Research Article Open Access
Radical Laparoscopic Treatment for Hepatic Hydatid Disease
Jarufe N*, Galindo JL, Bächler JP, Ahumada V, Rebolledo R, Crovari F, Guerra JF and Martínez J
Department of Digestive Surgery, Clinical Hospital Pontifical, Catholic University of Chile, Santiago, Chile
- Corresponding Author:
- Nicolas Jarufe. MD.
Chief of Department, Department of Digestive Surgery
Faculty of Medicine, Pontificia Universidad Católica de Chile
Marcoleta 350, Patio Interior, División de Cirugía, 8330033, Santiago, Chile
Tel: +56992991399
E-mail: njarufe@med.puc.cl
Received Date: March 28, 2016; Accepted Date: April 22, 2016; Published Date: April 28, 2016
Citation: Jarufe N, Galindo JL, Bächler JP, Ahumada V, Rebolledo R, et al. (2016) Radical Laparoscopic Treatment for Hepatic Hydatid Disease. J Gastrointest Dig Syst 6:419. doi:10.4172/2161-069X.1000419
Copyright: © 2016 Jarufe N, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Gastrointestinal & Digestive System
Abstract
Background: Surgical approach is considered the most effective treatment for hydatid liver disease (HLD). Nevertheless, there is no general consensus regarding whether either open or laparoscopic surgery is the best approach.
Aim: To evaluate laparoscopic approach for the surgical treatment of HLD.
Methods: A retrospective study was performed. Patients with uncomplicated HLD who underwent laparoscopic radical pericystectomy from April 2007 to May 2015 were included. Preoperative variables, cyst characteristics and recurrence rates were analysed.
Results: Twenty-four patients underwent radical laparoscopic surgery. The median age was 35 years (3-79). The median sizes were 8 cm (3-15). The in-hospital stay was 3 days (2-25) and the overall morbidity was 16% (4 cases), one patient presented biliary leak complication. No mortalities were registered. The median follow-up care of this cohort was 57,5 months (9-106), one case of thoracic recurrence was observed.
Conclusions: Based in our experience, treatment of uncomplicated HLD by laparoscopic pericystectomy is safe and feasible; it concluded no increase in perioperative morbidity, recurrence rate or mortality compared to previous published data.
Keywords
Hydatid liver disease; Pericystectomy; Laparoscopy
Introduction
Hydatid disease is a zoonosis caused by the larval stages of taeniid cestodes belonging to the genus Echinococcus. Cystic echinococcosis (CE) occurs as the result of an infection during the larval stages of E. granulosus [1]. CE has a wide geographical distribution; South America, Africa, Eastern Europe, the Mediterranean, Australia and part of Asia are the most affected areas [1]. In Chile, CE is a very common condition, particularly in the south region called Patagonia [2]. CE is considered to be a life-threatening disease due to its medical and economic outcomes. Natural evolution of CE could include vital organs invasion or cyst rupture, which could trigger anaphylaxic shock or sepsis. Frecuently, the liver is the most affected organ. Most of primary infections are due to simple cysts, but approximately 20% - 40% of patients have had multiple cyst infections [1]. Predominantly, these patients remain asymptomatic for a long time because cysts tend to have a slow growth rate. Symptoms depend not merely on the size and number of cysts, but also on the mass effect upon the surrounding structures. Symptoms could include hepatomegaly, abdominal pain, nausea and vomiting. Thoracic migration is rare, but can lead to serious pulmonary complications. A ruptured cyst can lead to a systemic immunological response, which causes anaphylaxis in nearly 10% of cases [1,3].
Currently, echinococcosis can be diagnosed with a combination of imaging and serology. Hydatid cysts may be visualized and evaluated with ultrasonography, computed tomography, or magnetic resonance imaging. Serology is utilized for primary diagnosis and for follow-up after treatment [4,5]. Frequently employed methods for screening tests are ELISA and Indirect hemagglutination (IHA). Sensitivity of ELISA assays is 60 to 90% and the specificity is approximately 90% [6]. Confirmatory tests using specific antigens can then be performed, such as immunoelectrophoresis and immunoblotting [7].
When cysts are located into to the liver we call it hydatid liver disease (HLD). Surgery represents the mainstay of treatment for HLD. There are described radical and conservative approaches to HLD. Conservative techniques include: unroofing, omentoplasty, capitonnage, partial cystectomy, and PAIR (puncture, aspiration, injection and re-aspiration). These techniques have been shown to be less effective in terms of recurrence and morbiditycompared to radical approach [8]. In contrast, radical surgery (pericystectomy or liver resection) has proved to offer better management of the residual cavity, and, therefore, a reduction in complications and cyst recurrence [9,10]. In recent years, there has been a tendency toward laparoscopic surgery. Additionally, there has been a lack of published experiences regarding radical surgeries that have used a minimally invasive approach [11,12]. Furthermore, most of the available data refer to conservative procedure, small (less than 5 cm) and peripheral cysts.
Due to the limited evidence available about the results of laparoscopic radical surgery, the aim of the present study is to describe the radical pericystectomy surgical technique, evaluate its safety, feasibility and follow up for the treatment of HLD.
Patients and Methods
Design
We performed a retrospective cohort study using the standards established by the ethics committee of our institution. The data were collected from a surgical database and clinical records of 24 patients undergoing radical laparoscopic surgical treatment (pericystectomy) for uncomplicated HLD with laparoscopic approach from April 2007 to May 2015 operated at Pontificia Universidad Católica de Chile, Hospital Clínico.
All cases were diagnosed based on history, physical examination, abdominal computed tomography (CT) and ELISA. To rule out pulmonary hydatid disease or trans-diaphragmatic cysts a thorax CT scan was performed prior to surgery. All patients were treated with albendazole (10 mg/kg/day) for at least 2 weeks, preoperatively, and 4 weeks, postoperatively.
The follow up protocol included a medical control every fifteen days during first month with liver tests and clinical examination, then every three months during the first year. At this point a CT or ultrasonography control was included. After the first year, we performed just clinical examination yearly.
The medical and surgical records of the patients were analysed according to the following preoperative parameters: age, sex, location, size and number of cysts diagnosed by imaging. The perioperative and postoperative parameters that were considered outcomes are: estimated blood loss, operative time, conversion to open surgery, intervention (Pericystectomy total, subtotal or partial), perioperative complications (bile leak, abscess, bilioma, and anaphylaxis), length of hospital stay and hospital re-entry, mortality perioperative, and recurrences.
Surgical technique
In order to understand the different levels of pericystectomy our team made the followings characterisations: i. a total pericystectomy was understood as the complete resection of the pericystic layer, ii. a subtotal pericystectomy was understood as a resection of more than 90%, and, finally, iii. a partial pericystectomy was understood as a resection of less than 90% of the pericystic, uninfluenced by the resection type, due to the fact that the residual cavity was always eliminated. However, in cases in which the perycystic membrane was attached to a major vessel (i.e., the suprahepatic or portal vein or the inferior vena cava), a small pellet of the pericystic membrane was left in place to avoid major vascular damage. We considered radical surgery total pericystectomy and subtotal pericystectomy with no residual cavity. This was the standard of treatment.
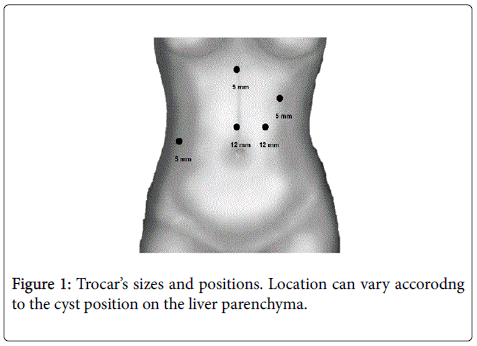
All patients were treated by radical laparoscopic surgery. A pneumoperitoneum with carbon dioxide was performed using a Veress needle. Afterwards, 0º optic trough a 12-mm umbilical trocar was used to carefully explore the abdomen for potential sites of cyst dissemination. The sizes and positions of the auxiliary trocars depended on the location of the cyst (Figure 1). Two long strips of gauze soaked with hypertonic sodium chloride solution as a scolecidal agent were placed around the cyst. Cyst was punctured, content was aspirated with a 14-gauge laparoscopic needle connected to a 50-ml syringe via a three-way stopcock, and then it was replaced with the scolecidal agent. At the moment of the puncture, an additional aspirator tip was placed close to the puncture point to avoid spillage of the cyst contents. After 5 minutes, the sodium chloride hypertonic solution was aspirated; a wide incision was then made to unroof the cyst and hydatid fragments, including the laminated membrane and daughter cysts, which were then removed and placed in a laparoscopic plastic bag for extraction. The residual cavity was carefully inspected for biliary openings and retained daughter cysts. Next step was the resection of the entire pericystic membrane, separating from the normal hepatic parenchyma, using an energy tool: harmonic scalpel or electrofulguration. Hemostasis is complemented with bipolar coagulator, vascular clips or intracorporeal suture. Special attention was given to bile communications. In all cases a standard laparoscopic cholecystectomy with Starsberg’s safe view approach was performed. In order to rule out bile leaks or communications an intraoperative cholangiography was performed. In cases were a bile leak was detected, intracorporeal suture or clips were used to close them. Finally, one or two drains were positioned around the surgical bed (Figure 2).
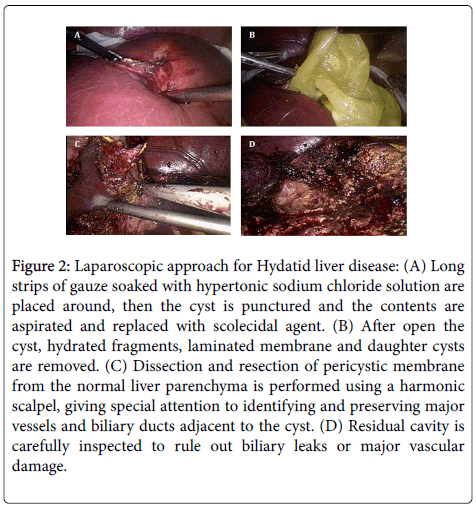
Figure 2: Laparoscopic approach for Hydatid liver disease: (A) Long strips of gauze soaked with hypertonic sodium chloride solution are placed around, then the cyst is punctured and the contents are aspirated and replaced with scolecidal agent. (B) After open the cyst, hydrated fragments, laminated membrane and daughter cysts are removed. (C) Dissection and resection of pericystic membrane from the normal liver parenchyma is performed using a harmonic scalpel, giving special attention to identifying and preserving major vessels and biliary ducts adjacent to the cyst. (D) Residual cavity is carefully inspected to rule out biliary leaks or major vascular
damage.
Statistical Analyses
Continuous variables are expressed as medians and ranges, and categorical variables are expressed as absolute numbers and%ages. All statistical analyses were performed using SPSS (version 20.0-Mac; SPSS Inc.; Chicago, IL) software.
Results
Clinical features
During the study period, a total of 24 patients underwent laparoscopic operations as a consequence of uncomplicated HLD. Median age of the entire cohort group was 35 years (3-79), and 62,5% of them were female. Median sizes were 8 cm (3-15). Most of the patients (n=23, 95.8%) had single cysts. All cysts were located between the segment II-VIII, with 9 patients (37.5%) involving the segment VI or VII. Preoperative features are summarized in Table 1.
| N=24 | ||
| Age (year) | 35 (3-79) | |
| Female | 15 (62.5%) | |
| ASA | I | 14 (58.3%) |
| II | 10 (41.6%) | |
| III- IV-V | 0 (0%) | |
| Cyst Size (cm) | 8 (3-15) | |
| Emergency Surgery | 0 (0%) | |
| Single cyst | 23 (95.8%) | |
| Prior recurrence | 1 (4.1%) | |
| Cyst Location* | I | 0 (0%) |
| II | 4 (16.6%) | |
| III | 4 (16.6%) | |
| IV | 4 (16.6%) | |
| V | 8 (33.3%) | |
| VI | 9 (37.5%) | |
| VII | 9 (37.5%) | |
| VIII | 5 (20.8%) |
Table 1: Preoperative features in patients underwent pericystectomy for HLD.
Perioperative variables
The median operative times was 162.2 minutes (60-255), median intraoperative bleeding was 113 ml (10-500), and median hospital stay was 3 days (2-25). Just one patient had a prolonged hospital stay due to a biliary leak; all rest had a hospital stay shorter than 10 days. Overall morbidity was 16.6% (4 patients); one case of a bile leak, one of an intraabdominal abscess and two cases of asyntomatic bilioma. No mortalities were registered. No conversion to open surgery, perioperative mortality, and anaphylaxis were observed. Detailed perioperative variables are described in Table 2.
| N= 24 | ||
| Estimated blood loss (ml) | 113 (10-500) | |
| Operative time (min) | 162.5 (60-255) | |
| Extension of pericystectomy* | Total | 7 (29.1%) |
| Subtotal | 12 (50%) | |
| Partial | 0 (0%) | |
| Conversion to open surgery | 0 (0%) | |
| Overall morbidity | 4 (16.6%) | |
| Bile leak | 1 (4.1%) | |
| Abscess | 1 (4.1%) | |
| Bilioma | 2 (8.2%) | |
| Anaphylaxis | 0 (0%) | |
| Mortality perioperative | 0 (0%) | |
| Hospital stay (days) | 3 (2-25) | |
| Hospital re-entry | 1 (4.1%) | |
| Recurrence | 1 (4.1%) | |
| *Total pericystectomy was defined as the complete resection of the pericystic layer, a subtotal pericystectomy was defined as a resection of more than 90%, and a partial pericystectomy was defined as a resection of less than 90% of the pericyst. | ||
Table 2: Perioperative variables in patients underwent pericystectomy for HLD.
One patient had a blood loss of 500 ml. Bleed was intraoperative due to cyst intrahepatic venous communications. Hemostasis was satisfactory at the end of the surgical procedure and no blood replacement was needed. Hospital stay was 4 days and no further complications were reported.
Patient with longer hospital stay (25 days) was due to a bile leak. This patient had a cyst in lateral segments 2 and 3 of 6 cm diameter. Early after surgery a bile leak was observed. Since fever and abdominal pain occurred and abdominal CT scan revealed perihepatic liquid a percutaneous drain was planned. Unfortunately, that attempt failed. A laparoscopic exploration was performed for intra-abdominal cleaning and drainage. After 48 hrs a new episode of fever and abdominal pain started, a new abdominal CT scan revealed a pelvic liquid accumulation, a second laparoscopic exploration was performed for intra-abdominal cleaning and drainage. After 11 days patient was discharged from hospital in good conditions and no biliary fistula.
Follow-up care
All patients maintained regular follow-up care for a median period of 57,5 months (9-106). No hospital re-entries were observed. Up to the present, one patient had a thoracic recurrence after 28 month of surgical treatment.
Discussion
Hydatid disease of the liver is a highly prevalent condition in certain regions of the world. Although have been proposed several alternative treatments (e.g., medical, PAIR, etc.), surgery remains the most effective treatment. Among all surgical procedures, radical surgery (pericystectomy or liver resection) has demonstrated to provide better management of the residual cavity, and, consequently, fewer perioperative complications, and recurrences [9,10,13].
The first case of laparoscopic approach for the treatment of HLD was described in 1992 [14], but due the potential risk of spillage and anaphylaxis during the procedure, the spread of this technique was initially limited. Since then, several studies have been published and reported good results for laparoscopy in terms of perioperative morbidity and postoperative pain; however, most of these studies were based on conservative laparoscopic procedures (drainage, partial cystectomy, etc.). Tuxun et al published a world review of 914 cases comparing open to laparoscopic surgery, combining data from 57 studies. They concluded that laparoscopic resection of hydatid cysts was safe and feasible, and provided similar outcomes to open surgery. Moreover, they shown that 75% of all laparoscopic cases that have been reported since 1992 were conservative procedures, and only approximately 10% were radical surgeries [15]. Unfourtunately those results were not organized by treatment options such as pericystectomy, cystectomy, and/or hepatectomy, among others, which reduce power to their conclusions.
We postulate that currently, radical surgery for hydatid cystic liver disease via a minimally invasive approach is feasible [8], and pericystectomy should be the procedure of choice. Considering that laparoscopy allows to a better visualization and control of the vasculobiliary structures during the procedure, particularly in cases in which a biliary fistula is suspected. In our centre, we have implemented this approach as the standard of treatment due to the promising results published in literature in terms of recurrence and perioperative complications. Until now, our results have supported this approach with low morbidity rate and no mortality; these values are comparable to those reported in other studies.
Ramia et al. published 24 cases that were treated by laparoscopy using total cystectomy, and observed a perioperative morbidity rate of 16%, no recurrences, and a median follow-up of 31 months (2-86) [16]. In our country, an initial report (8 cases) published by Manterola et al. found no recurrence or major morbidity in patients who were treated by laparoscopic radical resection [17], although this study included cyst diameter less than 7 cm, located in segments III, IV, V, VI, and VIII. Recently, Zaharie et al. published a comparative study of open and laparoscopic surgeries and found no differences in terms of overall surgical complications or recurrence [18]. Another study performed by Yagcsi et al. compared open versus laparoscopic approach and PAIR versus open approach. PAIR and open group exhibited higher incidences of biliary leak and cyst recurrence than the laparoscopic group. Despite these findings, the authors recommended laparoscopic surgery only for selected cases due to the risk of spillage, and the difficulties related to cyst manipulation 12).
These and other studies have demonstrated some benefits of laparoscopy. These studies are insufficient to recommend this approach over open surgery. The fact that most of the available evidence is based on cases that were treated with a conservative laparoscopic approach (cystectomy alone, cystectomy + omentoplasty, etc.) instead of radical surgery could explain this issue.
Although some studies have reported vascular injuries, the current evidence does not support that such injuries are a substantial risk, since no cases reported in the most recent literature [3,8,15]. Special considerations must be made if the cysts are located adjacent to major vessels (portal and/or suprahepatic veins, etc.). In such cases, we postulate that small pericystic pellets should be left attached to avoid injury. In our experience, this procedure did not affect either the outcome of the surgery or the recurrence rate.
Recently, a review of all cases treated by laparoscopy since 1992 (n=914) showed that the incidences of anaphylaxis and spillage are below 1% (0.9% and 0.3%, respectively) [15]. Moreover, no mortalities, or major morbidities related to these complications have been reported. In our experience, the use of gauze soaked with hypertonic sodium chloride solution, the intracyst injection of a scolecidal agent, laparoscopic suction and the administration of albendazole prior to the surgery, minimized the risk of spillage and other related complications.
Anaphylaxis is one of the limitations of this technique, and although in our centre no episodes of it have occurred, it is known that spillage of the cyst contents during laparoscopy can lead to this complication, for this reason, a careful management of cyst contents is required during the procedure.
Initially, the contraindications for laparoscopy included a diameter > 10 cm, multiple or intraparenchymal cysts, complicated cysts with cystobiliary communication, and proximity to large vessels. Based on our experiences, we think that number, size, and cyst location should not longer be considered as an absolute contraindication. Although it has been accepted that the laparoscopic approach tend to be more dificult when cysts are located in the central or posterior segments of the liver, as the case of large cysts (>10 cm) [19]. In the present study, the median cyst size was 8 cm (3-15) in the laparoscopic group, which is similar or even larger than the sizes reported in published series [12,16,17]. Currently, we have limited the contraindications for the laparoscopic approach only to patients with a ruptured cyst (complicated HLD) or suspected thoracic migration.
Several studies have attempted to compare open and laparoscopic approaches for the treatment of hydatid cyst liver disease. The conclusions are often contradictory, but it seems that, although the open procedure is faster, postoperative pain, hospital stay, and blood loss are reduced with laparoscopy.
Regarding the limitations and biases of this study, the losses of patients during the follow-up care and the retrospective nature plus relatively small sample size we think that our experience has indicated that radical laparoscopic surgery is feasible and safety for the treatment of uncomplicated HLD, regardless of the involved hepatic segment and cyst size, Despite the fact that this procedure can be technically challenging, low perioperative morbidity and lack of recurrence observed in cases treated with this approach and comparable results to open surgery trend us to prefer this minimally invasive approach. Moreover, we postulate that radical techniques, such as pericystectomy, could be considered as the treatments of choice during minimally invasive surgery, considering that evidence has shown that radical surgery represents a better management of the residual cavity, and, consequently, a decrease in the perioperative complications and recurrences.
Our group recommends adopting the laparoscopic radical pericystectomy as standard treatment for uncomplicated HLD in any location of the liver, combining the benefits of laparoscopic surgery with a better management supported by evidence to the hydatid cyst.
References
- Nunnari G, Pinzone MR, Gruttadauria S, Celesia BM, Madeddu G, et al. (2012) Hepatic echinococcosis: clinical and therapeutic aspects.World J Gastroenterol 18: 1448-1458.
- Manterola D (2011) Aspectos clínico-quirúrgicos de la hidatidosis hepática, una zoonosis de creciente preocupación. Rev Chil Cir 63: 641-649.
- Palanivelu C, Jani K, Malladi V, Senthilkumar R, Rajan PS, et al. (2006) Laparoscopic management of hepatic hydatid disease.JSLS 10: 56-62.
- McManus DP, Zhang W, Li J, Bartley PB (2003) Echinococcosis.Lancet 362: 1295-1304.
- Riganò R, Profumo E, Ioppolo S, Notargiacomo S, Ortona E, et al. (1995) Immunological markers indicating the effectiveness of pharmacological treatment in human hydatid disease. Clinical & Experimental Immunology 102: 281-285.
- Biava MF, Dao A, Fortier B (2001) Laboratory diagnosis of cystic hydatic disease.World J Surg 25: 10-14.
- Ortona E, Riganò R, Buttari B, Delunardo F, Ioppolo S, et al. (2003) An update on immunodiagnosis of cystic echinococcosis.Acta Trop 85: 165-171.
- Gavara CGI, López-Andújar R, Ibáñez TB, Ángel JMR,Herraiz ÁM, et al. (2015) Review of the treatment of liver hydatid cysts.World J Gastroenterol 21: 124-131.
- Aydin U, Yazici P, Onen Z, Ozsoy M, Zeytunlu M, et al. (2008) The optimal treatment of hydatid cyst of the liver: radical surgery with a significant reduced risk of recurrence. Turk J Gastroenterol 19: 33-39.
- Prousalidis J, Kosmidis C, Anthimidis G, Kapoutzis K, Karamanlis E, et al. (2012) Postoperative recurrence of cystic hydatidosis.Can J Surg 55: 15-20.
- Smego RA Jr, Sebanego P (2005) Treatment options for hepatic cystic echinococcosis.Int J Infect Dis 9: 69-76.
- Yagci G, Ustunsoz B, Kaymakcioglu N, Bozlar U, Gorgulu S, et al. (2005) Results of surgical, laparoscopic, and percutaneous treatment for hydatid disease of the liver: 10 years experience with 355 patients.World J Surg 29: 1670-1679.
- Yüksel O, Akyürek N, Sahin T, Salman B, Azili C, et al. (2008) Efficacy of radical surgery in preventing early local recurrence and cavity-related complications in hydatic liver disease. J Gastrointest Surg 12: 483-489.
- Dziri C, Haouet K, Fingerhut A (2004) Treatment of hydatid cyst of the liver: where is the evidence?World J Surg 28: 731-736.
- Tuxun T, Zhang JH, Zhao JM, Tai QW, Abudurexti M, et al. (2014) World review of laparoscopic treatment of liver cystic echinococcosis-- 914 patients. Int J Infect Dis 24: 43-50.
- Ramia JM, Poves I, Castellón C, Diez-Valladares L, Loinaz C, et al. (2013) Radical laparoscopic treatment for liver hydatidosis.World J Surg 37: 2387-2392.
- Manterola C, Fernández O, Muñoz S, Vial M, Losada H, et al. (2002) Laparoscopic pericystectomy for liver hydatid cysts.Surg Endosc 16: 521-524.
- Ertem M, Karahasanoglu T, Yavuz N, Erguney S (2002) Laparoscopically treated liver hydatid cysts.Arch Surg 137: 1170-1173.
- Zaharie F, Bartos D, Mocan L, Zaharie R, Iancu C, et al. (2013) Open or laparoscopic treatment for hydatid disease of the liver? A 10-year single-institution experience.Surg Endosc 27: 2110-2116.
Relevant Topics
- Constipation
- Digestive Enzymes
- Endoscopy
- Epigastric Pain
- Gall Bladder
- Gastric Cancer
- Gastrointestinal Bleeding
- Gastrointestinal Hormones
- Gastrointestinal Infections
- Gastrointestinal Inflammation
- Gastrointestinal Pathology
- Gastrointestinal Pharmacology
- Gastrointestinal Radiology
- Gastrointestinal Surgery
- Gastrointestinal Tuberculosis
- GIST Sarcoma
- Intestinal Blockage
- Pancreas
- Salivary Glands
- Stomach Bloating
- Stomach Cramps
- Stomach Disorders
- Stomach Ulcer
Recommended Journals
Article Tools
Article Usage
- Total views: 13370
- [From(publication date):
April-2016 - Sep 01, 2025] - Breakdown by view type
- HTML page views : 12339
- PDF downloads : 1031