The Silent Sinus Syndrome: A Collaborative Approach between Rhinologists and Oculoplastics- Case Report and Literature Review
Received: 03-Nov-2014 / Accepted Date: 22-Nov-2014 / Published Date: 30-Nov-2014 DOI: 10.4172/2161-119X.1000179
Abstract
The Silent Sinus Syndrome (SSS) is a rare phenomenon originally described in 1964 by Montgomery, which often occurs unilaterally in the maxillary sinus with opacification and collapse. It is characterized by ipsilateral enophthalmos and hypoglobus or mistakenly as an exophthalmos of the contralateral eye. The pathophysiology is caused by obstruction of the ostiomeatal complex with subsequent maxillary sinus hypoventilation and development of negative intra-sinus pressure resulting in bony changes and sinus collapse. Radiographic evaluation by the mean of CT scan orbits and paranasal sinuses as well as nasal endoscopic examination are mandatory in diagnosing such cases. Treating such cases require a collaborative multidisciplinary approach to ensure the best possible results. In this case report, we discuss this rare phenomenon in terms of clinical presentation, clinical and radiological evaluation and conclude with the optimal treatment approach.
Keywords: Silent sinus syndrome; Enophthalmos; Hypoglobus; Ostiomeatal complex; Maxillary sinus
258874Introduction
Silent Sinus Syndrome (SSS) is a rare clinical disorder that is typically characterized as spontaneous, painless, progressive enopthalmos and hypoglobus. It results from downward bowing of the orbital floor secondary to maxillary sinus collapse, in the absence of any symptoms of sinonasal disease [1]. In 1964, Montgomery was the first to present and publish two cases of unilateral enopthalmos and hypoglobus associated with ipsilateral maxillary sinus collapse; however, SSS term was only used 30 years later by Soparkar and colleagues [1,2]. Interestingly, the term imploding antrum is another term used for silent sinus syndrome in literatures review [3]. Recent to this in 2008, Brandt and wright suggested SSS to be included under the general term of chronic maxillary atelectasis [4]. It has been noticed that increasing numbers of case reports were published on SSS recently, which could be explained by the widespread use of Computed Tomography (CT) and endoscopic interventions in diagnosing such cases. This case report will illustrate the clinical and the imaging features of this rare phenomenon. Our aim from this report is to emphasize in the collaborative approach required to manage such patients with this syndrome. Additionally, this report will highlight the significance of rare but not to be missed differential diagnosis in any unexplained enophthalmos, hypoglobus or even exphthalmos.
Case Report
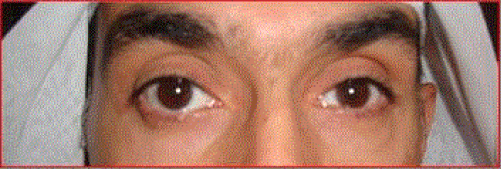
A 47-year-old, previously healthy, Caucasian presented to the orbital and oculoplastic clinic complaining of 2 weeks duration of occasional binocular vertical diplopia associated with right eye exophthalmos. On further questioning the patient, he denied having pain, loss of vision, rhinorrhea or any history of facial trauma. Moreover, he denied any past ophthalmic or sino-nasal surgeries. Careful ophthalmic examination revealed his Best -Corrected Visual Acuity (BCVA) to be 20/25 of the Right Eye (RE) and 20/30 of the Left Eye (LE). Exophthalmometer measurement of the RE was 17 mm compared to 14 mm for the LE (3 mm difference) and facial asymmetry was noticed. Full ocular movements were intact with normal findings on anterior and posterior segments’ examination. Initial diagnosis was RE exophthalmos; hence, thyroid function test was ordered with 3 weeks follow-up appointment given. The patient was seen in the follow-up visit but this time with new symptoms and complaints (Figure 1) as follow:
• More diplopia in primary gaze.
• Worse proptosis (4 mm) of the RE
• More pronounced facial asymmetry.
• Deep upper lid sulcus of the LE
• LE hypoglobus.
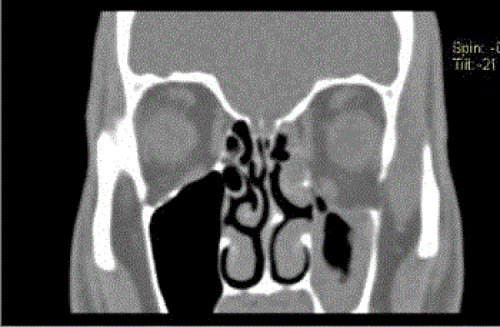
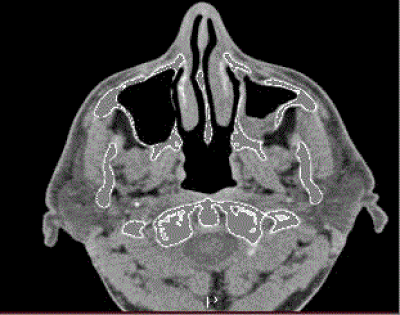
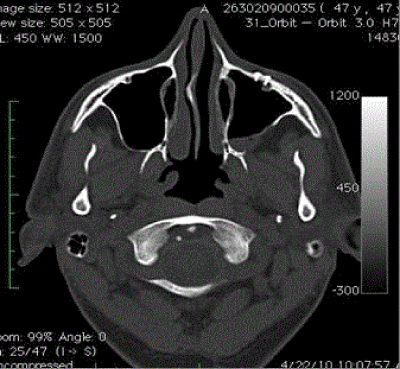
Consequently, axial and coronal CT scan images of the orbits and paranasal sinuses (Figures 2 and 3) were ordered. Radiological findings showed partial opacification of the left maxillary sinus with reduced maxillary sinus volume and ipsilateral globe prolapse associated with almost complete bony resorption of the left orbital floor. All of these findings were consistent with the diagnosis of Silent Sinus Syndrome.
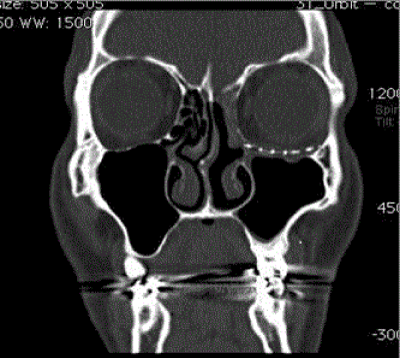
To ensure the best possible outcomes, the decision was made to do Combined Functional Endoscopic Sinus Surgery (FESS) with orbital floor reconstruction under the same anaesthesia and the same surgical table in a teamwork approach. FESS, in the form of uncinectomy and middle meatal antrostomy was performed. The left maxillary sinus was filled with secretions and polypoidal mucosa. Following the rhinologist’s intervention, oculoplastic took over performing anterior orbitotomy via transconjuctival approach with lateral canthatomy-cantholysis. Due to significant orbital floor loss, a Synpor titanium mesh 43 mm (radius) X 15 mm was fashioned and implanted to support the globe inferiorly. The histopathological examination showed non-specific chronic inflammation within the sinus mucosa. Bacterial and fungal cultures were negative. The patient was followed up for 12 months and showed dramatic improvement of the initially reported symptoms and signs. The patient reported no diplopia and thorough ophthalmic examination revealed good restoration of the upper lid sulcus with no signs of enopthalmos or hypoglobus (Figures 4 and 5) show almost normal maxillary sinus volume with restored orbital architecture supported by the titanium mesh implant in the left orbital floor.
Discussion
Upon reviewing literatures, several case reports have explained different presentations of this phenomenon; however, they all shared the combination of enophthalmos and hypoglobus in the presenting complaint. Due to its insidious course of presentation with no linked past history; SSS poses diagnostic challenge to otolaryngologists, ophthalmologists as well as general practitioners. When Soparkar et al. published his observations of SSS; only 30% of the cases had past history of sinus disease in childhood [5]. SSS is found to affect adults between the third and the fifth decades of life with no gender variation [4]. Additionally, experts of this phenomenon have found no association between smoking, alcohol consumption and genetics with the development of this rare syndrome [6]. The most common reported complaint to an ophthalmologist is changes to the facial appearance experienced by the patient or noticed by friends or family members [7]. It presents typically as unilateral asymmetry and can be sometimes misinterpreted as exophthalmos of the contralateral eye. According to Stevens et al. [3], approximately 50% of patients with enophthalmos are initially referred to ophthalmologists for investigations of contralateral exophthalmos or ptosis. Other presenting symptoms include lid lag, lagophthalmos, oscillopsia and transient vertical diplopia [8]. While enophthalmos is present in all cases, diplopia occurs in about one - quarter and it is typically vertical and painless [7,9]. These orbital symptoms can suggest a possible neuro-opthalmic disorder; however, the presence of enophthalmos with hypoglobus in previously healthy patients will narrow the differential diagnosis towards Silent sinus syndrome. In order to diagnose SSS; other causes that might present with similar symptoms must be ruled out first such as Horner’s syndrome, facial hemiatrophy, developmental anomalies or any past history of facial trauma [10]. In our case, the history was negative for the mentioned above disorders and his endocrine and autoimmune markers were negative too. Many theories have explained the pathophysiological process of this disease with varying degrees of evidence in literature. Gillman et al. in 1999 described the most acceptable theory behind the disease process [11]. Gillman et al. suggested that in SSS patients, obstruction of the Ostio Meatal Complex (OMC) leads into hypoventilation of the maxillary sinus with the subsequent development of intra-sinus negative pressure and thinning of the sinus wall. This chronically causes remodeling and bone resorption of the orbital floor causing malposition of the ipsilateral eye. Although this theory is widely accepted among observers of this phenomenon; however, no one yet knows the reason behind OMC obstruction [4]. Radiographic evaluation by the mean of CT scan orbits and paranasal sinuses is crucial to assess the anatomy of orbito-maxillary sinus structure and is mandatory upon labeling patients with such a disease.
| Diagnosis | Value |
|---|---|
| Enopthalmos | ranging from 1-6mm |
| Hypoglobus | ranging from 0 -6mm |
| Lid retraction Deeping of superior sulcus Exophthalmos |
mistakenly diagnosed |
Table 1: Shows most clinical manifestations of SSS.
CT scan findings show opacification (complete or partial) of the maxillary sinus and collapse with inferior bowing of the orbital floor towards affected maxillary sinus [12]. Cobb et al. further explains CT scan findings by linking the pathophysiological process to the radiological findings, ‘the maxillary sinus roof loses its normal upward convexity and the orbital floor is bowed downwards giving the appearance of reduced sinus volume with increased orbital volume’. This orbital volume expansion causes horizontal displacement of the eye level appearing as hypoglobus. Treating such cases require a collaborative multidisciplinary approach to ensure the best possible results. It involves the input of rhinology, oculoplastics as well as anesthesia with the availability of good nursing team in the operating theatre. Treatment from the otolaryngology points of view is aimed in restoring drainage and maintaining good aeration of the occluded maxillary sinus. Traditionally, the Caldwell-Luc procedure used to be the gold standard in treating such cases; however, this has been complicated by adhesions that cause stagnation of mucus clearance with re-obstruction of the maxillary sinus outlet [13]. Nowadays this approach was replaced by performing endoscopic maxillary antrostomy and uncinectomy with the aim of enlarging the maxillary ostium [10]. In many cases where the bony orbital floor is intact, the ENT intervention will be sufficient in restoring the sinus obstruction as well as orbital misalignment associated with ipsilaterally. Some publishers argue that it is advised to do Functional Endoscopic Sinus Surgery (FESS), then use the approach of ‘wait and see’ for few months to assess the need for oculoplastic intervention [14]. However, in our case, due to the extensive bony resportion of the left orbital floor with the poor inferior support of the orbital globe seen in the CT scan (Figures 2 and 3), the decision was made to do combined FESS with orbital floor repair. According to Cobb et al. reconstruction can be simultaneous or delayed to reduce the risk of visual loss or infection. Nevertheless, our combined approach yielded in rapid alleviation of symptoms as well as symmetrical cosmetic outcomes reported by our patient. When surgical intervention is required, otolaryngologists take over firstly to perform FESS then oculoplastic surgeons involve in intervening with orbital floor. The use of titanium mesh fixed with Leibinger screws is the preferred material in reconstructing and maintaining the normal orbital architecture, classically through transconjunctival or external lower lid approaches [4,15]. Again, it is important to emphasis that the decision to perform both combined procedures should take the teamwork approach with the patient’s view took in great consideration while weighing up the risks and benefits of such a decision.
Conclusion
Silent sinus syndrome is rare and often misdiagnosed pathology with a unilateral progressive and asymptomatic collapse of the maxillary sinus. The pathogenesis is not completely understood but appears to result from maxillary sinus collapse due to acquired obstruction of the maxillary sinus drainage. CT scan is usually required for a definite diagnosis. Treatment of such a disease consists of restoration of maxillary sinus aeration and reconstruction of the orbital floor in case needed. Any unexplained enophthalmos especially if associated with hypoglobus should hint for silent sinus syndrome as a differential diagnosis.
References
- Soparkar CN, Patrinely JR, Cuaycong MJ, Dailey RA, Kersten RC, et al. (1994) The silent sinus syndrome. A cause of spontaneous enophthalmos. Ophthalmology 101: 772-778.
- Montgomery Ww (1964) Mucocele of the Maxillary Sinus Causing Enophthalmos. Eye Ear Nose Throat Mon 43: 41-44.
- Stevens K, Omer S, Toocaram B, Rich P, Almemar A (2010) The imploding antrum syndrome: an unusual cause of double vision. PractNeurol 10: 101-104.
- Cobb AR, Murthy R, Cousin GC, El-Rasheed A, Toma A, et al. (2012) Silent sinus syndrome. Br J Oral MaxillofacSurg 50: e81-85.
- Hobbs CG, Saunders MW, Potts MJ (2004) Spontaneous enophthalmos: silent sinus syndrome. J LaryngolOtol 118: 310-312.
- Wang XR, Zhao XD (2004) Secondary silent sinus syndrome: case report. Chin Med J (Engl) 117: 785-786.
- Numa WA, Desai U, Gold DR, Heher KL, Annino DJ (2005) Silent sinus syndrome: a case presentation and comprehensive review of all 84 reported cases. Ann OtolRhinolLaryngol 114: 688-694.
- Borruat FX, Jaques B, Durig J (1999) Transient vertical diplopia and silent sinus disorder. J Neuroophthalmol 19: 173-175.
- Rose GE, Sandy C, Hallberg L, Moseley I (2003) Clinical and radiologic characteristics of the imploding antrum, or "silent sinus," syndrome. Ophthalmology 110: 811-818.
- Bossolesi P, Autelitano L, Brusati R, Castelnuovo P (2008) The silent sinus syndrome: diagnosis and surgical treatment. Rhinology 46: 308-316.
- Gillman GS, Schaitkin BM, May M (1999) Asymptomatic enophthalmos: the silent sinus syndrome. Am J Rhinol 13: 459-462.
- Bahgat M, Bahgat Y, Bahgat A (2012) Silent sinus syndrome. BMJ Case Rep 2012.
- Blackwell KE, Goldberg RA, Calcaterra TC (1993) Atelectasis of the maxillary sinus with enophthalmos and midface depression. Ann OtolRhinolLaryngol 102: 429-432.
- Hira NK, Lipham WJ, Marciniak MM (2004) Silent sinus syndrome. Optometry 75: 589-594.
- Wan MK, Francis IC, Carter PR, Griffits R, van Rooijen ML, et al. (2000) The spectrum of presentation of silent sinus syndrome. J Neuroophthalmol 20: 207-212.
Citation: Najaf F, AlTerki A, Al-Buluoshi A (2014) The Silent Sinus Syndrome: A Collaborative Approach between Rhinologists and Oculoplastics- Case Report and Literature Review. Otolaryngol (Sunnyvale) 4:179. DOI: 10.4172/2161-119X.1000179
Copyright: © 2014 Najaf Y, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 19889
- [From(publication date): 1-2015 - Aug 29, 2025]
- Breakdown by view type
- HTML page views: 15200
- PDF downloads: 4689