Rare Adult Sinonasal Embryonal Rhabdomyosarcoma with Optic Involvement
Received: 02-Apr-2011 / Accepted Date: 06-Jul-2012 / Published Date: 18-Jul-2012 DOI: 10.4172/2161-119X.1000118
Abstract
Rhabdomyosarcoma of the Paranasal sinus accounts for 10% to 15% of adult head and neck Rhabdomyosarcoma. We presented a 32-year-old man with a month history of the right eye vision loss and had no common symptoms as nasal obstruction or headache. The adult patients, who have nasal symptoms along with eye complaints, should be examined with nasal endoscopy by an otorhinolaryngologist and Rhabdomyosarcoma must be kept on mind in terms of differential diagnosis.
Keywords: Rhabdomyosarcoma, Adult paranasal sinus, Vision loss
251440Introduction
Rhabdomyosarcoma (RMS) is a fast growing, highly malignant and the most common sarcoma in childhood ages. RMS grows from mesenchymal tissue and RMS of the Paranasal sinus accounts for 10% to 15% of adult head and neck RMS [1,2]. Nasal obstruction, pain, proptosis, limitation of eye movement and vision loss are the common symptoms but, only eye symptoms without nasal symptoms are observed less often depending on the involvement region [3]. Radiotherapy and chemotherapy is preferred with a combination of surgery for treatment [4].
Case Report
32-year-old man was presented with a month history of the right eye vision loss, and the patient was followed by an ophthalmologist with diagnosis of the right eye optic papillitis. The patient was referred to Ear Nose Throat (ENT) department, because the complaints did not improve with medical treatment. The medical history was otherwise unremarkable. The nasal endoscopic examination revealed the presence of a homogeneous, blue-purple colour and well vascularised mass and the mass filled out the right middle meatus and pushed the middle turbinate medially. There was proptosis in the right side, but there was no restriction of eye movements. The retinal posterior pole of the right eye rose, and optic disc elevated in ophthalmoscopic examination. Visual acuity was assessed as counting fingers at 20 cm in the right eye. There was no palpable lymph node in neck examination.
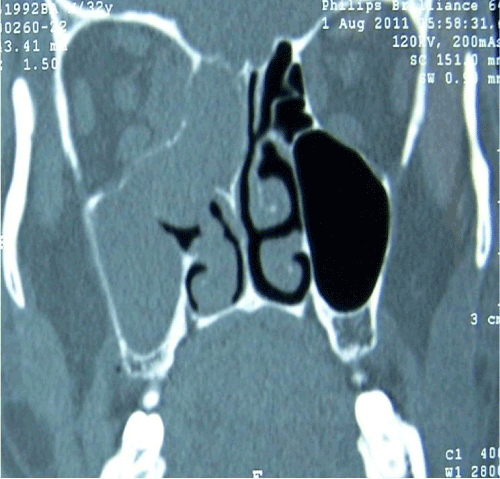
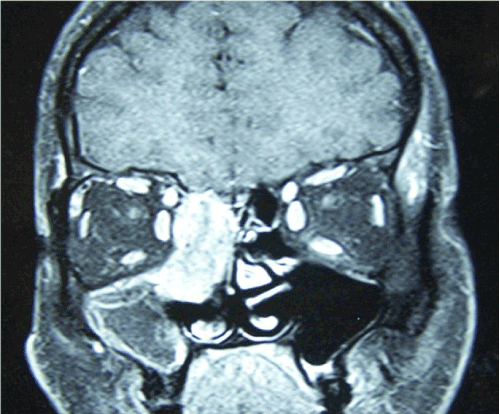
A Computed Tomography (CT) scans of the paranasal sinus showed a “homogeneous soft” tissue mass without calcification in the right middle-upper meatus, and maxillary sinus. There was minimal damage at medial wall of right orbit (Figure 1). The mass caused a deletion between extraconal and muscle plans through right orbital apex localization, but no destruction was observed at ethmoid apex on Magnetic Resonance Images (MRI) (Figure 2).
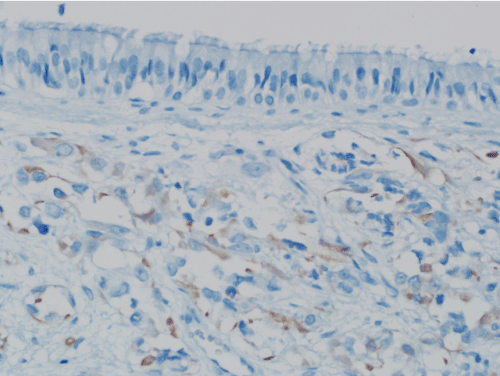
Navigation-assisted endoscopic complete excision of the tumour was done for surgical treatment. Immuno-histochemical examination of the mass showed strongly positive desmin (Figure 3) and positive myogenin but negative S-100, chromogranin and CD-99. It was reported as embryonal RMS.
Discussion
RMS is a fast growing, highly malignant and the most common sarcoma in childhood ages. RMS grows from mesenchymal tissue and accounts nearly for 5% to 10% of all childhood malignancies [1]. RMS is less frequently in adults than childhood [1]. There are some different clinical features between adult and child patients of RMS. Pediatric Rhabdomyosarcoma show a male preponderance, but it is not noted in adult patients. Our case was adult and RMS was located in the head and neck region but mostly adult RMS occurs in the extremities, while pediatric rhabdomyosarcoma occur predominantly in the head and neck sites [1]. RMS arises in the head and neck region in 40% of the cases, but it is less with a rate of 15% in adult RMS [2,3]. RMS of the paranasal sinus accounts for 10% to 15% of adult head and neck RMS.According to the localization of the head-neck region, RMS found in three sites; orbital, parameningeal (nasal cavity, paranasal sinus, nasopharynx, infratemporal fossa) and superficial (pharynx, scalp, buccal mucosa, parotid, external ear, tonsil, face) [2,3].
Ahmed and Tsokos [2] reported 14 cases with paranasal sinus involvement of the 39 patients with head and neck RMS. There were 9 ethmoidal and 5 maxillary sinus involvements [2]. RMS of the paranasal sinus is often arising from ethmoid and maxillary region and is locally aggressive tumour. Our case was determined in ethmoid sinus. Even the etiology is unknown, regional radiation is accused mostly. However, in a study, only two patients with RMS had a history of radiation in 13 adult cases [5] and also our case had no history of radiation.
Nasal congestion, rhinorrhea and nasal bleeding are the most common symptoms in sinonasal RMS. Pain, proptosis, limitation of eye movement and vision loss can be seen depending on the involvement region [3]. The initial symptoms were proptosis and vision loss due to compression of orbit in our case. Orbital involvement is an insidious and rapid clinical course and can lead to blindness [4]. Our case had only right eye vision loss without any additional symptoms and this made a delay for diagnosis for nearly one month. So if an adult patient has unilateral eye vision loss with or without nasal symptoms, endoscopic evaluation should be done in terms of differential and early diagnosis.
Subtypes of RMS are embryonal (70%), alveolar (20%) and other subtypes (10%). Alveolar subtype has the worst prognosis [5]. Alveolar rhabdomyosarcoma (ARMS) has a distinct histological appearance and usually presents in the soft tissues of the extremities, but Embryonal Rhabdomyosarcoma (ERMS) is often associated with mucosal or epithelial surfaces. ERMS is particularly found in the biliary system, vagina, head and neck, paratesticular region and urinary bladder. Pleomorphic RMS is more often encountered in adults than childhood. Our case was embryonal subtype. In sinonasal tract RMS is predominantly alveolar type [2,5] and ERMS is rare and our case was an adult ethmoidal ERMS. Ahmed and Tsokos [2] reported 14 sinonasal RMS with an age range of 9 to 40 and only one patient was left maxillary ERMS and others were ARMS. Another study reported 12 adult sinonasal RMS and 2 of them were ERMS and among ERMS, one patient had an ethmoid involving as in our case [5].
CT and MRI should be done to assess the spread of the disease and the relationship between the neighbourhood structures. CT shows the margins and relation with vital structures of masses. MRI provides superior soft tissue resolution and has high sensitivity in the pterygopalatine fossa, sinuses, and the infra temporal fossa for tumour extension. There is a high rate of distant metastasis in adults’ more than pediatric groups, so all-body Positron Emission Tomography (PET) scanning is recommended. Our case had no distant metastases in PETCT scan.
Endoscopy and biopsy are required to confirm the diagnosis and then pathological examination gives definitive diagnosis. There are not any pathognomonic endoscopic findings in RMS. Small paranasal sinus masses could not be identified endoscopically. Desmin and myogenin is painted as positive but cytokeratin, epithelial membrane antigen, CD45, CD99, S-100 are painted as negative in immunohistochemical examination [2,6]. The pattern of immunostaining for myogenin has been used to aid in the distinction of ARMS from ERMS [5]. Embryonal tumours characteristically show myogenin in < 50% of cells as in our case. We did not perform cytogenetic and RT-PCR analysis because the tumour cells are well differentiated and we gave careful attention to use histological ancillary techniques and immunostains to clarify this differential diagnosis. This undifferentiated histology can mimic other round-cell tumours, such as lymphoma, Ewing sarcoma, and olfactory neuroblastoma [7].
Ectopic pituitary adenoma, metastatic undifferentiated carcinoma, inflammatory nasal polyposis, inverted papilloma, schwannoma, pleomorphic adenoma, squamous cell carcinoma, lymphoma, osteogenic sarcoma, fibrosarcoma, chondrosarcoma and olfactory neuroblastoma might be considered in the differential diagnosis in nasal cavity masses [7]. Although RMS is distinctly rare in the sinonasal tract in adults, it should always be a consideration when a poorly differentiated malignant neoplasm is presented in sinonasal region regardless of the age of the patient.
The prognosis depends on the primary site, the histological subtype and tumour size [8]. Good prognosis for survival are; tumour to be smaller than 5 cm, the patients under 20 years of age, lack of regional or distant metastasis and negative surgical margins [6,9]. Tumours of the orbit have a better prognosis. Parameningeal RMS has more recurrence rates and has much more early metastasis because of the possibility of intracerebral spread [8]. Distant metastasis occurs in adults at the time of diagnosis in 60% of cases [1]. The 5-year survival rates are 56% to 65% [8]. There is not a fully-formed adult treatment protocol, but complete excision of the mass in pediatric treatment protocol is the prognostic factor that increases local control and survival [8].
Treatment of the RMS varies depending on the pathologic and clinical stage. Radiotherapy and chemotherapy are preferred with a combination of surgery [4]. Callender et al. reported 75% locoregional recurrence rate among patients with RMS after surgery [10]. Surgery is not used as a primary treatment modality [10]. The Intergroup Rhabdomyosarcoma Study Group (IRSG) recommends surgery for initial therapy, if there will be no functional loss followed by chemotherapy [11]. Patients have a better prognosis if the mass is resected completely. Residual tumour masses could be removed after chemotherapy [11]. Adult RMS is radiosensitive as other adult sarcomas, so radiotherapy is another choice of treatment modality. Occult lymph node metastases are uncommon; therefore, preventive neck dissection is not indicated. Endoscopic complete mass excision was done successfully instead of open surgery in our case, and chemotherapy was added, but radiotherapy was not preferred. No recurrence was observed during follow up for six months.
Conclusion
RMS is the most common sinonasal tumour in childhood age, but it is extremely rare in adults. Patients with sinonasal tumours often have nasal symptoms but also insidious eye symptoms could be seen rarely. If an adult patient has unilateral nasal complaint with eye symptoms, endoscopic evaluation should be done in terms of differential and early diagnosis by an otorhinolaryngologist.
References
- Wu TH, Huang JS, Wang HM, Wang CH, Yeh KY (2010) Long-term Survivors of Adult Rhabdomyosarcoma of Maxillary Sinus Following Multimodal Therapy: Case Reports and Literature Reviews. Chang Gung Med J 33: 466-471.
- Ahmed AA, Tsokos M (2007) Sinonasal rhabdomyosarcoma in children and young adults. Int J Surg Pathol 15: 160-5.
- Sturgis EM, Potter BO (2003) Sarcomas of the head and neck region. Curr Opin Oncol 15: 239-252.
- Karcioglu ZA, Hadjistilianou D, Rozans M, DeFrancesco S (2004). Orbital rhabdomyosarcoma.Cancer Control 11: 328-33.
- Montone KT, Barr FG, Zhang PJ, Feldman MD, LiVolsi VA (2009) Embryonal and alveolar rhabdomyosarcoma of parameningeal sites in adults: a report of 13 cases. Int J Surg Pathol 17: 22-30.
- Simon JH, Paulino AC, Smith RB, Buatti JM (2002) Prognostic factors in head and neck rhabdomyosarcoma. Head Neck 24: 468-473.
- Toda T, Atari E, Sadi AM, Kiyuna M, Kojya S (1999) Primitive neuroectodermal tumor in sinonasal region. Auris Nasus Larynx 26: 83-90.
- Crist WM, Anderson JR, Meza JL, Fryer C, Raney RB, et al (2001) Intergroup rhabdomyosarcoma study-IV: results for patients with nonmetastatic disease. J Clin Oncol 19: 3091-3102.
- Ulutin C, Bakkal BH, Kuzhan O (2008) A Cohort Study of Adult Rhabdomyosarcoma: A single Institution Experience. World Journal of Medical Sciences 3: 54-59
- Callender TA, Weber RS, Janjan N, Benjamin R, Zaher M, et al (1995) Rhabdomyosarcoma of the nose and paranasal sinuses in adults and children. Otolaryngol Head Neck Surg 112: 252-7.
- Moretti G, Guimarães R, Oliveira KM, Sanjar F, Voegels RL (2010) Rhabdomyosarcoma of the head and neck: 24 cases and literature review. Braz J Otorhinolaryngol 76: 533-537.
Citation: Erkul E, Pinar D, Yilmaz I, Cincik H, Cekin E, et al. (2012) Rare Adult Sinonasal Embryonal Rhabdomyosarcoma with Optic Involvement. Otolaryngology 2:118. DOI: 10.4172/2161-119X.1000118
Copyright: © 2012 Erkul E, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 16524
- [From(publication date): 8-2012 - Nov 04, 2025]
- Breakdown by view type
- HTML page views: 11728
- PDF downloads: 4796