Research Article Open Access
Role of Two Clusters of Cocaine-Dependent Outpatients in Treatment Retention
Flavia Ismael1 and Danilo Antonio Baltieri1,2*1Department of Psychiatry, University of Sao Paulo, Brazil
2Department of Psychiatry, ABC Medical School, Santo Andre, Sao Paulo, Brazil
- *Corresponding Author:
- Danilo Antonio Baltieri
Avenida Angelica, nº 2100, conjunto 13
CEP: 01228-200, Sao Paulo, SP, Brazil
Tel: +5511-3120-6896
E-mail: dbaltieri@uol.com.br
Received September 03, 2012; Accepted October 29, 2012; Published November 02, 2012
Citation: Ismael F, Baltieri DA (2012) Role of Two Clusters of Cocaine-Dependent Outpatients in Treatment Retention. J Addict Res Ther 3:136. doi:10.4172/2155-6105.1000136
Copyright: © 2012 Ismael F, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Addiction Research & Therapy
Abstract
Background: Cocaine dependents are a highly heterogeneous population. An appropriate system of classification should represent a broad understanding of underlying psychosocial aspects of cocaine dependence, as well as being related to a therapeutic proposal, a possible prognosis, and different forms of approach. Our aim was to identify types of cocaine dependents and evaluate if these types show different retention rates in a cognitive behavioral treatment.
Methods: The sample comprised 100 cocaine-dependent outpatients who were enrolled in an individual and manualized cognitive-behavioral treatment. Classes of participants sharing common psychosocial features, cocaine use-related aspects, and impulsiveness were identified with latent class analysis. The association of sociodemographic, clinical, and psychological variables with treatment retention was also investigated.
Results: Two clusters were delineated. Participants belonging to cluster 1 (n=60) were characterized by higher impulsiveness level, more years of cocaine use, higher educational level, more previous treatment episodes for cocaine addiction, and more frequent family history of cocaine use problems than Cluster 2 (n=40). Cluster 1 persons adhered longer to the treatment. As to the independent variables, only the highest educational level and the route of administration (crack cocaine) were associated with higher treatment retention.
Conclusions: Information about patients’ characteristics linked to noncompliance or dropout should be used to make treatment programs more responsive and attractive, combining more intensive and diversified psychosocial interventions.
Keywords
Cocaine dependence; Cluster analysis; Behavioralcognitive treatment; Treatment retention
Introduction
Cocaine dependence is a destructive and often chronic illness that is difficult to treat. There are approximately 0.9 million current users of cocaine in Brazil, and the Southern Cone Countries together account for more than two-third of all cocaine users of South America. In North America, there are about 1.9 million current cocaine users, with the United States of America having the highest prevalence rate at 2.4% of the population aged between 15 and 64 [1]. However, to date there are no effective pharmacotherapies for cocaine dependence and standard psychosocial treatments seem not to be effective for some cocainedependent patients.
Substantial number of cocaine dependents leave treatment before completing the program and this contributes to negative consequences to their health, families, finances, and job performance. While treatment retention is poor across the majority of substance use treatment studies, treatment completion rates in cocaine clinical trials are about 50% or less [2]. This high dropout rate has prompted researchers to describe cocaine users as being a challenging population. In fact, cocaine dependents experience difficulty abstaining due to cognitive impairments from repeated cocaine use, high levels of life stress, and strong social and environmental cues [3-5]. In addition, development of treatments has been complicated by the tendency for dependents not to complete treatment programs and their propensity for relapse.
There is a vast literature about predictors of treatment retention in cocaine dependence. Relevant predictors can be grouped into sociodemographic factors (such as gender, age, educational level, family antecedents), clinical factors (such as severity of addiction, history of previous treatments), and psychological factors (such as impulsiveness, comorbid psychopathology [6-8]. In fact, lower education level [9], younger age [10], longer drug use history, more previous treatment episodes [11], and higher impulsiveness as measured by the Barratt Impulsiveness Scale (BIS-11) [6] have been associated with early dropout from cocaine dependence treatment. However, other studies have not found demographic characteristics [12], drug use severityrelated variables [13], and impulsivity [14] to be predictive of treatment retention. These inconsistencies can be due to the fact that several studies have tested a large number of variables separately without a rationale for selecting or combining predictors; furthermore, some studies have investigated only static predicting factors (such as age, race, educational level), and not included dynamic factors (such as impulsiveness) that could be influenced by intervention. In addition, these inconsistencies cast doubt on the relevance of the current literature on cocaine treatment retention.
Cocaine dependents are a highly heterogeneous population. Their categorization into more homogeneous groups has received little attention from mental health professionals worldwide, when compared to other individuals with addiction, such as alcohol dependents. An appropriate system of classification should represent a broad understanding of underlying neurobiological and psychosocial aspects of this dependence, as well as being related to a therapeutic proposal, a possible prognosis, and different forms of approach.
To date, a few typologies of cocaine dependents have been developed and based mainly on personality characteristics [15], cocaine use onset age [16], and cocaine use severity-related variables [17,18]. With reference to latter typological proposal, two types of cocaine dependents were identified. Type A showed less family antecedents of substance abuse, lower impulsiveness levels, later onset age of cocaine use, and lower cocaine consumption severity, in terms of frequency and duration, than Type B. However, it is unclear if different types of cocaine dependents show different treatment retention rates.
Based on these findings, we performed a latent class analysis to identify types of cocaine dependents, and evaluated if these types show different retention rates in a cognitive behavioral treatment. In order to construct a typology, we combined static with dynamic variables within a biopsychosocial addiction model. Thus, the following items were used to construct a typology: (a) socio-demographic (educational level, family antecedents of cocaine use problems), (b) clinical (years of cocaine use, previous treatment for cocaine addiction), and (c) psychological (impulsiveness levels) variables. In addition, we evaluated if certain personality aspects were associated with the resulting clusters. Subsequently, we verified if each socio-demographic, clinical, and psychological variable was directly and independently associated with treatment retention.
We are aware that treatment retention is not an outcome measure properly; however, the capacity to retain patients in active participation is a sensible measurement associated with quality and efficacy of the health care [19,20]. Also, according to the National Treatment Agency for Substance Misuse, retention in drug treatment is the better available measure of treatment effectiveness [21].
Methods
Participants
Male patients, 18-60 years of age, with an International Classification of Diseases (ICD-10; World Health Organization, 1992) diagnosis of cocaine dependence that enrolled as outpatients in the Assistance Sector of the Interdisciplinary Group of Studies on Alcohol and Drugs at the University of Sao Paulo (PROGREA) were assessed for this study. This service (PROGREA) is exclusively dedicated to the treatment of men with drug abuse and dependence.
Participants met the following inclusion criteria: (a) ICD-10 criteria for cocaine dependence; (b) report of cocaine use at least four times in the month prior to admission; and (c) duration of cocaine use for a period of at least 12 months preceding enrolment into the study. Exclusion criteria were: (a) <18 years or ≥ 60 years of age; (b) patients with serious clinical coexisting diseases (e.g., inadequately controlled diabetes, cardiac failure, alcoholic cirrhosis, seizure disorders); (c) previous treatment with any medication to treat cocaine addiction within 6 months of this study; (d) concomitant psychiatric disorders evaluated with the Mini International Neuropsychiatric Interview (MINI version 5.0) [22]; (e) current use of any psychotropic medications; (f) inability to give full informed consent; and (g) clinical history of mental retardation as it may reduce the accuracy of the information given.
They were informed about the objectives of the study and the nature of the treatment offered. All patients were assured about the confidentiality of the data and were informed that they were free to withdraw their consent and discontinue participation in the study at any time without prejudice to their continued medical care. After signing a screening consent, participants were psychiatrically and physically examined by our staff. This study was approved by the Ethics Committee of the Clinical Hospital of the University of São Paulo, Brazil. All participants were also encouraged to participate in Narcotic Anonymous groups (NA) but this was not an obligatory condition of participation in the study.
Measures
In the first interview, after a full history and clinical examination, patients who fulfilled entry criteria were evaluated. Socio-demographic data, lifetime drug history, family antecedents of cocaine problems, daily consumption of cocaine, cocaine use onset age, years of cocaine use, and preferential route of administration were obtained in a standardized semi-structured interview commonly used in the therapeutic setting of the Interdisciplinary Group of Studies on Alcohol and Drugs of the Clinical Hospital of the University of São Paulo, Brazil. All participants were evaluated with the following measures:
The Timeline Follow-Back (TLFB): This self-reported substance abuse method was used to obtain reports of alcohol and cocaine use at the screening visit (the previous 30 days), and in the weekly visits (daily use during treatment) [23,24]. The primary outcome measures derived from TLFB data were the amount and frequency of cocaine use. The TLFB was administered by a trained researcher at screening and each weekly visit throughout the trial.
ASI (Addiction Severity Index-6): It is a structured interview to assess drug and alcohol use and areas of functioning usually affected by substance abuse, such as medical, employment, family/ social, psychiatric, and legal [25]. In the 6th version, there is one set of summary scores available, the ASI-6 Summary Scores for Recent Functioning (SS-Rs). The SS-Rs refer to status/functioning in the past 30 days, and provides objective information derived from items based on a combination of rational and empirical methods. They are psychometrically derived using Nonparametric Item Response Theory (NIRT) and classical psychometric methods. There is one score in each problem area, except for family/social in which there are 3 different scores: family/social problems, family/social support, and child problems. They represent standardized T-scores with a mean of 50 and a SD of 10, theoretically ranging from 0-100. Higher scores indicate greater problem severity. The ASI-6 was validated in Brazil [26].
Minnesota Cocaine Craving Scale (MCCS): It is composed of five items which correspond to intensity, frequency, duration of craving, changes in relation to previous week, and craving response to medication. For this study, we used only the first three items of the scale (visual analogue scale, ranging from 0 to 10) because these items can be used independently [27].
TCI (Temperament and Character Inventory): It is a selfadministered psychometric instrument [28] validated in Brazil [29]. It measures seven personality dimensions following a theory in a psychobiological and dimensional model that integrates the role of certain neurotransmitters (serotonin, dopamine, noradrenaline) in regulating behavior. TCI scores were converted into T-scores according to published normative data and previous research [30]. These dimensions are divided into four scales of Temperament and three of Character. The temperament scales are:
1. Novelty Seeking (NS): Tendency towards exploratory activity in response to novelty, lack of inhibition, impulsiveness. This dimension is related to the level of control and excitability and corresponds to the sum of four subscales measuring more specific traits: Exploratory excitability (11 items), Impulsiveness (10 items), Extravagance (9 items), and Disorderliness (10 items).
2. Harm Avoidance (HA): Tendency to anxiety, shyness, worry, and avoidance of punishment. This dimension is assessed by means of four subscales: Anticipatory worry (11 items), Fear of uncertainty (7 items), Shyness (8 items), and Fatigability (9 items).
3. Reward Dependence (RD): Attachment and social attachment systems. It is associated with dependence on external approval. This dimension encompasses three subscales: Sentimentality (10 items), Attachment (8 items), and Dependence (6 items).
4. Persistence (P): Capacity to maintain behavior in adverse conditions. It is characterized by making demands on self, hard working, striving for excellence. It has a single 8-item scale.
The Character scales are:
1. Self-directedness: Related to maturity, strength and selfsufficiency. Capacity to manage behavior guided by goals chosen voluntarily and individually and not by circumstances, impulses or external stimulus. This dimension is assessed as the sum of five subscales measuring more specific related traits: Responsibility (8 items), Purposefulness (8 items), Resourcefulness (5 items), Self-acceptance (11 items), and Congruent second nature (12 items).
2. Cooperativeness (C): Reveals an inclination towards social tolerance, empathy, friendliness, altruism, and respect for others. This dimension includes: Social acceptance (8 items), Empathy (7 items), Helpfulness (8 items), Compassion (10 items), and Pure-heartedness (9 items).
3. Self-Transcendence (ST): Reflects a tendency towards spirituality, idealism, religious or mystical feelings, and identification with the wider world, as well as the ability to accept ambiguity and uncertainty, and a sense of communion with others. This dimension encompasses three subscales: selfforgetfulness (11 items), transpersonal identification (9 items), and spiritual acceptance (13 items).
The Barratt Impulsiveness Scale (BIS-11): It is a self-report scale composed of 30 items with Likert-type questions which provide a total score of impulsivity and three sub-scores: attention, lack of planning and motor impulsivity. Scores vary from 30 to 120 and there is no established cut-off point [31,32].
Procedure
Each participant was enrolled in an individual and manualized treatment program based on Marlatt and Gordon [33] relapse prevention. This treatment was cognitive behavioral and psycho-educational in nature and was conducted by two doctors intensively trained in managing individuals with addiction. Patients attended Cognitive Behavioral Therapy (CBT) once a week for 12 weeks. The overall goal of these interventions was to increase the person’s ability to cope with high-risk situations that could precipitate relapses. During the sessions, the patients were recommended monitoring good and bad daily situations during all treatment and this was discussed with their doctors and, when possible, related to the addictive behavior. The following topics were standardized and applied to each patient during this treatment: management of negative mood, assertiveness, drug refusal skills, enhancement of social support networks, and relapse prevention.
In the present study, the main objective was to evaluate the role of two clusters of cocaine dependents on treatment retention. For the purposes of this study, a client was considered retained in treatment if he persisted to treatment completion. Treatment retention was then evaluated in two ways. Firstly, the patients who remained in the treatment during all 12 weeks were considered completers and the patients who did not attend follow-up were considered to have dropped out of the study. Secondly, we computed the number of weeks patients remained in treatment and treated this period as a continuous variable. The period of 12 weeks was used because this is the standard length of CBT treatment [34].
Analyses
Classes of participants sharing common psychosocial features, cocaine use-related aspects, and impulsiveness were identified with Latent Class Analysis (LCA). LCA is a statistical method which yields a probabilistic clustering approach, and is commonly used for identifying unobserved class memberships based on the information from a set of observed discrete variables that imperfectly measure the true class membership. Latent variable modeling does not rely on common assumptions that are easily violated, such as normality and linearity. Moreover, latent class models rely on person-based or case probabilities as opposed to distance or ad hoc probabilities to form maximum likelihood derived classes and subsequent goodness-of-fit indices. Similar to cluster analysis, however, final class solutions depend entirely on variables that are originally entered into the analysis. Specifically, rather than testing a previously specified, a priori solution, we examined the fit of a series of different LCA models. First, a single group was examined; then, additional groups were added to the model until no significant empirical and conceptual improvements were observed. The model’s empirical fit was based on the Bayesian Information Criterion [35], with lower values reflecting an improved fit. In addition, entropy was examined, which shows how well the indicators predict subgroup membership, with values of 0.70 or higher indicating good classification accuracy. The indicators entered into LCA were: BIS-11 mean levels, years since cocaine use started, family history of cocaine use problems, history of previous treatment for cocaine use problems, and educational level. The analyses were carried out in an exploratory fashion using Latent Gold 4.5.
Differences among cluster memberships as to continuous variables were determined using parametric or non-parametric tests, according to Levene’s criteria. Categorical variables were compared by using the χ2 test or Fisher’s exact test, following Monte Carlo method. The outcome measure-“time from the beginning of the treatment program until the withdrawal from it”-was analyzed by Kaplan-Meier survival analysis (log-rank test). Subsequently, bivariate analyses were conducted to verify associations between each independent variable and treatment retention. Lastly, a multiple logistic regression was used to predict treatment retention, using simultaneous forced entry. Only the independent variables with significance levels below 0.10 in bivariate analyses were retained in this model [36]. Statistical analyses were performed with the SPSS version 20.0 for the personal computer. For all statistical tests done, differences between groups were accepted as significant if they achieved the 0.05 level with 2-tailed tests.
Results
Descriptive statistics
The mean age of our total sample was 29.89 (SD=7.16) years, 65% were single or divorced, 56% were white, and 40% had not reached the 12th grade. The mean age of onset of cocaine use was 18.32 (SD=4.56) years, and the mean duration of cocaine use was 9.53 (SD=6.14) years. Sixty-four patients were smokers. Forty-four subjects were powder cocaine users, 23 patients reported using cocaine by smoking route of administration (crack), and 33 were dual users. No subjects reported using cocaine by intravenous route of administration.
Analysis of typology
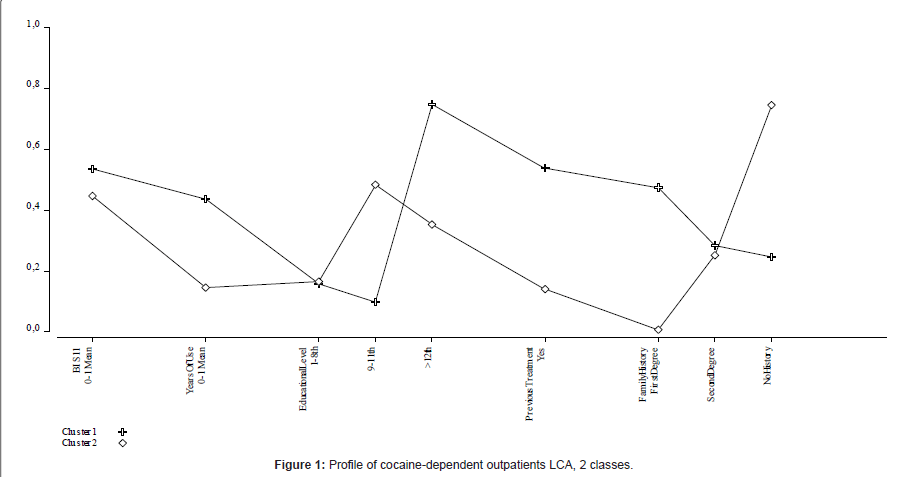
A total of five LCA models were examined, ranging from one to five classes. As shown in Table 1, the 2-class model was determined to be the best-fit model for the data as it had the lowest BIC (Bayesian Information Criterion) and AIC (Akaike Information Criterion), and the highest entropy value amongst the remaining four models. Thus, the two-class solution was retained in subsequent analyses. Participants belonging to Cluster 1 (n=60) were characterized by higher impulsiveness level, more years of cocaine use, higher educational level, more previous treatment episodes for cocaine addiction, and more frequent family history of cocaine use problems than Cluster 2 (n=40) (Figure 1). As shown in Table 2, the differences between these variables were statistically significant between both clusters.
| No of classes | LL | BIC (LL) | AIC (LL) | Class error | Entropy |
|---|---|---|---|---|---|
| 1 2 3 4 5 |
-962.87 -927.38 -917.87 -907.95 -899.70 |
1967.18 1941.95 1969.30 1995.50 2025.05 |
1943.74 1892.45 1893.75 1893.89 1897.39 |
0.000 0.063 0.062 0.107 0.145 |
1 0.80 0.79 0.80 0.77 |
Table 1: Fit indices for latent classes.
Characteristics of two clusters of cocaine dependents
As shown in Table 3, there were no significant differences between both clusters in terms of marital status, race, monthly income, history of living with other cocaine/crack users, involvement with criminal justice, number of sexual partners, alcohol use, smoking status, cannabis use, the ASI-6 subscales, and the following cravingrelated aspects: intensity, frequency, and duration. However, Cluster 1 persons consumed a larger quantity of cocaine and spent more money on crack/cocaine in the last 30 days, and were older than Cluster 2 individuals. As regards personality dimensional characteristics, cluster 1 subjects showed higher self-transcendence than their counterparts (Table 4).
| Variables | Cluster 1 (n=60) |
Cluster 2 (n=40) |
Test | p |
|---|---|---|---|---|
| BIS-11, mean (SD) | 71.23 (11.76) | 67.07 (5.60) | t=2.08, 98 df | 0.04* |
| Years of cocaine use, mean (SD) | 12.68 (5.79) | 4.80 (2.59) | t=8.08, 98 df | <0.01** |
| Educational Level, n (%) 1-8th 9-11th ≥ 12th |
10 (16.67) 5 (8.33) 45 (75) |
6 (15) 19 (47.50) 15 (37.50) |
χ2=21.01, 2 df | <0.01** |
| Previous treatment for cocaine addiction, n (%) |
33 (55) | 6 (15) | χ2=16.14, 1 df | <0.01** |
| Family history of cocaine dependence, n (%) First-degree parents Second degree parents None |
30 (50) 18 (30) 12 (20) |
0 9 (22.5) 31 (77.5) |
χ2=45.28, 2 df | <0.01** |
BIS: Barratt Impulsiveness Scale
*: p<0.05
**: p<0.01.
Table 2: Division of subjects into two clusters (LCA, 2 classes).
| Variables | Cluster 1 (n=60) |
Cluster 2 (n=40) |
Test | p |
|---|---|---|---|---|
| Age, mean (SD) | 32.40 (6.49) | 26.62 (6.86) | t=3.99, 98 df | <0.01** |
| Marital status, n (%) Married Single Separated / Widowed |
24 (40) 30 (50) 6 (10) |
11 (27.50) 25 (72.50) 4 (10) |
χ2=1.78, 2 df |
0.46 |
| Race, n (%) White Non-white |
37 (61.67) 23 (38.33) |
19 (47.50) 21 (52.50) |
χ2=1.96, 1 df |
0.16 |
| Money spent on crack/cocaine use in the past 30 days (in R$, the Brazilian currency), mean (SD) | 480 (526.45) | 261.75 (272.67) | t=2.41, 98 df | 0.02* |
| Monthly income (in R$), mean (SD) | 1326.33 (1334.84) | 950.75 (1052.46) | t=1.50, 98 df | 0.14 |
| Number of days cocaine used in the last 30, mean (SD) | 10.65 (8.76) | 8.80 (7.99) | t=1.07, 98 df | 0.29 |
| Days of cocaine used per week, mean (SD) |
2.38 (1.70) | 2.37 (1.83) | t=0.02, 98 df | 0.98 |
| Grams of cocaine used in the last 30 days, mean (SD) | 20.60 (26.29) | 7.66 (7.72) | t=3.02, 98 df | < 0.01** |
| Age of first cocaine use, mean (SD) | 19.72 (5.36) | 21.82 (6.51) | t=-1.77, 98 df | 0.08 |
| Route of administration, n (%) Intranasal Freebase Both |
21 (35) 17 (28.33) 22 (36.67) |
23 (57.50) 6 (15) 11 (27.50) |
χ2=5.23, 2 df |
0.08 |
| Live with other crack/cocaine users, n (%) | 9 (15) | 4 (10) | χ2=0.58, 1 df | 0.55 |
| Involvement with criminal justice, n (%) | 18 (30) | 7 (17.50) | χ2=2.06, 1 df | 0.15 |
| Number of sexual partners in the last 6 months, mean (SD) | 3.77 (6.95) | 1.95 (1.95) | t=1.61, 98 df | 0.11 |
| Alcohol use, n (%) < 50 units/week ≥ 50 units/week |
43 (71.67) 17 (28.33) |
28 (70) 12 (30) |
χ2=0.03, 1 df |
0.86 |
| Number of days alcohol used in the last 30, mean (SD) | 13.18 (12.70) | 13.47 (12.62) | t=-0.11, 98 df | 0.91 |
| Years of regular alcohol use, mean (SD) |
5.75 (3.17) | 4.92 (2.25) | t=1.42, 98 df | 0.16 |
| Smoking status, n (%) yes no |
36 (60) 24 (40) |
28 (70) 12 (30) |
χ2=1.04, 1df |
0.31 |
| Cannabis users, n (%) | 56 (93.33) | 32 (80) | χ2=4.04, 1df | 0.06 |
| Years of regular cannabis use, mean (SD)a |
4.29 (5.32) | 2.87 (3.74) | t=1.32, 86 df | 0.19 |
| Crack/cocaine craving intensity during the past week b, mean (SD) | 5.93 (2.61) | 5.60 (2.70) | t=0.62, 98 df | 0.54 |
| Crack/cocaine craving frequency during the past week b, n (%) Less than 3 times/day More than 3 times/day |
37 (61.67) 23 (38.33) |
21 (52.50) 19 (47.50) |
χ2=0.83, 1 df |
0.36 |
| Crack/cocaine craving duration during the last week b, n (%) Less than 10 minutes More than 10 minutes |
28 (46.67) 32 (53.33) |
19 (47.50) 21 (52.50) |
χ2=0.01, 1 df |
0.93 |
| ASI subscales, mean (SD) Drug Family/Child Alcohol Psychiatric Medical Legal Employment Family/Social Support Family/Social Problem |
55.95 (12.46) 69.87 (1.50) 46.88 (12.29) 50.30 (9.03) 49.03 (7.37) 56.68 (8.60) 51.07 (6.54) 53.53 (21.90) 64.33 (13.57) |
58.82 (11.32) 69.32 (2.44) 49.95 (11.25) 48.87 (8.61) 50.25 (6.56) 55.15 (7.55) 50.62 (6.34) 58.75 (19.88) 64.02 (14.18) |
t=-1.17, 98 df t=1.37, 98 df t=-1.26, 98 df t=0.79, 98 df t=-0.84, 98 df t=0.92, 98 df t=0.33, 98 df t=-1.21, 98 df t=0.11, 98 df |
0.24 0.17 0.21 0.43 0.40 0.36 0.74 0.23 0.91 |
*: p<0.05
a computed only for those that admitted to using cannabis
b measured by the MCCS (Minnesota Cocaine Craving Scale).
Table 3: Baseline characteristics.
Survival analysis
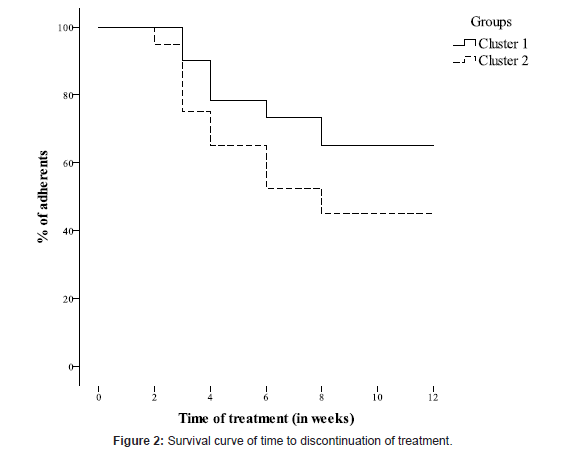
As shown in Figure 2, cluster 1 subjects remained longer in the therapeutic program than their counterparts (χ2=4.67, 1 df, p=0.03, logrank test). The mean time to treatment discontinuation was significantly different between both groups (t=2.18, 98 df, p=0.03), with Cluster 1 subjects showing 9.53 (SD=3.58) weeks of adherence as against 7.85 (SD=4.06) weeks in Cluster 2. This difference remained significant even after controlling for marital status (χ2=4.93, 1 df, p=0.03, stratified longrank test). Overall, 39 (65%) subjects in cluster 1 and 18 (45%) subjects in cluster 2 completed the treatment program, and this difference was also significant (χ2=3.02, 1 df, p=0.048).
| Variables | Cluster 1 (n=60) | Cluster 2 (n=40) | Test | p |
|---|---|---|---|---|
| NS, mean (SD) | 51.02 (9.97) | 48.47 (9.97) | t=1.26, 98 df | 0.21 |
| HA, mean (SD) | 50.11 (10.97) | 49.83 (8.47) | t=0.14, 98 df | 0.89 |
| RD, mean (SD) | 51.29 (9.71) | 48.06 (10.23) | t=1.59, 98 df | 0.11 |
| P, mean (SD) | 50.29 (11.06) | 49.56 (8.27) | t=0.36, 98 df | 0.72 |
| SD, mean (SD) | 48.88 (10.94) | 51.68 (8.69) | t=-1.38, 98 df | 0.17 |
| C, mean (SD) | 48.84 (10.70) | 51.73 (8.69) | t=-1.42, 98 df | 0.16 |
| ST, mean (SD) | 51.81 (9.93) | 47.29 (9.59) | t=2.26, 98 df | 0.02* |
*: p<0.05
NS=Novelty Seeking; HA=Harm Avoidance; RD=Reward Dependence; P=Persistence; SD=Self-directedness; C=Cooperativeness; ST=Self-transcendence.
Table 4: Temperament and character dimensions (T score) between both clusters.
Associations between treatment retention and independent variables
Binary and multivariate logistic regressions were performed. On bivariate analysis shown in Table 5, the following variables were associated with significantly increased odds of treatment retention: having higher educational level (≥ 12th grade), and showing higher mean scores on the employment ASI subscale. A multivariate adjustment confirmed the data that having a higher educational level and showing higher scores on the employment ASI subscale increased the odds of treatment retention (Table 6). In this multivariate analysis, the model was statistically significant (χ2 (5)=15.82, p < 0.01), with a low group membership variance (R2=0.20), and an overall predictability of 67%. We also checked model fit by using Hosmer and Lemeshow test (χ2(8)=9.96, p=0.27).
Discussion
When dividing our subjects into two typological groups it has been found that cluster 1 persons showed higher educational level, more frequent family history of cocaine use problems, higher impulsiveness level, more years of cocaine use, and more previous treatment episodes for cocaine addiction than Cluster 2 persons. In addition, cluster 1 persons were older, spent more money on cocaine use, consumed a larger quantity of cocaine in the last 30 days, and demonstrated higher self-transcendence level than cluster 2. Furthermore, cluster 1 persons adhered longer to the treatment. Considering some classifications of cocaine dependents to date, our clusters seem to be similar to those proposed by Ball et al. [17]. When independent variables were entered in a direct logistic regression model, only a higher educational level and higher scores on the employment ASI subscale were significantly related to treatment retention.
It is important to note that our sample is relatively “benign”, given that no subjects had other serious psychiatric problems such as other drug dependence and severe psychiatric comorbidity. This may be confirmed by the fact that all subjects were candidates to outpatient treatment and did not receive any medications. Each predictive factor that was included in our LCA was already tested in previous studies. Number of years since the client initiated cocaine use; problems stemming from cocaine use [13], and higher educational level [37] were already seen to be positively associated with treatment completion. Conversely, more previous treatment episodes [11], parental substance abuse [17], and higher impulsiveness level [14] have been already associated with early discontinuation of treatment. Nevertheless, these findings are mixed among different studies, probably due to heterogeneity of samples and lack of a theoretical model that encompasses different variables.
Some variables that have been tested separately in diverse studies can be intrinsically correlated with others. Studies have shown that the duration of cocaine abuse is positively correlated with some behavioral aspects, such as impulsivity and compulsivity. In fact, the longer cocaine users have been using this drug, the greater the loss of grey matter. Hence, these chronic users may show high attentional impairment and impulsivity [38]. High levels of impulsivity are shown to be associated with poor treatment outcomes and high dropout rates among substance abusers [6,7]. Our study did not support this finding. Although Cluster 1 persons demonstrated higher impulsiveness levels, they adhered longer to our 12-week treatment program than their counterparts. It is possible to suppose that impulsive individuals more readily engage in new activities and challenges, mainly during early phases of a treatment or even in short therapeutic programs [39]. As our treatment program was relatively short, this statement can be true to some extent. In addition, other studies suggest that cocaine dependents entering treatment with higher impulsiveness and less impaired decisionmaking abilities may respond favorably to behavioral interventions [14]. It is generally presumed that long-term cocaine use, heavy drug consumption, and problems stemming from this use decrease treatment retention; however, it can be expected that those with more severe drug-related problems may have a stronger motivation to seek help and to complete treatment.
| Variables | SE | Wald | df | p | OR | CI (95%) |
|---|---|---|---|---|---|---|
| Age | 0.03 | 0.04 | 1 | 0.84 | 0.99 | 0.94-1.05 |
| Marital status | ||||||
| Married Single Separated/Widowed (reference) |
0.72 0.69 |
0.16 0.23 |
1 1 |
0.69 0.63 |
1.33 1.39 |
0.33-5.46 0.36-5.37 |
| Race | ||||||
| White Non-white (reference) |
0.41 | 2.73 | 1 | 0.10 | 1.97 | 0.88-4.41 |
| Educational level | ||||||
| 1-8th 9-11th ≥ 12th (reference) |
0.64 0.50 |
6.68 0.01 |
1 1 |
0.01* 0.94 |
0.19 0.94 |
0.06-0.67 0.36-2.57 |
| Money spent on crack/cocaine use in the past 30 days | <0.01 | 0.01 | 1 | 0.93 | >0.99 | 0.99-1.01 |
| Monthly income | <0.01 | 1.32 | 1 | 0.25 | >0.99 | 0.99-1.01 |
| Number of days cocaine used in the last 30 | 0.02 | 0.19 | 1 | 0.66 | 1.01 | 0.96-1.06 |
| Days of cocaine used per week | 0.12 | 0.38 | 1 | 0.53 | 1.07 | 0.86-1.35 |
| Grams of cocaine used in the last 30 days | 0.01 | 0.64 | 1 | 0.42 | 1.01 | 0.99-1.03 |
| Age of first cocaine use | 0.03 | 1.25 | 1 | 0.26 | 0.96 | 0.90-1.03 |
| Years of cocaine use | 0.03 | 0.72 | 1 | 0.40 | 1.03 | 0.96-1.10 |
| Route of administration | ||||||
| Intranasal Freebase (reference) Both |
0.46 0.59 |
0.73 1.55 |
1 1 |
0.39 0.21 |
0.67 2.09 |
0.27-1.67 0.66-6.65 |
| Previous treatment for cocaine addiction | 0.42 | 0.10 | 1 | 0.75 | 1.14 | 0.51-2.58 |
| Live with other crack/cocaine users | 0.61 | 0.15 | 1 | 0.70 | 1.27 | 0.38-4.19 |
| Family history of cocaine dependence First-degree parents |
0.48 | 0.88 | 1 | 0.35 | 1.57 | 0.61-4.04 |
| Second degree parents None (reference) |
0.51 | 2.11 | 1 | 0.15 | 2.10 | 0.77-5.69 |
| Involvement with criminal justice | 0.46 | 0.34 | 1 | 0.56 | 0.76 | 0.31-1.89 |
| Number of sexual partners in the last 6 months | 0.05 | 0.98 | 1 | 0.32 | 0.96 | 0.87-1.05 |
| Alcohol use <50 units/week ≥ 50 units/week (reference) |
0.44 |
0.46 |
1 |
0.50 |
1.35 |
0.57-3.22 |
| Number of days alcohol used in the last 30 | 0.02 | 1.32 | 1 | 0.25 | 0.98 | 0.95-1.01 |
| Years of regular alcohol use | 0.05 | 0.03 | 1 | 0.85 | 1.01 | 0.91-1.12 |
| Cigarette smokers | 0.42 | 0.39 | 1 | 0.53 | 0.77 | 0.33-1.76 |
| Cannabis smokers | 0.65 | 2.91 | 1 | 0.09 | 3.01 | 0.85-10.83 |
| Years of regular cannabis usea | 0.04 | <0.01 | 1 | 0.96 | 0.96 | 0.92-1.09 |
| Crack/cocaine craving intensity during the past week b | 0.08 | <0.01 | 1 | 0.96 | 0.99 | 0.86-1.16 |
| Crack/cocaine craving frequency during the past week b | ||||||
| Less than 3 times/day More than 3 times/day (reference) |
0.411 | 0.19 | 1 | 0.66 | 0.84 | 0.37-1.88 |
| Crack/cocaine craving duration during the last weekb | ||||||
| Less than 10 minutes More than 10 minutes (reference) |
0.41 | 0.80 | 1 | 0.37 | 1.44 | 0.65-3.19 |
| ASI subscales | ||||||
| Drug | 0.02 | <0.01 | 1 | 0.95 | 0.99 | 0.97-1.03 |
| Family/Child | 0.12 | 2.33 | 1 | 0.13 | 1.19 | 0.95-1.50 |
| Alcohol | 0.02 | 0.02 | 1 | 0.91 | 1.01 | 0.97-1.04 |
| Psychiatric | 0.02 | 0.12 | 1 | 0.72 | 1.01 | 0.96-1.05 |
| Medical | 0.03 | 0.03 | 1 | 0.86 | 1.01 | 0.95-1.06 |
| Legal | 0.02 | 0.04 | 1 | 0.84 | 0.98 | 0.95-1.04 |
| Employment | 0.03 | 4.75 | 1 | 0.03* | 1.08 | 1.01-1.15 |
| Family/Social Support | 0.01 | <0.01 | 1 | 0.98 | > 0.99 | 0.98-1.02 |
| Family/Social Problem | 0.02 | <0.01 | 1 | 0.95 | 1.01 | 0.97-1.03 |
| TCI subscales | ||||||
| NS | 0.06 | 0.13 | 1 | 0.72 | 0.98 | 0.88-1.09 |
| HA | 0.04 | 0.46 | 1 | 0.50 | 0.97 | 0.89-1.06 |
| RD | 0.06 | 0.01 | 1 | 0.91 | 0.99 | 0.88-1.12 |
| P | 0.13 | 0.98 | 1 | 0.32 | 0.88 | 0.68-1.13 |
| SD | 0.03 | 0.20 | 1 | 0.65 | 0.99 | 0.93-1.05 |
| C | 0.03 | 0.84 | 1 | 0.36 | 0.97 | 0.91-1.03 |
| ST | 0.03 | 0.04 | 1 | 0.83 | 1.01 | 0.94-1.08 |
| BIS | 0.02 | 1.97 | 1 | 0.16 | 1.03 | 0.99-1.07 |
* p < 0.05; ** p < 0.01
aComputed only for those that admitted to using cannabis
bMeasured by the MCCS (Minnesota Cocaine Craving Scale)
NS: Novelty Seeking; HA: Harm Avoidance; RD: Reward Dependence;
P: Persistence; SD: Self-Directedness; C: Cooperativeness; ST: Self-
Transcendence; BIS: Barratt Impulsiveness Scale.
Table 5: Bivariate analysis of sociodemographic, clinical, and psychological factors associated with treatment retention.
| Variables | S.E. | Wald | df | p | OR | CI (95%) |
|---|---|---|---|---|---|---|
| Race White Non-white (reference) |
0.46 |
0.93 |
1 |
0.34 |
1.55 |
0.63-3.78 |
| Educational level 1-8th 9-11th ≥12th (reference) |
0.68 0.54 |
5.13 0.01 |
1 1 |
0.02* 0.91 |
0.21 0.94 |
0.06-0.81 0.33-2.70 |
| Cannabis smokers | 0.71 | 1.27 | 1 | 0.26 | 2.22 | 0.56-8.88 |
| ASI subscale Employment |
0.04 |
4.95 |
1 |
0.03* |
1.08 |
1.01-1.16 |
*: p<0.05.
Table 6: Multivariable analysis of factors associated with treatment retention (Direct Logistic Regression Analysis).
Impulsiveness is a vulnerability factor for substance dependence. However, when impulsiveness is measured by self-report questionnaires, its meaning can be unclear, given the influence of subjects’ insight and view of self. In addition, impulsiveness is a multifaceted construct, and self-report assessments may represent different levels of analyses, from detailing specific behavioral processes to more general personality characteristics. Higher scores on the employment ASI subscale were associated with treatment retention in our study. Some studies have shown that patients with high need for employment counseling can remain in treatment longer than patients with low employment needs [40]. In fact, unemployed patients may experience lower difficulty attending treatment sessions than employed ones. In addition, some subjects may be identifying the treatment as a way to improve their social condition and reinsertion. However, there are mixed results about the relationship of treatment retention and employment status [9,11].
Cluster 1 persons showed higher scores on self-transcendence. This character trait can be seen as a developmental process that forms a pathway to wisdom. It is correlated with hope, emotional well-being, and a sense of coherence in both healthy and people with serious illnesses [41]. Some theories of self-transcendence show the relationship between the concept of vulnerability and self-transcendence, such that increased levels of vulnerability influence increased levels of selftranscendence. From a developmental perspective, it is considered that “life events that heighten one’s sense of mortality, inadequacy, or vulnerability can trigger developmental process toward a renewed sense of identity and expanded self-boundaries” [42]. Although selftranscendence may be a factor underlying certain aspects of Cluster 1 persons, such as impulsiveness [43], this character trait was not related to treatment retention when it was analyzed separately.
Cocaine dependence is a multi-factorial disorder involving biological, genetic, and psychosocial interactions. Hence, multiple variables can be necessary to classify this extremely complex population. Despite the heterogeneity of our clients, many therapeutic programs offer only a single type of treatment. With this “one size fits all” model, variations in retention have been commonly attributed to client factors or characteristics. Although this may be true to some extent, health services should broaden the scope of services offered to meet heterogeneous needs of clients, and identify treatment practices and therapists which improve retention. Information about patients’ characteristics linked to noncompliance or dropout should be used to make treatment programs more responsive and attractive, combining more intensive and diversified psychosocial interventions.
Probably the continuous development of typologies will contribute to determine what type of treatment is more suitable for certain types of patients. If patients’ data obtained at the beginning of treatment are useful for designing a more adequate management, health professionals will pay higher attention to this task. On the basis of this information it is possible to identify the population whose treatment should receive the most attention and investment [44]. Future efforts should be made to study how the commitment to the treatment of both clusters could be improved. Currently, there is no medication that has been shown to be broadly effective for retaining cocaine dependents in treatment, nor in reducing cocaine use. Despite this, it is possible that available treatments can be more effective in some subgroups of patients. Thus, a fruitful strategy may be the identification of characteristics linked to differential response to specific treatments.
Some limitations of this study must be cited:
• Only cocaine users who agreed to participate in this study were included. Hence, it is not clear whether these findings would apply to individuals who would refuse to participate in clinical studies or fail to meet inclusion criteria;
• There were no other psychotherapeutic procedures or incentives along with CBT, which could increase the retention of the patients;
• Our research did not include women. Some studies have shown that gender difference exerts different roles in treatment retention and craving [40,45];
• Since a post-treatment follow-up was not administered, we may not affirm that more impulsive individuals will maintain higher retention rates.
Acknowledgements
We wish to thank CNPQ (Conselho Nacional de Desenvolvimento Científico e Tecnológico-National Counsel of Technological and Scientific Development).
References
- United Nations Office on Drugs and Crime (2012) World Drug Report. United Nations publication, Vienna.
- Stotts AL, Mooney ME, Sayre SL, Novy M, Schmitz JM, et al. (2007) Illusory predictors: Generalizability of findings in cocaine treatment retention research. Addict Behav 32: 2819-2836.
- Cleck JN, Blendy JA (2008) Making a bad thing worse: adverse effects of stress on drug addiction. J Clin Invest 118: 454-461.
- Grant S, London ED, Newlin DB, Villemagne VL, Liu X, et al. (1996) Activation of memory circuits during cue-elicited cocaine craving. Proc Natl Acad Sci USA 93: 12040-12045.
- Turner TH, LaRowe S, Horner MD, Herron J, Malcolm R (2009) Measures of cognitive functioning as predictors of treatment outcome for cocaine dependence. J Subst Abuse Treat 37: 328-334.
- Moeller FG, Dougherty DM, Barratt ES, Schmitz JM, Swann AC, et al. (2001) The impact of impulsivity on cocaine use and retention in treatment. J Subst Abuse Treat 21: 193-198.
- Patkar AA, Murray HW, Mannelli P, Gottheil E, Weinstein SP, et al. (2004) Pre-treatment measures of impulsivity, aggression and sensation seeking are associated with treatment outcome for African-American cocaine-dependent patients. J Addict Dis 23: 109-122.
- Verdejo-Garcia A, Betanzos-Espinosa P, Lozano OM, Vergara-Moragues E, Gonzalez-Saiz F, et al. (2012) Self-regulation and treatment retention in cocaine dependent individuals: a longitudinal study. Drug Alcohol Depend 122: 142-148.
- Claus RE, Kindleberger LR, Dugan MC (2002) Predictors of attrition in a longitudinal study of substance abusers. J Psychoactive Drugs 34: 69-74.
- Siqueland L, Crits-Christoph P, Gallop R, Barber JP, Griffin ML, et al. (2002) Retention in psychosocial treatment of cocaine dependence: predictors and impact on outcome. Am J Addict 11: 24-40.
- King AC, Canada SA (2004) Client-related predictors of early treatment drop-out in a substance abuse clinic exclusively employing individual therapy. J Subst Abuse Treat 26: 189-195.
- Hoffman JA, Caudill BD, Koman JJ, Luckey JW, Flynn PM, et al. (1994) Comparative cocaine abuse treatment strategies: Enhancing client retention and treatment exposure. J Addict Dis 13: 115-128.
- Gainey RR, Wells EA, Hawkins JD, Catalano RF (1993) Predicting treatment retention among cocaine users. Int J Addict 28: 487-505.
- Schmitz JM, Mooney ME, Green CE, Lane SD, Steinberg JL, et al. (2009) Baseline neurocognitive profiles differentiate abstainers and non-abstainers in a cocaine clinical trial. J Addict Dis 28: 250-257.
- Moss PD, Werner PD (1992) An MMPI typology of cocaine abusers. J Pers Assess 58: 269-276.
- Johnson WA, Sterk CE (2003) Late-onset crack users: an emergent HIV risk group. J Acquir Immune Defic Syndr 33: S229-S232.
- Ball SA, Carrol KM, Babor TF, Rounsaville BJ (1995) Subtypes of cocaine abusers: Support for a type A - type B distinction. J Consult Clin Psychol 63: 115-124.
- Feingold A, Ball SA, Kranzler HR, Rounsaville BJ (1996) Generalizability of the type A/type B distinction across different psychoactive substances. Am J Drug Alcohol Abuse 22: 449-462.
- McLellan AT, Chalk M, Bartlett J (2007) Outcomes, performance, and quality: What's the difference? J Subst Abuse Treat 32: 331-340.
- Siegal HA, Li L, Rapp RC (2002) Abstinence trajectories among treated crack cocaine users. Addict Behav 27: 437-449.
- Beynon CM, McMinn AM, Marr AJ (2008) Factors predicting drop out from, and retention in, specialist drug treatment services: A case control study in the North West of England. BMC Public Health 8: 149.
- Amorim P (2000) Mini International Neuropsychiatric Interview (MINI): Validation of a short structured diagnostic psychiatric interview. Rev Bras Psiquiatr 22: 106-115.
- Pettinati HM, Kampman KM, Lynch KG, Suh JJ, Dackis CA, et al. (2008) Gender differences with high-dose naltrexone in patients with co-occurring cocaine and alcohol dependence. J Subst Abuse Treat 34: 378-390.
- Sobell LC, Maisto SA, Sobell MB, Cooper AM (1979) Reliability of alcohol abusers' self-reports of drinking behavior. Behav Res Ther 17: 157-160.
- Cacciola JS, Alterman AI, Habing B, McLellan AT (2011) Recent status scores for version 6 of the Addiction Severity Index (ASI-6). Addiction 106: 1588-1602.
- Kessler F, Cacciola J, Alterman A, Faller S, Souza-Formigoni ML, et al. (2012) Psychometric properties of the sixth version of the Addiction Severity Index (ASI-6) in Brazil. Rev Bras Psiquiatr 34: 24-33.
- Focchi GR, Leite MC, Andrade AG, Scivoletto S (2005) Use of dopamine agonist pergolide in outpatient treatment of cocaine dependence. Subst Use Misuse 40: 1169-1177.
- Cloninger CR, Svrakic DM, Przybeck TR (1993) A psychobiological model of temperament and character. Arch Gen Psychiatry 50: 975-990.
- Fuentes D, Tavares H, Camargo CHP, Gorenstein C (2000) Inventário de Temperamento e de Caráter de Cloninger: Validação da versão em Português. In: Gorenstein C, Andrade LHSG, Zuardi AW (Eds.) Escalas de Avaliação Clínica em Psiquiatria e Psicofarmacologia. São Paulo: Lemos. pp. 363-376.
- Arnau MM, Mondon S, Santacreu JJ (2008) Using the temperament and character inventory (TCI) to predict outcome after inpatient detoxification during 100 days of outpatient treatment. Alcohol Alcohol 43: 583-588.
- Patton JH, Stanford MS, Barratt ES (1995) Factor structure of the Barratt impulsiveness scale. J Clin Psychol 51: 768-774.
- Von Diemen L, Szobot CM, Kessler F, Pechansky F (2007) Adaptation and construct validation of the Barratt Impulsiveness Scale (BIS 11) to Brazilian Portuguese for use in adolescents. Rev Bras Psiquiatr 29: 153-156.
- Marlatt GA, Gordon JR (1993) Relapse Prevention: Maintenance Strategies in the Treatment of Addictive Behaviors.
- Aharonovich E, Hasin DS, Brooks AC, Liu X, Bisaga A, et al. (2006) Cognitive deficits predict low treatment retention in cocaine dependent patients. Drug Alcohol Depend 81: 313-322.
- Nylund KL, Asparouhov T, Muthén BO (2007) Deciding on the number of classes in latent class analysis and growth mixture modeling: a Monte Carlo simulation study. Structural Equation Modeling 14: 535-569.
- Hosmer DW, Lemeshow S (1989) Applied logistic regression. (2nd Edn.), Wiley Series in Probability and statistics, New York.
- Means LB, Small M, Capone DM, Capone TJ, Condren R, et al. (1989) Client demographics and outcome in outpatient cocaine treatment. Int J Addict 24: 765-783.
- Ersche KD, Barnes A, Jones PS, Morein-Zamir S, Robbins TW, et al. (2011) Abnormal structure of frontostriatal brain systems is associated with aspects of impulsivity and compulsivity in cocaine dependence. Brain 134: 2013-2024.
- Helmus TC, Downey KK, Arfken CL, Henderson MJ, Schuster CR (2001) Novelty seeking as a predictor of treatment retention for heroin dependent cocaine users. Drug Alcohol Depend 61: 287-295.
- McCaul ME, Svikis DS, Moor RD (2001) Predictors of outpatient treatment retention: Patient versus substance use characteristics. Drug Alcohol Depend 62: 9-17.
- Levenson MR, Jennings PA, Aldwin CM, Shiraishi RW (2005) Self-transcendence: conceptualization and measurement. Int J Aging Hum Dev 60: 127-143.
- Reed PG (2008) The theory of self-transcendence. In: Smith MJ, Liehr PR (Eds.), Middle range theory for nursing. Springer, New York.
- Herrero MJ, Domingo-Salvany A, Torrens M, Brugal MT, Gutierrez F (2008) Personality profile in young current regular users of cocaine. Subst Use Misuse 43: 1378-1394.
- Baltieri DA, Correa Filho JM (2012) Role of two clusters of male alcoholics in treatment retention. Eur Addict Res 18: 201-211.
- Mertens JR, Weisner CM (2000) Predictors of substance abuse treatment retention among women and men in an HMO. Alcohol Clin Exp Res 24: 1525-1533.
Relevant Topics
- Addiction Recovery
- Alcohol Addiction Treatment
- Alcohol Rehabilitation
- Amphetamine Addiction
- Amphetamine-Related Disorders
- Cocaine Addiction
- Cocaine-Related Disorders
- Computer Addiction Research
- Drug Addiction Treatment
- Drug Rehabilitation
- Facts About Alcoholism
- Food Addiction Research
- Heroin Addiction Treatment
- Holistic Addiction Treatment
- Hospital-Addiction Syndrome
- Morphine Addiction
- Munchausen Syndrome
- Neonatal Abstinence Syndrome
- Nutritional Suitability
- Opioid-Related Disorders
- Relapse prevention
- Substance-Related Disorders
Recommended Journals
Article Tools
Article Usage
- Total views: 14626
- [From(publication date):
October-2012 - Nov 09, 2025] - Breakdown by view type
- HTML page views : 9947
- PDF downloads : 4679