The Kaleidoscope of the Operative Solutions for Hearing Restoration in Charge Syndrome: A Critical Review
Received: 09-Jun-2017 / Accepted Date: 19-Jun-2017 / Published Date: 26-Jun-2017 DOI: 10.4172/2161-119X.1000309
Abstract
Exclusively full texts, cited in PUBMED and MEDLINE search engines, that contain all the selected keywords “Charge syndrome”, “cochlear implant”, “cochlear implantation”, “bionic ear” and “ear malformation” have been selected to review the literature on surgical bionic hearing restoration in CHARGE syndrome. A total of 20 publications that specifically deal with the topic have been published between January 1999 and February 2017. At least ten main different otologic and oto-neurosurgical approaches have been suggested in bionic fitting. The otologic approaches were aided by a microscope or an endoscope or by a combined technique, with or without mastoidectomy. The review is conclude by proposing a strategy for the surgical bionic treatment of hearing in children with CHARGE syndrome.
Introduction
Children affected by CHARGE syndrome usually show hearing loss (conductive, sensorineural or mixed) with choanal atresia, abnormal ossicles and cochlear hypoplasia, absent semicircular canals (particularly lateral) [1] and cranial nerve deficiencies, that involve the vestibular, cochlear, facial and olfactory nerves [2].
A kaleidoscope of surgical approaches have been utilized in literature to overcome the several problems and risks of cochlear implantation, a solution frequently proposed in these patients in order to ameliorate the hearing loss. [3]
The purpose of this paper is to outline the panorama of surgical techniques used for positioning a bionic device in children with CHARGE syndrome. The pros and cons of the different surgical techniques are critically evaluated.
Microscopic Technique
Surgical techniques proposed in literature and utilizing a microscope can include or avoid a mastoidectomy:
(1) House [4] proposed mastoidectomy with posterior tympanotomy, opening of the middle ear through the facial recess to reach the round window (RW) region and perform the cochleostomy to insert the array of the cochlear implant (CI).
(2) Kronenberg et al. [5] suggested a suprameatal route through a retroauricular tympanotomy without mastoidectomy.
(3) The ‘‘Veria’’ operation [6] avoids mastoidectomy. The cochleostomy is performed through an endaural approach, while the CI array is inserted with a supero-posterior approach. A modification of this technique has been proposed by Hausler [7] with the insertion of the array through the external auditory canal (EAC).
(4) A percutaneous CI technique has been developed with access from the mastoid through the facial recess to the cochlea by using customized drill guides based on imaging studies [8].
(5) The combined approach technique modifies the classic approach proposed by House [4], using a transcanal approach for the cochleostomy, combined with a small mastoidectomy and a small posterior tympanotomy to insert the array [9].
(6) Subtotal petrosectomy has also been suggested in combination with cochlear implantation [10].
(7) The middle cranial fossa (MF) approach, which avoids middle ear opening, was proposed by Colletti et al. [11]. After adequate exposure of the MF floor, a triangular bony area between the greater superficial petrous nerve and the projection of the labyrinthine portion of the facial nerve (FN) has to be drilled out to face the basal cochlear turn. Then through the cochleostomy the electrode carrier is inserted into the cochlea.
(8) An auditory brainstem implant (ABI) has also been suggested to be fitted in the lateral recess of the IV ventricle through the foramen of Luschka [12].
Endoscopic Technique
The endoscopic technique has been introduced in CI surgery [13] to permit a direct vision of the hidden malformed auditory structures and to perform a safe cochleostomy for the insertion of the array.
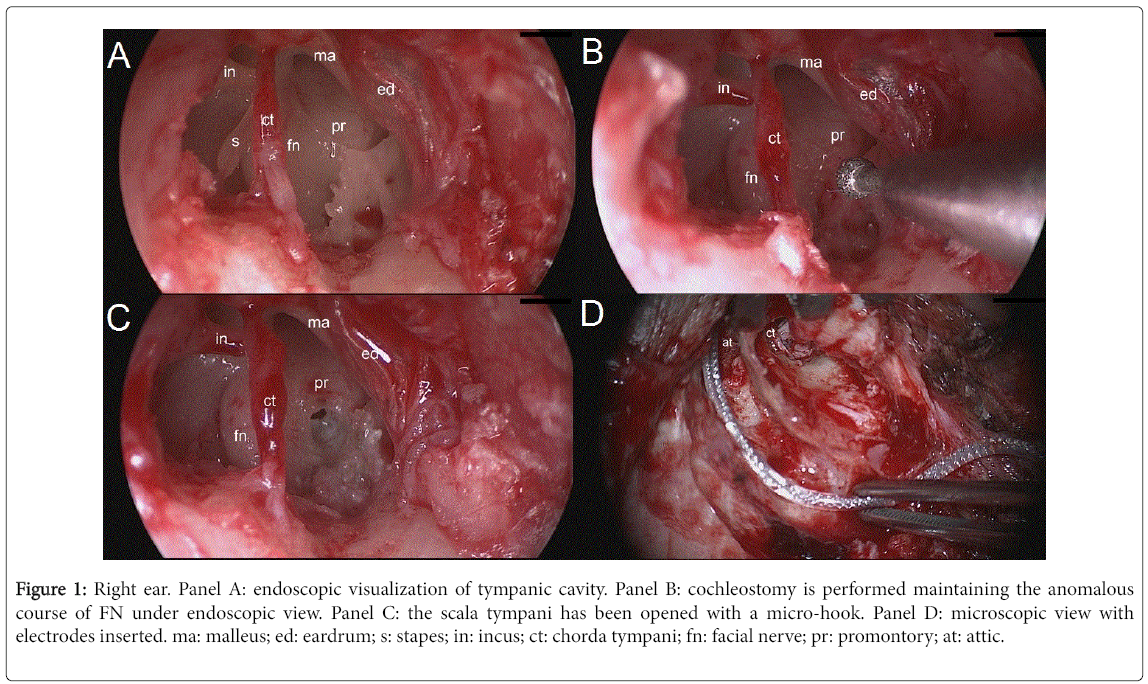
An innovative combined microscopic/endoscopic technique, named endoscopic assisted approach, has been very recently introduced to treat hearing loss in patients with ear malformations in CHARGE syndrome [14]. This technique permits a direct magnification of the middle ear structures, even in case of anomalous course of the FN (Figure 1), that sometimes may hide the RW niche.
Figure 1: Right ear. Panel A: endoscopic visualization of tympanic cavity. Panel B: cochleostomy is performed maintaining the anomalous course of FN under endoscopic view. Panel C: the scala tympani has been opened with a micro-hook. Panel D: microscopic view with electrodes inserted. ma: malleus; ed: eardrum; s: stapes; in: incus; ct: chorda tympani; fn: facial nerve; pr: promontory; at: attic.
The different surgical approaches proposed in literature with their benefits and drawbacks are summarized in Table 1.
| Surgery | Technique | Benefits | Drawbacks |
|---|---|---|---|
| Microscopic with Mastoidectomy | Posterior tympanotomy [4] | Most commonly used approach: mastoidectomy with posterior opening of middle ear through the facial recess to expose RW | Risk of injury to the facial nerve and to chorda tympani |
| Combined approach [9] | Transcanal approach for cochleostomy, small mastoidectomy and posterior tympanotomy | Risk of injury to the facial nerve and to chorda tympani | |
| Subtotal petrosectomy [10] | Blind sac closure of the EAC, closure of Eustachian tube, abdominal fat obliteration in combination with cochlear implantation | Higher risk of post-operative complications. Radical surgery limited to patients with chronic suppurative otitis media or existing mastoid cavities | |
| Microscopic without Mastoidectomy | Suprameatal route [5] | Introduction of the electrode through a retroauricolar tympanotomy; FN is protected by the incus | Presence of low-lying dura; stretching of the electrode during the insertion; difficult RW visualization and inferior cochleostomy |
| “Veria” procedure [6] | Endaural approach for cochleostomy, supero-posterior approach for the electrode | Specific surgical instrumentation required | |
| Endoaural approach [7] | Direct insertion of the electrode through the EAC | Difficult RW visualization and antero-inferior cochleostomy | |
| Percutaneous CI technique [8] | Access from the mastoid to the cochlea through the facial recess; use of customized drill guides manufactured on the basis of preintervention radiological studied | Intra-operative CT scan requires; markers in the bone to plan a safe drill trajectory | |
| Middle cranial fossa approach [11] | Avoids middle ear opening. Exposure of MF floor; a limited bony area is drilled out to face the basal cochlear turn | Difficult surgery; high risk of FN damage and major complications | |
| Auditory brainstem implant [12] | Fitted in the lateral recess of the IV ventricle through the foramen of Luschka | Poor auditory outcomes; high risk of major neurological complications. Limited to patient with cochlear nerve aplasia | |
| Endoscopic with Mastoidectomy | Endoscopic assisted CI procedure [14] | Safe cochleostomy performed through endoscopic approach; magnification of middle ear structures (RW); strict control on FN course. Mastoidectomy and posterior tympanotomy | Learning curve, careful hemostasis of operative field |
| Endoscopic without Mastoidectomy | Endoscopic CI procedure [13] | Endoscopic magnification of middle ear structures (RW), intramastoid tunnel for the electrode | Learing curve, careful hemostasis of operative field |
Table 1: Surgical approaches proposed in literature with their benefits and drawbacks.
Discussion
Many surgical bionic procedures have been proposed in literature for CI in CHARGE syndrome to try to overcome the challenging and high risk rate surgery due to the several anatomical malformations that may be present in every structure of the auditory system.
Main surgical risks
The frequent anomalous course of FN observed in CHARGE syndrome explains the very high risk of damaging it [15].
Another important anatomical detail is related to the RW access, not only difficult, but sometimes impossible to perform with microscopic techniques due to the FN course that obscure it or due to an abnormal conformation of the niche area [16].
In these conditions, the identification of the RW region and the control of the FN course could be very difficult to obtain with the traditional microscopic technique, as reported in literature [3].
In this population, the correct exposure of the anatomical structures of the middle ear is crucial for correct array placement with the optimal electrode carrier vector and best cochlear location [17] and for the control of the high risk of gusher [18].
Critical review of the surgical solutions
Nowadays, the most commonly used technique in CI surgery consists of posterior tympanotomy with mastoidectomy with the aid of a microscope. The major complications reported are mainly due to the need to perform mastoidectomy and to drill the posterior tympanic space to access the middle ear cavity and RW [1]. Although the microscope provides multiplanar visualization of the anatomical spaces, it often does not allow a complete and direct visualization of the RW membrane. In case of narrow tympanotomy, the maneuver for electrode positioning can be very laborious and may cause damage to FN, to the ossicular chain or to tympanic membrane and chorda tympani.
The advantages of the suprameatal approach [5] are well known: preservation of the mastoid without damage of the mucosa and scar tissue in the mastoid cavity; safe distance between the FN and the suprameatal tunnel reducing FN and chorda tympani injures; surgical procedure feasible even when important surgical landmarks, i.e. lateral semicircular canal and incus, are absent.
Despite these advantages there are some controversial issues reported in literature for this surgical approach. The main criticism is that the insertion of the electrode into the scala tympani takes place without direct visualization of the scala tympani, precluding observation of its status. Thus, in case of malformations of middle and/or inner ear the surgical procedure may be ineffective and sometimes unsafe.
The ‘‘Veria’’ operation [6] has the disadvantage that specific surgical instrumentation is required. The procedure proposed by Hausler [7], with direct electrode insertion through the EAC without mastoidectomy, often is not able to guarantee a wide visualization of the RW and the execution of inferior cochleostomy remains very difficult.
The percutaneous CI technique needs intra-operative CT scan; moreover markers in the bone have to be placed to plan a safe drill trajectory [8].
The combined approach technique, as the posterior tympanotomy, does not permit to reduce the risk of FN and chorda tympani damage [9].
Free et al. [10] suggested to perform subtotal petrosectomy in middle ear malformations to help identify available landmarks and to reduce the risk of developing meningitis. This procedure is indicated with chronic suppurative otitis media or existing mastoid cavities [8], but can be complicated by important subcutaneous collection of cerebrospinal fluid (CSF).
Lesser et al. [19] stated that cochlear implantation through the MF is challenging even for experienced surgeons, as it requires a highly precise technique with limited operative field; anatomical landmarks identification is difficult and the risk of FN damage is high. They affirmed that this approach should not be considered the first choice for patients that can be managed with a more traditional insertion route.
The poor auditory outcomes obtained (CAP 1-2) in patients treated with an ABI and the high risk of major neurological complications observed with this approach limit nowadays its use only in children with cochlear nerve aplasia [20].
The improved knowledge of endoscopic middle ear anatomy, particularly of the RW niche [13], has led to develop this new surgical route for CI positioning without mastoidectomy and with the exclusive use of 0° endoscope. It has the important advantage to directly visualize the posterior and anterior bony pillar of the RW niche, the fustis and the RW membrane.
The endoscopic magnification permits a “safe” insertion of the array through the RW membrane into the scala tympani with less drilling of the niche; moreover it permits a direct view of the basal turn of the cochlea.
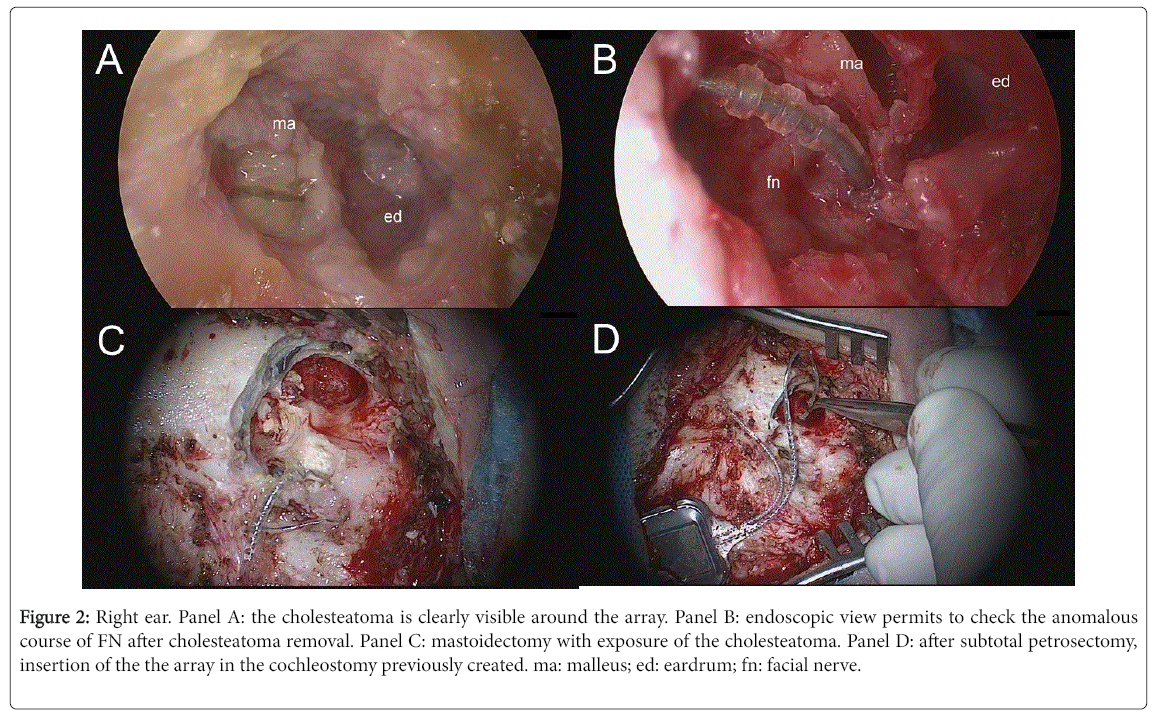
The innovative endoscopic assisted technique [14] allows always to clearly see the structures of the tympanic cavity, as the course of FN, even when anoumalous. It permits to overcome the difficulties due to the anatomical distortion of the auditory structures in children with CHARGE syndrome and allows always to maintain under direct control the anatomical landmarks into the tympanic cavity, as the position of the FN, the RW membrane and the scala tympani, in order to reduce the risk of injuries (Figure 1). This technique is very promising also for revision surgery; Figure 2 shows an example of CI revision surgery for secondary cholesteatoma performed in a patient affected by Charge syndrome. The cholesteatoma had caused the extrusion of the array and a wide erosion of scutum and posterior wall of EAC.
Figure 2: Right ear. Panel A: the cholesteatoma is clearly visible around the array. Panel B: endoscopic view permits to check the anomalous course of FN after cholesteatoma removal. Panel C: mastoidectomy with exposure of the cholesteatoma. Panel D: after subtotal petrosectomy, insertion of the the array in the cochleostomy previously created. ma: malleus; ed: eardrum; fn: facial nerve.
The main cons consist of the time necessary to learn the use of this one-handed technique and require to perform a careful hemostasis for a clean operative field.
Conclusion
This review provides useful informations for clinicians making decisions about cochlear implantation in children with ear malformations associated to CHARGE syndrome and gives a “literature based” counselling to patients and their families about prognosis.
A preoperative radiological evaluation is mandatory. MRI parasagittal scanning of IAC delineates size and conformation of auditory nerves; temporal bone CT scans highlight the course of FN and show the anatomical landmarks of middle and inner ear. Radiological evaluation, together with clinical and audiological statement, will help the surgeon choose the best surgical approach.
Endoscopic assisted approach permits to check directly the anatomical auditory distorted structures and even in the most complex conditions it assures a correct cochleostomy, followed by the best scalar location of the array in the cochlea using a microscope.
Conflict of Interest
All of the authors have read and approved the manuscript. None of them have any financial relationship to disclose.
References
- Rodriguez K, Shah RK, Kenna M (2007) Anomalies of the middle and inner ear. Otolaryngol Clin North Am 40: 81-96, vi.
- Carner M, Colletti L, Shannon R, Cerini R, Barillari M, et al. (2009) Imaging in 28 children with cochlear nerve aplasia. Acta Otolaryngol 129: 458-461.
- Birman CS, Brew JA, Gibson WP, Elliott EJ (2015) CHARGE syndrome and cochlear implantation: Difficulties and outcomes in the pediatric population. Int J Pediatr Otorhinolaryngol 79: 487-492.
- Kronenberg J, Migirov L, Dagan T (2001) Suprameatal approach: New surgical approach for cochlear implantation. J Laryngol Otol 115: 283-285.
- Kiratzidis T, Iliades T, Arnold W (2002) Veria Operation. II. Surgical results from 101 cases. ORL J Otorhinolaryngol Relat Spec 64: 413-416.
- Hausler R (2002) Cochlear implantation without mastoidectomy: The pericanal electrode insertion technique. Acta Otolaryngol 122: 715–719.
- Warren FW, Balachandran R, Fitzpatrick JM, Labadie RF (2007) Percutaneous cochlear access using bone-mounted, customized drill guides: Demonstration of concept in vitro. Otol Neurotol 28: 325–329.
- Lavinsky L, Lavinsky-Wolff M, Lavinsky J (2010) Transcanal cochleostomy in cochlear implantation: Experience with 50 cases. Cochlear Implant Int 11: 228–232.
- Free RH, Falcioni M, Di Trapani G, Giannuzzi AL, Russo A, et al. (2013) The role of subtotal petrosectomy in cochlear implant surgery--a report of 32 cases and review on indications. Otol Neurotol 34: 1033-1040.
- Colletti V, Fiorino FG, Carner M, Pacini L (1998) Basal turn cochleostomy via the middle fossa route for cochlear implant insertion. Am J Otol 19: 778-784.
- Colletti V, Carner M, Fiorino F, Sacchetto L, Pacini L (2002) Hearing restoration with auditory brainstem implant in three children with cochlear nerve aplasia. Otol Neurotol 23: 682-693.
- Marchioni D, Grammatica A, Alicandri-Ciufelli M, Genovese E, Presutti L (2014) Endoscopic cochlear implant procedure. Eur Arch Otorhinolaryngol 271: 959-966.
- Marchioni D, Carner M, Soloperto D, Sacchetto A, Genovese E, et al. (2017) Endoscopic-assisted cochlear implant procedure in CHARGE syndrome: Preliminary report. Acta Oto-Laryngologica Case Report 2: 52-58.
- Zheng Y, Schachern PA, Djalilian HR, Paparella MM (2002) Temporal bone histopathology related to cochlear implantation in congenital malformation of the bony cochlea. Otol Neurotol 23: 181-186.
- Leong AC, Jiang D, Agger A, Fitzgerald-O'Connor A (2013) Evaluation of round window accessibility to cochlear implant insertion. Eur Arch Otorhinolaryngol 270: 1237–1242.
- O’Connell BP, Hunter JB, Wanna GB (2016) The importance of electrode location in cochlear implantation. Laryngoscope Investig Otolaryngol 1: 169-174.
- Mylanus EA, Rotteveel LJ, Leeuw RL (2004) Congenital malformation of the inner ear and pediatric cochlear implantation. Otol Neurotol 25: 308-317.
- Lesser JC, Brito Neto RV, Martins GS, Bento RF (2017) Cochlear implantation through the middle fossa approach: A review of related temporal bone studies and reported cases. Int Arch Otorhinolaryngol 21: 102-108.
- Lundin K, Stillesjö F, Nyberg G, Rask-Andersen H (2016) Experiences from auditory brainstem implantation (ABIs) in four pediatric patients. Cochlear Implants Int 17: 109-115.
Citation: Marchioni D, Carner M, Soloperto D, Sacchetto A, Genovese E, et al. (2017) The Kaleidoscope of the Operative Solutions for Hearing Restoration in Charge Syndrome: A Critical Review. Otolaryngol (Sunnyvale) 7:309. DOI: 10.4172/2161-119X.1000309
Copyright: © 2017 Marchioni D, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 3902
- [From(publication date): 0-2017 - Aug 30, 2025]
- Breakdown by view type
- HTML page views: 2981
- PDF downloads: 921