Sudden Sensorineural Hearing Loss After Total Thyroidectomy Surgery Under General Anesthesia
Received: 15-Jun-2016 / Accepted Date: 23-Jun-2016 / Published Date: 30-Jun-2016 DOI: 10.4172/2161-119X.1000245
Keywords: Sudden sensorineural hearing loss; Total thyroidectomy; General anesthesia
252170Introduction
Sudden sensorineural hearing loss is defined as sensorineural hearing loss of 30 dB or greater in at least three contiguous frequencies as recorded in audiometry developing within a period of three days or less. Even though many etiologic factors have been brought forward, only 10-15% of cases have had their etiologies shedlight on [1]. In most patients the sudden sensorineural hearing loss is regarded idiopathic. The approximate incidence of sudden sensorineural hearing loss is 5-20/100.000 and its potential causes that can be brought forward are infectious, autoimmune, traumatic, vascular, neoplastic, metabolic and neurologic cases. In a meta-analysis consisting of 23 idiopathic sudden sensorineural hearing loss case studies, infectious agents were reported to be the most common cause [2].
Excluding otologic interventions, sudden hearing loss is a condition that rarely occurs after surgical operations done under general anesthesia. Most of these develop after cardiopulmonary bypass surgery where extracorporeal circulation is used. In addition to this, sudden sensorineural hearing loss has been reported to develop after surgical operations with the exclusion of otologic and cardiopulmonary interventions [3].
In this case report, the clinical case of a patient diagnosed with multinodular goiter who developed unilateral sudden sensorineural hearing loss at an early postoperative stage after total thyroidectomy under general anesthesia together with a review of the literature wil be discussed.
Case Report
Our department was consulted on the case of a 43 year old female patient who developed right sided hearing loss 6-7 h after a total thyroidectomy operation. The patient affirmed to having no ear complaint and that her hearing was normal prior to the operation. Together with hearing loss the patient also complained of ear fullness without tinnitus and dizziness. The patient had no history of chronic disease or use of ototoxic drugs. The patient’s intraoperative blood pressure level, heart rate and oxygen saturation were within normal limits.
The patient’s otologic examination was unremarkable. There was no spontaneous nystagmus and fistula test was negative. The routine blood tests and electrocardiography done before the operation were normal. According to the American Society of Anesthesiologists (ASA) classification, the patient was taken to operation with a status of ASA 1 and was administered with midazolam 1-2 mg/kg, lidocaine 1 mg/kg, propofol 2 mg/kg, rocuronium 0.6 mg/kg, sevoflurane and remifentanil 0.2 mcg/kg/min. Nitrous oxide was not used during anesthesia.
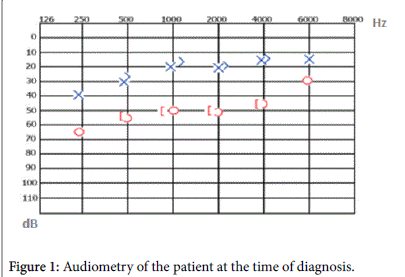
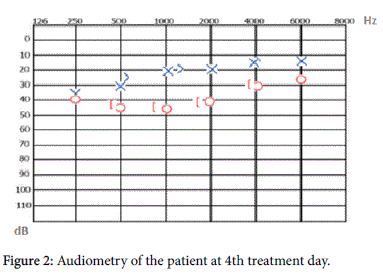
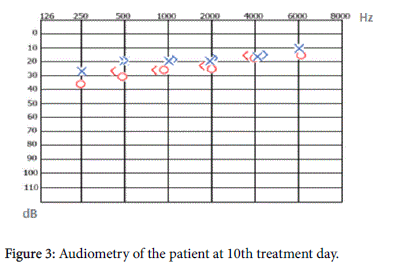
In the patient’s pure tone audiometry test a sensorineural hearing loss of 53 dB was confirmed (Figure 1) at the bone conduction thresholds. The patient was diagnosed with sudden sensorineural hearing loss and decreasing doses of systemic steroid (Metilprednizolon sodyum süksinat 1 mg/kg, terminated within three weeks with decreasing doses) and plasma volume expansion solution (dextran 40) was started. At the same time hypocalcemia was confirmed in the blood test and calcitriol medication started . The right ear audiometry test was done on the 4th day of treatment and the hearing level was found to be at 43 dB (Figure 2) at the bone conduction thresholds. However the audiometry test of both ears done on the 10th day of treatment showed the hearing levels to be within normal limits (Figure 3). The patient’s calcium level normalized 3 days after resolution of the hearing loss. The patient did not have any synthetic thyroid hormone replacement treatment between the time hearing loss developed to the time it resolved. With resolution of the hearing loss the patient was discharged and is still under follow up.
Discussion
Sudden sensorineural hearing loss is frequently encountered in ear nose and throat practice and up to date it is a well-recognized otological emergency. Even though it is a pathology that has been recognized for a long time, its etiopathogenesis and treatment is still debatable. As much as many etiologic factors have been put forward, most of the cases are idiopathic. Sudden sensorineural hearing loss that develops after surgical operations under general anesthesia are quite rare and frequently occur after otologic and coronary artery bypass surgeries. However sudden sensorineural hearing loss has also been reported to occur after other surgical interventions. Consequently not only does this condition occur under general anesthesia but also in interventions where spinal anesthesia is used.
Arenberg [4] repoted a case of sudden sensorineural hearing loss after cardiopulmonary bypass surgery in 1972. Even though the etiologic factors of sudden sensorineural hearing loss that develops under general anesthesia have been put forward, determining the exact cause is quite difficult. The potential causes include ototoxic drug use, nitrous oxide, variations in middle ear pressure, vascular pathologies, perioperative hypoperfusion, variations in cerebrospinal fluid pressure, valsalva maneuver, perilymphatic fistula, microemboli and viral infections [5,6].
Sudden sensorineural hearing loss that develops after spinal anesthesia was first reported in 1914. As sudden sensorineural hearing loss can be unilateral or bilateral, it can also occur at an early or late stage. Hearing loss that occurs during spinal anesthesia is thought to develop due to changes in cerebral spinal fluid pressure. Decrease in pressure and leakage of cerebral spinal fluid after dural puncture results in a quick decrease in perilymphatic pressure. Sudden decrease in cerebral spinal fluid can cause unmeasurable changes in endolymphatic pressure and consequently can result in reissner membrane and basilar membrane damage. As a result, changes in the position of the hair cells causes hearing loss. Moreover acute increase in cerebral spinal fluid pressure and conduction to the perilymph causing damage to the basilar membrane has been thought to result in hearing loss [6].
Microembolism is one of the most culpable factors of sudden sensorineural hearing loss that is seen after general anesthesia. Increased platelet count and platelet aggregability is thought to be a source of microembolism during the postoperative period [4]. Especially, sensorineural hearing loss that develops after cardiovascular surgery is mostly as a result of emboli particles created during cardiopulmonary bypass. The number of arterial microembolism significantly increases during extracorporeal perfusion and hearing loss is believed to be as a result of microemboli that occurs between the basilar artery and its branches to the inner ear [6].
Hearing loss that develops during anesthesia for cardiopulmonary bypass procedures has a generally bad prognosis. In most patients full recovery never occurs. This is believed to be as a result of an emboli that blocks microcirculation of the inner ear causing ischemic injury to stria vascularis and hairy cells. Sudden sensorineural hearing loss that develops after general anesthesia for procedures other than bypass surgery have relatively good prognosis. It has been reported that approximately 50% of patients have at least partial recovery. From these facts microembolism plays a very small role than expected as an etiologic factor of sudden sensorineural hearing loss after general anesthesia for interventions other than cardiopulmonary bypass surgery. For this reason, the other etiologic factors are more prominent in these patients.
The type of anesthesia used during the operation can also cause hearing loss. Nitrous oxide is one of the well-recognized agents in this field. Nitrous oxide has a dissolution of 30 folds compared to nitrogen and can therefore quickly penetrate into the middle ear and increase the pressure in the middle ear . This high pressure is directed towards the inner ear and by means of the oval and round window, can cause perilymphatic fistula resulting in sensorineural hearing loss [3,4]. For this reason, vestibular symptoms should be checked and fistula test done during the postoperative period. In our case nitrous oxide was not used during any stage of the anesthesia.
In this case sudden sensorineural hearing loss developed after total thyroidectomy operation. The total excision of thyroid gland was thought to be able to cause sudden hearing loss as it produces thyroid hormone which affects general metabolism. The effects of serum thyroid hormone levels on hearing function has been known for a long time. Both hyperfunction and hypofunction of thyroid gland can cause dynamic changes on hearing. In a cross sectional study, Oiticica et al. [7] studied the metabolic defects of 166 patients who presented with sudden hearing loss within a period of 10 years. They found that thyroid hormone levels was normal in 116 patients (78.4%) whereas in 32 patients (21.6%) it was not normal. Long periods of thyroid hormone deficiencies has been shown to cause hearing function variations in both humans and experimental animal studies. Psaltakos et al. [8] determined the hearing levels of 52 patients who had undergone total thyroidectomy using pure tone audiometry and transient evoked otoacoustic emission before and 6-8 weeks after the operation. The patients were not given levothyroxine and Thyroid Stimulating Hormone(TSH) was monitored during the postoperative period. An increase in all of the hearing levels was noted in the postoperative audiometry and the S/N ratio on otoacoustic emission was seen to be lower in the postoperative period compared to the preoperative period. On the contrary, Mra and Wax [9] did not find any changes on audiogram and otoacoustic emission during the 6 week period of acute thyroxin depletion after total thyroidectomy. Whereas in our case hearing loss developed at an early postoperative period (~ 6 h) after total thyroidectomy and taking into account the half life of thyroid hormone we came to the conclusion that hypothyroidism could not be an etiologic factor in this case.
Hypocalcemia whether symptomatic or asymptomatic is frequently seen after thyroid surgery and even though most cases resolve spontaneously it can be permanent in conditions where parathyroid gland is damaged. Sensorineural hearing loss is a less known sign of hypoparathyroidism. In a study on 20 idiopathic hypoparathyroidsm patients, pure tone audiometry was done and bilateral sensorineural hearing loss found in 15% of the patients and this hearing loss was thought to be as a result of long periods of low calcium levels in the inner ear fluids [10]. In our case while the preoperative calcium levels were normal, hypocalcemia developed at the same postoperative period as hearing loss.
Even though there were no signs of hypocalcemia on physical examination of the patient, calcitriol treatment was started and on approximately the 10th postoperative day calcium levels normalized. Hearing loss and hypocalcemia developed at the same period whereas hearing loss resolved 3 days before calcium levels normalized. For this reason this patient’s hearing loss most probably did not occur as a result of sudden changes in calcium level.
We have presented a rare case of sudden sensorineural hearing loss in this case report. Sudden sensorineural hearing loss has been reported to occur after many different operations under general anesthesia. Even though many etiologic factors have been put forward in these patients, generally a definite factor is not clear. In this study occurance of metabolic changes that can cause hearing loss in the postoperative period is seen in patients undergoing endocrine surgery under general anesthesia however it was found that the patient’s hearing loss was not in a correlated progression with these factors. The patient’s TSH levels gradually increased in the postoperative period but the hearing levels resolved to normal limits. Similarly hearing resolved before calcium levels came within normal limits. In the period when hearing had normalized hypocalcemia was still present.
Conclusion
Sudden sensorineural hearing loss is a rare condition that develops after surgical interventions under general and spinal anesthesia. For this reason patients should be informed before the operation and awareness should be created by educating anesthesiologist, surgeons and assisting health personnels.
References
- Oiticica J, Bittar RS (2010) Metabolic disorders prevalence in sudden deafness. Clinics (Sao Paulo) 65: 1149-1553.
- Kuhn M, Heman-Ackah SE, Shaikh JA, Roehm PC (2011) Sudden sensorineural hearing loss: a review of diagnosis, treatment, and prognos is. Trends Amplif 15: 91-105.
- Pau H, Selvadurai D, Murty GE (2000) Reversible sensorineural hearing loss after non-otological surgery under general anaesthetic. Postgrad Med J 76: 304-306.
- Evan KE, Tavill MA, Goldberg AN, Silverstein H (1997) Sudden sensorineural hearing loss after general anesthesia for nonotologic surgery. Laryngoscope 107: 747-752.
- Girardi FP, Cammisa FP Jr, Sangani PK, Parvataneni HK, Khan SN, et al. (2001) Sudden sensorineural hearing loss after spinal surgery under general anesthesia. J Spinal Disord 14: 180-183.
- Sprung J, Bourke DL, Contreras MG, Warner ME, Findlay J (2003) Perioperative hearing impairment. Anesthesiology 98: 241-257.
- Narozny W, Kuczkowski J, Mikaszewski B (2006) Thyroid dysfunction-underestimated but important prognostic factor in sudden sensorineural hearing loss. Otolaryngol Head Neck Surg 135: 995-996.
- Psaltakos V, Balatsouras DG, Sengas I, Ferekidis E, Riga M, et al. (2013) Cochlear dysfunction in patients with acute hypothyroidism. Eur Arch Otorhinolaryngol 270: 2839-2848.
- Mra Z, Wax MK (1999) Effects of acute thyroxin depletion on hearing in humans. Laryngoscope 109: 343-350.
- Garty BZ, Daliot D, Kauli R, Arie R, Grosman J, et al. (1994) Hearing impairment in idiopathic hypoparathyroidism and pseudohypoparathyroidism. Isr J Med Sci 30: 587-591.
Citation: Aricigil M, Yucel A, Alan MA, Aydemir F, Aziz SK (2016) Sudden Sensorineural Hearing Loss After Total Thyroidectomy Surgery Under General Anesthesia. Otolaryngol (Sunnyvale) 6:245. DOI: 10.4172/2161-119X.1000245
Copyright: © 2016 Arıcıgil M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 16174
- [From(publication date): 6-2016 - Jun 30, 2025]
- Breakdown by view type
- HTML page views: 15160
- PDF downloads: 1014