Case Report Open Access
Restoration of a Non-restorable Lateral Incisor Using Forced Orthodontic Eruption, Fiber Post and Zirconıa-Ceramic Restoration
Pinar Cevik1* and Ozlem Akinci2
1 Department of Prosthodontics, Gazi University, Ankara, Turkey
2 Department of Orthodontics, Mustafa Kemal University, Hatay, Turkey
- *Corresponding Author:
- Pinar Cevik
Assistant professor, Department of Prosthodontics
Faculty of Dentistry, Gazi University
Ankara, Turkey
Tel: +905437733793
Fax: +903122034192
E-mail: dt_pinarcevik@yahoo.com
Received date: February 10, 2014; Accepted date: April 8, 2014; Published date: April 15, 2014
Citation: Pinar Cevik, Ozlem Akinci (2014) Restoration of a Non-restorable Lateral Incisor Using Forced Orthodontic Eruption, Fiber Post and Zirconia-Ceramic Restoration. J Interdiscipl Med Dent Sci 2:116. doi:10.4172/2376-032X.1000116
Copyright: © 2014 Cevik P, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at JBR Journal of Interdisciplinary Medicine and Dental Science
Abstract
Trauma with accompanying crown or root fracture of young permanent incisor is a major problem and a tragic experience and creates a psychological pressure on patients. These cases are sometimes treated with an implant placement after extraction of there lated tooth. We present here an alternative interdisciplinary treatment of severely damaged permanent tooth in a young patient. This case report describes a multidisciplinary approach of a dental trauma that leads esthetic permanent restoration. Inaddition, alveolar bone is conserved and the adjacent teeth need not a fixed prosthesis.
Keywords
Orthodontic extrusion; Anterioresthetic
Introduction
The success of traumatic injuries of permanent incisors depends on how far the fracture border from the gingival margin. It is important to create a dry and retentive area around the fracture field for the future prosthetic rehabilitation. Esthetic and functional problems related to the restoration of teeth with fractured crown are particularly relevant to prosthetic dentistry. For complicated crown fractures, treatment strategies may involve;
reattachment of the fractured crown [1,2]
prosthetic reconstruction whether the fracture line is large or small [2]
extraction of the related tooth [3,4]
orthodontic extrusion [5].
The present case report describes the management of complicated maxillary lateral incisor crown fracture with maintaining the healthy alveolar bone, orthodontic eruption and the final all ceramic complete crown restoration.
Case Report
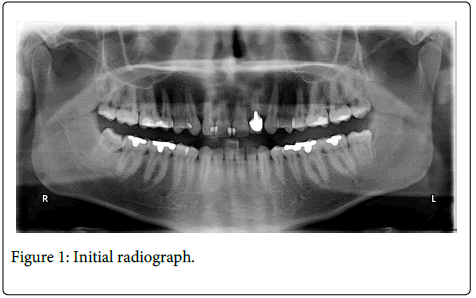
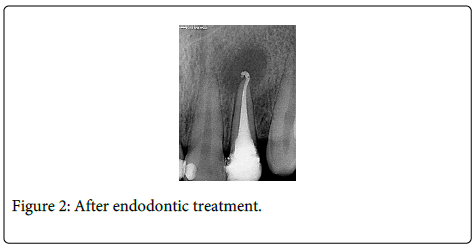
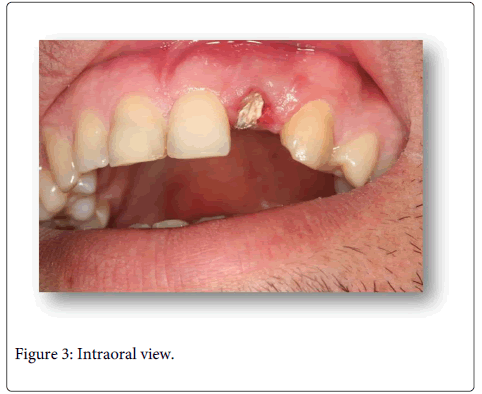
A 20-year-old boy was referred to the Department of Prosthodontics at the Selcuk University Faculty of Dentistry with a crown fracture of traumatic no restorable maxillary left lateral incisor. The patient reported that he had a food related traumatic injury on left lateral incisor previously. Patient’s history indicated that the related tooth had been restored with screw intracanal post and metal ceramic prosthetic restorationwith no root canal obturation. After radiographic examination, a periapical lesion was determined on the apical section of lateral incisor without any bone or root fracture (Figure 1). The periodontal space around the tooth was widened and there was no damage around the adjacent teeth. Vitality responses of adjacent teeth were checked. After getting positive response to pulp vitality tests from the adjacent teeth, conventional endodontic retreatment was performed of tooth 22. Obturation was radiographically followed and periapical radiolucency and gutta-percha overfilling was observed at the apical area (Figures 2 and 3).
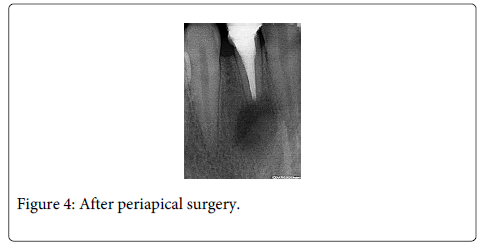
After clinical and radiographic consideration base on the persistence of apical radiolucency, apical surgery with removal of the 3 mm of apical root was planned. Prognosis of bone regeneration was observed after periapical surgery (Figure 4).
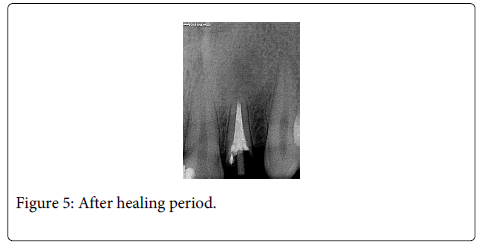
After 7 months healing period of root-end resection, a radiographic image was taken and good bony repair was observed around the periapical area. To gain a core structure around the orthodontic bracket bonding site, a fiber reinforced composite post (FRC Postec Plus, IvoclarVivadent, Liechtenstein) was placed inside the related root and a composite core (Multicore Flow, IvoclarVivadent, Lienchtenstein) was built up to obtain a crown structure for the orthodontic extrusion (Figure 5).
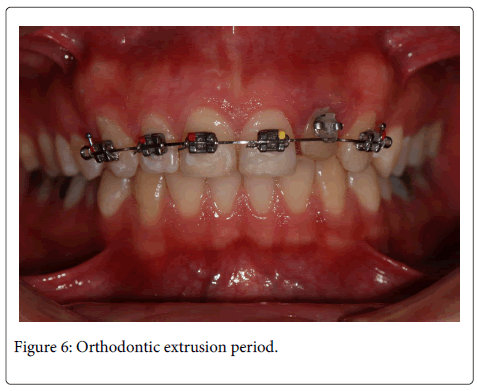
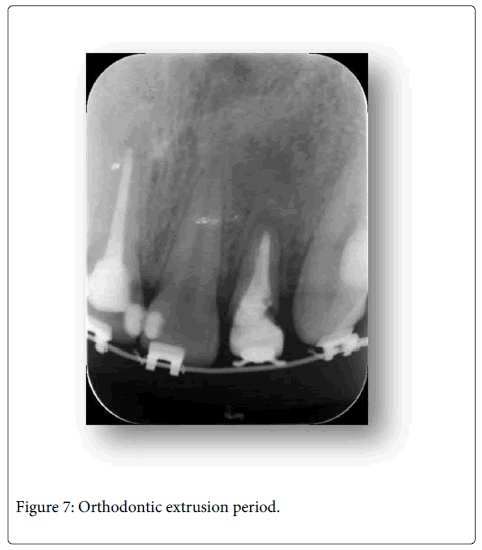
After FRC post placement and composite core restoraiton, the root was orthodontically extruded before fixed prosthetic restoration. Stainless steel standard edgewise brackets (790-010, Dentaurum, Pforzheim, Germany) with an average base surface area of 10 mm2, were bonded (Blugloo, Ormco Corp, Glendora, Calif) from maxillary right canine to left canine. The bracket on the left lateral incisor was poisoned approximately 1,5 mm more cervically to allow for the extrusion. Extrusion was initiated by ligation of an elastic archwire (Dentaurum, Pforzheim, Germany). After 5 week extrusion period, the extruded root was stabilized for 13 weeks by same bonded brackets. While extrusion period, palatal side of the left lateral incisor was gradually reduced by a diamond burr in order to cut off the contact with the opposite teeth (Figures 6 and 7).
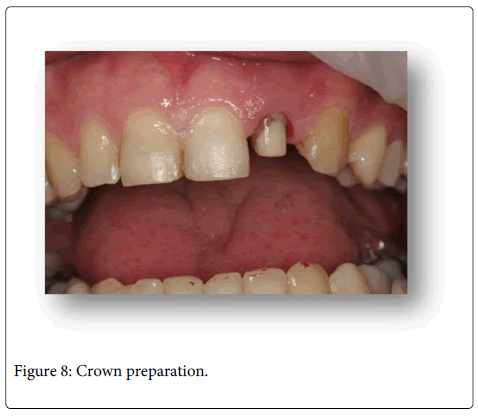
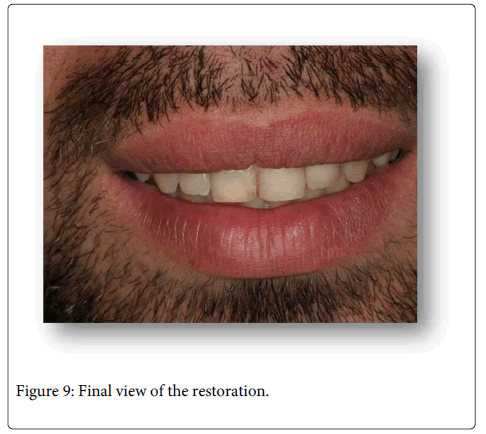
After atraumatic extrusion of the related root, a ferrule effect was obtained around the left lateral incisor for the final ceramic restoration on the post core. Then the clinical procedure consisted of cleaning the crown structure acid etching using 37% phosphoric acid (Total Etch; Ivoclar-Vivadent, Liechtenstein) and application of adhesive, after which a transparent strip crown (Systemp Crown, IvoclarVivadent, Liencheinshten) was filled with composite and placed on the tooth prior to all ceramic complete crown restoration. All ceramic complete crown preparation was generated and a definitive impression of the prepared tooth was made using polyvinylsiloxane impression material (Virtual Putty and Lightbody, IvoclarVivadent Liechtenstein) after then (Figure 8). The interim prosthesis was fabricated and inserted into the relevant tooth. Zirconia framework (Vita Zirconzahn, GmbH & Co KG, Germany) for the left lateral incisor was fabricated and layered with feldspatic porcelain (Vita Zahnfabrik, GmbH & Co KG, Germany). The definitive all ceramic restoration was fabricated with canine guided occlusion. Finally, the crown was cemented with self-cure adhesive resin cement (RelyX™ Unicem, 3M Espe, USA). The patient was given postoperative instructions for the prosthetic restoration and oral hygiene instructions were given. The patient was scheduled for follow-up appointments for every six months (Figure 9).
Discussion
In the present situation, a multidisciplinary approach was defined providing good esthetic and minimizing costly treatment variations. In the present case, orthodontic extrusion was described as an alternative to immediate implant placement in such traumatic crown-root fractures.
Orthodontic extrusion is a treatment option in subgingival crown root fractures for the remaining root to obtain a healty periodontal tissue and ferrule effect around the tooth [5,6]. Ferrule effect is considered to be crucial for the optimal biomechanical behaviour of restored teeth [6]. The major disadvantage of this treatment is long treatment period as the extrusion and stabilization period requires additional time and cost [4,7]. If retention periods of 8 to 12 weeks are not observed, a relapse of tissues may occur due to incomplete tissue remodelling and lack of stability [7].
On the basis of contemporary resin adhesives and resin post systems, fiber reinforced esthetic composite posts are translucent and compatible with root canal dentin with elastic modulus so prevent the root fractures [8,9]. In this case, FRC post and composite core was used to gain a ferrule effect around the tooth during extrusion period.
It has been reported that endodontically treated teeth are vulnerable to fractures, and therefore they frequently require coronal restorations [10]. Conventional metal-ceramic full crown restorations have some disadvantages with regard to esthetics, as they entail a strong risk of restricting translucency, and also of causing discoloration with reference to the associated thin gingival tissue in the cervical area [11]. Zirconia reconstructions have the potential substitute the conventional metal-ceramic fixed-dental prosthesis due to their biocompatibility and similar mechanical strength with metal ceramics [12,13]. Zirconia seems to provide the desired long term stability for clinical applications [13]. Due to these advantages, a zirconia ceramic restoration was selected for the prosthetic treatment to gain an esthetic and durable anterior prosthetic restoration.
References
- Baratieri LN, Monteiro S Jr, CaldeiradeAndrada MA (1990) Tooth fracture reattachment: case reports. Quintessence Int 21: 261-270.
- Turkistani J, Hanno A (2011) Recent trends in the management of dentoalveolar traumatic injuries to primary and young permanent teeth. Dent Traumatol 27: 46-54.
- Adanir N, Ok E, Erdek Y (2008) Re-attachment of Subgingivally Oblique Fractured Central Incisor Using a Fiber Post. Eur J Dent 2: 138-141.
- Heda CB, Heda AA, Kulkarni SS (2006) A multi-disciplinary approach in the management of a traumatized tooth with complicated crown-root fracture: A case report. J Indian SocPedodPrev Dent 24: 197-200.
- Bondemark L, Kurol J, Hallonsten AL, Andreasen JO (1997) Attractive magnets for orthodontic extrusion of crown-root fractured teeth. Am J OrthodDentofacialOrthop 112: 187-193.
- Maitin N, Maitin S, Rastogi K, Bhushan R (2013) Aesthetic management of a complicated crown fracture: a multidisciplinary approach. BMJ Case Rep 3:2013.
- Holst S, Hegenbarth EA, Schlegel KA, Holst AI (2007) Restoration of a nonrestorable central incisor using forced orthodontic eruption, immediate implant placement, and an all-ceramic restoration: a clinical report. J Prosthet Dent 98: 251-5.
- Aksornmuang J, Foxton RM, Nakajima M, Tagami J (2004) Microtensile bond strength of a dual-cure resin core material to glass and quartz fibre posts. J Dent 32: 443-450.
- Kim HD, Lee JH, Ahn KM, Kim HS, Cha HS (2013) Effect of silane activation on shear bond strength of fiber-reinforced composite post to resin cement. J AdvProsthodont 5: 104-109.
- Sevük C, Gür H, Akkayan B (2002) Fabrication of one-piece all-ceramic coronal post and laminate veneer restoration: a clinical report. J Prosthet Dent 88: 565-568.
- McLean JW (2001) Evolution of dental ceramics in the twentieth century. J Prosthet Dent 85: 61-66.
- Piconi C, Maccauro G (1999) Zirconia as a ceramic biomaterial. Biomaterials 20: 1-25.
- Stawarczyk B, Ozcan M, Hämmerle CH, Roos M (2012) The fracture load and failure types of veneered anterior zirconia crowns: an analysis of normal and Weibull distribution of complete and censored data. Dent Mater 28: 478-487.
Relevant Topics
- Cementogenesis
- Coronal Fractures
- Dental Debonding
- Dental Fear
- Dental Implant
- Dental Malocclusion
- Dental Pulp Capping
- Dental Radiography
- Dental Science
- Dental Surgery
- Dental Trauma
- Dentistry
- Emergency Dental Care
- Forensic Dentistry
- Laser Dentistry
- Leukoplakia
- Occlusion
- Oral Cancer
- Oral Precancer
- Osseointegration
- Pulpotomy
- Tooth Replantation
Recommended Journals
Article Tools
Article Usage
- Total views: 16472
- [From(publication date):
April-2014 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 11673
- PDF downloads : 4799