Research Article Open Access
Rehabilitation with ΟΔ¬?¬?Software Controlled Short Tension Impulses TherapyΟΔ¬?¬ù (So.Co.Short) for Lumbar and Cervical Chronic Radiculopathy
Raoul Saggini1*, Simona Maria Carmignano2, Marco Supplizi3, Emilio Ancona2, Lucia Cosenza2 and Rosa Grazia Bellomo4
1Physical and Rehabilitation Medicine, Department of Medical Oral and Biotechnological Sciences, Director of the School of Specialty in Physical and Rehabilitation Medicine, “Gabriele d’Annunzio” University, Chieti-Pescara (Italy), National Coordinator of Schools of Specialty in Physical and Rehabilitation Medicine, Italy
2School of Specialty in Physical and Rehabilitation Medicine, “Gabriele d’Annunzio” University of Chieti-Pescara, Italy
3Physiotherapist, Lecturer, Faculty of Physiotherapy “G.d’Annunzio” University-Chieti, Italy
4Physical and Rehabilitation Medicine, Department of Medical Oral and Biotechnological Sciences,“Gabriele d’Annunzio” University, Chieti-Pescara, Italy
- *Corresponding Author:
- Raoul Saggini
Gabriele d’Annunzio University, V.le Abruzzo 322
66100 Chieti, Italy
Tel: +39 0871 3553005-3553007
Fax: +39 335 8339950
E-mail: raoul.saggini@unich.it
Received date: August 07, 2017; Accepted date: August 28, 2017; Published date: August 31, 2017
Citation: Saggini R, Carmignano SM, Supplizi M, Ancona E, Cosenza L, et al. (2017) Rehabilitation with “Software Controlled Short Tension Impulses Therapy” (So.Co.Short) for Lumbar and Cervical Chronic Radiculopathy. J Nov Physiother 7:363. doi: 10.4172/2165-7025.1000363
Copyright: © 2017 Saggini R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Novel Physiotherapies
Abstract
Background: Recent studies have highlighted a new use of electrical stimulation called electroceutical therapy that uses electrical stimulation similar to frequency modulated electromagnetic neural stimulation (FREMS) that influence and modify the functions of the body. A pilot study was designed aimed to evaluate the efficacy of “Software Controlled Short Tension Impulses Therapy” (So.Co.Short) in subjects with lumbar and cervical radiculopathy in chronic phase treated with two different protocol one daily or and the other every other day. Furthermore, the second endpoint is monitor analgesic intake for 2 month after the end of protocol.
Materials and Methods: 60 patients with chronic cervical radiculopathy were included, aged between 31 and 80 years and 70 subjects with chronic lumbar radiculopathy aged between 28 and 80 years. Patients underwent a session, using a newly-developed biomedical device that allows the application of software-controlled electric impulses of variable tension, frequency and duration “Software Controlled Short Tension Impulses Therapy”- (So co.Short) for 10 sessions with two modalities of application: daily or every other day. At the beginning (T0) and the end (T1) of the treatment all patients performed Visual Analogic Scale (VAS), Neck Disability Index (NDI) or Oswestry Disability Index (ODI). A drug diary was kept by each subject to monitor analgesic intake at T0 (before 2 weeks at beginning of study) and 1 month after the end of protocols.
Results: Results confirm effectiveness for pain relief and reduction of analgesic intake.
Conclusion: In conclusion, the findings of this study confirm that So.Co.Short is safe and leads to pain relief and improvement of healing in lumbar and cervical chronic radiculopathy. Probably the best application is on every other days, because stimulating the production of growth factors and triggering the relief of pain, must leave enough time for the molecules produced to act on the inflammatory process.
Keywords
Chronic radiculopathy; Pain relief; Electroceutical medicine; Rehabilitation; Low back pain; Neck pain
Introduction
Peripheral radiculopathy is pathology with a multiple and complex etiology and it represents the major cause of neuropathic pain. Patients with neuropathic pain usually are more heavily burdened than patients with nociceptive pain and they suffer more often from insomnia, anxiety, and depression [1,2].
Lumbar radiculopathy can involve both the back and the legs. In addition, both neuropathic and nociceptive pain pathways contribute to lower back and associated leg pain. Generally, the leg pain component is due to neuropathic pain, and the back pain component is due to nociceptive mechanisms [3]. Cervical radiculopathy is defined as a syndrome of pain and/or sensorimotor deficits due to compression of a cervical nerve root. The compression can occur as a result of disc hernia, lumbar spondylolisthesis, instability, trauma, or rarely, tumors. Patient presentations can range from complaints of pain, numbness, and/or tingling in the upper extremity to electrical type pains or even weakness [4,5]. Both cervical that lumbar radiculopathy can be a debilitating disease that can cause patients significant impairment. The damage can be significant both economically, from lost work and wages, and psychologically, from prolonged pain and impaired social functioning. The goal for treatment should be the rapid diagnosis and treatment of this condition in order to facilitate the return of the patient to their normal state of health.
Several studies and systematic reviews show that the management of radicular pain is still controversial [6-8]. Other studies examined the efficacy of Transcutaneous Electrical Nerve Stimulator (TENS) in musculoskeletal disorders and neuropathic pain have been published so TENS has been increased popularity used as a treatment of acute and chronic pain [9-11].
Afterwards, clinical trials showed that frequency modulated electromagnetic neural stimulation (FREMS), as a non- pharmacological treatment, is a safe and effective therapy for pain in peripheral radiculopathy, leading to the amelioration of symptoms and improvement of peripheral nerve function Bosi et al. [12]. Recent studies have highlighted a new use of electrical stimulation called “electroceutical therapy” that uses electrical stimulation to influence and modify the functions of the body that allow the treatment of various pathologies Through autogenously production of neurotransmitters [13].
Other studies have shown that the factors involved in regenerative processes of peripheral nervous tissue can be stimulated by controlled voltage pulse generator therapy as activation of cell membrane channels, synchronization of vasomotor responses increase of peripheral blood flow and endothelial growth factors [14].
Based on these considerations, a pilot study was designed aimed to evaluate the efficacy of “Software Controlled Short Tension Impulses Therapy” (So.Co.Short) in subjects with lumbar and cervical radiculopathy in chronic phase treated with two different protocol one daily or and the other every other day. Furthermore, the second endpoint is monitor analgesic intake for 1 month after the end of protocol.
Materials and Methods
This pilot study carried out at Universitary Center of Physical and Rehabilitative Medicine of “G.d’Annunzio” Universitary in accordance with the Helsinki Declaration of 1964. All participants were informed about the study methods and issued their written consent before making the therapeutic protocol.
Inclusion criteria
18 years of age, with chronic lumbar and cervical radiculopathy, pain for more than one month, pain level of at least 3 on Visual Analogic Scale (VAS scale), and written informed consent.
For cervical radiculopathy, we include patients with a neurologic condition characterized by dysfunction of a cervical spinal nerve, the roots of the nerve, or both. It usually presents with pain in the neck and one arm, with a combination of sensory loss, loss of motor function, or reflex changes in the affected nerve-root distribution [15].
For lumbar radiculopathy a condition of the peripheral nervous system that causes the appearance of intense pain at the lumbo-sacral area of the back, which radiates along one of the lower limbs and reaching the foot with motor and sensory deficits [16,17].
Pain level was of at least 3 on Visual Analogic Scale (VAS scale) for both pathological conditions.
Exclusion criteria for treatment were:
• Pregnancy;
• Pacemaker;
• Lack of self-sufficiency in ADL and IADL;
• Severe deterioration of the cognitive state (Mini-Mental State Examination ≥ 24);
• Neurodegenerative diseases, cancer, cardiopulmonary, and renal failure.
• Concomitant inflammatory diseases, administration of nonsteroidal anti-inflammatory drugs (NSAID) in the 2 weeks preceding the study;
• Indication for surgical treatment.
Patients’ recruitment and sample collection
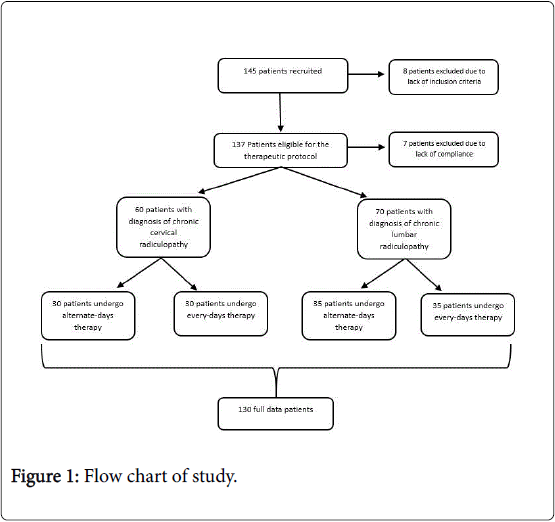
60 patients with chronic cervical radiculopathy were included, aged between 31 and 80 years (mean age: 53 years, 11 M, 19 F) and 70 subjects with chronic lumbar radiculopathy aged between 28 and 80 years (average age: 57 years old, 15 M, 24 F) (Figure 1).
In the 60 patients with cervical radiculopathy, at magnetic resonance imaging (MRI) was demonstrated the presence of 10 herniated discs, 19 multiple slipped disc, 31 localized protrusions.
In the 70 subjects with lumbar radiculopathy, the MRI revealed the presence of 12 herniated discs, 21 multiple protrusions, 37 localized protrusions.
The patients underwent a session, using a newly-developed biomedical device that allows the application of software-controlled electric impulses of variable tension, frequency and duration – “Software Controlled Short Tension Impulses Therapy”- (So co.Short) for 10 sessions.
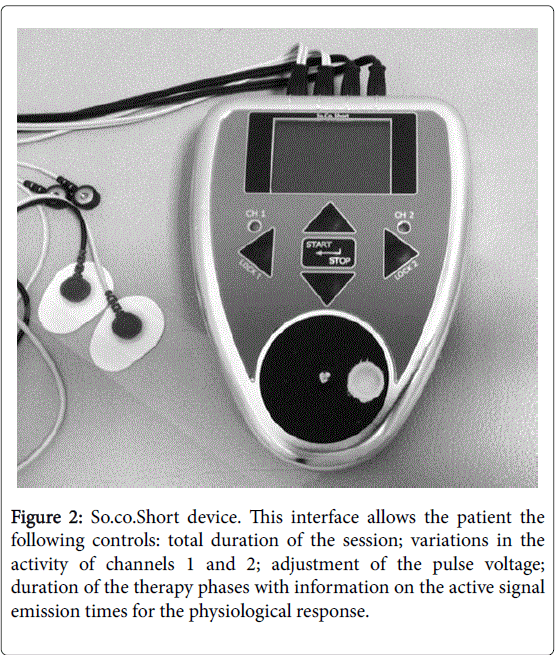
It is a technology consisting of biocompatible electrical signals generated by computerized neuro-stimulators and applied through trans-cutaneous electrodes (Figure 2).
Figure 2: So.co.Short device. This interface allows the patient the following controls: total duration of the session; variations in the activity of channels 1 and 2; adjustment of the pulse voltage; duration of the therapy phases with information on the active signal emission times for the physiological response.
The So.co.Short is software controlled voltage pulse generator with two independent channels, which varies the "pulse patterns", according to the pathology being treated and patient response.
The technical characteristics of the device are: a frequency ranging from 1Hz a 500Hz, amplitude of 0V a 200V regulated by patient depending on the specific perception of the pulse; and a rise time lower than 25 ns. The impulses were managed by specific software, which varied the pulse patterns according to the patient response.
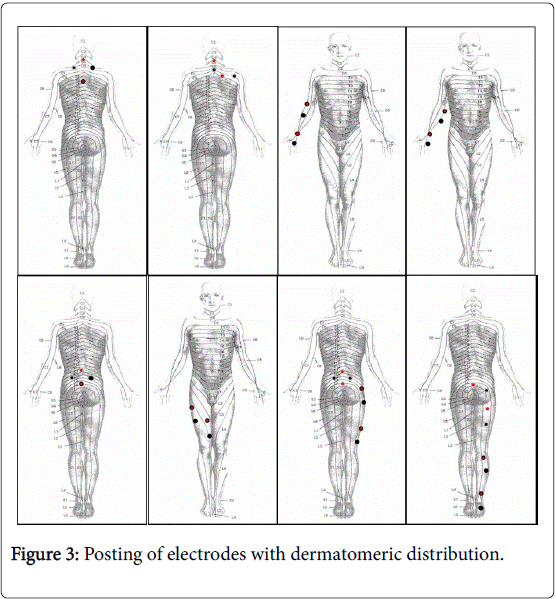
Furthermore, So.Co.Short system differs from other device because it allows positioning the electrodes throughout the peripheral area, following the dermatomeric distribution (Figure 3).
In the cervical radiculopathy group, 30 patients underwent therapy on alternate days and 30 patients underwent daily treatment. In the lumbar radiculopathy group, 35 patients underwent therapy on alternate days, 35 patients underwent day-to-day treatment.
Each session lasted 27 minutes in the cervical radiculopathy group and 31 minutes in the lumbar radiculopathy group.
Clinical assessment
At the beginning (T0) and the end (T1) of the treatment all patients performed:
-Evaluation of balance and gait by administration of Visual Analogic Scale (VAS);
-Assessment of pain and patient-rated disability with Neck Disability Index (NDI) for cervical radiculopathy group. The NDI can be scored as a raw score [18] or doubled and expressed as a percent [19].
Each section is scored on a 0 to 5 rating scale, in which zero means 'No pain' and 5 means 'Worst imaginable pain'. Al the points can be summed to a total score. The test can interpreted as a raw score, with a maximum score of 50, or as a percentage.
-Assessment of pain and patient-rated disability with Oswestry Disability Index (ODI) for lumbar radiculopathy group. It is a selfadministered questionnaire divided into ten sections designed to assess limitations of various activities of daily living. Each section is scored on a 0-5 scale, 5 representing the greatest disability. The index is calculated by dividing the summed score by the total possible score, which is then multiplied by 100 and expressed as a percentage. Thus, for every question not answered, the denominator is reduced by 5. If a patient marks more than one statement in a question, the highest scoring statement is recorded as a true indication of disability. The questionnaire takes 3.5-5 min to complete and approximately 1 min to score [20].
A drug diary was kept by each subject to monitor analgesic intake at T0 and at T1 1 month after the end of protocols. A specially devised drug diary was used to measure analgesic intake.
Statistical analysis
Statistical analysis was performed by Fischer's PLSD test. The minimum level of statistical significance was P<0.05. The software used for the analysis was GraphPad Prism (version 5) software (Abacus Concepts GraphPad Software, San Diego, CA).
Results
In the present study, 130 patients with chronic radiculopathy (aged 28 to 80 years) were evaluated and treated. All completed the prescribed therapeutic protocol and performed the second evaluation at the end of the treatment cycle. In all subjects treated, a statistically significant reduction (p<0.05) of the level of pain measured with VAS scale was obtained after each treatment session (expressed in the first two graphs as average trend) (Figure 4).
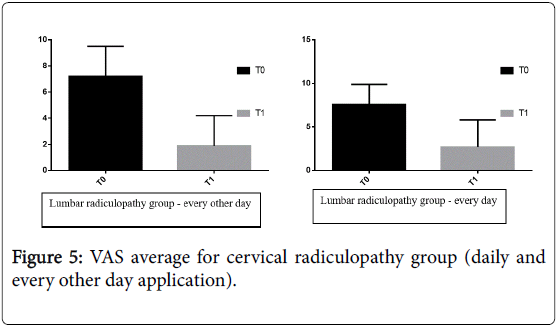
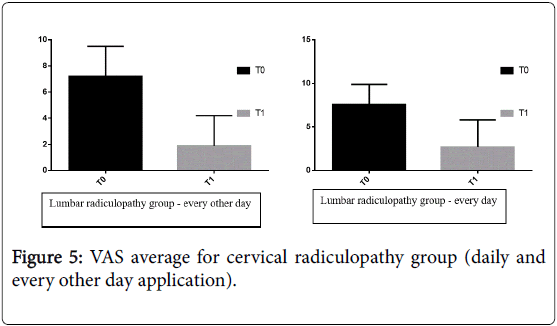
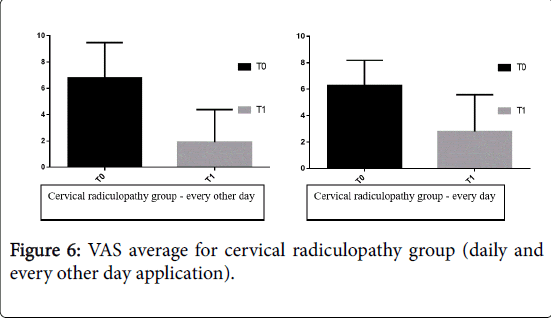
In detail, with regard to subjects with lumbar radiculopathy group who underwent therapy on every other day, there was an average pain level of 7.2 ± 2.3 at T0 and 1.9 ± 2.3 at T1 p=0.045 (p ≤ 0.05); in patient who underwent daily it was showed a decrease in the average pain level of 7.6 ± 2.3 at T0 and 2.7 ± 3.1 at T1 p=0.043 (p ≤ 0.05). In subjects with cervical radiculopathy, who underwent therapy on every other day, an average VAS score of 6.8 ± 2.7 at T0 and 1.9 ± 2.5 at T1 was found p=0.040 (p<0.05.); In patients who performed daily therapy, an average VAS level of 6.3 ± 1.9 to T0 and 2.8 to 2.8 at T1 was recorded p=0.392 (p<0.05.) in Figures 5 and 6.
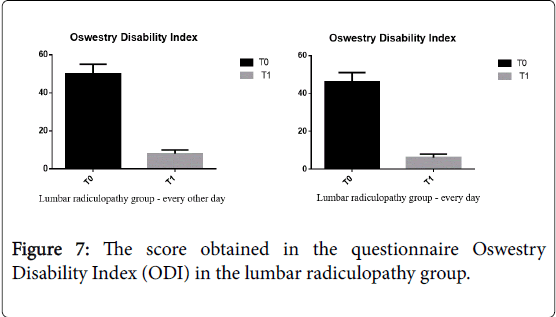
The score obtained in the questionnaire Oswestry Disability Index (ODI) in the lumbar radiculopathy group who performed therapy on every other days decreased on average from 50% (severe disability) at T0 to 8% (minimal disability) at T1 p=0.030 (p<0.05.); in the " group treated daily ODI score decreased by 46% (severe disability) at T0 to 6% at T1 (minimal disability) p=0.037 (p<0.05.) in Figure 7.
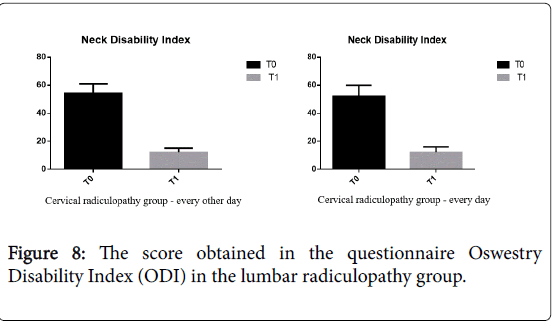
The score obtained in the questionnaire Neck Disability Index (NDI) in the cervical radiculopathy group who performed therapy on every other days decreased on average from 54% (severe disability) at T0 to 12% (mild disability) at T1 p=0.045 (p<0.05.); in the group treated daily NDI score decreased by 52% (severe disability) at T0 to 12 % at T1(mild disability) p=0.047 (p<0.05.) in Figure 8.
Medicines that were taken by the patient or prescribed by the general physician for pain control comprise mainly non-steroidal antiinflammatory drugs (e.g. aspirin, ibuprofen) and compound analgesic preparations (e.g. co-dydramol, co-proxamol). All other drugs were excluded.
To calculate drug intake, a percentage formula was used:
Drug intake (%) = Number of days with drugs/ Total number of days x 100.
All patients reduced after 2 month the intake of the analgesic by 60%.
Discussion
The evolving development of medical and surgical therapies has significantly improved the physician's ability to manage patients with cervical and lumbar radiculopathy, yet many continue to suffer debilitating symptoms from their disease and chronic pain [21].
Transcutaneous electrical nerve stimulation (TENS) is the application of electrical stimulation of varying frequency, intensity and pulse duration to the skin for pain relief and it is one of the most used approaches in rehabilitation medicine for radiculopathies [22].
Different TENS modalities use varying combinations of frequency and intensity settings on the device to elicit pain relief. TENS is generally believed to be a safe non-invasive intervention which may produce significant analgesia in many patients with moderate predictable pain associated with a range of conditions [23,24].
Tens acts according to this Gate-Control Theory of Pain, activity in large diameter low threshold mechanoreceptive (touch-related) nerve fibers could inhibit the transmission of action potentials from small diameter higher threshold nociceptive (pain-related) fibers through pre and post synaptic inhibition in the dorsal horn of spinal cord. Humans utilize this mechanism whenever they rub their skin to relieve pain. Because nociceptive fibers (A-delta and C-fibers) have a higher threshold of activation than mechanoreceptive fibers (A-beta fibers) Melzack and Wall proposed that it would be possible to selectively stimulate mechanoreceptive fibers by titrating the amplitude of electrical currents delivered across the surface of the skin (as TENS). This would prevent signals from nociceptive fibers from reaching higher centre of the brain, thus reducing pain [25].
The device used in this study is similar to Frequency-modulated electromagnetic neural stimulation FREMS and it is based on the new concept of “Electroceutical medicine” involves the use of electrical modalities as a modulator of biological processes. Cell membrane responsiveness to an electrical stimulus is determined by the characteristics of its strength duration curve and electrical characteristics. FREMS, being based on TENS methodology, falls within the generic definition of TENS; nevertheless, the electrical stimulus in FREMS significantly differs from those commonly used in other known electrotherapies, mainly TENS apparatuses. FREMS sends pulses with waveforms which recall the cellular action potential associated with packets of complex stimuli that adapt to the biological characteristics of the patient. Electrical stimulation to influence and modify the functions of the cells by supplying electrical impulses directed to specific nerve fibers. FREMS provides sequences of biphasic electrical stimuli that vary simultaneously and automatically in frequency, pulse duration and amplitude, reaching relatively high intensity (300 V) in association with a very short duration (10-100 μs), maintaining electrical balance in the tissues [26].
This feature is novel with respect to existing electrotherapies, which are normally based on ‘geometrical’ waveforms characterized by lower peak intensity and higher pulse duration. Regarding FREMS, it should be emphasized that specific new mechanisms of action have been described, such as enhancement of micro vascular blood flow measured by laser doppler flowmetry [27].
Bevilacqua et al. demonstrated that VEGF release during FREMS may help explain the positive effects on nerve conduction [28].
Furthermore, the biochemical mechanisms underlying nerve root damage remain, unknown, but some studies demonstrated that TGF- β1, IGF-1, IL-6 and IL-6R are located in the protruded disc tissue and they are related to inflammatory process in response to tissue damage.
Cohen et al. [29] demonstrated, using northern analysis that treatment of various cell lines with IL-6 for 6-48 h resulted in a significant induction of vascular endothelial growth factor (VEGF) mRNA. It has been reported that IL-6 also interferes with pain sensation in rats; for instance, intra-cerebral-ventricular injection of IL-6 induces thermal hyperalgesia. In line with this finding is the results can confirm that So.co.Short can modulate pain and the nerve regenerative processes through the possible release of growth factors (especially endothelial) that modulate blood supply and reduce the inflammatory process by promoting healing.
Conclusion
This study investigated the safety and efficacy of So.co Short and results seem to confirm its effectiveness, probably the best application is on every other day, because stimulating the production of growth factors and triggering the relief of pain, must leave enough time for the molecules produced to act on the inflammatory process. A relevant aspect to take into account when considering any new treatment is cost and side effects: the reduction in the use of pain medication results in a reduction in health costs and the risks associated with drug abuse.
A limitation of our study is that the criteria for inclusion did select patients with painful radiculopathy with different etiology and, assessment was done only with subjective scales, No control group or placebo group is included. Therefore, greater research will be needed in the future.
References
- Finnerup NB, Otto M, McQuay HJ, Jensen TS, Sindrup SH (2005) Algorithm for neuropathic pain treatment: an evidence based proposal. Pain118:289-305.
- Waterman BR, Belmont PJ Jr, Schoenfeld AJ (2012) Low back pain in the United States: incidence and risk factors for presentation in the emergency setting. Spine J12:63-70.
- Park SY, An HS, Moon SH, Lee HM, Suh SW, et al. (2015) Neuropathic pain components in patients with lumbar spinal stenosis. Yonsei Med J 56: 1044-1050.
- Carette S, Fehlings MG (2005) Clinical practice. Cervical radiculopathy. N Engl J Med 353:392-399.
- Humphreys SC, Chase J, Patwardhan A, Shuster J, Lomasney L, et al. (1998) Flexion and traction effect on C5-C6 foraminal space. Arch Phys Med Rehabil 79:1105-1109.
- Hedeboe J, Buhl M, Ramsing P(1982)Effects of using dexamethasone and placebo in the treatment of prolapsed lumbar disc. ActaNeurolScand65:6-10.
- Cherkin DC, Deyo RA, Street JH, Barlow W (1996) Predicting poor outcomes for back pain seen in primary care using patients' own criteria.Spine (Phila Pa 1976) 21:2900-2907.
- Croft PR, Macfarlane GJ, Papageorgiou AC, Thomas E, Silman AJ(1998) Outcome of low back pain in general practice: a prospective study.BMJ316:1356-1359.
- Osiri M, Welch V, Brosseau L, Shea B, McGowan J, et al. (2000) Transcutaneous electrical nerve stimulation for knee osteoarthritis. Cochrane Database Syst Rev 4:CD002823.
- Barlas P, Ting SLH, Chesterton LS, Jones PW, Sim J (2006) Effects of intensity of electroacupuncture upon experimental pain in healthy human volunteers: a randomized, double-blind, placebo-controlled study. Pain 122:81-89.
- Johnson M, Martinson M (2007) Efficacy of electrical nerve stimulation for chronic musculoskeletal pain: a meta-analysis of randomized controlled trials. Pain130:157-165.
- Bosi E, ContiM, Vermigli C, Cazzetta G, PerettiE, et al. (2005) Effectiveness of frequency-modulated electromagnetic neural stimulation in the treatment of painful diabetic neuropathy. Diabetologia 48: 817-823.
- Guest JF, Ayoub N, Greaves T (2015) Clinical outcomes and cost-effectiveness of an externally applied electroceutical device in managing venous leg ulcers in clinical practice in the UK. J Wound Care 24: 572-580.
- Ferroni P, Roselli M, Guadagni F, Martini F, Mariotti S, et al. (2005)Biological Effects of a Software-controlled Voltage Pulse Generator (PBK-2C) on the Release of Vascular Endothelial Growth Factor (VEGF). In Vivo 19: 949-958.
- Bogduk N (2003)The anatomy and pathophysiology of neck pain. Phys Med RehabilClin N Am14:455-472.
- Kawakami M,Weinstein JN,Chatani K,Spratt KF,Meller ST,et al. (1994) Experimental lumbar radiculopathy. Behavioral and histologic changes in a model of radicular pain after spinal nerve root irritation with chromic gut ligatures in the rat.Spine 19:1795-1802.
- Van der Windt DA, Simons E, Riphagen II, Ammendolia C, Verhagen AP, et al. (2008) Physical examination for lumbar radiculopathy due to disc herniation in patients with low-back pain. Cochrane database of systematic reviews.
- Vernon H, Mior S (1991) The neck disability index: A study of reliability and validity. J Manipulative PhysiolTher 14:409-415.
- Riddle DL, Stratford PW (1998) Use of generic versus region specific functional status measures on patients with cervical spine disorders. Physical Therapy78:951-963.
- Fairbank JC, Couper J, Davies JB, O’brien JP (1980) The Oswestry low back pain disability questionnaire. Physiotherapy 66: 271-273.
- ManchikantiL, Singh V, Falco FJ, Cash KA, Fellows B (2010) Comparative Outcomes of a 2-year follow-up of cervical medial branch blocks in management of chronic neck pain: a randomized, double-blind controlled trial. Pain Phys13:437-450.
- Sluka KA, Walsh D (2003)Transcutaneous electrical nerve stimulation: basic science mechanisms and clinical effectiveness. J Pain4:109-121.
- Reichstein L, Labrenz S, Ziegler D, Martin S (2005) Effective treatment of symptomatic diabetic polyneuropathy by high- frequency external muscle stimulation. Diabetologia48:824-828.
- Van der Spank JT, Cambier DC, De Paepe, Danneels LA, Witvrouw E, et al. (2000) Pain relief in labour by transcutaneous electrical nerve stimulation TENS. Archives of Gynecology and Obstetrics 264: 131-136.
- Johnson M (2001) Transcutaneous Electrical Nerve Stimulation (TENS) and TENS-like devices. Do they provide pain relief. Pain Reviews8:121-158.
- Barrella M, Toscano R, Goldoni M, Bevilacqua M (2007) Frequency rhythmic electrical modulation system (FREMS) on Hreflex amplitudes in healthy subjects. EuraMedicophys 43:37-47.
- Conti M, Peretti E, Cazzetta G, Galimberti G, Vermigli C, et al. (2009) Frequency-modulated electromagnetic neural stimulation enhances cutaneous microvascular flow in patients with diabetic neuropathy. J Diabetes Complications 23:46-48.
- Bevilacqua M, Dominguez LJ, Barrella M, BarbagalloM (2007) Induction of vascular endothelial growth factor release by transcutaneous frequency modulated neural stimulation in diabetic polyneuropathy. J Endocrinol Invest 30: 944-947.
- Cohen T, Nathari D, Cerem LW, Neufeld G, Levi BZ (1996) Interleukin-6 induces the expression of vascular endothelial growth factor. J BiolChem 271:736-741.
Relevant Topics
- Electrical stimulation
- High Intensity Exercise
- Muscle Movements
- Musculoskeletal Physical Therapy
- Musculoskeletal Physiotherapy
- Neurophysiotherapy
- Neuroplasticity
- Neuropsychiatric drugs
- Physical Activity
- Physical Fitness
- Physical Medicine
- Physical Therapy
- Precision Rehabilitation
- Scapular Mobilization
- Sleep Disorders
- Sports and Physical Activity
- Sports Physical Therapy
Recommended Journals
Article Tools
Article Usage
- Total views: 3192
- [From(publication date):
October-2017 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 2354
- PDF downloads : 838