Case Report Open Access
Rehabilitation of Non-Syndromic Oligodontia of Primary and Permanent Dentition in Young patient-A Rare Case Report
Rathee Manu1*, Goel Mahesh2, Kumar Arun3, Mehta Richa1 and Kundu Renu1
1Department of Prosthodontics, Post Graduate Institute of Dental Sciences, Rohtak, Haryana, India
2Department of Oral & Maxillofacial Surgery, Post Graduate Institute of Dental Sciences, Rohtak, Haryana, India
3Department of Pedodontics & Preventive Dentistry, Post Graduate Institute of Dental Sciences, Rohtak, Haryana, India
- *Corresponding Author:
- Rathee Manu
Sr. Professor and HOD
Department of Prosthodontics
Post Graduate Institute of Dental Sciences
Rohtak, Haryana, India
Tel: +919416141376
E-mail: ratheemanu@gmail.com
Received date: November 26, 2013; Accepted date: March 26, 2014; Published date: April 3, 2014
Citation: Rathee M, Mahesh G, Arun K, Richa M, Renu K (2014) Rehabilitation of Non-Syndromic Oligodontia of Primary and Permanent Dentition in Young patient-A Rare Case Report. J Interdiscipl Med Dent Sci 2:117. doi:10.4172/2376-032X.1000117
Copyright: © 2014 Manu R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at JBR Journal of Interdisciplinary Medicine and Dental Science
Abstract
Background: Oligodontia is a genetic disorder which represents the congenital absence of more than six teeth in primary, permanent or both dentitions. It is usually a part of a syndrome and seldom occurs as an isolated entity. Genes responsible for non syndromic oligodontia are found to be MSX1 and PAX9 genes.
Methods: Karyotyping was done taking sample from peripheral blood. Cytogenetic chromosome analysis revealed a normal male karyotype (46, XY) without any structural or numerical chromosome abnormalities. Hand wrists, clavicles, vertebral skeleton, skull and chest were found to be normal on radiological examination. After excluding other possible differential factors, the final diagnosis of non-syndromic Oligodontia was made. Preliminary impressions were made using impression compound and was molded on the edentulous ridge. Custom trays were fabricated and border molding was done using green stick impression compound and secondary impressions were made using zinc oxide eugenol impression paste. After maxillo-mandibular jaw relations, dentures were processed through compression molding technique. Dentures were inserted and the patient was taught about the insertion and removal of the dentures. Post insertion instructions regarding denture wear, functions of speech, mastication, hygiene and maintenance were given to the patient and the parent.
Results: The patient was using prosthesis and happy with it during one year follow up. The rehabilitation with removable dentures at current age and later with osseo-integrated implants served as a satisfactory treatment outcome in such patients.
Conclusion: This case report presents prosthodontic rehabilitation of a rare case of non-syndromic oligodontia in a 7-year old male patient with agenesis of all permanent teeth except the maxillary central incisors.
Keywords
Agenesis; Hypodontia; Oligodontia
Introduction
Tooth agenesis is a common developmental anomaly that appears in 2.2 to 10% of the general population; excluding agenesis of third molars [1]. Different terminologies have been used to describe the agenesis of teeth in the primary or permanent dentition. Hypodontia is used to describe the agenesis of one or few teeth; Oligodontia is used to describe agenesis of six or more teeth excluding the third molars and anodontia is the total absence of teeth [2].
Oligodontia usually occurs as a part of syndromes. It may occur as a non-syndromic isolated familial trait linked to mutations of the MSX1 and PAX9, or as a sporadic finding [2]. The tooth agenesis is associated with more than 49 syndromes. Non-syndromic oligodontia has been found either sporadic or familial in nature [3]. Syndromic and non syndromic form of Oligodontia can be differentiated by ruling out presence of associated symptoms.
Oligodontia presents clinical symptoms depending on the number and location of missing teeth. Positional changes of teeth, variation in their morphology and size may occur in the existing teeth. It may be associated with growth disturbances of the maxillofacial skeleton thus affecting the facial appearance [4]. In addition to loss of function and esthetic compromise, psychological development is an important concern in the oral rehabilitation of growing patients [5]. The main objective of management is to improve esthetics, function and psychological health [6,7]. This case report presents a case of oligodontia involving both primary and permanent dentition in a child patient rehabilitated with removable prosthesis.
Case Report
A seven year old male child reported with the chief complaint of many missing teeth. Child’s mother gave the history of uneruption of teeth except upper back teeth. His past medical history was non-contributory and family history revealed that he was born to non-consanguineous marriage with normal delivery and no one in his family had congenitally missing teeth. There was history of extraction of deciduous maxillary right first molar and restorations in other deciduous teeth present. The patient had no history of trauma. The patient does not have any problem in speech however reported difficulty in chewing food particularly the solid food eg. Apple. On extra oral examination, patient’s appearance was near normal except senile facial appearance because of missing teeth and deficient lip support. Skin of the patient’s body was mildly dry and non-atrophic. No frontal and temporal bossing was present. Nose, ears and mid-face of the patient appeared normal. Fine sparse hairs were present on the temporal area. Eyebrows were also sparse (Figure 1).
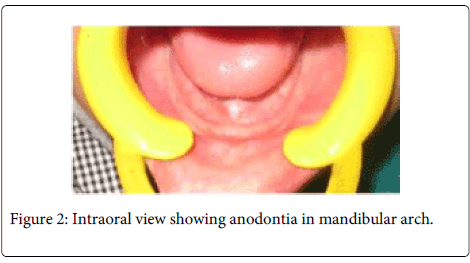
Intraoral examination revealed the presence of deciduous second molars and deciduous left first molar in the maxillary arch and complete anodontia in the mandibular arch with considerably normal but shallow alveolar ridge (Figure 2).
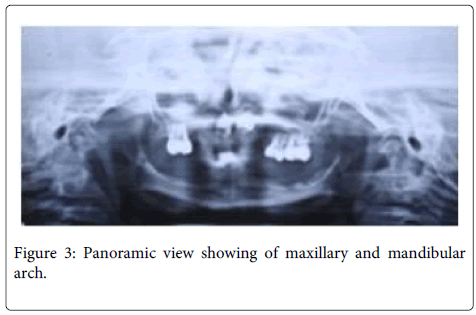
Teeth present were abnormal in morphology and were restored. Buccal mucosa, palate and floor of the mouth appeared to be normal. Flow of saliva was observed normal. Panoramic radiograph revealed the absence of tooth germs of clinically missing teeth except the developing maxillary central incisors along with the presence of 54, 64 and 65 in the maxillary arch. Deciduous molars present showed no resorption of roots (Figure 3). During examination, patient showed no signs of mental disturbance and his behavior in the dental office was age appropriate.
In view of these findings a provisional diagnosis of non-syndromic oligodontia or Oligodontia-I was made with differential diagnosis of Ectodermal Dysplasia; Rieger syndrome and Van der Woude syndrome. Patient was referred to pediatrician to rule out associated syndromes and systemic disorders. Karyotyping was done taking sample from peripheral blood then treating it with Sodium-Heparin-EDTA. Cytogenetic chromosome analysis of PHA stimulated peripheral blood lymphocytes revealed a normal male karyotype (46, XY) without any structural or numerical chromosome abnormalities.
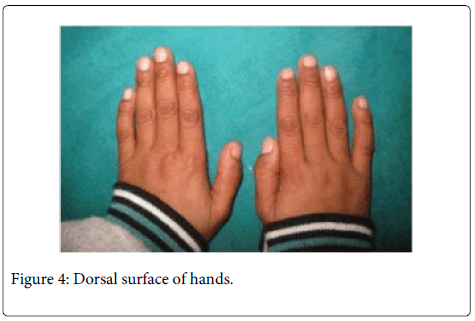
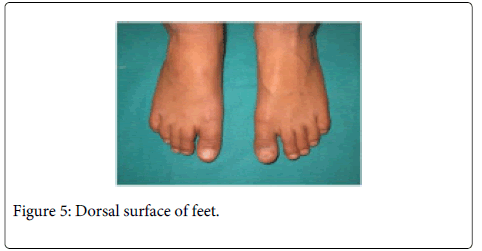
Routine examination of blood including serum calcium, alkaline phosphate, TSH, T3, T4 was done. The findings of these investigations were within normal range. During physical examination, hair were not thin and sparse, nails were not brittle and no difficulty in perspiration was seen, which ruled out ectodemaldysplsia; on occular examination, no signs of glaucoma was seen, ruling out Rieger syndrome and Van Der Woude syndrome was ruled out as there was no associated cleft palate or any mucosal cysts in lower lip (Figures 4 and 5).
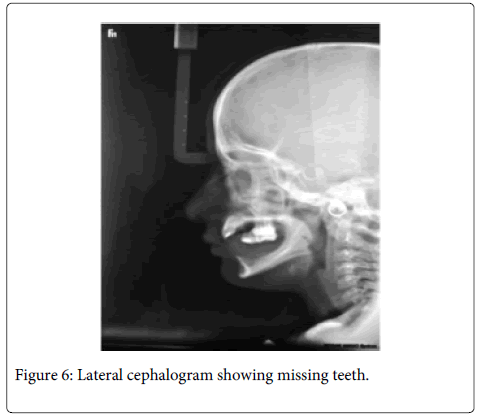
Hand wrists, clavicles, vertebral skeleton, skull and chest were found to be normal on radiological examination (Figure 6). Based on above findings the final diagnosis of non-syndromic Oligodontia was made.
The rehabilitation with removable dentures at current age and later with osseointegrated implants was discussed with the parents. The child was familiarized with the materials to be used. Preliminary impressions were made using impression compound (Pinnacle impression compound, DPI, India). The impression compound was molded on the edentulous ridge using fingers without support of stock tray as the size of the arch was very small. Custom trays were fabricated using auto polymerizing acrylic resin (DPI-RR Cold acrylic resin, DPI, India). Border molding was done using green stick impression compound (Pinnacle Tracing sticks, DPI, India) and secondary impressions were made using zinc oxide eugenol impression paste (Impression paste, DPI, India). There were no undercuts on the teeth to resist impression making with zinc oxide eugenol impression paste. Record bases were made using auto polymerizing acrylic resin (DPI-RR Cold acrylic resin, DPI, India).
The maxillary rim was adjusted for lip support, esthetics and phonetics. The mandibular occlusal rim was adjusted with occlusal plane kept lower to angle of mouth and vertical dimension of occlusion was established. The maxillo-mandibular jaw relations were transferred to the articulator. The try-in was done to verify esthetics, phonetics and jaw relations. The patient and his mother evaluated and approved the trial denture. Clasps were used to provide retention to the maxillary removable partial denture. Dentures were processed through compression molding technique using heat cure acrylic resin (DPI- heat cure acrylic resin, DPI, India). Dentures were inserted and the boy was taught the way to insert and remove the dentures. Post insertion instructions regarding denture wear, functions of speech, mastication, hygiene and maintenance were given to the patient and the parent. The child was recalled after 24 hours and a week for follow up. The child was happy and seemed to have adjusted well to the dentures.
Recall visits were scheduled every three months for follow-up. After 3 months of insertion of dentures, the patient presented with the complaint of loose maxillary denture. On examination, it was observed that the right maxillary permanent central incisor crown was showing beneath the denture base.
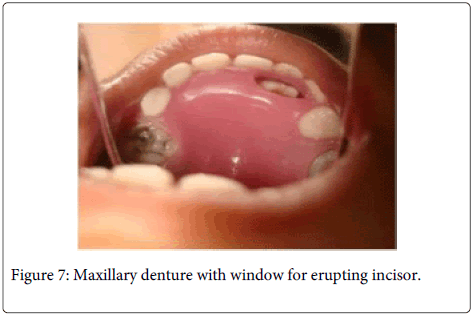
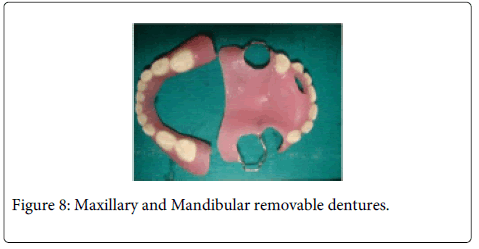
Radiographic evaluation revealed an erupting permanent maxillary right central incisor. Necessary trimming of the denture base were done to accommodate the erupting tooth and facilitate eruption (Figures 7 and 8).
The patient was using prosthesis and happy with it during one year follow up. Patient did not turn up after that (Figure 9).
Discussion
Oligodontia is an anomaly having an overall prevalence of 0.14% [8], with prevalence of 0.3% in the permanent dentition and 0.5% to 0.9% in primary dentition [9]. Population studies on the prevalence of hypodontia suggest that majority (more than 80%) will present with one or two congenitally missing teeth and only less than 1% will present with six or more missing teeth [10]. The incidence of oligodontia is reported to vary from 0.08 to 0.16% [4]. Rolling S reported only 0.16% of the Danish school children with five or more missing permanent teeth [11]. The incidence rate suggested by Schalk-van der is 0.08% of the population [12]. In the study by Ravan and Nielsen of 1530 Danish school children, 0.26% had six or more missing teeth. In a Swedish study prevalence was 0.19%. Its prevalence is estimated at 0.14% in the white population [13].
Non-syndromic familial oligodontia has, in most cases, been shown to be inherited as an autosomal dominant trait. Mutations in the genes MSX1 and PAX9 that encode transcription factors has been demonstrated to be associated with isolated, non-syndromic oligodontia [14]. Oligodontia condition should not be neglected as it may result in various disturbances like abnormal occlusion, altered facial appearance which may cause psychological distress, difficulty in mastication and speech especially during the formative age. Thus early diagnosis and treatment of these patients is very important.
The treatment of oligodontia could be challenging if there are several missing teeth and malocclusion is present. Treatment planning should take into account the age of the patient, number and condition of retained teeth, number of missing teeth, condition of supporting tissues, the occlusion and interocclusal space [15]. Dental treatment can vary depending on the severity of the disease and generally requires a multidisciplinary approach. Treatment options include orthodontic therapy, implants, adhesive techniques, removable partial prostheses, fixed prostheses and over dentures [16-18]. Most young patients require the fabrication of a partial denture as an interim procedure before definitive restoration is planned. Early treatment improves speech and masticatory function in addition to psychological implications that may greatly help in regaining self-confidence of the young patient. It is postulated that in cases where early prosthetic reconstruction is essential, the aim should be to provide the patient with interim solutions which satisfy aesthetic and functional requirements and avoid unnecessary damage to tissues. Prosthodontic rehabilitation is fundamental in these situations that allow the child to lead a normal life without damaging self-esteem or psychological development and ensuring that behavior remains unaffected [5]. Further, in the case reported above the prosthetic rehabilitation using complete dentures had lot of benefits including better social acceptance, self-esteem and restoring normal functional demands of the patient such as chewing.
Heuberer et al. [19] proposed dental implant treatment as viable treatment alternatives for compensating oligodontia in adolescents. Provided that other treatment options are considered, the areas of skeletal growth are respected and the patients as well as parents are well informed.
Conclusion
Child patient suffering from oligodontia may have severe functional, esthetic and psychological problems especially during the early years of life as reported in the present case. These conditions should be evaluated carefully for the presence of associated symptoms and treated at the earliest with multidisciplinary approach. Removable prosthodontics is an interim restoration for successful rehabilitation of these patients at young age with added advantages of greater self-esteem, better social acceptance, re-establishment of the masticatory function and aesthetics.
References
- De Coster PJ, Marks LA, Martens LC, Huysseune A (2009) Dental agenesis: genetic and clinical perspectives. J Oral Pathol Med 38: 1-17.
- Kotsiomiti E, Kassa D, Kapari D (2007) Oligodontia and associated characteristics: assessment in view of prosthodontic rehabilitation. Eur J ProsthodontRestor Dent 15: 55-60.
- Gorlin RJ, Cohen MMJ, Levin LS (1990) Syndromes of the head and neck. (3rdedn), Oxford University Press, New York, USA.
- Worsaae N, Jensen BN, Holm B, Holsko J (2007) Treatment of severe hypodontia-oligodontia--an interdisciplinary concept. Int J Oral MaxillofacSurg 36: 473-480.
- Giray B, Ak�?§a K, Iplik�?§io�?�?lu H, Ak�?§a E (2003) Two-year follow-up of a patient with oligodontia treated with implant- and tooth-supported fixed partial dentures: a case report. Int J Oral Maxillofac Implants 18: 905-911.
- Tsai PF, Chiou HR, Tseng CC (1998) Oligodontia--a case report. Quintessence Int 29: 191-193.
- Heuberer S, Dvorak G, Zauza K, Watzek G (2012) The use of onplants and implants in children with severe oligodontia: a retrospective evaluation. Clin Oral Implants Res 23: 827-831.
- Polder BJ, Van't Hof MA, Van der Linden FP, Kuijpers-Jagtman AM (2004) A meta-analysis of the prevalence of dental agenesis of permanent teeth. Community Dent Oral Epidemiol 32: 217-226.
- Vastardis H, Karimbux N, Guthua SW, Seidman JG, Seidman CE (1996) A human MSX1 homeodomain missense mutation causes selective tooth agenesis. Nat Genet 13: 417-421.
- Larmour CJ, Mossey PA, Thind BS, Forgie AH, Stirrups DR (2005) Hypodontia--a retrospective review of prevalence and etiology. Part I. Quintessence Int 36: 263-270.
- Singer SL, Henry PJ, Lander ID (2010) A treatment planning classification for oligodontia. Int J Prosthodont 23: 99-106.
- Durstberger G, Celar A, Watzek G (1999) Implant-surgical and prosthetic rehabilitation of patients with multiple dental aplasia: a clinical report. Int J Oral Maxillofac Implants 14: 417-423.
- Créton M, Cune M, Verhoeven W, Muradin M, Wismeijer D, et al. (2010) Implant treatment in patients with severe hypodontia: a retrospective evaluation. J Oral MaxillofacSurg 68: 530-538.
- Stockton DW, Das P, Goldenberg M, D'Souza RN, Patel PI (2000) Mutation of PAX9 is associated with oligodontia. Nat Genet 24: 18-19.
- Dhanrajani PJ (2002) Hypodontia: etiology, clinical features, and management. Quintessence Int 33: 294-302.
- Finnema KJ, Raghoebar GM, Meijer HJ, Vissink A (2005) Oral rehabilitation with dental implants in oligodontia patients. Int J Prosthodont 18: 203-209.
- Locker D, Jokovic A, Prakash P, Tompson B (2010) Oral health-related quality of life of children with oligodontia. Int J Paediatr Dent 20: 8-14.
- Correia MF, Nogueira MN, Bedran TB, PalomariSpolidorio DM (2013) Aesthetic rehabilitation of oligodontia in primary dentition with adhesive partial denture. Case Rep Dent : 872476.
- Heuberer S, Dvorak G, Mayer C, Watzek G, Zechner W (2014) Dental implants are a viable alternative for compensating oligodontia in adolescents. Clin Oral Implants Res.
Relevant Topics
- Cementogenesis
- Coronal Fractures
- Dental Debonding
- Dental Fear
- Dental Implant
- Dental Malocclusion
- Dental Pulp Capping
- Dental Radiography
- Dental Science
- Dental Surgery
- Dental Trauma
- Dentistry
- Emergency Dental Care
- Forensic Dentistry
- Laser Dentistry
- Leukoplakia
- Occlusion
- Oral Cancer
- Oral Precancer
- Osseointegration
- Pulpotomy
- Tooth Replantation
Recommended Journals
Article Tools
Article Usage
- Total views: 15691
- [From(publication date):
April-2014 - Jul 19, 2025] - Breakdown by view type
- HTML page views : 11028
- PDF downloads : 4663