Stapes Surgery Using Stapedotomy versus Partial Stapedectomy
Received: 28-Jan-2017 / Accepted Date: 15-Feb-2017 / Published Date: 22-Feb-2017 DOI: 10.4172/2161-119X.1000291
Abstract
Objectives: To compare the audiological outcomes of two different approaches of stapes surgery, stapedotomy versus partial stapedectomy. Specifically, our experience in this area will be reviewed and compared to results from other centers performing this kind of surgery. Methods: A retrospective chart review of patients who underwent a stapes surgery between 1997 and 2015. A total of 84 surgeries were performed during this period. Seventy-seven subjects were included in the present study. The audiological results as well as the postoperative vertigo were compared. Results: There is significant improvement demonstrated in postoperative closure of Air Bone Gap in both groups. The partial stapedectomy group showed a significant improvement of air–bone gap closure of 10 dB or more (500 Hz to 2000 Hz) compared with the stapedotomy group, which was achieved in 53.1% and 42.2% of both group respectively. Interestingly, by including the full range of speech frequencies (500 Hz to 4000 Hz), the stapedotomy procedure showed better audiological results than partial stapedectomy. The postoperative vertigo was higher in the partial stapedectomy group. Conclusion: The results of this study clearly show that stapedotomy provides good audiometric results and a lower incidence of complications compared to partial stapedectomy.
Keywords: Stapedotomy; Stapedectomy; Stapes surgery
254561Introduction
Otosclerosis is defined as an overgrowth of the bone of the otic capsule just anterior to stapes footplate in between cochlea and vestibule. In such scenario, the stapes is unable to function normally as a piston and eventually becomes completely fixated, which results in a weaker conduction [1,2]. Clinical features are characterised by hearing loss, tinnitus and vertigo, or combination of these. The prevalence of clinical otosclerosis as reported by Declau et al. during the study of a series of temporal bones is 0.3% to 0.4% of the Caucasian population,
while the overall incidence is recorded as 2% for the general population [1]. Clinical otosclerosis should be distinguished from histological otosclerosis. Histological otosclerosis is about 10 times more common than clinical otosclerosis and is found in 10% of the Caucasian population as revealed by Menger et al. [2]. Stapes surgery is the treatment of choice for clinical otosclerosis and is frequently applied in different countries, although a hearing aid is also a feasible alternative [3].
Early attempts to correct the conductive hearing loss associated with otosclerosis date to the late 19th century. The first stapedial operations were performed in 1875 by Kessel who attempted stapedial mobilization [4]. After that, the history of surgical treatment of otosclerosis went through continuous improvements in the surgical technique and instrumentation. Stapedectomy was conducted by Rosen in 1995 [5]. In 1958, Shea [6] introduced the stapedial prosthesis by removing the stapes, sealing the oval window with an autograft vein wall, and then reconstructing the sound-conducting mechanism with an artificial prosthesis [7,8]. After that, Professor Henri André Martin introduced stapedotomy with the use of piston prosthesis. Nowadays, the surgical techniques used for the treatment of otosclerosis are stapedectomy, partial stapedectomy and stapedotomy with more tendencies towards the latter recently.
The aim of this study was to evaluate the success rates of stapedotomy compared to partial stapedectomy in the operative management of otosclerosis.
Materials and Methods
A retrospective chart review was performed on all patients who underwent stapes surgery in our tertiary centre in Saudi Arabia between 1997 and 2015. All patients were either operated using partial stapedectomy or stapedotomy technique using Skeetermicrodrill (SkeeterOtologic Drill System, Medtronic Xomed surgical products). The stapedotomy is performed by just creating a hole at the foot plate and inserting the piston in it, while in partial stapedectomy part of the foot plate should be removed.
All surgeries were performed by staff surgeons. Seven patients with incomplete data as well as the revision surgeries were excluded from the study. All other patients were included and the following information was gathered from their charts:
1. Demographic information: age, gender.
2. History of preoperative or postoperative vertigo.
3. Preoperative as well as postoperative pure tone audiogram, specifically the bone conduction, air conduction and the air-bone gap at the frequencies 500 H, 1 kH, 2 kH, 3 kH and 4 kH.The preoperative averages mean of the air conduction and bone conduction pure tone thresholds at frequencies 500 H to 4 kHz was compared with postoper-ative values. Preoperative air-bone gap (ABG) means at 0.5, 1, 2 and 4 kHz was also compared with postoperative values.
In addition, subjects were divided and their data was analysed according to the technique used. We consider the surgery to be successful according to the audiological results, specifically the closure of air bone gap. The postoperative ABG of both groups were compared based on classification of ABG<10 dB, ABG=10-20 dB or ABG>20 dB. Data were entered into a personal computer and analyzed by the Statistical Package for Social Sciences (SPSS) software version 11.0 (SPSS®: Inc., Chicago, IL, USA). The level of significance was set at (P ≤ 0.05).
This study was approved by the Institutional Review Board (IRB), King Saud University, College of Medicine, Riyadh. All subjects, or their legal guardian, had previously granted consent to the use of relevant data.
Results
Demographics
A total of 84 stapes surgery were performed in the period from 1997 to 2015 of which seven patients were excluded due to insufficient data. Of the 77 subjects included in the present study, 32 underwent partial stapedectomy while 45 underwent stapedotomy. The mean age was 38 years. Unexpectedly, our data showed that male patients are more than female with a ratio of 1.2/1. The left ear was more than the right one (Table 1).
Postoperative vertigo
About 6/77 (7.8%) patients complained of an immediate postoperative vertigo which has been improved within 4-6 days. Four of them underwent partial stapedectomy and two stapedotomy. By looking to the percentage of postoperative vertigo in each group, we found that 12.5% (4/32) of partial stapedectomy and 4.4% (2/45) of stapedotomy developed postoperative vertigo. Although the results demonstrate that postoperative vertigo was more evident in the partial stapedectomy group, the difference was statistically insignificant.
General audiological results
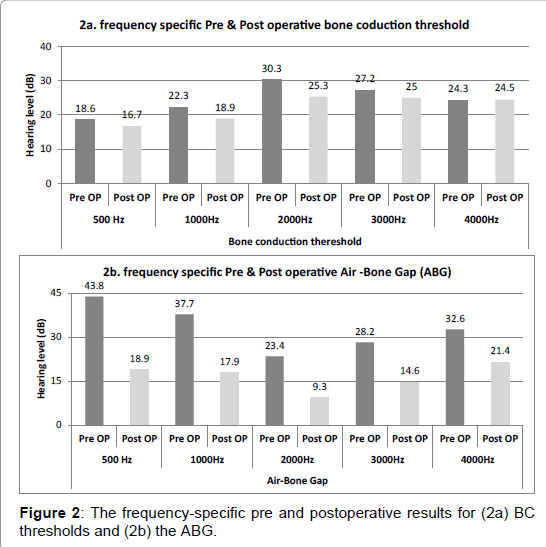
The overall audiological results showed an improvement in the air conduction (AC) and bone conduction (BC) thresholds as well as the ABG. The mean BC thresholds improved from 24.6 dB preoperatively to 22.1 dB postoperatively. The AC thresholds improved by about 19.4 dB, from the average preoperative hearing level of 57.8 dB to 38.4 dB postoperatively. The mean preoperative ABG was 33.1 dB. This has improved to 16.4dB postoperatively. Thus, a mean of 50.5% ABG closure had been achieved (Figure 1).
| Partial Stapedectomy | Stapedotomy | Total | |
|---|---|---|---|
| Subjects, n= | 32 | 45 | N=77 |
| Mean age | 37,5 years | 38,6 years | 38,2 years |
| Male/Female | M=13/F=19 | M=29/F=16 | M=42/F=35 |
| Right/Left ear | 14/18 | 21/24 | 35/42 |
| Post OP vertigo | 4/32 (12.5%) | 2/45 (4.4%) | 6/77 (7.8%) |
| Average PTA for 500-4000 Hz | Pre Post | Pre Post | Pre Post |
| AC Threshold (dB) | 55,8 37,9 | 59,2 38,7 | 57,8 38,4 |
| BC Threshold (dB) | 23,9 22,6 | 25 21,7 | 24,6 22,1 |
| ABG (dB) | 31,6 15,5 | 34,1 17,1 | 33,1 16,4 |
Table 1: Summary of demographic and audiological data.
By looking at the frequency specific results, BC thresholds were improved in all frequencies except at 4 kH where it showed a mild, statistically insignificant (p value 0.091) change from 24.3 dB preoperative to 24.5 dB postoperative. The ABG showed improvement in all frequencies, with low frequencies demonstrating better outcomes than high frequencies. The closure of ABG was statically significant at all frequencies except at 4kH was statically insignificant (p value 0.067). The maximum ABG improvement was at 500 Hz (24.9 dB), while the worst result was at 4 kH (11.2 dB) (Figures 2a and 2b).
Comparing the audiological results of partial stapedectomy vs. stapedotomy:
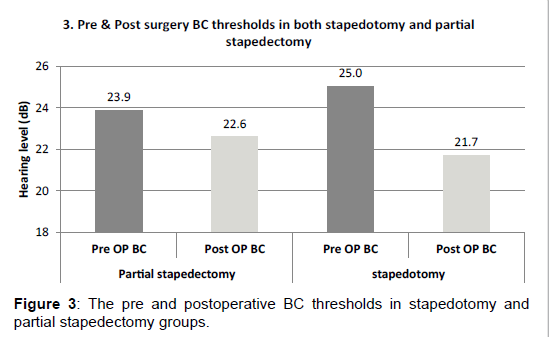
The comparison between the partial stapedectomy with stapedotomy group in term of consistence of the postoperative bone conduction, we found there was no deterioration of postoperative bone conduction rather than a mild improvement in both groups have been documented. The stapedotomy group showed a better improvement of the bone conduction than the partial stapedctomy group (Figure 3). The improvement of BC after stapedotomy found to be statistically significant at 1 k, 3 k and 4 k with p Value of 0.045, 0.001 and 0.0001, respectively.
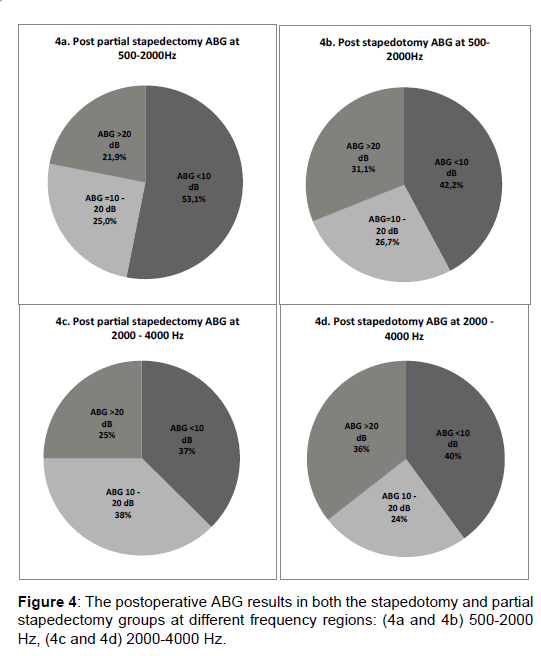
By exploring ABG closure and comparing both groups, we found that Partial Stapedectomy showed significant closure at 2 K and 3 K with p value of 0.004 and 0.031, respectively. The present study showed an interesting observation. By considering only the low frequencies (500 Hz to 2 kHz), the postoperative ABG<10 dB is documented in 53.1% and 42.2% of partial stapedectomy and stapedotomy group respectively. But when we look at the high frequency (2000 Hz–4 kHz), the postoperative ABG<10 dB is more evident in the stapedotomy group (40%) compared with partial stapedectomy group (37%) (Figures 4a-4d).
Discussion
In clinical practice otosclerosis is encountered about twice as frequently in females as in males [11,12]. In the present study, the number of male patients was higher than the female patients (42:35). However, this ratio could be misleading due to many cultural factors. Women in our society usually hesitate to attend medical service. Males however might be more concerned about their hearing than females because their hearing is a major factor at work. In our society the ratio of working females is much smaller compared to working men.
We found less post-operative vertigo following stapedotomy compared with partial stapedectomy, which is supported by previous reports who came to the same conclusion that stapedotomy is less prone to complications than stapedectomy [11,13-15]. In our study, no cases of sensorineural hearing loss documented following stapedotomy or partial stapedectomy. This has also been confirmed previously in the literature demonstrating that the postoperative sensorineural hearing loss is rare [8,11,16]. The current study confirm what has already been proven in the literature: stapes surgery has excellent audiological outcome [3,8,11,17,18].
It has been reported in previous studies that stapedotomy shows better high frequency audiological outcomes compared to stapedectomy, which is also associated with better speech discrimination in a number of publications [8,17]. The same finding is seen in the present study where the stapedotomy group showed better audiological outcome than the partial stapedectomy group, when we looked at the high frequencies (2-4 kHz).
Conclusion
Stapedotomies are more effective and a traumatic than partial stapedectomies because of better hearing results when the full range of speech frequencies (500 Hz-4000 Hz) is considered. Stapedotomy operation should be preferred owing to a lower incidence of postoperative vertigo as demonstrated in the present study.
References
- Declau F, Van Spaendonck M, Timmermans JP, Michaels L, Liang J, et al. (2001) Prevalence of otosclerosis in an unselected series of temporal bones. Otol Neurotol 22: 596-602.
- Menger DJ, Tange RA (2003) The aetiology of otosclerosis: A review of the literature. Clin Otolaryngol Allied Sci 28: 112-120.
- Bittermann AJ, Vincent R, Rovers MM, van der Heijden GJ, Tange RA, et al. (2013) A nonrandomized comparison of stapes surgery with and without a vein graft in patients with otosclerosis. Otol Neurotol 34: 827-831.
- Kessel J (1878) Ueber das Mobilisieren des Steigbugels durch Ausschneiden des Trommelfelles, Hammers und Ambosses bei Undurchgangigkeit der Tuba. Arch Ohrenh 13: 69-73.
- Rosen S (1955) Restoration of hearing in otosclerosis by mobilization of the fixed stapedial footplate: An analysis of results. Laryngoscope 65: 224-269.
- Shea JJ Jr. (1958) Fenestration of the oval window. Ann Otol Rhinol Laryngol 67: 932-951.
- Coker NJ, Duncan NO 3rd, Wright GL, Jenkins HA, Alford BR (1988) Stapedectomy trends for the resident. Ann Otol Rhinol Laryngol 97: 109-113.
- George LS (2002) Causes of conductive hearing loss after stapedectomy or stapedotomy: A prospective study of 279 consecutive surgical revisions. Otol Neurotol 23: 281-288 .
- Colletti V, Sittoni V, Fiorino FG (1988) Stapedotomy with and without stapedius tendon preservation versus stapedectomy: Long term results. Am J Otol 9: 136-141.
- Husban HA (2013) Outcome of management of otosclerosis by stapedotomy compared to stapedectomy in a Jordanian population. Oman Med J 28: 36-38.
- Morrison AW (1970) Otosclerosis: A synopsis of natural history and management. Br Med J 2: 345-348.
- Thamjarayakul T, Supiyaphun P, Snidvongs K (2010) Stapes fixation surgery: Stapedectomy versus stapedotomy. Asian Biomed 4: 429-434.
- Sakamoto T, Kikuta S, Kikkawa YS, Tsutsumiuchi K, Kanaya K, et al. (2015) Differences in postoperative hearing outcomes and vertigo in patients with otosclerosis treated with laser-assisted stapedotomy versus stapedectomy. ORL 77: 287-293.
- Hossain MD, Md. Rafiquzzaman, Ahamed NU, Asaduzzaman AKM, Md. Tauhidul Islam, et al. (2014) Surgical findings and audiological outcomes of stapedotomy in patients with otosclerosis. Bangladesh J Otorhinolaryngol 20: 87-92.
- Gokler A, Akin I, Sahan M, Sagit M, Sonbay D (2009) Stapedectomy versus stapedotomy. Int. Adv. Otol. 5: 116-117.
- Motta G, Ruosi M, Motta S (1996) Stapedotomy vs. stapedectomy. Comparison of hearing results. Acta Otorhinolaryngol Ital 16: 36-41.
- House HP, Hansen MR, Al Dakhail AA, House JW (2002) Stapedectomy versus stapedotomy: Comparison of results with long-term follow-up. Laryngoscope 112: 2046-2050.
Citation: Alzhrani F, Baqays A, Almutawa H (2017) Stapes Surgery Using Stapedotomy versus Partial Stapedectomy. Otolaryngol (Sunnyvale) 7:291. DOI: 10.4172/2161-119X.1000291
Copyright: © 2017 Alzhrani F, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 5885
- [From(publication date): 0-2017 - Aug 20, 2025]
- Breakdown by view type
- HTML page views: 4879
- PDF downloads: 1006