Reliability of Two Surgical Methods for Oroantral Communication Closure; A Clinical Study of 20 Patients
Received: 28-Mar-2012 / Accepted Date: 01-May-2012 / Published Date: 07-May-2012 DOI: 10.4172/2161-119X.1000113
251229Introduction
An Oroantral Communication (OAC) is an open connection between the oral cavity and maxillary sinus. OAC is an uncommon complication in oral surgery and occurs mostly at the upper first molar, followed by the second molar, third molar, and bicuspid. OAC is frequently encountered in patients who undergo large numbers of extractions [1-4].
OACs may close spontaneously, especially when the defect is <5 mm. Nevertheless, to our knowledge, it has never been shown that small OACs (5 mm) heal by themselves. Additionally, it is difficult to determine the size of the OAC clinically. If the communication is not diagnosed and managed properly, there is a risk that an epithelialized permanent oroantral fistula with resultant maxillary sinusitis, a prevalent complication, may develop [5]. To prevent chronic sinusitis and the development of fistulas, it is generally accepted that all of these defects should be closed within 24 to 48 hours [6].
The primary cause of OAC is the anatomic proximity of the root apices to the sinus floor or projection of the roots into the maxillary sinus. Other causes of OAC include dentoalveolar infections, destruction of a portion of the sinus by cysts or benign or malignant tumors, Paget's disease, trauma, complication of the Caldwell–Luc procedure, and dentoalveolar or implant surgery [3,7-9].
Several methods of surgical OAC repair have been described, but only a few have gained wide acceptance. The choice among these procedures is influenced by not only the amount and condition of the tissue available for repair but also the size and location of the defect. In the present study, we evaluated the reliability of two OAC closure technics. The influence of various clinical parameters on the success rate was analyzed.
Materials and Methods
A total of 20 patients who were referred to Istanbul University, Faculty of Dentistry, Department of Oral Surgery with OAC were selected for this study. The patients who were above ASA 2 and immunocompromised and who have previously operated were excluded from the study.
The diagnosis was established by the nose-blowing test and introduction of a silver probe into the antrum through the fistula. Before surgery, the patients were examined, and periapical and panoramic radiographs were taken to evaluate the size of the bone defect and presence of sinusitis or foreign material within the sinus. The age, gender, location, size, and duration of the OAC and features of antral infection were recorded. Ten patients were treated with Buccal Advancement Flaps (BAFs), and 10 were treated with Palatal Rotation–Advancement Flaps (PRAF). All surgeries were performed by the same surgeon.
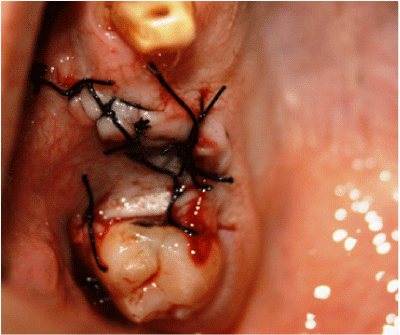
In the BAF procedures, a broad-based trapezoid mucoperiosteal flap was created. After cleaning the fistula, the alveolar bone was smoothed, and the flap was advanced and sutured to the palatinal tissue with silk suture material (3-0 Doğsan, Trabzon, Turkey) (Figure 1).
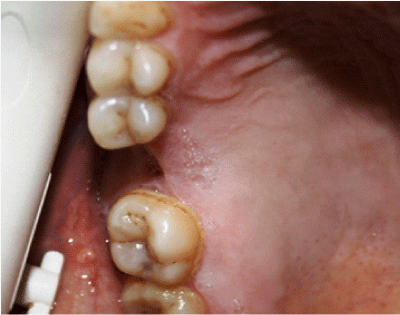
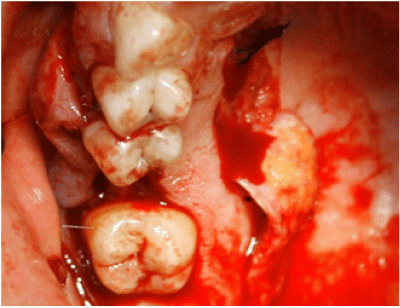
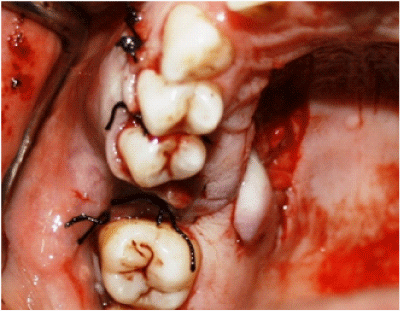
For PRAF procedures, full-thickness mucoperiosteal flaps were designed based on the greater palatine vessels. The anterior extension of the flap was determined by measuring the distance of the arc of flap rotation, i.e., the distance from the greater palatine foramen to the lateral–anterior bony fistula border. The width of the flap was determined by the bony defect and angle of rotation. The medial border of the flap was 2 to 3 mm lateral to the mid-palatal raphe. At the lateral border, a strip of about 5 mm of palatal marginal gingiva beside the teeth was left to avoid periodontal damage. The alveolar bone was smoothed, and the PRAF was rotated, advanced, and sutured to the buccal tissue with vertical and simple mattress sutures using silk suture material (3-0 Doğsan, Trabzon, Turkey) (Figures 2-4).
After PRAF surgery, a surgical splint was prepared and used for 1 week. The surgical splints were prepared in a nonpressure-fit fashion to allow for nutrition of the flaps.
After the operations, the patients were instructed to avoid activities that may produce pressure changes between the nasal passages and oral cavity for at least 2 weeks, such as sucking on a straw, blowing the nose, and sneezing with a closed mouth. The patients were placed on a soft diet during this period. Antibiotics and nasal decongestants were given for 1 week postoperatively.
Sutures were removed 10 days after the surgery. The results were assessed at 1 and 3 months postoperatively. Acute sinus disease was treated with amoxicillin/clavulanate (1 g/125 mg × 3/d for 10–14 d), nasal decongestants, and Nonsteroidal Anti-Inflammatory Drugs (NSAIDs ). No chronic sinus disease was seen in this study.
The criterion for successful repair was complete healing of the flap without symptoms or signs of leakage. Follow-up evaluations were performed at 15 days, 1 month, and 3 months after treatment.
Results
All patients in the PRAF group were male, and the mean age in this group was 55 years. In the BAF group, two patients were female, and the mean age in his group was 34 years (Table 1).
| Technique | Patient | Gender | Age (y) | Fistula region | Etiology | Size (mm) | Complications |
|---|---|---|---|---|---|---|---|
| BAF | 1 | M | 54 | Right first molar | Tooth extraction | <5 | No |
| BAF | 2 | M | 39 | Left fist molar | Tooth extraction | <5 | No |
| BAF | 3 | F | 41 | Right second molar | Tooth extraction | <5 | No |
| BAF | 4 | M | 20 | Right third molar | Tooth extraction | <5 | No |
| BAF | 5 | F | 54 | Left second molar | Tooth extraction | <5 | No |
| BAF | 6 | M | 32 | Right first molar | Tooth extraction | <5 | No |
| BAF | 7 | M | 32 | Right first molar | Tooth extraction | <5 | No |
| BAF | 8 | M | 28 | Right first molar | Tooth extraction | <5 | No |
| BAF | 9 | M | 28 | Left first molar | Tooth extraction | <5 | No |
| BAF | 10 | M | 42 | Left second molar | Tooth extraction | <5 | No |
| PRAF | 11 | M | 43 | Left second molar | Tooth extraction | >5 | No |
| PRAF | 12 | M | 73 | Left first molar | Odontogenic cyst | >5 | Yes |
| PRAF | 13 | M | 46 | Left first molar | Tooth extraction | >5 | No |
| PRAF | 14 | M | 65 | Left second molar | Tooth extraction | >5 | No |
| PRAF | 15 | M | 54 | Left second molar | Odontogenic cyst | >5 | No |
| PRAF | 16 | M | 47 | Right second molar | Tooth extraction | >5 | No |
| PRAF | 17 | M | 71 | Left second molar | Tooth extraction | >5 | No |
| PRAF | 18 | M | 56 | Right second molar | Tooth extraction | >5 | No |
| PRAF | 19 | M | 44 | Left second molar | Tooth extraction | >5 | No |
| PRAF | 20 | M | 54 | Left first molar | Tooth extraction | >5 | No |
Table 1: Distribution of patient characteristics, defect region, size, etiology, and surgical techniques (BAF: Buccal Advancement Flap, PRAF: Palatal Rotation–Advancement Flap).
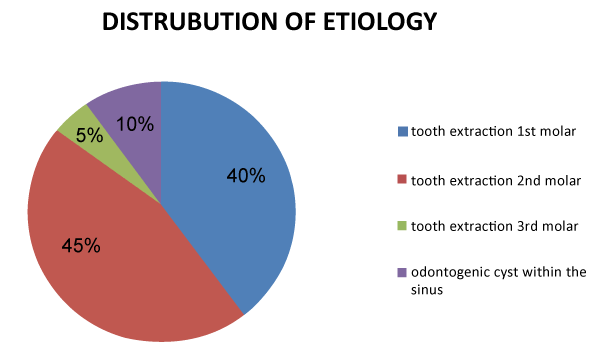
We preferred PRAF when the defect size was >5 mm; smaller defects were treated with BAF. The main reason for the OAC was second molar extraction (45%), followed by first molar extraction (40%), odontogenic cyst within the sinus (10%), and invasions and third molar extraction (5%) (Figure 5).
Of the 20 patients, 19 healed uneventfully. The donor site of the palatal flap was completely healed 3 months postoperatively, and grafts were not necessary. No flap necrosis was found in either group, with the exception of one patient who had undergone the Caldwell–Luc procedure and the palatal island flap technique. In this case, a second surgical intervention was performed, and an autogenous cartilage graft was harvested from the ear. This graft was placed in the bone defect, and soft tissue closure was obtained with a palatal advancement flap.
Discussion
Oroantral fistulas can arise as late sequelae from complex facial trauma, infection, tumors, maxillary molar extraction, or radiation. Patients with oroantral fistulas are prone to chronic respiratory infections due to the persistent communication of the sinuses with food and oral secretions. Complications frequently include cellulitis of the surrounding soft tissue, sinusitis, and, in rare cases, central nervous system infections [10]. Extraction of the upper second molar was the most frequent cause in our sample.
Buccal flaps are preferable for closure of small (<5 mm) and immediate OAC [11]. Flap coverage is improved by horizontal periosteal incisions. The flap may also result in a very shallow vestibular sulcus, which can interfere with prosthodontic rehabilitation and maintenance of oral hygiene. Although lauded for their ease of performance and good blood supply, buccal flaps require careful manipulation [9]. In contrast, a reduction in the buccal sulcus depth is currently becoming less of a problem with the possibility of implant-retained overdentures. We encountered no complication after BAFs.
All palatal flaps are based on the greater palatine artery, and its integrity has been considered an important success factor. In anteriorly based palatal flaps, the terminal part of the greater palatine artery is its nasopalatine branch, which ascends up through the incisive foramen into the nose, where it anastomoses with the septal branches of the sphenopalatine artery. This establishes the basis for retrograde flow through the nasopalatine artery when the greater palatine neurovascular bundle is transected [12]. An appropriate length/ width ratio is important for the success of random flaps. The success rate of the flap can be improved by optimization of the length/width ratio [5]. In this study, PRAFs were successfully used in nine patients. One dehiscence was observed in an older male patient, and a second surgical intervention was performed. An autogenous cartilage graft was harvested from the ear, the graft was placed in the bone defect, and soft tissue closure was obtained with a palatal advancement flap.
In conclusion, a buccal or palatal flap still seems to be the treatment of choice for OAC when primary suturing of the gingiva does not provide adequate closure of the communication. We suggest BAF rather than PRAF for fistulas smaller than 5 mm because the intact bony interface underneath the fistula provides sufficient support against trauma to the flap during the healing period. In wider fistulas, PRAF should be chosen for support of the soft tissue. Buccal flaps may result in a very shallow vestibular sulcus, which can interfere with prosthodontic rehabilitation and maintenance of oral hygiene, whereas palatal flaps have excellent blood supply, and the buccal sulcus remains intact. As a result, we conclude that the treatment choice should be individualized based on the size of the communication and carefully planned to avoid undesired results.
References
- Visscher SH, van Minnen B, Bos RR (2010) Closure of oroantral communications: a review of the literature. J Oral Maxillofac Surg 68: 1384-1391.
- Ehrl PA (1980) Oroantral communication. Epicritical study of 175 patients, with special concern to secondary operative closure. Int J Oral Surg 9: 351-358.
- Guven O (1998) A clinical study on oroantral ?stulae. J Craniomaxillofac Surg 26: 267-271.
- Punwutikorn J, Waikakul A, Pairuchvej V (1994) Clinically signi?cant oroantral communications--a study of incidence and site. Int J Oral Maxillofac Surg 23: 19-21.
- Lee JJ, Kok SH, Chang HH, Yang PJ, Hahn LJ, et al. (2002) Repair of oroantral communications in the third molar region by random palatal ?ap. Int J Oral Maxillofac Surg 31: 677-680.
- Poeschl PW, Baumann A, Russmueller G, Poeschl E, Klug C, et al. (2009) Closure of oroantral communications with Bichat's buccal fat pad. J Oral Maxillofac Surg 67: 1460-1466.
- Babajews A (1986) Multiple myeloma presenting as an oro-antral ?stula. Br J Oral Maxillofac Surg 24: 52-57.
- McMahon P, Tzadik A (1986) Paget's disease of the bone presenting as an apparent oral antral ?stula. Arch Otolaryngol Head Neck Surg 112: 668-670.
- Hernando J, Gallego L, Junquera L, Villarreal P (2010) Oroantral communications. A retrospective analysis. Med Oral Patol Oral Cir Bucal 15: e499-e503.
- Deune EG, Manson PN (2004) Use of the serratus anterior free flap to treat a recurrent oroantral fistula. J Craniofac Surg 15: 335-340.
- Yalcin S, Oncu B, Emes Y, Atalay B, Aktas I (2011) Surgical treatment of oroantral fistulas: a clinical study of 23 cases. J Oral Maxillofac Surg 69: 333-339.
- Anavi Y, Gal G, Silfen R, Calderon S (2003) Palatal rotation-advancement flap for delayed repair of oroantral fistula: a retrospective evaluation of 63 cases. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 96: 527-534.
Citation: Cankaya AB, Erdem MA, Cakarer S, Isler SC, Demircan S, et al. (2012) Reliability of Two Surgical Methods for Oroantral Communication Closure; A Clinical Study of 20 Patients. Otolaryngology 2:113. DOI: 10.4172/2161-119X.1000113
Copyright: © 2012 Cankaya AB, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 17000
- [From(publication date): 6-2012 - Dec 10, 2025]
- Breakdown by view type
- HTML page views: 12189
- PDF downloads: 4811