Research Article Open Access
Prevalence on the Use of Traditional Medicine in Brunei Darussalam
| Nurolaini K1*, Wint Z1, Jaini NH2, Jaludin NH2, Hamid MA2 and Linda YYL2 | |
| 1Pengiran Anak Puteri Rashidah Sa'adatul Bolkiah Institute of Health Sciences, Universiti Brunei Darussalam, Brunei Darussalam | |
| 2Department of Pharmaceutical Services, Raja Isteri Pengiran Anak Saleha Hospital, Ministry of Health, Brunei Darussalam | |
| Corresponding Author : | Nurolaini K Deputy Dean (Academic, Research & Internationalisation) & Senior Lecturer Pengiran Anak Puteri Rashidah Sa'adatul Bolkiah Institute of Health Sciences Universiti Brunei Darussalam, Jalan Tungku Link Gadong, BE1410, Brunei Darussalam Tel: 2463001-2210 Fax: 6732461-081 E-mail: Nurolaini.kifli@ubd.edu.bn |
| Received March 17, 2014; Accepted May 14, 2014; Published May 18, 2014 | |
| Citation: Nurolaini K, Wint Z, Jaini NH, Jaludin NH, Hamid MA, Linda YYL (2014) Prevalence on the Use of Traditional Medicine in Brunei Darussalam. J Homeop Ayurv Med 3:155. doi: 10.4172/2167-1206.1000155 | |
| Copyright: © 2014 Nurolaini K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Traditional Medicine & Clinical Naturopathy
Abstract
The use of traditional medicines (TM) and Complementary Alternative Medicines (CAM) are common in Western Pacific countries including Brunei and Singapore. Our cross-sectional study assessed the prevalence of TM use amongst Brunei population. The objectives are to compare the practices on the use of TM with conventional medicines and to address the safety and cost implication. This study was conducted for a period of 12 months from October 2007. It was a cross-sectional study using a structured self-administered questionnaire which was pretested from the pilot study. Questionnaires were randomly administered to all patients attending the tertiary hospitals and health centres in Brunei. The questionnaires are bilingual and consists of 27-item questions. Both sexes were included in the study, and participants had to be mentally competent and of age between 16 years and 85 years. Data entry and analysis were done using SPSS version 16.0. Information leaflets were given to participants, and their written-informed consent was obtained. There were 2,400 respondent for this study of which 32% (n=777) were male and 68% (n=1,623) were female, 85 % were Malays, and 55% were in employment status. The proportion of Bruneians who have used some form of TM during their lifetime was 59%, (n=1,396). Use of TM is equal in proportion among Chinese (62%) and Malay ethnicities (59%). Use of TM was highest in the 56 years and above age group (71%), p<0.01. It was higher amongst female respondents compared to males p<0.001. 64% respondents indicated that TM was safe. 76% (n= 1,804) of respondents answered that TM are easily available. Majority of TM users (91%) used local herbs and 63% used TM for general health and vitality. 43% of users of prescribed medicines (common cold remedies, antipyretics and antibiotics) reported using TM as well. 73% of respondents did not report their use of TM to their doctors. 94% (n=1,284) of the respondents claimed that there were no adverse effects accompanying use of TM. 62% perceived TM is safe due to the traditional practices and natural sources. 82% of TM users spend less than BND $50 on TM every month. We concluded from this study that there is a high prevalence of TM use in Brunei despite the free health care services provided in the country. Doctors need to understand TM better and communicate more with their patients regarding TM use. This can be due to their use as maintenance of health rather than for treatment of illness. TM is also easily available and perceived to be safe because it had been used for generations and of natural sources despite their limited scientific evidence. The lack of regulation and perceptions of TM being safe needs extra cautions to avoid any potential serious adverse herb-drug interactions. Therefore, medical and health care workers should not ignore this perceptions and patients’ education is utmost important.
According to the World Health Organization (WHO) [8], Traditional Medicines in the ASEAN region is define as any medicinal product for human use consisting of active ingredients derived from natural sources (plants, animals and/or minerals) used in the system of traditional practice. This may include botanical and herbal medicines used traditionally for therapeutic purposes over an undefined period of time.Therefore, the system of traditional practice is a diverse health practices, approaches, knowledge and beliefs incorporating plant, animal, and/or mineral based medicines, spiritual therapies, manual techniques and exercises applied singularly or in combination to maintain well-being, as well as to treat, diagnose or prevent illness. WHO defines Complementary Alternative Medicine (CAM) to a broad set of health care practices that are not part of that country's own tradition and are not integrated into the dominant health care system [8].
One example of the traditional medicines is Traditional Chinese Medicine (TCM) which is a holistic form of medicine with a 5,000 year history [9]. It is one of the popular complementary medicines in the United Kingdom. TCM comprises of Traditional Chinese Herbal Medicine(TCHM), acupuncture, acupressure, massage (tuina), energy therapy (qi gong) and other practices. Another example of traditional medicine is Indian traditional medicine (Ayurveda), which is the oldest medical system in the world. In India, 70% of the population relies on the system of traditional medicines, mainly Ayurveda, Unani and Siddha [10]. A traditional Indonesian herbal medicine (Jamu), thought to originate from Java island; is well known to the people in Brunei. Jamu is a holistic therapy with influences from Indian, Chinese and Arabian classical medicines and the use of massage is particularly important. Traditionally Jamu is prepared at home from fresh herbal plants, but nowadays few people have the time and skill to prepare this traditionally and thus many of the Jamu sold today are processed and packaged in powder form, or tablets/capsules. The powder form can be brewed with hot water instantly.
In Brunei, there are local folk remedies known as “Ubat kampong” which are believed to be practiced among indigenous groups which have knowledge about the herbal plants found locally. One example of Ubat Kampung in Brunei is made by boiling a combination of plants or ginger roots for about 10-20 minutes. The boiled water can be taken orally for various medicinal reasons such as general well being. So far, there are no reported data on the use of TM in Brunei but its use is likely to be of the same order as in the study reported by Chong et al. [1]. In a pilot study reported by our group, 69% out of the 150 Bruneians undertaken the study has admitted to using TM and 70% says that there are easily available for the public [4]. This data is similar to a study conducted in 2005 by Lim et al. on CAM use in Multiracial Singapore, where 76% (95% C.I. 73.9-77.9%) used CAM over a 12-month period [3].
The purpose of conducting this cross-sectional study was to determine the prevalence of TM use amongst patients attending the government tertiary hospitals and health centres in Brunei. Most Bruneians would seek treatment at the government hospitals or health centre’s due to the free health care services provided by the Government [11]. The objectives are tocompare the practices on the use of TM with Conventional Medicines; and to address the safety, availability and cost implication on the use of TM in Brunei.
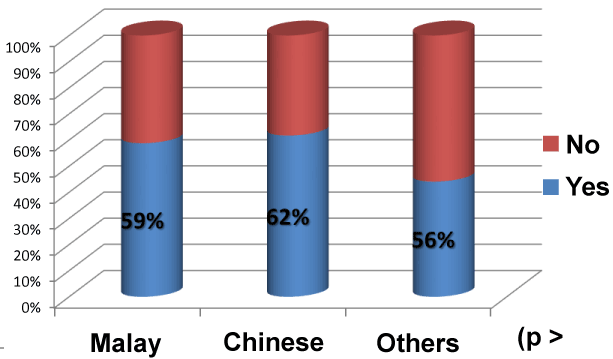
The proportion of Bruneians who have used some form of TM during their lifetime was 59%, (n=1,396). Use of TM is equal in proportion among Chinese (62%) and Malay ethnicities (59%) (Figure 2).
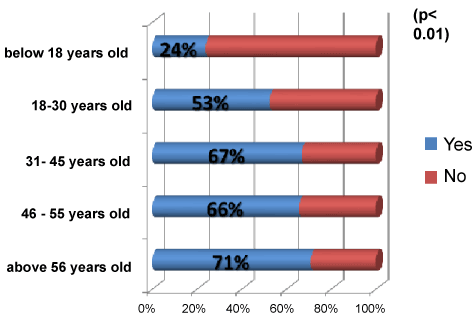
Use of TM was highest in the 56 years and above age group (71%), p<0.01. It was higher amongst female respondents compared to males p<0.001 (Figure 3).
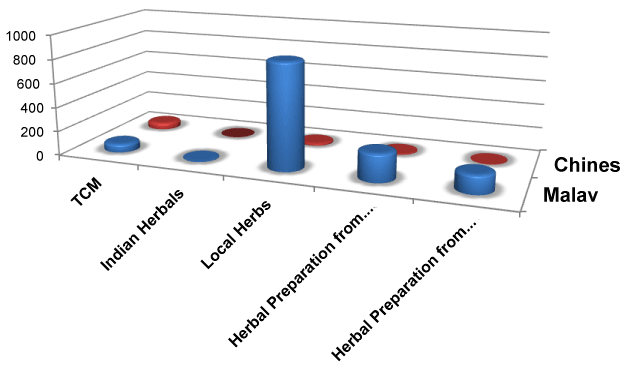
From figure 4, the most commonly used TM amongst Malays in Brunei is local herbs. Herbal preparations from Malaysia are equally popular with herbs found in Indonesia (these are normally commercialized products sold in the market).
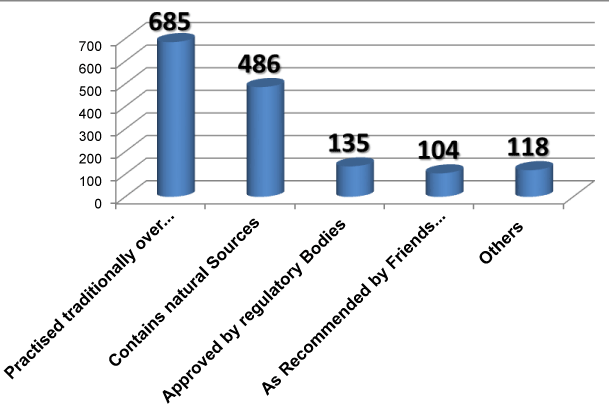
Sixty two percent of the respondents indicated that TM was safe. Figure 6 below indicates that sixty two percent perceived that TM is safe due to traditional practices and natural sources.
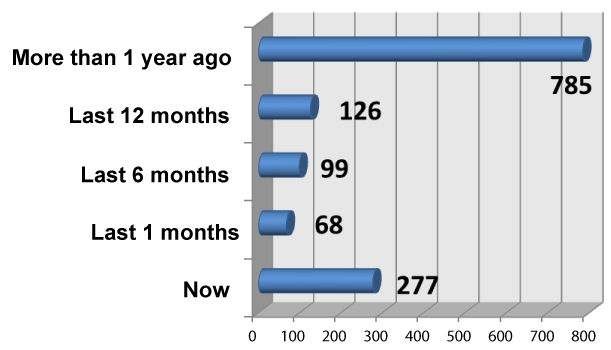
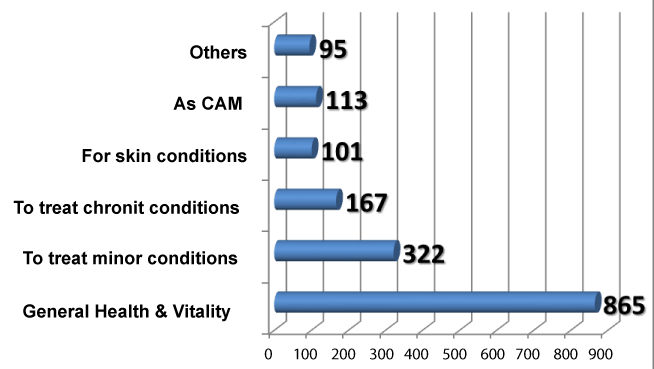
The majority of TM users (91%) used local herbs and 63% used TM for general health and vitality, see Figure 8. Other types of TM used are Traditional Chinese Medicine (TCM), Herbs from Malaysia, Indonesia and India. Participants were also asked in what time period they k took TM (Figure 7).
Forty three percent of users of prescribed medicines (common cold remedies, antipyretics and antibiotics) reported using TM as well. Seventy three percent of respondents did not report their use of TM to their doctors. Ninety four percent (n=1,284) of the respondents claimed that there were no adverse effects accompanying the use of TM. Seventy six percent (n=1,804) of respondents answered that TM is easily available. Eighty two percent of TM users spend less than BND $50.00 on TM every month.
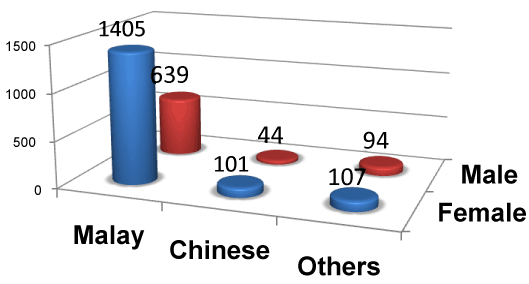
Out of the 2,400 participants, 85% were Malaysand 55% were in employment; whereas the rest are students and unemployed. The ethnicity distribution is similar to Brunei’s demographic profile where the predominant ethnic group Malays, comprises 65.7%, the Chinese ethnic group is 10.3% and other races including expatriates make up the rest of the population with 24.0% [11].
The use of TM in this study is similar in proportion among Chinese (62%) and Malay ethnicities (59%). The types of TM used amongst the Malay ethnic group are local herbs, followed by herbs from Malaysia and herbs from Indonesia. Chinese participants used TCM as their choice of TM. 63% (n=865) of participants used TM for maintaining health and vitality rather than for treatment of major or minor illnesses. This is similar to the study conducted in Singapore [3].
Use of TM for this study was highest in the 56 years and above age group (71%), p<0.01. This can be explained by the age of the patients attending tertiary hospitals in Brunei as they are mainly from this age group and present with chronic conditions. In agreement with a previous study done by Chong et al. [1] older age groups in their study had a higher prevalence of CAM use, especially traditional remedies for treating ailments.
It was higher amongst female respondents compared to males p<0.001. This is not surprising as most of the participants in this study are female participants. This is also in agreement with study done in 2005 by Chong et al. [1] where 58% were females.
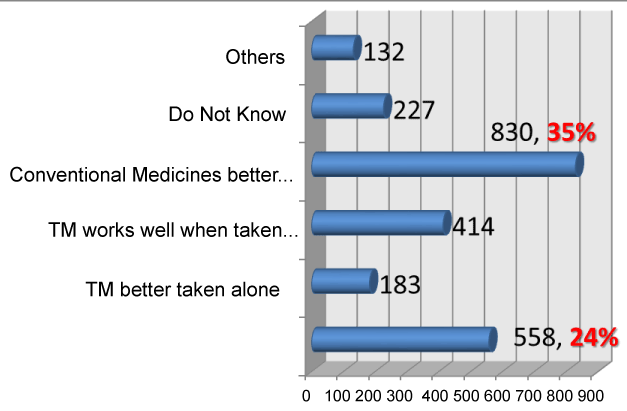
21.9% of CAM users in the medical wards in the tertiary hospital took prescribed medications in the study done by Chong et al. [1]. Participants in this survey would have taken conventional medicines in their life too. Thus their knowledge and perceptions between TM and conventional medicines are also being investigated. 35% participants (n=830) know that conventional medicines are far better than TM but 24% participants (n=558) still believed that TM is better taken together with conventional medicines. 94% (n=1,284) of the respondents claimed that there were no adverse effects accompanying the use of TM.
Most traditional medicines can be used effectively in the hands of an experienced practitioner and most of the herbs used are intrinsically fairly safe. Unfortunately lack of regulation, quality issues and the discovery of some toxic metals in some products has led to concerns about the safety of TM [12]. 62% participants in this study perceived TM is safe because it had been used for generations and is of natural sources despite their limited scientific evidence. The rest of the participants are unsure and claimed it is not safe. 76% (n=1,804) of participants mentioned that TM is easily available and 32% (n=434) said it can be found in specialized shops and supermarkets. 82% of TM users spend less than BND $50 on TM every month. The lack of regulation and perceptions of TM being safe needs extra caution to avoid any potentially serious adverse herb-drug interactions. Therefore, medical and health care workers should not ignore these perceptions and patients’ education is of utmost important.
Doctors need to understand TM better and communicate more with their patients regarding TM use. 73% of TM users did not discuss their use of TM and Conventional medicines with their doctors. This can be due to their use for maintenance of health rather than for treatment of illness. 43% of users of prescribed medicines (e.g. for common cold remedies, antipyretics and antibiotics) reported using TM as well. This is similar to other studies reported elsewhere where user of CAM may not inform their doctors of their use.
It is worth highlighting the limitations in our study. First, the sampling of the participants in this study may not represent the whole of Brunei’s population. Secondly, the socioeconomic characteristics of the participants of this study were not polled; such as the level of education, monthly income, and religion and marital status. These factors can affect the use of TM. Finally the sample size of certain ethnic groups such as Chinese and other minorities were too small to be analyzed. However, our data is also comparable with CAM user in multiethnic groups in Brunei as well as Singapore [1,3].
We concluded from this study that there is a high prevalence of TM use in Brunei despite the free health care system provided in the country. Doctors and allied health professions need to understand TM better and communicate more with their patients regarding TM use. Most medical schools have not integrated modules on traditional medicines as part of their curriculum in patient care. Perhaps this is something that needs to be considered in the future.
References
- Chong VH, Rajendran N, Wint Z (2008) Prevalence and predictive factors for complementary and alternative medicine use in Brunei Darussalam. Singapore Med J 49: 1012-1016.
- World Health Organisation (2012) The regional strategy for traditional medicine in Western pacific region (2011-2020), Manila, Philippness.
- Lim MK, Sadarangani P, Chan HL, Heng JY (2005) Complementary and alternative medicine use in multiracial Singapore. Complement Ther Med 13: 16-24.
- Kifli N, Wint Z, Lim L (2007) Perception, attitudes, knowledge and practices on traditional medicine among Bruneians – a pilot study. Brunei Darussalam J Health 2: 82-85.
- Eisenberg DM, Kessler RC, Foster C, Norlock FE, Calkins DR, et al. (1993) Unconventional medicine in the United States. Prevalence, costs, and patterns of use. N Engl J Med 328: 246-252.
- Oldendick R, Coker AL, Wieland D, Raymond JI, Probst JC, et al. (2000) Population-based survey of complementary and alternative medicine usage, patient satisfaction, and physician involvement. South Carolina Complementary Medicine Program Baseline Research Team. South Med J 93: 375-381.
- Robinson A, McGrail MR (2004) Disclosure of CAM use to medical practitioners: a review of qualitative and quantitative studies. Complement Ther Med 12: 90-98.
- World Health Organization (2000) General Guidelines for Methodologies on Research and Evaluation of Traditional Medicine, Geneva, Switzerland.
- Teng L, Shaw D, Barnes J (2006) Traditional Chinese Herbal Medicines, Pharm J 276: 361-363.
- Williamson E (2006) Ayurveda: introduction to Pharmacists. Pharm J276: 108-110.
- http://www.moh.gov.bn/satisticshealthguidelines/download/HIB_2012.pdf
- Brody TM; Larner J, Minneman KP (2005) Brody’s Human Pharmacology: molecular to clinical.Elsvier Mosby, Philadelphia.
Figures at a glance
 |
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 | Figure 4 |
 |
 |
 |
 |
| Figure 5 | Figure 6 | Figure 7 | Figure 8 |
Relevant Topics
- Acupuncture Therapy
- Advances in Naturopathic Treatment
- African Traditional Medicine
- Australian Traditional Medicine
- Chinese Acupuncture
- Chinese Medicine
- Clinical Naturopathic Medicine
- Clinical Naturopathy
- Herbal Medicines
- Holistic Cancer Treatment
- Holistic health
- Holistic Nutrition
- Homeopathic Medicine
- Homeopathic Remedies
- Japanese Traditional Medicine
- Korean Traditional Medicine
- Natural Remedies
- Naturopathic Medicine
- Naturopathic Practioner Communications
- Naturopathy
- Naturopathy Clinic Management
- Traditional Asian Medicine
- Traditional medicine
- Traditional Plant Medicine
- UK naturopathy
Recommended Journals
Article Tools
Article Usage
- Total views: 17154
- [From(publication date):
June-2014 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 12373
- PDF downloads : 4781
