasure and reward center. The limbic system consists of the amygdala, the nucleus accumbens, the prefrontal cortex and the hippocampus. In addition to the pleasure and reward, the mesolimbic dopamine system is associated with the functions of movement, preservation, and compulsion (Table 1).
| Absorption | Peak concentration | Factors impacting absorption | Bioavailability |
|---|---|---|---|
| Quick Fast, rapid drug delivery to the brain | 22 min | Depth of inhalation, frequency of puffs, breath hold | Varies 2-56 percent Heavy users 23-27 percent Occasional users 10-14 percent |
Table 1: Inhalation/smoking [1,5,20].
Pharmacokinetics
Smoking marijuana has the highest addictive potential due to rapid and efficient drug delivery from the lungs to the brain [1,5,20].
A major fraction of THC is destroyed by pyrolysis, which causes the variance in systemic bioavailability between heavy and occasional users. More than 2000 compounds mostly unknown in their exact clinical structure and physical and mental effects are produced by pyrolysis during smoking of marijuana. These chemicals inc lude different classes of chemicals including nitrogenous compounds, amino acids, hydrocarbons, sugar, terpenes and simple fatty acids [2] (Table 2).
| Absorption | Peak concentration | Factors impacting absorption | Bioavailability |
|---|---|---|---|
| Slow | 1-2 h, can be delayed to up to 8 h | Degradation of the drug in the stomach and First-pass | Ranges from 10-20 percent |
Table 2: Oral route [1,4,5,21].
Compared to inhalation, the onset of effects is delayed in oral use, peak concentrations are lower but the duration of pharmacokinetic effects are extended with a delayed return to baseline [1,21]. First pass metabolism means that only a fraction of the marijuana ingested actually becomes available in the blood stream [4,21].
The suppository form of natural marijuana as well as synthetic THC is available as an ovular capsule that can be inserted vaginally or rectally. The capsules are typically about an inch long and are made from a mixture of coconut oil infused with marijuana or FECO (Full Extract Cannabis Oil)-infused cocoa butter. Once inserted, the capsule dissolves and is absorbed into the bloodstream through the thin lining of the intestinal wall [1] (Table 3).
| Absorption | Peak concentration | Factors impacting absorption | Bioavailability |
|---|---|---|---|
| Fast | 30 min | High first past metabolism | Similar to oral route |
Table 3: Oralmucosal/sublingual [4,21].
In transcutaneous absorption, the transport across the skin layers is limited by the hydrophobic qualities of cannabis, making it the ratelimiting step. A transcutaneous carrier selected from the group consisting of water, short carbon chain alcohols, dimethysulfoxide, polyethylene glycol, polypropylene glycol, glycerin, mineral oil and mixtures thereof [4,20].
The delivery to the brain when administered transcutaneously is much slower compared to smoking. Steady state plasma concentrations were found to be maintained for at least 48 h [1] (Table 4).
| Absorption | Peak concentration | Factors impacting absorption | Bioavailability |
|---|---|---|---|
| Fast | 15 min | Low first past metabolism | Twice of oral route |
Table 4: Rectal [1].
Metabolism of Cannabis
THC is metabolized in the liver by microsomal hydroxylation and oxidation via CP450 enzymes. The hydroxylation of THC through CP450 enzymes leads to the production of the equipotent active metabolite 11-OH-THC. Cytochromes involved in the oxidation of THC are CYP 450 2C9, 2C19 and 3A4. More than 100 THC metabolites including di- and trihydroxy compounds, ketones, aldehydes, and carboxylic acids, have been identified. The oxidation of the psychoactive 11-OH-THC produces the inactive metabolite THC-COOH, which is with its conjugates the major end product of biotransformation. Extra-hepatic sites in the brain, intestine and lung might contribute to the metabolism of cannabis [1,2] (Table 5).
| Absorption | Peak concentration | Factors impacting absorption | Bioavailability |
|---|---|---|---|
| Slow | 2 h Steady state plasma concentrations were found to be maintained for at least 48 h | Transport across the skin layers No first-pass metabolism | 10 percent |
Table 5: Transcutaneous [4].
Marijuana has been shown to affect the pharmacokinetics of other drugs in several ways through inhibition of the CP450 enzyme. It mediates the absorption of other drugs and may also slow down the absorption of others and to enhance or delay the penetration of drugs into the brain. Marijuana interacts through CP 450 with medications levels for example warfarin and theophylline and is linked to toxic levels or supra-therapeutic INR values. Also antidepressants for example SSRIs inhibit the hepatic CP450 enzymes. Prozac and Paxil extend the availability of marijuana in the serum due to competition with the enzyme [22].
Distribution
It is essential to know the pharmacokinetic effects of marijuana to understand the onset and magnitude of its effects as well as the toxicity and extended potency. In addition, marijuana has many documented acute and chronic toxic effects on brain and behaviour [22,23].
Central to Marijuana’s toxicity is that it is a highly lipophilic substance that is taken up by tissues that are highly perfused in the blood circulation, such as heart, lung, brain, muscle and liver as well as adipose tissues. With prolonged marijuana exposure, fatty acid conjugates of THC and 11-OH-THC are formed, increasing the stability of these compounds and allowing even its extended storage in the tissues. Studies with radioactive tracers for THC have shown a large volume distribution of the active form of THC and its slow elimination from body stores long after use for continued pharmacological effects. The half-life of infrequent users is 1.3 days and for frequent user it is 5 to 13 days [1,2,24].
Therefore the pharmacological effects of marijuana and also its toxic effects can persist for a prolonged period of time after the last ingestion or exposure, which makes it highly unpredictable. Also the effects of marijuana increase in potency in frequent and long term users since cannabis release from storage in the tissues to be added to the newly ingested amount of marijuana [25].
The pharmacokinetics of marijuana is distinct from other addictive substances, for example alcohol and opioids, which have a much shorter half-life and do not have the quality to be stored and recirculate into the blood system. Marijuana’s toxic effects persist and are much more unpredictable [26].
Marijuana transfer through placenta and breast milk
The psychoactive ingredient of marijuana (THC) is reported to transfer through the placenta vessels to the fetus or embryo. Due to the lipophilic qualities of marijuana it accumulates in the milk. An analysis of breast milk from chronic heavy marijuana users indicated an eight-fold concentration in milk compared to the mother’s plasma level [1] (Table 6).
| Overall Clearance rate | Route of excretion | Conjugation | Primary metabolites |
|---|---|---|---|
| Woman 11.8+-3 L/h | Feces 65% | Hepatic: water-soluble metabolite after conjugation with glucuronic acid | Feces: 11-OH-THC |
| Men 14.9 +-3.7 L/h | Urine 20% | Renal: Tubular reabsorption and low renal excretion of the unchanged drug | Urine: THC-COOH |
Table 6: Excretion of marijuana [1,41,42].
Therapeutic Effects of Marijuana
“Medical marijuana” is marijuana in its natural form, and is claimed to have therapeutic effects for various medical indications and conditions, mainly through legislative acclimation. The medical use of the herbal form of cannabis (marijuana) has not been approved by any regulatory agency worldwide [6].
Its natural forms have not been approved for any conditions by the FDA, only synthetic forms have. There are two different synthetic forms on the market that are FDA approved. Those are dronabinol (Marinol) and nabilone (Cesamet). Those are approved for the indications as an appetite enhancer in AIDS patients and for nausea in patients undergoing chemotherapy [6,22].
Toxic Effects of Marijuana
In contrast to the undocumented and inconsistently reported clinical benefits, the toxic effects of marijuana are consistently noted and demonstrated in studies [1,2,4,22].
Mental and behavioural effects
As classified as a hallucinogen, Marijuana impairs the users coordination, perception regarding time and surroundings, comprehension of information and cognition. Some studies suggest these cognitive changes are permanent [22,23].
Marijuana causes the user to be impaired in their alertness and judgment. Users become “stoned” and can develop psychotic symptoms consisting of hallucinations, paranoia and delusions [4,26-28]. Even a single dose of cannabis can lead to substanceinduced psychotic disorder. In patients with pre-existing schizophrenia, it leads to higher rates of readmissions and in bipolar disease it can precipitate a manic episode with or without pre-existing Bipolar Disease [4,29].
These psychotic reactions increase the likelihood of violent behaviors and impairs the person in properly operate machinery. Under the influence of cannabis, higher rates of traffic accidents and deaths are reported [2,5,6].
Furthermore, marijuana frequently causes and induces anxiety and depression in the users, which might be brief panic reactions but long lasting psychiatric symptomatology is described [30-33].
In the adolescents, the use of marijuana is associated with induced ADHD and causes higher dropout rates in schools and well as an increased likelihood to use other illicit substances as well as licit substances like alcohol and opiates [2,4,6,23].
Marijuana users overall have a reduced quality of life compared to non-users. In users with pre-existing mental conditions for example anxiety or depression, the decline in quality of life is even more severe [34]. Marijuana's negative effects on attention, memory, and learning can last for days or weeks after the acute effects of the drug wear off. Consequently, someone who smokes marijuana daily may be functioning at a reduced intellectual level most or all of the time. Several studies have also linked heavy marijuana use to lower income, greater welfare dependence, unemployment, criminal behavior and lower life satisfaction [32,35].
Physical effects
Marijuana causes dose dependent tachycardia and increases the cardiac labor. The risk of suffering an acute cardiac event is increased 5 fold for previously healthy individuals and even higher for users with pre-existing cardiac conditions [5]. Higher levels of carboxyhemoglobulin in the circulating blood cause hypoxia and ischemia in organs. Marijuana also causes a reduced blood flow in the brain by increasing the cerebrovascular resistance and systolic velocity significantly compared to non-users [5].
In the periphery, the parasympathomimetic tone in the user’s body is decreased by marijuana. The dilation of blood vessels leads potentially to othostatic hyotension and subsequently to syncopes [4,5].
The smoke of marijuana causes symptoms of COPD and users wheeze and frequently cough. The sputum production is increased similar to users inhaling tobacco [4,36].
Marijuana also causes negative effects in pregnancy. It alters the neurological development in the embryo in utero. Babies born from mothers who consumed cannabis have a higher pitch cry and tremble more. Cannabis also reaches the new-born through transmission in the breast milk [5].
In addition, the use of marijuana is linked to the development of certain cancers. Gliomas, prostate and cervical cancers are described. In pregnant women increased incidents of leukemia, rhabdomyosarcomas and astrocytomas are linked to cannabis use [4].
Marijuana also influences reproductive organs negatively. A study from Denmark found significant lower sperm concentrations in marijuana smokers compared to non-smokers [37,38]. Another study found that THC suppresses the adrenal cortical hormones prolactin, thyroid hormones and growth hormones [4].
Marijuana Addiction/Tolerance/Dependence
Marijuana is classified in the US as a Schedule I drug which, like heroin, contains substances with a high potential for abuse, with no current accepted medical use and a lack of accepted safety for medical use [1].
Marijuana affects the same reward systems in the brain as alcohol, cocaine and opioids in two different ways [2]. Marijuana induces the release of endorphins in the brain from the nucleus accumbens and the orbito-frontal cortex, which produce the feeling of pleasure and reward. Endorphins are hormones that are naturally produced in the brain that have an opioid like effect. In addition, Marijuana acts as a dopamine agonist in the brain, stimulating reinforcement regions in the meso-telencephalic dopamine (DA) system [26,39].
Due to the developing tolerance, greater amount of cannabis are required over time to experience the same effect. Tolerance to cannabis occurs in relation to mood, psychomotor performance, sleep, arterial pressure, body temperature and antiemetic properties [2,40].
In addictive use, attempts are made to cut back on their use and a great amount of time is spent to obtain the drug. During periods of abstinence, the user is experiencing cravings or a strong desire to use cannabis [4,26,40,41].
With discontinuation of the use or in between doses, withdrawal symptoms occur. Symptoms of marijuana withdrawal are consistent of: anxiety, depression, decreased appetite, headaches, insomnia, irritability, muscle tension, nausea, nightmares and unpleasant vivid dreams [4].
In earlier studies it was described that symptoms of withdrawal start after 4 h and returning to baseline after 4-7 days. In the recent studies the withdrawal typically occurred between 1-3 days and peaks between 2-6 days. Most intoxicating and withdrawal effects were lasting up to 4-14 days depending on the frequency of use, dose, and route of administration [1].
This long lasting effect of marijuana differentiates the drug from other substances, e.g. alcohol which are eliminated much faster with shorter periods of intoxication and withdrawal [2,26].
Detection of Marijuana
The detection of cannabinoids is necessary for many different purposes: impaired driving investigations, crime investigations, pharmacokinetics, drug treatment or workplace drug testing. Marijuana can be detected in body fluids following exposure through active/passive inhalation as well as oral consumption or transdermal or rectal application and through exposure through breastfeeding [1,2,5].
Marijuana can be detected in saliva, blood, urine, hair and nails. In the blood, 95-99 percent of the THC and THC-COOH are found in the plasma fraction, bound to lipoproteins. In order to detect marijuana, multi-step extractions to separate marijuana from endogenous lipids and proteins are required because of its lipophilic quality. In addition, marijuana has a high affinity to glass or plastic containers [1,24,40,41].
Various laboratory techniques are available for screening as well as confirmation tests for detection of marijuana. The preferred screening test or the detection of marijuana is the Immunoassay. Test kits are available as urine dip tests that can be used with small amount of urine and results read immediately. Screening tests are for instant detection and not very costly. False positive results occur through structurally related drugs or artefacts through pH, detergents or surfactants. Examples for medications that can cause a false positive test result for marijuana are: Ibuprofen, Naproxen, Ketoprofen, Promethazine, Pantoprazole, Riboflavin. Other substances that can create false positive results are Baby Soaps and Shampoos [1].
In case a confirmatory test is desired, the most frequently used method to detect marijuana is Chromatography-Mass Spectrometry [2]. These tests generally require the substance to be sent out and take more time and are also more expensive. Levels of marijuana can be measured in the serum and in the urine per Quantitative Liquid Chromatography-Tandem Mass Spectrometry. The Substance Abuse and Mental Health Services Administration set the lower level threshold for the detection of cannabinoids with a cut-off of 50 ng/ml. That level is consistent with recent or heavy use [1,42].
Urine
The preferred material for analysis for marijuana is urine since it is easy to collect and higher levels and longer detection times. Due to marijuana’s particular pharmacological dynamics, being stored and redistributed into the system, it can be detected very long after exposure or last ingestion for up to several months. The longest reported case, a user had used marijuana heavily for more than ten years and his urine was positive at a concentration >20 ng/ml (by immunoassay) 67 days after last use [1,4,24,39,43].
Oral fluid testing
Oral fluid testing is the best test for determining cases of driving under the influence of marijuana as well as workplace testing and drug treatment. The oral mucosa is exposed to high concentrations of THC during smoking. Several hours after exposure, the oral mucosa serves as a depot for release of THC into the oral fluid (saliva). Compared to urine, the detection time in oral fluids is shorter which makes it more indicative of recent marijuana use. THC can be detected in the saliva for up to 24 h after use by radioimmunoassay [1,4,5,21]
Sweat
Sweat testing is mostly used in criminal justice, workplace testing as well as monitoring for drug treatment and lastly clinical studies. The main method for detection of marijuana in sweat is radioimmunoassay [1].
Hair
Marijuana accumulates into the hair in different ways. Hair tests generally take the most recent 1.5 inches of growth and use those for testing. This method provides a detection period of approximately 90 days [16].
Serum
THC can be detected in the plasma immediately after the first cigarette puff [1]. Marijuana is detectable in the blood for approximately 2-3 days after use in an infrequent user. Frequent marijuana use can be detected in the blood for approximately 2 weeks [1].
Conclusion
Marijuana is not a practicable or safe drug for recreational or therapeutic use due to its pharmacology. The exact contents of marijuana are yet not known with it’s over 421 components and 60 pharmacologically active cannabinoids. THC is thought to be the only psychoactive ingredient but further research is needed to determine the role and effect of the cannabinoids [1,2,4].
Marijuana has a high addiction potential, impairing the users judgment and leading to hazardous situations when used despite the negative consequences in users personal life, occupation and lastly health. Marijuana causes tolerance, dependence and withdrawal in between uses. Withdrawal symptoms are very unpleasant and consistent of: anxiety, depression, decreased appetite, headaches, insomnia, irritability, muscle tension, nausea, nightmares and unpleasant vivid dreams [4].
Marijuana is consumed for subjective reasons driven by compulsive behavior to continue the use of the drug. The moment of euphoria is short in nature and followed by the feeling of being “stoned”. Users experience distortion of time and location followed by paranoia, anxiety and other hallucinations or delusions. Marijuana users have a decreased quality of life and are more likely to suffer from psychiatric conditions like depression and anxiety [16,30,34].
In the case of “medical marijuana” the toxic effects are so severe that if they would be explained and understood, potential patients (not seeking marijuana) would ask their physician for an alternative treatment. The knowledge of the fact that marijuana is carcinogenic and toxic during pregnancy and nursing period might stop certain users. Further, marijuana is not FDA approved and classified as s Schedule I medication with no proven medical benefit [6].
Marijuana has a long half-life and, due to its lipophilic quality, persists in the body for a long time following its last exposure and makes its effects dangerous to predict in terms of its toxicity. Users walk around “impaired”. This pharmacological quality differentiates marijuana from other drugs for example opioids and alcohol, which are cleared out of the users system in a shorter, specific time window and do not accumulate and have more predictable effects [1].
References
- Huestis MA (2007) Human cannabinoid pharmacokinetics. Chem Biodives 4: 1770-1804.
- Sharma P, Murthy P, Bharath MM (2012) Chemistry, metabolism and toxicology of cannabis: Clinical implications. Iran J Psychiatry 7: 149-156.
- Grotenhermen F, Müller-Vahl K (2012) The therapeutic potential of cannabis and cannabinoids. Dtsch Arztebl Int 109: 495-501.
- Lamarine RJ (2012) Marijuana: Modern medical chimaera. J Drug Educ 42: 1-11.
- Grotenhermen F (2007) The toxicology of cannabis and cannabis prohibition. Chem Biodivers 4: 1744-1769.
- Hill KP (2015) Medical marijuana for treatment of chronic pain and other medical and psychiatric problems: A Clinical Review. JAMA 313: 2474-2483.
- Felder CC, Joyce KE, Briley EM, Mansouri J, Mackie K, et al. (1995) Comparison of the pharmacology and signal transduction of the human cannabinoid CB1 and CB2 receptors. Mol Pharmacol 48: 443-450.
- Green G (2003) The cannabis grow bible: The definitive guide to growing marijuana for recreational and medical use green candy: 47.
- Hillig KW, Mahlberg PG (2004) A chemotaxonomic analysis of cannabinoid variation in Cannabis (Cannabaceae). Am J Bot 91: 966-975.
- Frank M, Rosenthal E (1998) The Marijuana Grower's Guide.
- McLaren J, Swift W, Dillon P, Allsop S (2008) Cannabis potency and contamination: A review of the literature. Addiction 103: 1100-1109.
- National Institute on Drug Abuse (2015) Is Marijuana addictive?.
- Russo EB, Hohmann AG (2013) Role of cannabinoids in pain management. In: Deer T, Gordin V, editors. Comprehensive treatment of chronic pain by medical, interventional and behavioral approaches. New York: Springer: 181-197.
- Agurell S, Halldin M, Lindgren JE, Ohlsson A, Widman M, et al. (1986) Pharmacokinetics and metabolism of delta 1-tetrahydrocannabinol and other cannabinoids with emphasis on man. Pharmacol Rev 38: 21-43.
- Jensen B, Chen J, Furnish T, Wallace M (2015) Medical marijuana and chronic pain: A review of basic science and clinical evidence. Curr Pain Headache Rep 19: 50.
- Hosking RD, Zajicek JP (2008) Therapeutic potential of cannabis in pain medicine. Br J Anaesth 101: 59-68.
- Pertwee RG (2008) The diverse CB1 and CB2 receptor pharmacology of three plant cannabinoids: Delta9-tetrahydrocannabinol, cannabidiol and delta9-tetrahydrocannabivarin. Br J Pharmacol 153: 199-215.
- Iversen L (2003) Cannabis and the brain. Brain 126: 1252-1270.
- Limebeer CL, Rock EM, Mechoulam R, Parker LA (2012) The anti-nausea effects of CB1 agonists are mediated by an action at the visceral insular cortex. Br J Pharmacol 167: 1126-1136.
- Strougo A, Zuurman L, Roy C, Pinquier JL, van Gerven JM, et al. (2008) Modelling of the concentration effect relationship of THC on central nervous system parameters and heart rate insight into its mechanisms of action and a tool for clinical research and development of cannabinoids. J Psychopharmacol 22: 717-726.
- Borgelt LM, Franson KL, Nussbaum AM, Wang GS (2013) The pharmacologic and clinical effects of medical cannabis. Pharmacotherapy 33: 195-209.
- Thompson AE (2015) Jama patient page. Medical Marijuana. JAMA 313: 2508.
- Crean RD, Crane NA, Mason BJ (2011) An evidence based review of acute and long-term effects of cannabis use on executive cognitive functions. J Addict Med 5: 1-8.
- Dackis CA, Pottash AL, Annitto W, Gold MS (1982) Persistence of urinary marijuana levels after supervised abstinence. Am J Psychiatry 139: 1196-1198.
- Alexander S (2016) Therapeutic potential of cannabis-related drugs. Prog Neuropsychopharmacol Biol Psychiatry. 64: 157-166.
- Gold M, Miller NS (1992) Seeking drugs/alcohol and avoiding withdrawal: The neuroanatomy of drive states and the withdrawal. Psychiatric Annals: 430-435.
- Moore TH, Zammit S, Lingford-Hughes A, Barnes TR, Jones PB, et al. (2007) Cannabis use and risk of psychotic or affective mental health outcomes: A systematic review. Lancet 370: 319-328.
- Tramèr MR, Carroll D, Campbell FA, Reynolds DJ, Moore RA, et al. (2001) Cannabinoids for control of chemotherapy induced nausea and vomiting: Quantitative systematic review. BMJ 323: 16-21.
- Aspis I, Feingold D, Weiser M, Rehm J, Shoval G, et al. (2015) Cannabis use and mental health-related quality of life among individuals with depressive disorders. Psychiatry Res 230: 341-349.
- Aspis I (2015) Cannabis use and mental health-related quality of life among individuals with depressive disorders. Psychiatry Res 230: 341-349.
- Zvolensky MJ, Cougle JR, Johnson KA, Bonn-Miller MO, Bernstein A (2010) Marijuana use and panic psychopathology among a representative sample of adults. Exp Clin Psychopharmacol 18: 129-134.
- Meier MH, Caspi A, Ambler A, Harrington H, Houts R, et al. (2012) Persistent cannabis users show neuropsychological decline from childhood to midlife. Proc Natl Acad Sci U S A 109: E2657-2664.
- Grover S and Basu D (2004) Cannabis and psychopathology: Update 2004. Indian J Psychiatry 46: 299-309.
- Fergusson DM, Boden JM (2008) Cannabis use and later life outcomes. Addiction 103: 969-976.
- Brook JS, Lee JY, Finch SJ, Seltzer N, Brook DW (2013) Adult work commitment, financial stability and social environment as related to trajectories of marijuana use beginning in adolescence. Subst Abus 34: 298-305.
- Tetrault JM, Crothers K, Moore BA, Mehra R, Concato J, et al. (2007) Effects of marijuana smoking on pulmonary function and respiratory complications: A systematic review. Arch Intern Med 167: 221-228.
- Gundersen TD, Jorgensen N, Andersson AM, Bang AK, Nordkap L, et al. (2015) Association between use of marijuana and male reproductive hormones and semen quality: A study among 1,215 healthy young men. Am J Epidemiol: 135-138.
- Harclerode J (1984) Endocrine effects of marijuana in the male: Preclinical studies. NIDA Res Monogr 44: 46-64.
- Ellgren M, Spano SM, Hurd YL (2007) Adolescent cannabis exposure alters opiate intake and opioid limbic neuronal populations in adult rats. Neuropsychopharmacology 32: 607-615.
- Nocon A, Wittchen HU, Pfister H, Zimmermann P, Lieb R (2006) Dependence symptoms in young cannabis users? A prospective epidemiological study. J Psychiatr Res 40: 394-403.
- Lemberger L, Silberstein SD, Axelrod J, Kopin IJ (1970) Marihuana: Studies on the disposition and metabolism of delta-9-tetrahydrocannabinol in man. Science 170: 1320-1322.
- Hollister LE, Kanter SL (1980) Laboratory Verification of "heavy" and "light" users of cannabis. Drug Alcohol Depend 5: 151-152.
- The Substance Abuse and Mental Health Services Administration.
Relevant Topics
- Addiction Recovery
- Alcohol Addiction Treatment
- Alcohol Rehabilitation
- Amphetamine Addiction
- Amphetamine-Related Disorders
- Cocaine Addiction
- Cocaine-Related Disorders
- Computer Addiction Research
- Drug Addiction Treatment
- Drug Rehabilitation
- Facts About Alcoholism
- Food Addiction Research
- Heroin Addiction Treatment
- Holistic Addiction Treatment
- Hospital-Addiction Syndrome
- Morphine Addiction
- Munchausen Syndrome
- Neonatal Abstinence Syndrome
- Nutritional Suitability
- Opioid-Related Disorders
- Relapse prevention
- Substance-Related Disorders
Recommended Journals
Article Tools
Article Usage
- Total views: 219942
- [From(publication date):
specialissue-2017 - Aug 15, 2025] - Breakdown by view type
- HTML page views : 217246
- PDF downloads : 2696