Case Report Open Access
Physiotherapy Management of Peripheral Unilateral Isolated Hypoglossal Nerve Palsy in a 53 Year Old Woman: A Case Report
| Maduagwu Stanley M1*, Kaidal Amina2, Aremu Bukuola J1, Kodiya Aliyu M3, Adetoyeje Y Oyeyemi4, Adewale Oyeyemi L4, Jaiyeola Olabode A1 and Mungonu Mustapha1 |
|
| 1Department of Physiotherapy, University of Maiduguri Teaching Hospital, Nigeria | |
| 2Department of Physical and Health Education, University of Maiduguri, Nigeria | |
| 3Department of Ear, Nose and Throat, University of Maiduguri Teaching Hospital, Nigeria | |
| 4Department of Physiotherapy, University of Maiduguri, Nigeria | |
| Corresponding Author : | Maduagwu Stanley M Department of Physiotherapy University of Maiduguri Teaching Hospital Bama Road, Maiduguri, Borno State, Nigeria Tel: +2348034998207 E-mail: madusta@yahoo.com |
| Received February 21, 2014; Accepted July 14, 2014; Published July 16, 2014 | |
| Citation: Stanley MM, Amina K, Bukuola AJ, Aliyu KM, Oyeyemi AY, et al. (2014) Physiotherapy Management of Peripheral Unilateral Isolated Hypoglossal Nerve Palsy in a 53 Year Old Woman: A Case Report. J Nov Physiother 4:218. doi: 10.4172/2165-7025.1000218 | |
| Copyright: © 2014 Stanley MM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Novel Physiotherapies
Abstract
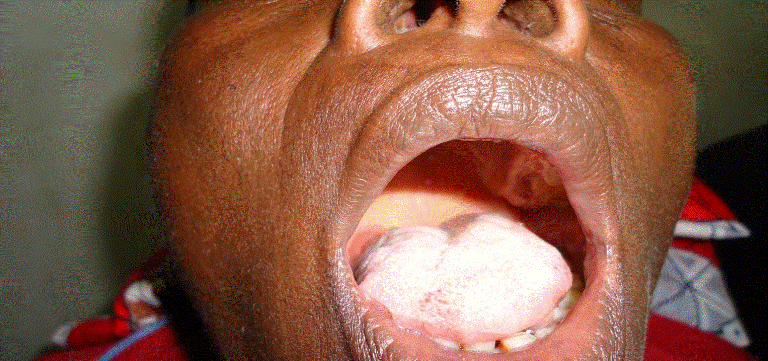
Hypoglossal nerve palsy is not common in literature, especially its physiotherapy assessment and management. We described a case of a 53 year old woman who presented clinically with right sided atrophy of the tongue, ipsilateral deviation and fasciculation, a speech defect, inability to swallow solids, and difficulty in swallowing fluid as a result of one year history of hypoglossal nerve palsy after a traditional uvulectomy. She was fully assessed and received physiotherapy management in the form of electrical stimulation and a home programme in combination with spiritual therapy. After 11 weeks of treatment there was improvement in terms of her initial clinical presentation.
Figures at a glance
 |
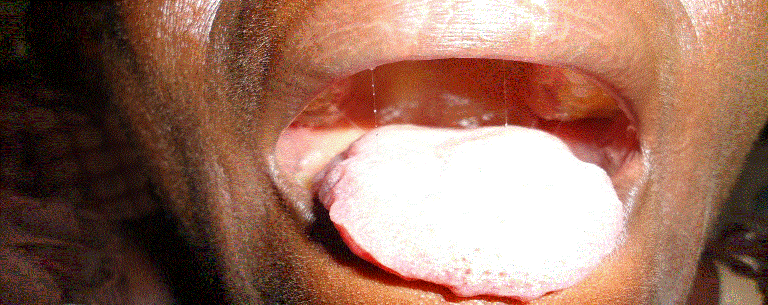 |
| Figure 1 | Figure 2 |
Relevant Topics
- Electrical stimulation
- High Intensity Exercise
- Muscle Movements
- Musculoskeletal Physical Therapy
- Musculoskeletal Physiotherapy
- Neurophysiotherapy
- Neuroplasticity
- Neuropsychiatric drugs
- Physical Activity
- Physical Fitness
- Physical Medicine
- Physical Therapy
- Precision Rehabilitation
- Scapular Mobilization
- Sleep Disorders
- Sports and Physical Activity
- Sports Physical Therapy
Recommended Journals
Article Tools
Article Usage
- Total views: 18960
- [From(publication date):
September-2014 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 14135
- PDF downloads : 4825
