Research Article Open Access
Variables Associated with Drug and Alcohol Abuse among Male and Female users with Severe Mental Disorders
Marie-Josée Fleury1,2*, Guy Grenier2 and Jean-Marie Bamvita21McGill University; Montreal Addiction Rehabilitation Centre - University Institute, Canada
2Douglas Hospital Research Centre, Montreal, Quebec, Canada
- Corresponding Author:
- Marie-Josée Fleury
Montreal Addiction Rehabilitation Centre-University Institute
Montreal, Quebec, Canada
E-mail: flemar@douglas.mcgill.ca
Received date: January 20, 2014; Accepted date: April 28, 2014; Published date: April 30, 2014
Citation: Fleury MJ, Grenier G, Bamvita JM (2014) Variables Associated with Drug and Alcohol Abuse among Male and Female users with Severe Mental Disorders. J Addict Res Ther S10:005. doi:10.4172/2155-6105.S10-005
Copyright: © 2014 Fleury MJ, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Addiction Research & Therapy
Abstract
Objectives: According to current literature, the most reliable variables associated with substance abuse are sociodemographic variables, mainly gender. Based on longitudinal research and a comprehensive framework, this study aimed to determine variables associated with substance abuse among users with severe mental disorders and between males and females of this general sample.
Methods: A cohort of 297 users with severe mental disorders was interviewed after an 18-month follow-up period. A hierarchical linear regression analysis was carried out using five blocks of independent variables at baseline (sociodemographic, clinical, needs and functionality, negative life events, social support). Two additional models were built to separately assess variables associated with substance abuse in males and females, using multiple linear regression analysis.
Results: Drug and alcohol abuse among users with severe mental disorders was associated with being non-French speaking, younger, male, a resident in autonomous housing, or an individual with less functionality and high severity of needs. Seven variables were associated with substance abuse among females while nine variables were independently associated with substance abuse among males.
Conclusion: The results confirm that socio-demographic variables are the most important variables associated with substance abuse among users with severe mental disorders. Language (being non-French-speaking) was the most important variable associated with substance abuse among users with severe mental disorders, and the only variable common to both males and females. These results suggest that mental health services need to pay special attention to certain linguistic minorities that are more likely to experience substance abuse issues.
Keywords
Co-occurring disorders; Drug abuse; Alcohol abuse; Severe mental disorders; Gender; Diagnosis; Socio-demographic variables
Variables Associated with Drugs and Alcohol Abuse in users, Males and Females, with Severe Mental Disorders
The high prevalence of drug or alcohol abuse among individuals with severe mental disorders has often been revealed in the literature [1-4]. Individuals with co-occurring severe mental disorders and substance abuse usually face stigma, problems with the law [5], poor education, unemployment, loneliness, poverty and homelessness as compared to those with severe mental disorders only [6]. They also have more serious psychiatric symptoms, poorer treatment outcomes [1], and use health services more often [7,8]. These negative impacts justify the necessity to better identify variables associated with substance abuse among individuals with severe mental disorders and (to better precise) their relative importance.
Cross-sectional studies have identified variables associated with substance abuse [7,9-17], the most reliable being socio-demographic variables such as age, gender [12,14,15], education [12,14], marital status, living situation [11,12], and employment history [13]. Users with substance abuse are more likely to be male, young, and single, with low education and low incomes [15,17]. Previous studies have found notable differences between males and females concerning prevalence of substance abuse [18,19], patterns of substance use [20,21], outcomes [9,11,13], presence of co-occurring disorders [5,22-25] and access to substance treatment [14,20,21].
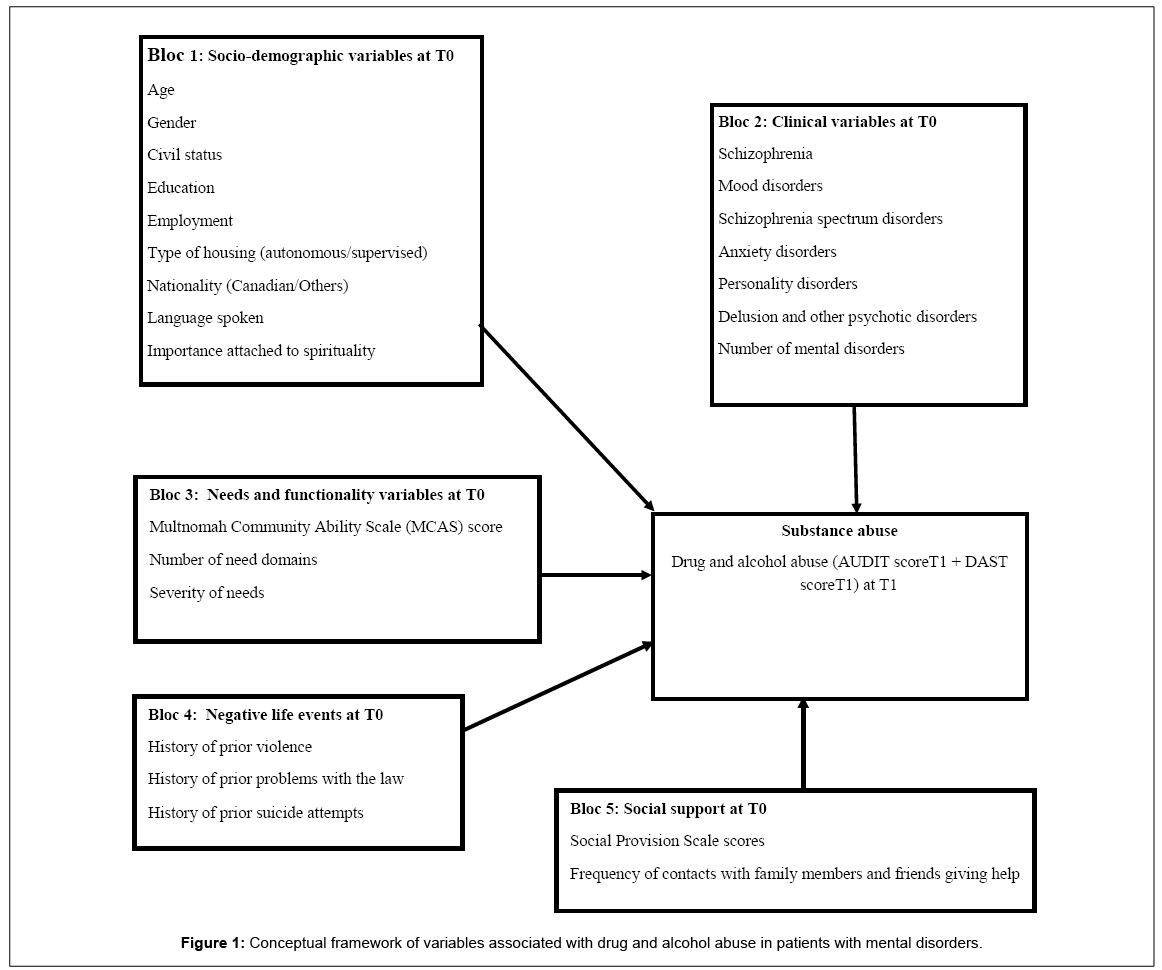
Although variables associated with substance abuse among males and females have been described extensively in cross-sectionals studies, most analyzed variables associated with a specific substance (alcohol, cannabis, etc.) or with one specific mental disorder (schizophrenia, mood disorders) [12,26-28]. To the best of our knowledge, no previous study has analyzed variables associated with substance abuse and severe mental disorders in general, and very few studies specifically related to severe mental disorders exist. The knowledge of variables associated with substance abuse among a sample of users with severe mental disorders could be useful with a view to targeting appropriate interventions for this clientele. Furthermore, longitudinal analysis offers a stronger method than cross-sectional analysis for examining variables associated with substance abuse. No known study has compared variables associated with substance abuse based on gender in using a longitudinal framework. Based on a longitudinal research and a comprehensive framework (Figure 1), this study intends to determine variables associated with substance abuse: 1) among users with severe mental disorders; and 2) between males and females of this general sample.
Methods
Study design and network characteristics
This cohort study involved two measures. Users with severe mental disorder were first recruited and interviewed between December 2008 and September 2010 (T0), and were interviewed again approximately 18 months later, between January 2011 and November 2011 (T1). Recruitment took place at a Mental Health University Institute (MHUI) and at two Health and Social Service Centers (HSSCs) located in the south-west sector of Montreal, Canada. This urban area covers two local health networks serving a population of 258,000. The MHUI offers specialized mental health services (i.e. second- and third-line services). The two HSSCs, created through the merger of general hospitals, community local health centers, and nursing homes, provide primary and specialised mental health-care services. Other professionals and organizations offering health services in the south-west sector of Montreal have been described in greater detail in a previous publication [29].
Selection criteria and recruitment of the sample
The study protocol was approved by the ethics boards of the mental health institute and the two HSSCs. Study participants were 18 to 65 years of age, diagnosed with a severe mental disorder according to DSM-IV criteria (e.g. schizophrenia, bipolar disorder, major depression), lived in one of the two local health networks covered by the study, and were followed at the MHUI or one of the two HSSCs. Users gave consent for the research team to access their medical record, and referred this team to their case manager, for the purpose of filling a questionnaire on patient community functioning. Users undergoing involuntary psychiatric treatment, as determined by a judicial board, and persons with a history of hospitalization or emergency room visits in the three months prior to the initial interview were considered unable (i.e. too fragile or unstable clinically) to complete the questionnaire, and were thus excluded from the study. The sampling strategy and data collection have been described in detail in related publications [29,30].
Measuring instruments
Data was collected at baseline and at 18-month follow-up using five questionnaires administered in English or French, according to patient choice, and patient medical records were accessed at the MHUI.
The main instruments were the Alcohol Use Disorders Identification Test (AUDIT) [31] and the Drug Abuse Screening Test-20 (DAST-20) [32]. The AUDIT (Cronbach’s alpha (CA) = 0.88; [33]) measures alcohol consumption level and consequences with 10 items offering two or multiple answers, for a maximum possible score of 40 [34]. A score of 8 to 11 indicates hazardous or harmful alcohol use [34] and a score of 12 or above indicates alcohol dependence [33]. The DAST-20 (CA = 0.74; [35]) evaluates patient drug use and consequences, including neuro-adaptive symptoms with 20 yes/no questions, for a maximum possible score of 20. A score of 6 or more indicates drug abuse [35].
Other standardized instruments used at both measuring points were the Social Provisions Scale (SPS) [36] which explores level of patient integration and social support in ten items (e.g. emotional support, social integration), based on a four-point-Likert scale; the Multnomah Community Ability Scale (MCAS) that assesses user community interaction in 17 items (e.g. obstacles to interaction, social competencies), based on a five-point Likert scale [37]; and the Montreal Assessment of Needs Questionnaire (MANQ), developed by the present research team [30], and derived from the Camberwell Assessment of Need (CAN; [38]) which measures 26 need domains with analog scales ranging from 0 to 10. All questionnaires were completed by participants, with the exception of the MCAS, which was completed by each participant’s principal case manager. Moreover, participants’ medical records were used to compile complementary clinical data and included DSM-IV diagnoses, history of prior suicide attempts, history of violence, and history of legal problems.
Analysis
Analyses were conducted according to the conceptual framework displayed in Figure 1. The dependent variable was Alcohol and drug abuse at follow-up period (T1). This variable was obtained by summing up DAST and AUDIT scores, yielding a continuous variable labelled “Alcohol and drug abuse”. Independent variables were organized into socio-demographic variables, clinical variables, needs and functionality variables, negative life event variables and social support. These variables are reported as the most often associated with substance abuse among individuals with severe mental health disorders according to the literature [12,20,28].
Univariate analyses consisted of frequency distribution for categorical variables and mean values for continuous variables to describe participants in the sample at T1. Using the dependent variable, comparison analyses were carried out between participants with and without substance abuse disorders, based on DAST and AUDIT scores. A hierarchical linear regression analysis was carried out using the five blocks of independent variables according to the order presented in Figure 1, which is adapted from Caron’s SQOL framework [39] and has been used in a previous paper with the same sample [30]. The blocks that were most reliable and less subject to interpretation were entered first (e.g. socio-demographic variables, followed by clinical variables). Each block was first entered using a backward elimination technique, for an alpha value of 0.5. Variables retained from each block were forced in the next step along with the following block of variables. For each partial model produced from different blocks, goodness-offit and variance explained were calculated so that the contribution of each block could be estimated. Two additional models were built to separately assess variables associated with substance abuse in males and females, using a multiple linear regression analysis. For both models, total variance was explained and goodness-of-fit also estimated.
Results
Of 437 users recruited at baseline (T0), a total of 351 (80%) agreed to participate, and 86 subjects (20%) declined. Refusals were compared to participants based on age, sex and housing type [40]. Of the 351 participants, 297 (84.6%) were interviewed after an 18-month follow-up period (T1). Subjects who dropped out of the study were also compared with participants along the same variables (age, sex and housing type), adding diagnosis [30]. No statistically significant differences were found for both groups at T0 and T1.
At T1, there were 153 (51.5%) males and 144 (48.5%) females, with a mean age of 48 (SD: 10.4), as shown in Table 1. A majority of patients were French-speaking (64.0%), and single (75.4%). Two thirds (62.3%) had completed only primary or secondary school. The most prevalent severe mental disorder was mood disorder (41.8%) and schizophrenia (38.0%). A total of 121 participants (40.7%) had drug or alcohol abuse at TI. DAST score ranged from 0 to 15, with a mean of 1.4 (SD: 1.2). AUDIT score ranged from 0 to 32, with a mean of 5.3 (SD: 5.7). The continuous dependent variable “Alcohol and drug abuse”, ranged from 0 to 39, with a mean at 6.7 (SD: 6.5).
| Categories | Sub-categories | Variables | n | % |
|---|---|---|---|---|
| Socio-demographic variables | Age [Mean (SD)] | 48.5 | 10.4 | |
| Gender | Men | 153 | 51.5 | |
| Women | 144 | 48.5 | ||
| Language spoken | French | 190 | 64.0 | |
| English | 61 | 20.5 | ||
| French/English | 7 | 2.4 | ||
| Others | 37 | 12.5 | ||
| Civil status | Single/Never married | 224 | 75.4 | |
| In couple/Married/Remarried | 33 | 11.1 | ||
| Separated /Divorced/Widow | 40 | 13.5 | ||
| Education | Primary/Secondary school | 185 | 62.3 | |
| College/University | 110 | 37.0 | ||
| Clinical variables |
Severe mental disorders | Mood disorders | 124 | 41.8 |
| Schizophrenia | 113 | 38.0 | ||
| Schizophrenia spectrum disorders | 38 | 12.8 | ||
| Delusion and other psychotic disorders | 28 | 9.4 | ||
| Second diagnosis | Personality disorders | 81 | 27.3 | |
| Moderate or mild mental retardation | 37 | 12.5 | ||
| Anxiety disorders | 36 | 12.1 |
Table 1: Socio-demographic, socio-economic and clinical variables (N = 297).
The five blocks of independent variables were entered in the model consecutively (Table 2). From the first block of socio-demographic variables, four variables were retained in the model using the backward elimination technique: language (French-speaking), age (younger), gender (male) and type of housing (autonomous). No variable was retained from the clinical block. From the needs and functionality block, two additional variables were retained: severity of needs and MCAS score. No other variable was retained in subsequent blocks, yielding a six-variable model with three negatively associated variables (language, age, community interaction), and three positively associated variables (gender, type of housing, severity of needs). This model explained 28% of the variance. The strongest contribution came from the first block of socio-demographic variables (26%). The goodness-of-fit of the model was acceptable.
| Socio-demographic variables at T0 | Clinical variables at T0 | Needs and functionality variables at T0 | Negative life events at T0 | Social support at T0 | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Variables at baseline (T0) |
β | P | β | P | β | P | β | P | β | t | P | 95.0% CI | Colinearity statistics | ||
| LL | UL | Tolerance | VIF | ||||||||||||
| Language | -.482 | .000 | -.482 | .000 | -.468 | .000 | -.468 | .000 | -.468 | -8.784 | .000 | -7.761 | -4.920 | .869 | 1.151 |
| Age | -.169 | .001 | -.169 | .001 | -.149 | .003 | -.149 | .003 | -.149 | -2.946 | .003 | -.153 | -.030 | .963 | 1.038 |
| Gender | .160 | .002 | .160 | .002 | .150 | .003 | .150 | .003 | .150 | 2.968 | .003 | .657 | 3.246 | .968 | 1.034 |
| Autonomous housing | .166 | .002 | .166 | .002 | .150 | .007 | .150 | .007 | .150 | 2.696 | .007 | .542 | 3.472 | .795 | 1.259 |
| Severity of needs | .109 | .039 | .109 | .039 | .109 | 2.076 | .039 | .009 | .321 | .899 | 1.112 | ||||
| Community functionality (MCAS score) | -.101 | .049 | -.101 | .049 | -.101 | -1.973 | .049 | -.136 | .000 | .951 | 1.052 | ||||
| Total variance explained (R2) | 26.2% | 26.2% | 28.4% | 28.4% | 28.4% | ||||||||||
| Goodness-of-fit | |||||||||||||||
| F | 25.888 | 25.888 | 19.170 | 19.170 | 19.170 | ||||||||||
| P | <0.001 | <0.001 | <0.001 | <0.001 | <0.001 | ||||||||||
Table 2: Variables associated with drug-alcohol abuse among users with mental disorders: hierarchical linear regression analysis.
Variables associated with substance abuse in males and females are displayed in Tables 3 and 4 respectively. Seven variables are independently associated with substance abuse in females, including one marginally. Three of them are positively associated: nationality, severity of needs and, marginally, delusion and other psychotic disorders. Four variables are negatively associated: language, importance attributed to spirituality, schizophrenia, and mood disorders. This model explains 33% of the total variance with an acceptable goodness-of-fit. Nine variables are independently associated with substance abuse in males. Four of them are positively associated: autonomous housing, mood disorders, prior history of violence and, marginally, schizophrenia. Five others are negatively associated: age, language, number of mental health diagnoses, prior history of legal problems, and social support. This model explains 38% of the total variance, with an acceptable goodness-of-fit.
| Determinants at baseline (T0) | Standardized Beta | t | P value | 95.0% CI | Colinearity statistics | ||
|---|---|---|---|---|---|---|---|
| LL | UL | Tolerance | VIF | ||||
| Canadian nationalitya | .181 | 2.232 | .027 | .421 | 7.019 | .831 | 1.203 |
| Languagea | -.478 | -5.728 | .000 | -8.036 | -3.909 | .783 | 1.276 |
| Importance attributed to spiritualitya | -.206 | -2.780 | .006 | -.630 | -.106 | .989 | 1.012 |
| Schizophreniab | -.197 | -2.091 | .039 | -5.252 | -.144 | .612 | 1.633 |
| Mood disordersb | -.237 | -2.639 | .009 | -4.946 | -.706 | .675 | 1.482 |
| Delusion & other psychotic disordersb | .144 | 1.912 | .058 | -.108 | 6.271 | .962 | 1.040 |
| Severity of needsc | .198 | 2.532 | .013 | .063 | .512 | .891 | 1.122 |
Total variance explained (R2): 33.0%; Goodness-of-fit: F = 8.654; P <0.001
a= Socio-demographic variables; b= Clinical variables; c= Negative life events; d=Social support.
Table 3: Variables associated with drug-alcohol abuse among female users with mental disorders: Multiple linear regression analysis.
| Standardized Beta | t | P value | 95.0% CI | Colinearity statistics | |||
|---|---|---|---|---|---|---|---|
| LL | UL | Tolerance | VIF | ||||
| Agea | -.286 | -4.031 | .000 | -.272 | -.093 | .878 | 1.139 |
| Type of housing (autonomous)a | .216 | 2.977 | .003 | .989 | 4.900 | .843 | 1.186 |
| Languagea | -.436 | -5.948 | .000 | -8.200 | -4.109 | .822 | 1.216 |
| Schizophreniab | .164 | 1.702 | .091 | -.361 | 4.833 | .475 | 2.106 |
| Mood disordersb | .222 | 2.255 | .026 | .404 | 6.151 | .455 | 2.197 |
| Number of mental health diagnoses (except dependence)b | -.221 | -2.698 | .008 | -3.620 | -.558 | .661 | 1.512 |
| Prior history of violencec | .188 | 2.424 | .017 | .473 | 4.661 | .735 | 1.360 |
| Prior history of problems with the lawc | -.176 | -2.274 | .025 | -4.775 | -.333 | .737 | 1.357 |
| Social support (SPS score)d | -.141 | -2.054 | .042 | -.264 | -.005 | .939 | 1.065 |
Total variance explained (R2): 38.0%; Goodness-of-fit: F = 9.549; P <0.001
a=Socio-demographic variables; b=Clinical variables; c=Negative life events; d=Social support.
Table 4: Variables associated with Drug-Alcohol abuse in male users with mental disorders: Multiple linear regression analysis.
Discussion
The results confirm that socio-demographic variables are the most important variables associated with substance abuse for users with severe mental disorders in clinical as well as epidemiological studies [12]. Among six variables included in the final model, four were sociodemographic. The association of substance abuse with males and the young were expected [12,14,20,21]. The greatest prevalence of substance abuse among males has been found in all cultures [41] and frequency of abuse decreases with age [41]. However, the most important variable associated with substance abuse was non-French-speaking. Patients speaking French were less likely to engage in substance abuse than non-French speaking patients. Previous studies have found disparities in the prevalence of mental disorders and substance abuse disorders prevalence between linguistic majoritarian and minority groups [42-44]. According to the data of the Canadian Community Health Survey 1.2, Canadian English-speaking had higher prevalence of alcohol dependence that French-speaking within or outside Quebec [42,43]. Those differences could be explained by cultural, social or historical factors. Substance abuse is more common among certain groups such as people from North and East Europe [45]. Nearly half of Quebec English-speaking are immigrants [42]. Moreover, historically, the MHUI served mainly English-speaking clients, and the south-west sector of Montreal includes a large proportion of people of Irish origin [46], which had a reputation to be heavy drinkers [47]. The association between substance abuse and autonomous housing is probably as a result of supervised housing admission criteria. This type of housing usually refuses to admit users with disturbing behaviors such as substance abuse [48]. Conversely, users living in autonomous housing have a high probability of having drug dealers or consumers in their neighborhoods because their poor socio-economic condition [10]. Finally, the associations between lower community interaction, higher severity of needs and substance abuse among users with severe mental disorders were logical. Users with co-occurring mental disorders and substance abuse usually have severe needs, more particularly in psychological distress and safety to self [49,50], which could explain their difficulty in integrating in the community.
The additional models built to compare sex categories show that variables associated with substance abuse in males and females respectively were very different. Non-French-speaking was the only variable present both among males and females probably for the reasons explained previously.
For females, Canadian nationality and absence of importance to spirituality were associated with substance abuse. An explanation could be the greater differentiation of male and female roles among immigrants. In some cultures and religions, consumption of alcohol or drugs by females is highly disapproved of, which would dissuade them from substance abuse [51]. Moreover, substance abuse is often associated with loss or absence of faith, which points to the importance of incorporating spirituality in addiction treatment [6]. The association between substance abuse and absence of mood disorders among females was particularly unexpected considering that they are more likely to have major depression or bipolar disorders than males [21]. According to the literature [52,53], mood disorders would predispose females to substance abuse. The amalgam of alcohol and drug abuse could explain the absence of association, some substances being associated with major depression and bipolar disorders and other not. Concerning the association with absence of schizophrenia among females, several studies have found that users with co-occurring schizophrenia and substance abuse were mainly males [2,54,55]. Concerning the association with severity of needs, it is acknowledged that females express more easily their needs than males and are less reluctant to seek help [56]. Females with co-occurring severe mental disorders and substance abuse are also more affected than males by psychological distress [53]. Moreover, childcare is a need almost exclusive to females [57] and is usually unmet [57,58]. In a previous study on the structure of needs among users with schizophrenia, Korkeila et al. [59] found that childcare was associated with drug problems, alcohol problems and daytime activities in within a same needs factor.
For males, age was associated with substance abuse. Males generally begin to use alcohol and drugs sooner than females [21,23,26,60]. Age could also explain the association between mood disorders and substance abuse among males. According to the literature, substance abuse is usually associated with onset of bipolar disorders at an earlier age [61,62]. Moreover, the maniac component is predominant among males with bipolar disorders [62] and over indulging in everything, including substance use, is one of the criteria of mania [24]. The association between substance abuse and a lower number of mental disorders among males can be explained by the fact they are less likely to have anxiety disorders and major depression than females [61]. Furthermore, according to the literature, males with severe mental disorders living in autonomous housing are usually single, and can be motivated to use alcohol or drugs to reduce their loneliness [63]. Concerning the association with prior history of violence, it is known that the potential for violent or aggressive behavior of males with severe mental disorders increases when they are intoxicated [64,65]. Substance abuse would be the main variable associated with violence [66]. The association with absence of prior history of legal problems could be explained by our selection criteria, since persons following involuntary psychiatric treatment as determined by a judiciary board, are excluded. Finally, the association with absence of social support among males can be explained by the fact they usually receive less help from their relatives and friends than females [67]. Family and social supports influence admission and pursuit of treatment [68] and predict better outcomes for users with co-occurring mental and substance abuse disorders [69]. Another explanation could be that males are more likely than females to use alcohol and drugs in view to eliminate their inhibitions and then establish relationship with others individuals [63].
This study presents some limitations. First, since our sample consisted of a heterogeneous group of users with severe mental disorders living in the community, our results may not be applicable to populations in other settings or to other clienteles, such as persons with a specific mental disorder (e.g. schizophrenia). Second, due to the low proportion of users having alcohol or drug abuse only, it was impossible to analyse the two substance abuse disorders separately. Finally, the amalgam in our dependent variable of drugs and alcohol abuse could explain some unexpected results, mainly those concerning diagnosis. Alcohol or some specific drugs are mainly associated with specific mental disorders. Future studies could target specific severe mental disorders (such as schizophrenia or severe depression) and/or substance abuse.
Conclusion
This study was innovative in using a comprehensive framework including socio-demographic, clinical, needs and functionality, negative life events, and social support variables among individuals with severe mental disorders and substance abuse. The identification of variables associated with substance abuse among a sample of users with severe mental disorders in general could be useful in view to target appropriate interventions for this clientele. The study found that non-French-speaking (Quebec minority group) is the most important variable associated with substance abuse by this clientele. As a result, mental health services need to focus particularly on linguistic minorities where the propensity for individuals to experience substance abuse issues may be greater. Strategies such as harm reduction and motivational interviewing adapted to cultural minorities, as well as the utilization of cultural interpreters, may help mitigate against linguistic and cultural factors that pose barriers to treatment. As well, the results revealed that substance abuse among users with severe mental disorders is associated with greater severity of needs and lower community functionality. Programs such as integrated dual diagnosis treatment, day hospital, supervised housing and assertive community treatment should be prioritized for this specific clientele. Furthermore, substance abuse among males and females with severe mental disorders is associated with very distinct variables. For males, it is important for mental health services to focus their attention on young individuals living in autonomous housing, with little social support and a history of violence. For females, the intervention must be focused on decreasing the severity of needs and recovery.
Acknowledgements
The study was funded by the Canadian Institute of Health Research (CIHR). We would like to thank this grant agency and all the individuals who participated in the research.
References
- Castel S, Rush B, Urbanoski K, Toneatto T (2006) Overlap of clusters of psychiatric symptoms among clients of a comprehensive addiction treatment service. Psychol Addict Behav 20: 28-35.
- Hättenschwiler J, Rüesch P, Modestin J (2001) Comparison of four groups of substance-abusing in-patients with different psychiatric comorbidity. ActaPsychiatrScand 104: 59-65.
- Kokkevi A, Stefanis C (1995) Drug abuse and psychiatric comorbidity. Compr Psychiatry 36: 329-337.
- Ross HE, Glaser FB, Germanson T (1988) The prevalence of psychiatric disorders in patients with alcohol and other drug problems. Arch Gen Psychiatry 45: 1023-1031.
- Norman SB, Tate SR, Wilkins KC, Cummins K, Brown SA (2010) Posttraumatic stress disorder's role in integrated substance dependence and depression treatment outcomes. J Subst Abuse Treat 38: 346-355.
- Laudet AB, Magura S, Vogel HS, Knight E (2000) Support, mutual aid and recovery from dual diagnosis. Community Ment Health J 36: 457-476.
- Urbanoski KA, Rush BR, Wild TC, Bassani DG, Castel S (2007) Use of mental health care services by Canadians with co-occurring substance dependence and mental disorders. PsychiatrServ 58: 962-969.
- Kessler RC, McGonagle KA, Zhao S, Nelson CB, Hughes M, et al. (1994) Lifetime and 12-month prevalence of DSM-III-R psychiatric disorders in the United States. Results from the National Comorbidity Survey. Arch Gen Psychiatry 51: 8-19.
- Dennis ML, Scott CK, Funk R, Foss MA (2005) The duration and correlates of addiction and treatment careers. J Subst Abuse Treat 28 Suppl 1: S51-62.
- Broadman AP, Hodgson RE, Lewis M, Allen K (1999) North Staffordshire Community Beds Study: longitudinal evalution of psychiatric in-patient units attached to community mental health centres. I: Methods, outcome and patient satisfaction. Br J Psychiatry 175:70-78.
- Müller SE, Weijers HG, Böning J, Wiesbeck GA (2008) Personality traits predict treatment outcome in alcohol-dependent patients. Neuropsychobiology 57: 159-164.
- Blanchard JJ, Brown SA, Horan WP, Sherwood AR (2000) Substance use disorders in schizophrenia: review, integration, and a proposed model. ClinPsychol Rev 20: 207-234.
- Bradizza CM, Stasiewicz PR, Paas ND (2006) Relapse to alcohol and drug use among individuals diagnosed with co-occurring mental health and substance use disorders: a review. ClinPsychol Rev 26: 162-178.
- Meade CS, McDonald LJ, Graff FS, Fitzmaurice GM, Griffin ML, et al. (2009) A prospective study examining the effects of gender and sexual/physical abuse on mood outcomes in patients with co-occurring bipolar I and substance use disorders. Bipolar Disord 11: 425-433.
- Edlund MJ, Harris KM (2006) Perceived effectiveness of medications among mental health service users with and without alcohol dependence. PsychiatrServ 57: 692-699.
- Wüsthoff LE, Waal H, Ruud T, Gråwe RW (2011) A cross-sectional study of patients with and without substance use disorders in Community Mental Health Centres. BMC Psychiatry 11: 93.
- Urbanoski KA, Cairney J, Bassani DG, Rush BR (2008) Perceived unmet need for mental health care for Canadians with co-occurring mental and substance use disorders. PsychiatrServ 59: 283-289.
- Compton WM, Thomas YF, Stinson FS, Grant BF (2007) Prevalence, correlates, disability, and comorbidity of DSM-IV drug abuse and dependence in the United States: results from the national epidemiologic survey on alcohol and related conditions. Psychol Med 64:566-576.
- Rush B, Urbanoski K, Bassani D, Castel S, Wild TC, et al. (2008) Prevalence of co-occurring substance use and other mental disorders in the Canadian population. Can J Psychiatry 53: 800-809.
- Tuchman E (2010) Women and addiction: the importance of gender issues in substance abuse research. J Addict Dis 29: 127-138.
- Kay A, Taylor TE, Barthwell AG, Wichelecki J, Leopold V (2010) Substance use and women's health. J Addict Dis 29: 139-163.
- Kelly TM, Daley DC, Douaihy AB (2012) Treatment of substance abusing patients with comorbid psychiatric disorders. Addict Behav 37: 11-24.
- Encrenaz G, Messiah A (2006) Lifetime psychiatric comorbidity with substance use disorders: does healthcare use modify the strength of associations ?Soc Psychiatry PsychiatrEpidemiol 41: 378-385.
- Strakowski SM, DelBello MP (2000) The co-occurrence of bipolar and substance use disorders. ClinPsychol Rev 20: 191-206.
- Erfan S, Hashim AH, Shaheen M, Sabry N (2010) Effect of comorbid depression on substance use disorders. SubstAbus 31: 162-169.
- Compton MT, Weiss PS, West JC, Kaslow NJ (2005) The association between substance use disorders, schizophrenia-spectrum disorders, and Axis IV psychosocial problems. Soc Psychiatry PsychiatrEpidemiol 40:939-946.
- Dickey B, Azeni H (1996) Persons with dual diagnoses of substance abuse and major mental illness: their excess costs of psychiatric care. Am J Public Health 86: 973-977.
- Verduin ML, Carter RE, Brady KT, Myrick H, Timmerman MA (2005) Health service use among persons with comorbid bipolar and substance use disorders. PsychiatrServ 56: 475-480.
- Fleury MJ, Grenier G, Bamvita JM, Perreault M, Caron J (2012) Determinants associated with the utilization of primary and specialized mental health services. Psychiatr Q 83: 41-51.
- Fleury MJ, Grenier G, Bamvita JM, Tremblay J, Schmitz N, et al. (2013) Predictors of quality of life in a longitudinal study of users with severe mental disorders. Health Qual Life Outcomes 11: 92.
- Bohn MJ, Babor TF, Kranzler HR (1995) The Alcohol Use Disorders Identification Test (AUDIT): validation of a screening instrument for use in medical settings. J Stud Alcohol 56: 423-432.
- Skinner HA (1982) The drug abuse screening test. Addict Behav 7: 363-371.
- Accietto C (2003) La validation d'une version française du questionnaire A.U.D.I.T. "Alcohol Use Identification Test" (Genève, Université de Genève).
- Saunders JB, Aasland OG, Babor TF, de la Fuente JR, Grant M (1993) Development of the Alcohol Use Disorders Identification Test (AUDIT): WHO Collaborative Project on Early Detection of Persons with Harmful Alcohol Consumption--II. Addiction 88: 791-804.
- Cocco KM, Carey KB (1998) Psychometric properties of the Drug Abuse Screening Test in Psychiatric Outpatients. Psychological Assessment 10:408-414.
- Cutrona CE (1986) Behavioral manifestations of social support: a microanalytic investigation. J PersSocPsychol 51: 201-208.
- O'Malia L, McFarland BH, Barker S, Barron NM (2002) A level-of-functioning self-report measure for consumers with severe mental illness. PsychiatrServ 53: 326-331.
- Phelan M, Slade M, Thornicroft G, Dunn G, Holloway F, et al. (1995) The Camberwell Assessment of Need: the validity and reliability of an instrument to assess the needs of people with severe mental illness. Br J Psychiatry 167: 589-595.
- Caron J (2012) Predictors of quality of life in economically disadvantaged populations in Montreal. Social Indicator Research 107:411-427.
- Fleury MJ, Grenier G, Bamvita JM, Tremblay J (2013) Factors associated with needs of users with severe mental disorders. Psychiatr Q 84: 363-379.
- AdlafE, Blackburn J, Demers A, Kellner F, Single E, Webster I (1997) Social determinants, alcohol consumption and health: a secondary analysis of Canada's Alcohol and other drugs Survey (1994) (Canada, CCSA).
- Puchala C, Leis A, Lim H, Tempier R (2013) Official language minority communities in Canada: is linguistic minority status a determinant of mental health? Can J Public Health 104: S5-5S11.
- Tempier R, Vasiliadis HM, Gilbert F, Demyttenaere K, Bruffaerts R, et al. (2010) Comparing mental health of Francophone populations in Canada, France, and Belgium: 12-month prevalence rates of common mental disorders (Part 1). Can J Psychiatry 55:289-294.
- Tempier R1, Meadows GN, Vasiliadis HM, Mosier KE, Lesage A, et al. (2009) Mental disorders and mental health care in Canada and Australia: comparative epidemiological findings. Soc Psychiatry PsychiatrEpidemiol 44: 63-72.
- Otero-Sabogal R, Sabogal F, Perez-Stable EJ, Hiatt RA (1995) Dietary practices, alcohol consumption, and smoking behavior: ethnic, sex, and acculturation differences. J Natl Cancer InstMonogr 18:73-82.
- Cahn CH (1981) Douglas Hospital, 100 years of history and progress (Montreal, Douglas Hospital).
- O'dwyer P (2001) The Irish and substance abuse.in: Straussner SLA (edn) Ethnocultural factors in substance abuse treatment, pp. 199-215 (New York, The Guilford Press).
- Fleury MJ, Piat M, Grenier G, Bamvita JM, Boyer R, et al. (2010) Components associated with adequacy of help for consumers with severe mental disorders. Adm Policy Ment Health 37: 497-508.
- vanVugt MD, Kroon H, Delespaul PA, Mulder CL (2014) Assertive community treatment and associations with substance abuse problems. Community Ment Health J 50: 460-465.
- Baksheev GN, Thomas SD, Ogloff JR (2010) Psychiatric disorders and unmet needs in Australian police cells. Aust N Z J Psychiatry 44: 1043-1051.
- Greenfield TK, Room R (1997) Situational norms for drinking and drunkenness: trends in the US adult population, 1979-1990. Addiction 92: 33-47.
- Kessler RC, Crum RM, Warner LA, Nelson CB, Schulenberg J, et al. (1997) Lifetime co-occurrence of DSM-III-R alcohol abuse and dependence with other psychiatric disorders in the National Comorbidity Survey. Arch Gen Psychiatry 54: 313-321.
- Grella CE, Karno MP, Warda US, Niv N, Moore AA (2009) Gender and comorbidity among individuals with opioid use disorders in the NESARC study. Addict Behav 34: 498-504.
- Mueser KT, Yarnold PR, Levinson DF, Singh H, Bellack AS, et al. (1990) Prevalence of substance abuse in schizophrenia: demographic and clinical correlates. Schizophr Bull 16: 31-56.
- Westreich L, Guedj P, Galanter M, Baird D (1997) Differences between men and women in dual-diagnosis treatment. Am J Addict 6: 311-317.
- Shapiro S, Skinner EA, Kessler LG, Von Korff M, German PS, et al. (1984) Utilization of health and mental health services. Three Epidemiologic Catchment Area sites. Arch Gen Psychiatry 41:971-978.
- Hansson L, Björkman T, Svensson B (1995) The assessment of needs in psychiatric patients. Interrater reliability of the Swedish version of the Camberwell Assessment of Needs instrument and results from a cross-sectional study. ActaPsychiatrScand 92: 285-293.
- Middelboe T, Mackeprang T, Hansson L, Werdelin G, Karlsson H, et al. (2001) The Nordic Study on schizophrenic patients living in the community. Subjective needs and perceived help. Eur Psychiatry 16: 207-214.
- Korkeila J, Heikkilä J, Hansson L, Sørgaard KW, Vahlberg T, et al. (2005) Structure of needs among persons with schizophrenia. Soc Psychiatry PsychiatrEpidemiol 40: 233-239.
- Weiss RD, Griffin ML, Mazurick C, Berkman B, Gastfriend DR, et al. (2003) The relationship between cocaine craving, psychosocial treatment, and subsequent cocaine use. Am J Psychiatry 160: 1320-1325.
- Krishnan KR (2005) Psychiatric and medical comorbidities of bipolar disorder. Psychosom Med 67: 1-8.
- Azorin JM, Belzeaux R, Kaladjian A, Adida M, Hantouche E, et al. (2013) Risks associated with gender differences in bipolar I disorder. J Affect Disord 151: 1033-1040.
- Séguin M, Lesage A, Chawky N, Guy A, Daigle F, et al. (2006) Suicide cases in New Brunswick from April 2002 to May 2003: the importance of better recognizing substance and mood disorder comorbidity. Can J Psychiatry 51: 581-586.
- Barlow K, Grenyer B, Ilkiw-Lavalle O (2000) Prevalence and precipitants of aggression in psychiatric inpatient units. Aust N Z J Psychiatry 34: 967-974.
- Donald M, Dower J, Kavanagh D (2004) Integrated versus non-integrated management and care for clients with co-occurring mental health and substance use disorders: a qualitative systematic review of randomised controlled trials. SocSci Med 60:1371-1783.
- Brochu S, Cousineau MM, Provost C, Erickson P, Fu S (2010) Quand drogues et violence se rencontrent chez les jeunes: un cocktail explosif? Drogues, santé etsociété 9:149-178.
- Brunette M, Drake RE (1998) Gender differences in homeless persons with schizophrenia and substance abuse. Community Ment Health J 34: 627-642.
- Beckman LJ, Bardsley PE (1986) Individual characteristics, gender differences and drop-out from alcoholism treatment. Alcohol Alcohol 21: 213-224.
- Moos RH, Moos BS (2007) Treated and untreated alcohol-use disorders: course and predictors of remission and relapse. Eval Rev 31: 564-584.
Relevant Topics
- Addiction Recovery
- Alcohol Addiction Treatment
- Alcohol Rehabilitation
- Amphetamine Addiction
- Amphetamine-Related Disorders
- Cocaine Addiction
- Cocaine-Related Disorders
- Computer Addiction Research
- Drug Addiction Treatment
- Drug Rehabilitation
- Facts About Alcoholism
- Food Addiction Research
- Heroin Addiction Treatment
- Holistic Addiction Treatment
- Hospital-Addiction Syndrome
- Morphine Addiction
- Munchausen Syndrome
- Neonatal Abstinence Syndrome
- Nutritional Suitability
- Opioid-Related Disorders
- Relapse prevention
- Substance-Related Disorders
Recommended Journals
Article Tools
Article Usage
- Total views: 37142
- [From(publication date):
specialissue-2014 - Sep 04, 2025] - Breakdown by view type
- HTML page views : 28196
- PDF downloads : 8946