Research Article Open Access
Treatment Results of Anal Cancer: A Single-institution Long-term Experience
Anna Hemer, Annika Holmqvist, Gunnar Adell and Maria Albertsson*
Division of Oncology, Department of Clinical and Experimental Medicine, Faculty of Medicine and Health Sciences, County Council of Östergötland, Linköping University, 581 85 Linköping, Sweden
- Corresponding Author:
- Maria Albertsson
Division of Oncology, Department of Clinical
and Experimental Medicine, Faculty of Medicine
and Health Sciences, County Council of Östergötland
Linköping University, 581 85 Linköping, Sweden
Tel: +46 (0) 10 103 0000
E-mail: Maria.albertsson@regionostergotland.se
Received Date: Feb 9, 2016, Accepted Date: Mar 15, 2016, Published Date: Mar 22, 2016
Citation: Hemer A, Holmqvist A, Adell G, Albertsson M (2016) Treatment Results of Anal Cancer: A Single-institution Long-term Experience. J Gastrointest Dig Syst 6:402. doi:10.4172/2161-069X.1000402
Copyright: © 2016 Hemer A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Gastrointestinal & Digestive System
Abstract
Background: Anal and perianal cancer is a rare form of cancer. In this study we report results obtained using external beam radiotherapy with or without concurrent chemotherapy in the treatment of anal cancer. It is a singleinstitute long-term evaluation of 138 patients.
Methods: Retrospective analysis of 138 patients treated with radiotherapy (RT) with or without chemotherapy (CT) for an anal carcinoma (T1-4N0-N3M0).
Results: Overall Survival (OS) was 75% and Disease-free Survival (DFS) 68%. Interruptions in treatment were associated with a lower rate of survival.
Conclusion: This study confirms the outcomes of RT with or without CT in the treatment of anal cancer. High rates of side effects imposed tailored CT and RT as well as improved radiation techniques and better chemotherapy regimens.
Keywords
Anal cancer; Chemotherapy; Radiotherapy; Survival; Side effects
Introduction
Anal and perianal cancer is a rare form of cancer but its incidence is increasing worldwide. The incident rate is particularly high among the HIV positive population, and the incidence is higher for woman then men. Historically anal carcinoma was treated with surgery which necessitated a colostomy. Today, treatment is based on chemotherapy and radiotherapy. In this study we report long-term treatment results from a single institution. The majority of patients in this study have curable locoregional disease, highlighting the importance of optimizing locoregional therapy. The aim of the study was to investigate the outcome for those patients in the South East region, a rural part of Sweden, diagnosed with anal carcinoma. Furthermore, our aim was to study symptoms, treatment efficacy, side effects, quality of life and multidisciplinary collaboration in the cohort.
Method
Patients
The study included 138 patients diagnosed with anal carcinomfa in the Östergötland Region during a ten-year period from January 2003 until September 2014. Two of these 138 patients were misclassified and were in fact suffering from another form of cancer. Journals could not be found for 8 of the patients. A retrospective journal analysis was carried out for the 128 remaining patients. The following parameters were documented in a database; gender, age on diagnosis, TNM stage, symptoms, date of diagnosis, treatment regimen, follow-up data, multidisciplinary collaboration between the oncologist and surgeon, compliance of the treatment, acute and long-term side effects, relapse, distant metastasis, quality of life one year after treatment and intention of treatment (palliative or curative).
The American Joint Committee on Cancer’s guidelines (seventh edition) for TNM classification were used for tumour staging.
Patients were divided into three groups based on age: Patients younger than 50 years of age, patients between 50 and 70 years and patients older than 70 years.
Treatment guidelines
The treatment in Linkoping was based on Nordic guidelines for anal carcinoma, (NOAC). In 2012, clinicians made the decision to replace 5- fluorouracil with Capecitabine due to the toxicity of 5- fluorouracil. Before commencing treatment all patients were required to be assessed at a Multidisciplinary Team (MDT) meeting attended by oncologists, surgeons, pathologists and radiation therapists. The MDT meeting is an important tool in the treatment of CRC patients as it facilitates and coordinates their examination and treatment.
Previously, a pause of two weeks was recommended after 46 Gy of radiotherapy treatment in order to minimize acute toxicity. Recent studies indicate that a pause of 2 weeks after 46 Gy of radiotherapy treatment is associated with a lower rate of survival [1,2]. Therefore, this two-week gap in radiotherapy treatment is now avoided wherever possible.
The majority of patients (32) had cisplatin (carboplatin)/5-FU as an induction treatment. In the later part of the study 5 FU was exchanged to Capecitabine (16 patients). 2 patients underwent a different chemotherapy regime (Table 1).
| Year | N (cisplatin (carboplatine)/capecitabin | N (cisplatin (carbolatine)/5-fu | Other |
|---|---|---|---|
| 2014 | 5 | 0 | 0 |
| 2013 | 6 | 0 | 0 |
| 2012 | 4 | 5 | 0 |
| 2011 | 0 | 7 | 0 |
| 2010 | 0 | 5 | 0 |
| 2009 | 1 | 3 | 2 |
| 2008 | 0 | 3 | 0 |
| 2007 | 0 | 1 | 0 |
| 2006 | 0 | 3 | 0 |
| 2005 | 0 | 2 | 0 |
| 2004 | 0 | 2 | 0 |
| 2003 | 0 | 1 | 0 |
Table 1: Chemotherapy treatment over time.
End points
The primary end point was to study the five-year overall survival rate for the patients. However, it was also intended to study side effects of treatment, quality of life (one year after completion of treatment), symptoms, and frequency of MDT collaborations.
Toxicity during the treatment, as well as up to three months after treatment, was classified as an acute side effect. Subsequent toxicity was classified as a long-term side effect. Quality of life was analysed for disease-free patients one year after completing treatment.
The five-year survival rate for the cohort was compared using the following parameters; gender, age, TNM stage, relapse, distant metastasis, chosen treatment method and compliance of treatment. Only treatment for the primary cancer was documented. Treatment after relapse or distant metastasis was not included in the study.
In this study we have chosen to document the serious side effects of chemotherapy treatment. The following side effects of chemotherapy treatment was studied; emboli/thrombosis, neuropathy, nephrotoxicity, cardiac effects, leukocytopenia, low levels of haemoglobin, thrombocytopenia, serious infections and ototoxicity.
Local relapses included tumours that occurred in the anal region, tumours in the prostate, urethra, vagina, sacrum, pelvis, and tumours in regional lymph nodes in the groin and rectum.
Statistics
Overall survival was calculated using Kaplan-Meier curves and comparisons of the survival curves from group to group were carried out using the Gehan-Wilcoxon test.
The tests were performed with a significance level of 5%. All analyses were performed using IBM SPSS Statistics 22.
Tables and diagrams were made in IBM SPSS Statistics 22 and Microsoft Excel version 14.4.4.
This study was approved by the Institutional Review Board of Linköping University Hospital.
Results
Symptoms
Information about symptoms could be found in the journals of the 124 patients.
Most frequently reported were bleeding (56%), a feeling of discomfort in the anal region/a lump (22%) and pain during defecation (19%).
Multidisciplinary collaboration
In total, 101 of the patients in the cohort were discussed at an MDT meeting (radiation therapist, oncologist and surgeon) prior to treatment.
Gender, age, and TNM stage
Of the cohort, 62% were women and 38% men. Ten of the patients were younger than 50 years of age, 81 in the range between 50 and 70 years and 37 over 70 years.
The average and median age for the cohort was 66 years of age. The average and median age was the same for women and men (66 years).
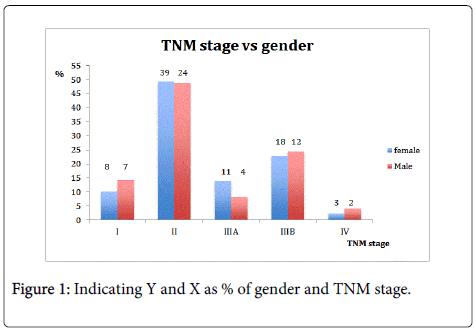
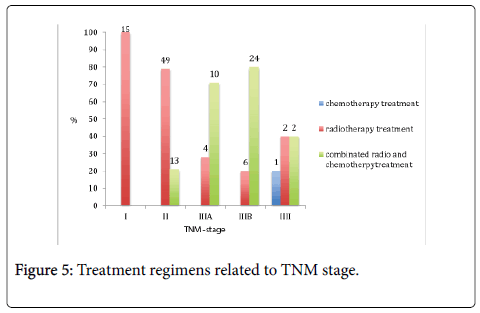
Eleven percent of the patients were classified as TNM stage 1, 49% as stage 2, 12% as stage 3A, 24% as stage 3B and 4% as stage 4 (Figure 1).
Survival analyses
Age, gender and TNM stage vs. five-year survival
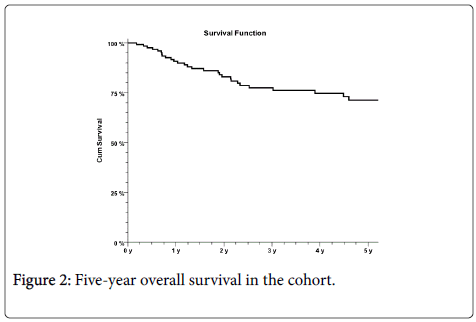
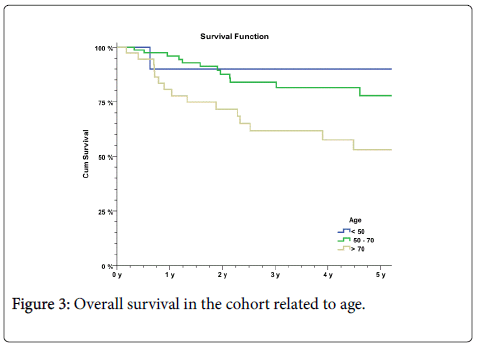
Overall survival (OS) for the cohort was 75% and disease-free survival (DFS) 68% (Figure 2). Five-year OS was significantly higher for the two younger patient groups than for the oldest group (p=0.015) (Figure 3).
At the end of the study, 91 of the patients (71%) were alive and 37 (29%) were deceased. Of the non-survivals, 31 patients (84%) died as a result of the anal cancer. All non-survival patients <50 years of age died of the disease, while for patients between 50 and 70 years of age this Figure was 92%. Among patients older than 70 years of age, 74% of deaths were caused by the disease.
Women fared better (OS=77%, DFS=75%) than men (OS= 63%, DFS=60%), however no significant differences between the genders were found.
Significant differences between the TNM stages were found (p=0.002). The OS of patients was 81% in stage 1, 81% in stage 2, 67% in stage 3A, 62% in stage 3B and 0 in stage 4, respectively.
Treatment and its compliance vs. survival
In their primary treatment plan, 122 of the patients were treated with curative intent and 6 of the patients with palliative intent. Five of those with palliative treatment intent were over the age of 70.
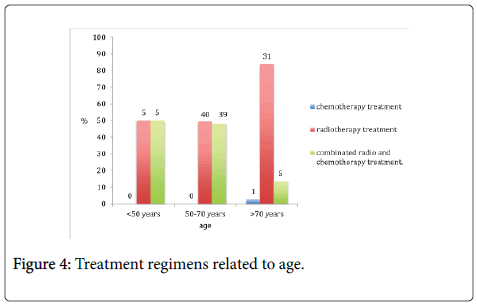
In total, 125 patients were given radiotherapy, either as monotherapy or in combination with chemotherapy (Figures 4 and 5). Of those, 110 were treated with curative intent. The remaining 15 patients were either treated with palliative intent, given pre or postoperative treatment, or the information was missing from their journals.
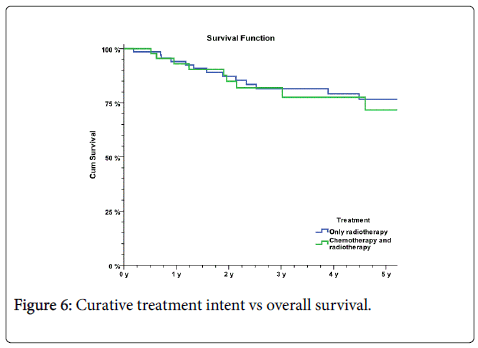
In total, 49 of the patients in the cohort have been treated with chemoradiotherapy in their primary treatment plan. One patient received Glivec (imatinib), one was treated exclusively with chemotherapy and one was treated with abdominoperineal resection. Seventy-six of the patients were treated with radiotherapy as monotherapy (OS=73%). OS for patients treated with chemoradiotherapy was 73%. For those patients with curative intent, OS was 77% for radiotherapy as monotherapy and 68% for chemoradiotherapy treatment (Figure 6).
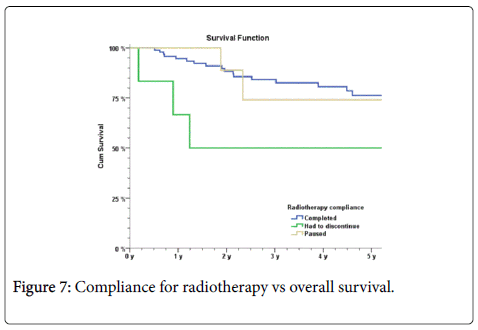
Fifty-nine of the patients treated with radiotherapy had an interruption in the radiotherapy. An interruption in the treatment was associated with lower OS (Figure 7) Fifty-seven patients had a treatment interruption of >7 days. A termination of radiotherapy gave a significantly lower OS (p=0.02).
Relapse and distant metastasis vs. survival
Of the observed patients, 25% suffered a relapse and 9% distant metastasis. Most common was a relapse in the anal region. For distant metastasis, the liver was the most common site. Twelve of the patients with distant metastasis suffered a relapse. Relapse and distant metastasis showed significantly lower OS (p (relapse)=0.002, p (distant metastasis)> 0.001).
Treatment, side effects of treatment and quality of life
Relapse vs survival
It has been shown that 11 (34%) of the 32 patients suffering a local relapse were treated with chemotherapy. For three of the patients, chemotherapy could not be completed due to the side effects of treatment, while in three cases an interruption in treatment was required due to side effects of the treatment. Only five patients suffering a relapse received chemotherapy according to their primary treatment plan.
All of the relapsing patients were treated with radiotherapy. Eighteen (56%) of these had an interruption in their radiotherapy, 11 were treated without interruption, and for three patients, the data was missing from their journals.
In total, 9 relapsing patients suffered no interruption or other compliance problems during their chemoradiotherapy.
Distant metastasis vs survival
Of the 12 relapsing patients with distant metastasis, 4 were treated with chemotherapy. Of these, two patients could not complete their chemotherapy due to the side effects of the treatment. One patient required a postponement of their chemotherapy due to toxicity. All of the patients with distant metastasis received radiotherapy.
Efficiency of treatment
A regression of the tumour was observed in 105 of the 125 patients treated with radiotherapy. Surgery in the form of an abdominoperineal resection, either due to tumour remaining after primary treatment or because of a local relapse, was required in 18% of the patients. In 72% of the cases, the tumour was radically excised.
Side effects
Altogether, 50 patients were treated with chemotherapy, either as monotherapy or in combination with radiotherapy. Of those, 52% suffered serious acute toxicity as described in the method. Age appeared to have no significance in relation to side effects. Most side effects were noted with Cisplatin in combination with 5- FU. Sixty-two percent of the patients taking this combination were affected by acute toxicity due to their treatment, while 36 % of the patients treated with Cisplatin/Capecitabine suffered acute toxicity.
Among 125 patients given radiotherapy, 99% exhibited some kind of side effect, either acute, long-term or both. Aside from this, 92 of the patients (74%) treated with radiotherapy were affected by long-term side effects. The most frequently reported long-term side effects were stoma, faecal incontinence and diarrhoea.
Side effects related to age
In total, 60% of patients <50 years of age suffered acute toxicity related to their chemotherapy. The corresponding data for patients between 50-70 years of age was 51%, and 52% for patients >70 years of age. In the youngest patient group, 60% completed their chemotherapy without interruption or other compliance problems. The corresponding data was 54% for patients between 50- 70 years of age, and 33% for the oldest patient group.
Discussion
Anal cancer is a rare tumour, the incidence of which has been rising over the past 25 years. In this article we present the results obtained from one region of Sweden over the course of ten years. The patients were consecutively collected, classified and discussed at Multidisciplinary Meetings (MDT). A multidisciplinary approach is mandatory, involving radiation therapists, medical oncologists, surgeons, radiologists and pathologists.
Survival is related to stage, age, gender and compliance of treatment. The primary aim of treatment is to achieve a cure with locoregional control while preserving anal function and providing the best possible Quality of Life.
Prior to the development of chemoradiotherapy i.e., the mid -1980s, the treatment of choice for anal cancer was Abdominoperineal resection (APR), a procedure involving the removal of the anus and rectum as well as their draining lymph nodes and resulting in a permanent colostomy [3]. The five-year survival after APR for anal carcinoma is in the range of 40-70%, with a worse outcome for those with larger tumours and nodal metastases. APR is now reserved as salvage therapy for those individuals with persistent disease after combined chemo and radiation.
Work on the use of chemotherapy in combination with radiotherapy was first published in the mid-1990s, from both UKCCCR [4] and EORTC [5]. Both trials found a higher CR with the addition of chemotherapy. With an almost 20% advantage for the combined group. They concluded that combined chemo radiation therapy for anal carcinoma improved locoregional control and reduced the need for a colostomy without increasing late complications.
Follow Up
Because most anal carcinomas regress slowly, they regress even after completion of chemoradiotherapy. It is estimated that by 12 weeks after the completion of treatment, the majority of patients should manifest the maximum treatment response. There is currently no consensus as to whether this response should be assessed by physical examination alone or in combination with a biopsy. It is also not clear whether a biopsy should play a role in the management of those individuals with a complete clinical response.
There is little data available about predictors of local failure, but one retrospective study was identified where the outcome was evaluated in 254 patients treated for anal cancer with either radiotherapy alone or combined chemo and radiation [6]. Local failure occurred in 39% with a median time to failure of 20 months. Five-year local control of the disease varied significantly between those patients receiving radiation alone and those patients receiving combined chemo and radiation. For patients receiving radiation alone, age, total radiation dose <50 Gy and higher T stage predicted local failure. Conversely, for patients receiving combined chemo and radiation there was no predictive factor.
In our material the prognoses were worse for older patients. Their tolerance for treatment was lower, combination therapy was less common in this group and it is also obvious that when treatment was interrupted it had a negative impact on survival.
The majority of our patients were treated with cisplatin and 5-Fu intravenously. During the study, the standard treatment was changed to Capecitabine and cisplatin. This is described as equally effective and it is reported that Capecitabine can be used as an acceptable alternative to 5-Fu treatment for anal carcinoma [7]. Our study supports these results.
Chemoradiotherapy for anal carcinoma can have both acute and chronic side effects. Acute side effects include diarrhoea, mucositis, skin erythema and desquamation and myelosuppression. Late complications, some of which necessitate surgery with or without colostomy, include anal ulcers, stricture/stenosis, fistulae and necrosis. Reported late event rates following chemoradiotherapy for anal cancer are in the range of 3%-16%. The risk for these complications increases as a function of both total radiation dose and fraction size.
In our material we observed anal problems in 86 patients, however the majority of minor degree. Since our material was collected retrospectively, the results must be interpreted with great caution, however, a colostomy was necessary in 31 of the 86 patients with late side effects.
The majority of patients treated with chemotherapy and RT after the diagnoses of anal cancer have excellent outcomes [8]. However, special problems in psychological adjustment are posed as a result of both immediate side effects as well as late toxicities that may also adversely affect Quality of Life.
Although more research needs to be done, the results of recent studies suggest that more emphasis needs to be placed on identifying and addressing treatment-related symptoms during and after chemo radiation for anal cancer. Long-term follow up of these patients is necessary to identify and treat the consequences of successful cancer therapy.
We intend to select a number of patients for long-term monitoring and interview regarding quality of life. There have been some reports in the literature concerning this matter [9-11].
Metastatic Disease
Metastatic disease develops in 10-17% of patients treated with chemo radiation therapy. The most common site of distant metastasis is the liver. Metastatic anal cancer is normally treated with systemic chemotherapy, typically utilizing a combination of 5-FU and cisplatin. Carboplatin and paclitaxel show encouraging activity for this disease with a response rate of 53% and a median survival of 12 months [12]. Overall, about 60% one-year survival and 32% five-year survival rates with systemic chemotherapy have been reported [13].
In general, there is not much of a role for surgery in the treatment of metastatic disease except to provide palliation for pain, bleeding or faecal incontinence.
There is an increasing interest in newer, targeted therapies for anal cancer. It was recently demonstrated that there is a high rate of expression of epidermal growth factor (EGFR) within most anal cancer cell lines [14]. Cetuximab is an EGFR blocker that is used in conjunction with radiotherapy to treat squamous cell carcinoma of the head and neck. There have been two small early phase trials in order to evaluate the use of cetuximab in anal cancer [15,16]. Both trials demonstrated significant toxicities with cetuximab that precluded incorporation of this agent into routine chemotherapy protocols for anal cancer. One of the trials demonstrated a 95% initial complete response rate, with a three-year local regional control rate of 64%. Therapy targeted against the EGFR may ultimately prove beneficial in the future with less toxic agents; however, the lack of widespread data at this stage precludes definitive recommendations regarding its role.
It is of outmost importance to use clinical trials in order to develop new therapy alternatives, such as EGFR inhibitors with radiation therapy and chemotherapy. A greater understanding of the biology of human papillomavirus in anal cancer, as well as how to translate this knowledge to screening, prevention and treatment resistance, is also needed in order to improve the survival rate and Quality of Life for these patients.
Squamous cell carcinoma of the anus is strongly associated with human papillomavirus (HPV) infection, representing the causative agent in 80-85% of patients. This will be further investigated in this material.
Conclusion
Overall survival for the entire group was 75% and disease-free survival 68%. This is comparable to other results reported in the literature.
High rates of side effects imposed tailored CT and RT and improved radiation techniques and better chemotherapy regimens.
References
- Konski A, Garcia M Jr, John M, Krieg R, Pinover W, et al. (2008) Evaluation of planned treatment breaks during radiation therapy for anal cancer: update of RTOG 92-08.Int J Radiat Oncol Biol Phys 72: 114-118.
- Bilimoria KY, Bentrem DJ, Rock CE, Stewart AK, Ko CY, et al. (2009) Outcomes and prognostic factors for squamous-cell carcinoma of the anal canal: analysis of patients from the National Cancer Data Base.Dis Colon Rectum 52: 624-631.
- Ryan DP, Compton CC, Mayer RJ (2000) Carcinoma of the anal canal.N Engl J Med 342: 792-800.
- (1996) Research. UACTWPUC-oCoC. Epidermoid anal cancer: results from the UKCCCR randomised trial of radiotherapy alone versus radiotherapy, 5-fluorouracil, and mitomycin. Lancet 348:1049-1054.
- Bartelink H, Roelofsen F, Eschwege F (1997) Concomitant radiotherapy and chemotherapy is superior to radiotherapy alone in the treatment of locally advanced anal cancer: results of a phase III randomized trial of the European Organization for Research and Treatment of Cancer Radiotherapy and Gastrointestinal Cooperative Groups. Journal of clinical oncology 15: 2040-2049.
- Renehan AG, Saunders MP, Schofield PF, O'Dwyer ST (2005) Patterns of local disease failure and outcome after salvage surgery in patients with anal cancer.Br J Surg 92: 605-614.
- Meulendijks D, Dewit L, Tomasoa NB, van Tinteren H, Beijnen JH, et al. (2014) Chemoradiotherapy with capecitabine for locally advanced anal carcinoma: an alternative treatment option.Br J Cancer 111: 1726-1733.
- Ajani JA, Winter KA, Gunderson LL, Pedersen J, Benson AB, et al. (2008) Fluorouracil, mitomycin, and radiotherapy vs fluorouracil, cisplatin, and radiotherapy for carcinoma of the anal canal: a randomized controlled trial.JAMA 299: 1914-1921.
- Welzel G, Hägele V, Wenz F, Mai SK (2011) Quality of life outcomes in patients with anal cancer after combined radiochemotherapy.Strahlenther Onkol 187: 175-182.
- Bentzen AG, Balteskard L, Wanderås EH, Frykholm G, Wilsgaard T, et al. (2013) Impaired health-related quality of life after chemoradiotherapy for anal cancer: late effects in a national cohort of 128 survivors.Acta Oncol 52: 736-744.
- Godlewski G, Prudhomme M (2000) Embyrology and anatomy of the anorectum. Surg clinc 80: 319-343.
- Kim R, Byer J, Fulp WJ, Mahipal A, Dinwoodie W, et al. (2014) Carboplatin and paclitaxel treatment is effective in advanced anal cancer.Oncology 87: 125-132.
- Faivre C, Rougier P, Ducreux M, Mitry E, Lusinchi A, et al. (1999) 5-fluorouracile and cisplatinum combination chemotherapy for metastatic squamous-cell anal cancer.Bull Cancer 86: 861-865.
- Paliga A, Onerheim R, Gologan A, Chong G, Spatz A, et al. (2012) EGFR and K-ras gene mutation status in squamous cell anal carcinoma: a role for concurrent radiation and EGFR inhibitors?Br J Cancer 107: 1864-1868.
- Olivatto LO, Vieira FM, Pereira BV, Victorino AP, Bezerra M, et al. (2013) Phase 1 study of cetuximab in combination with 5-fluorouracil, cisplatin, and radiotherapy in patients with locally advanced anal canal carcinoma.Cancer 119: 2973-2980.
- Deutsch ELC, Pignon JP (2013) Unexpected toxicity of cetuximab combined with conventional chemoradiotherapy in patients with locally advanced anal cancer: results of the UNICANCER ACORD 16 phase II trial. Ann Oncol 24:2834-2838.
Relevant Topics
- Constipation
- Digestive Enzymes
- Endoscopy
- Epigastric Pain
- Gall Bladder
- Gastric Cancer
- Gastrointestinal Bleeding
- Gastrointestinal Hormones
- Gastrointestinal Infections
- Gastrointestinal Inflammation
- Gastrointestinal Pathology
- Gastrointestinal Pharmacology
- Gastrointestinal Radiology
- Gastrointestinal Surgery
- Gastrointestinal Tuberculosis
- GIST Sarcoma
- Intestinal Blockage
- Pancreas
- Salivary Glands
- Stomach Bloating
- Stomach Cramps
- Stomach Disorders
- Stomach Ulcer
Recommended Journals
Article Tools
Article Usage
- Total views: 11656
- [From(publication date):
April-2016 - Jul 04, 2025] - Breakdown by view type
- HTML page views : 10756
- PDF downloads : 900