Treatment of an Acute Respiratory Failure Child Caused by Special Airway Foreign Body
Received: 06-Aug-2013 / Accepted Date: 13-Sep-2013 / Published Date: 23-Sep-2013 DOI: 10.4172/2161-119X.1000141
Abstract
Objective: To explore the combined treatment and effect because of lime foreign body in airway with inhalantion injury of children.
Methods: One child whose respiratory tract was injured and obstructed by lime was admitted to our hospital, and systematic anti-infection and antishock procedures were performed. Then he received tracheal intubation and mechanical ventilation. The child underwent rigid bronchoscopy and the bronchial casts (lime) were removed under general anaesthesia. Subsequently, fiberoptic bronchoscopy was used again, the remaining lime powder was removed by hair brush, and then bronchoalveolar lavage was performed. The secretion of respiratory tract was retained for bacterial culture and susceptibility test.
Results: The mechanical ventilation was withdrawn on the seventh day after perioperative treatment. The right upper lung which was atelectasis before surgery was improved after surgery. Pulmonary function showed that resistance of main air duct was normal while that of small air duct was elevated.
Conclusion: The key for successful treatment is to remove bronchial casts (lime) as soon as possible. Bronchoalveolar lavage and bronchial scrubbing are also important. The combined perioperative treatment can reduce the operation risk and incidence of post-operative complication.
Keywords: Child, Airway foreign body, Respiratory failure, Treatment
254030Introduction
Respiratory foreign body and subsequent inhalant injury in children is a severe emergent disease in otorhinolaryngology. Inhalation injury (usually referred to as “respiratory tract burn”) is mainly caused by aspiration of hot smog, gas, dust and chemical substances into the respiratory tract. The clinical occurrence of respiratory foreign body and inhalation injury in combination is characterized by multiple complications, intricate treatments and high mortality rate. As a clinically rare combination, its perioperative care is extremely difficult. This report is a summary of successful treatment of a case of lime aspiration into the respiratory tract of a child with concomitant inhalation injury admitted to our hospital on November 5th, 2007.
Data and Methods
Clinical data
General information: A 20 months old male baby was admitted to our hospital at 5:00 a.m. on November 5th, 2007 for cough and dyspnea that had started half a day before the admission. On the day before the admission, the baby had accidentally fallen into a lime pool and climbed out of the pool by himself. His family had noticed the lime residue on his face and had taken him to a local hospital. About 12 hours later, the baby developed symptoms like cough, dyspnea and vomiting with gradual aggravation. Therefore, the baby was transferred to our hospital.
Main clinical manifestations at admission: Red-purple spots and petechia were seen on the head and face. The baby showed confusion, listlessness and extreme shortness of breath and dyspnea with significant inspiratory three-concave sign (T: 39°C, RR: 40 ~ 50 times/min). Sound of breath was rough on both sides and wet rale could be auscultated. Sound of breath was weaker on the right side. Heart rhythm was regular and no murmur was auscultated (HR: 150-170 bpm). Transcutaneous oxygen saturation (SaO2) was about 70% to 80%.
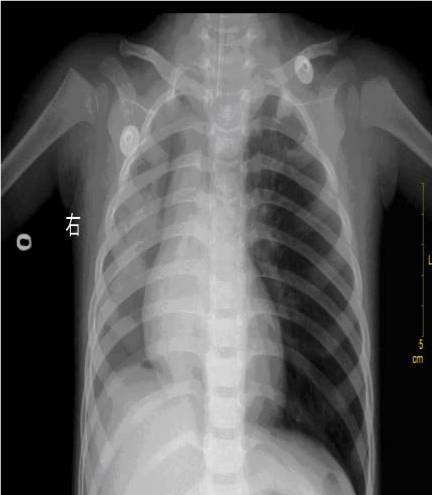
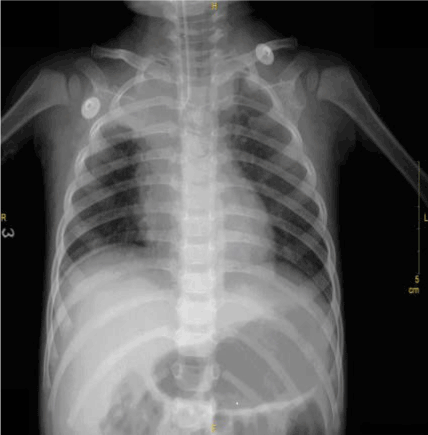
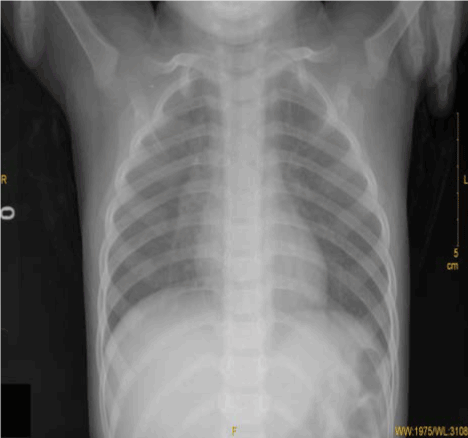
Main auxiliary examinations at admission: Bedside chest posteroanterior radiograph showed aspiration pneumonia in the right lung and atelectasis in right middle-lower lung with minimal pneumothorax in the right lung and minimal gas in the right mediastinum (Figure 1). The Complete blood count showed the following values; WBC 24. 3×109/L, N: 81%, L: 19%. The Blood gas analysis (given oxygen inhalation at 2-4 L/min via nasal catheter) showd PaO2 41 mmHg and PaCO2 32.40 mmHg at pH 7.308.
Methods
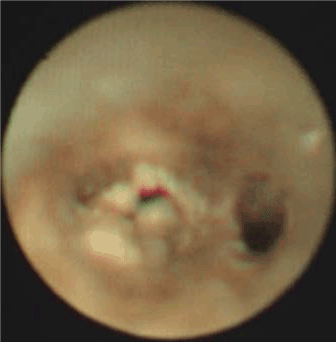
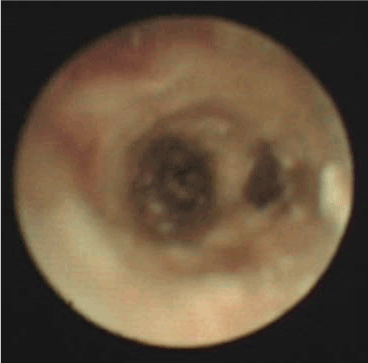
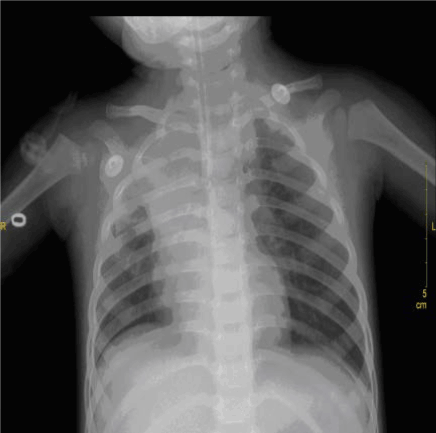
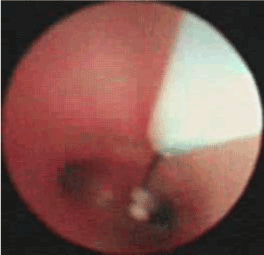
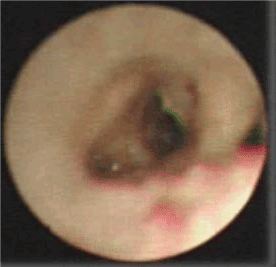
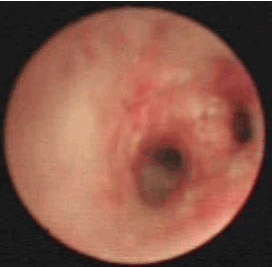
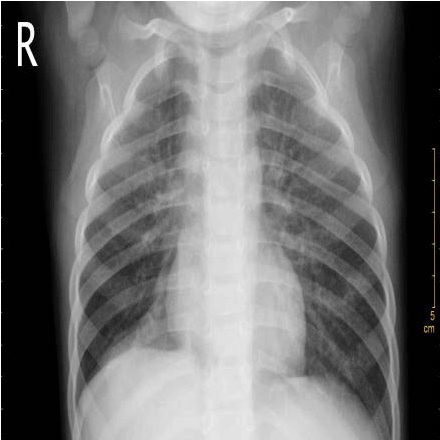
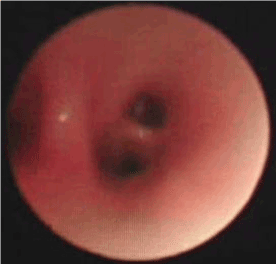
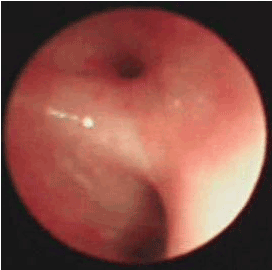
After being admitted, the baby was given a systemic disinfection and anti-shock therapy. An intravenous meprednisone and a bronchial antispasmodic agent aminophylline were also administered. Immediate tracheal intubation was performed and subsequent assisted mechanical ventilation provided. P-CMV mode was used in the assisted ventilation with the following parameters; RR: 40 times/min, peak inspiratory pressure (PIP) 27 cm H2O, Positive End-Expiratory Pressure (PEEP) 6 cm H2O, inspired oxygen concentration (FIO2) 100% and SaO2 around 65%-80%. Repeated blood gas analysis showed a pH value 7.345, PaO2 55mmHg and PaCO2 34.40mmHg. Since, hypoxemia had not significantly improved even after these initial treatments, it was inferred that the right bronchia might have been obstructed by a foreign body, possibly with a concomitant inhalation injury. Hence, on the same day, the baby was sent to the operation room and underwent removal of the foreign body by rigid bronchoscopy and bronchoalveolar lavage by Bronchofibroscopy (BAL) under general anesthesia. A subcutaneous injection of 0.01mg/Kg scopolamine was given to reduce airway secretion and inhibit the vagus nerve 30 minutes before the operation. General anesthesia was induced by intravenous injection of hydroxybutyratepropofol and inhalation of isoflurane via face mask. As an auxiliary procedure, topical anesthesia of laryngeal and tracheal mucosa was induced by 1% dicaine under laryngoscope. In the meantime, the baby was monitored for breath, heart rate, Electrocardiogram (ECG) and blood oxygen saturation. High-flow oxygen was supplied via bronchial side-port. Ultra-thin bronchofibroscope (Olympus BF-XP26, Japan) was used in the surgery. The bronchofibroscope examination started from the point of entry of tracheal intubation. Then, trachea, bronchus and bronchi of each lobe and segment were examined. During the procedure, it was observed that the mucosa of left bronchus and its branches were congested and swollen with considerable amount of viscous white secretion. It was removed thereafter. The bronchi were then lavaged with 37°C 0.9% normal saline. The mucosa of the right bronchus showed significant congestion and erosion with large amount of white lime powder deposits in the bronchi of the right upper, middle and lower lobes. The bronchus was almost completely blocked (Figure 2). The bronchofibroscope was then replaced by a rigid bronchoscope 3.5 STORZ and introduced via laryngoscope. Large amount of lime powder was removed by bronchial clamp. Then, bronchofibroscope was placed back for observation. It was observed that the obstruction in the right bronchus and its branches were mostly cleared. Mucosa was erosive, swollen and slightly ulcerative. In spite of these procedures, considerable quantity of residual lime powder could be observed on the bronchial wall. A Protective brush was used to brush the remaining lime powder and then lavage performed. The lavage solution was 100 mL of 37°C normal saline containing 1:200000 epinephrine (diluted by normal saline), 0.5 g cefoperazone and 5 mg dexamethasone injection. About 5-10 mL lavage solution was injected via the biopsy port of bronchofibroscope each time and was aspirated by negative pressure suction device maintained at 10.6-13.3 Kpa pressure. Lavage was repeated until clear aspirated solution was seen and the bronchi were mostly unobstructed. Finally, 0.25 g of cefoperazone was injected. During the lavage, airway secretion was obtained for bacterial culture and susceptibility test as guidance for drug selection. After the lavage, mucosa of the left bronchus was congested and swollen and no secretion was seen. While in the right upper, middle and lower bronchus mucosa was congested and erosive. The lime powder in this region was cleared and the bronchus partially unobstructed (Figures 3 and 4). The baby was then sent to the Intensive Care Unit (ICU) after the operation. Oxygen saturation was maintained at 95% under mechanical ventilation (RR: 30 times/min; FIO2 90%, PEEP 5 cm H2O, PIP 22 cm H2O). The parameters were modified when applicable. The patient was frequently turned over and patted on the back and was positioned in a way that allowed drainage. Airway irrigation and stronger anti-inflammatory and nutritionally supportive treatments were given. Repeated blood gas analysis showed a pH value 7.501, PaO2 62 mmHg and PaCO2 27.30 mmHg. Chest X-ray examination on November 6th, 2007 suggested pneumonia and concomitant atelectasis in the right lung which were significantly better compared to the previous examination and were now more prominent in right upper lobe (Figure 5). The patient showed improvement with better pulmonary ventilation. Still, there were chances for residual lime powder in smaller bronchi leading to continued obstruction and chemical damage. On November 8th, again the baby underwent bronchoalveolar lavage by bronchofibroscopy under general anesthesia. After the lavage, it was observed that mucosa of the left bronchi was mildly congested and swollen. The pseudo-membrane could be seen adhering to the bronchial mucosa of right middle and lower lobes, while the point of entry of the upper lobe was unobstructed (Figure 6). After operation, the baby was sent to ICU for subsequent monitoring. On November 12th, repeated complete blood count showed WBC 12.2×109/L, N 66% and L 32%. Chest X-ray revealed that atelectasis was better as compared to previous examination and emphysema in the left lung was also cured (Figure 7). Blood gas analysis showed a pH value 7.426, PaO2 96 mmHg and PaCO2 35.0 mmHg. The baby was conscious and autonomous respiration was restored. Both the primary disease and complication had improved. The mode of ventilation was switched from mechanical to Synchronized Intermittent Mandatory Ventilation (SIMV). Parameters of assisted ventilation were gradually modified and eventually assisted ventilation was completely removed. The baby showed no shortness of breath or cyanosis when given oxygen inhalation via nasal catheter and was then transferred to the ENT unit. Oxygen nebulization of drugs was performed and antibiotic regimen selected based on the results of bacterial culture of the secretion collected from damaged mucosa. The formula for nebulization was 5 ml 0.9% sodium chloride, 0.25 g cefoperazone, 5 mg ambroxol and 1 mg pulmicort respules. On November 15th, the baby underwent another BAL. After the procedure, it was observed that mucosa of the left bronchus had been restored. The right bronchus showed much less white pseudomembrane and the mucosa was repaired by new tissues. The bronchial mucosa of right middle and lower lobes were mildly swollen (Figure 8). Chest X-ray on November 18th showed that the atelectasis on the right upper lung was cured after treatment (Figure 9). Thereafter, the baby was discharged from hospital.
Results
On December 10th, the baby was admitted again due to “recurrent irritating cough during the past 2 weeks”. Complete blood count showed WBC 14.6×109/L, N 55% and L 42%. Chest X-ray revealed that atelectasis on right upper lung was cured, but there was infection in the right lower lung (Figure 10). The baby underwent another three BALs. In the last BAL, the entrance of right middle and lower lobes showed scar contracture and stenosis. The entrance of the upper lobe was slightly narrowed and no abnormality was seen in the left lung. The mucosa was smooth and no narrowing of the entrance was seen (Figures 11 and 12).
Discussion
Respiratory foreign body in children is a severe emergent disease in otorhinolaryngology. Without timely and effective treatment, the disease causes a series of complications and is life-threatening in severe cases. Inhalation injury is damage to the airway or lung tissues caused by large quantity of inhaled hot air, smog of flame, hot vapour and toxic chemicals with concomitant burns in other sites [1]. Data reported by foreign and domestic scientists suggest that the mortality is generally 40-60% and could be as much as 80%. Patients with severe respiratory burn show even higher mortality of 90% [2]. Improvement of the perioperative treatment and post operative assessment in children with respiratory foreign body and concomitant inhalation injury is an effective way to reduce mortality and help patients survive the shock stage.
The characteristics of inhalation injury of respiratory tract by lime
The baby had inhaled lime powder, which is highly hydroscopic. Lime, when inhaled is hydrated in the airway and becomes calcium hydroxide. During the reaction, huge amount of heat is produced resulting in damage to the epithelial cells of airway mucosa and increased secretion by glands. Therefore, large amount of secretion is generated and airway mucosa gets congested and swollen. In the meantime, the heat also stimulates alveolar epithelial cells and causes acute lung injury. In severe cases, necrotizing pseudomembrane inflammation can also occur. Consequently, exfoliated pseudomembrane causes obstruction of the small airways. Progressive obstruction of small airways leads to alveolar emphysema, alveolar atelectasis and atelectasis in a segment or lobe which eventually results in ventilation and air-exchange dysfunction followed by hypoxemia and carbon dioxide retention. Without timely treatment, patients die of respiratory and circulation failure.
Precise and early diagnosis
Precise and early diagnosis is critical for improving the cure rate of respiratory foreign body and concomitant inhalation injury and reducing complications. The diagnosis is mainly based on aspiration of foreign body and typical symptoms together with necessary examinations, such as physical examinations, X-ray examination, blood gas analysis and complete blood count. In this case, the baby showed confusion, listlessness and extreme shortness of breath on admission. RR was 40 to 50 times/min, and transcutaneous SaO2 70-80%. Results of blood gas analysis and chest X-ray suggested damage and lime particles were detected in the bronchus below carina. Hypoxemia lasted for more than 24 hours, with concomitant symptoms of atelectasis and emphysema. The patient was diagnosed with respiratory foreign body with concomitant severe inhalation injury and respiratory failure according to the guidelines of Modern Therapeutics of Respiratory Diseases and diagnostic criteria of respiratory failure [3,4].
Early aministration of high dose glucocorticoid
Besides severity of inhalation injury, timing of administration of glucocorticoid is also a critical factor in deciding the clinical outcome. A Research study by Jing-Min Cao et al. [5] has demonstrated that dexamethasone effectively regulated such abnormality by promoting the synthesis of alveolar surfactant, stabilizing cells and lysosomal membrane and reducing permeability of microvasculature, thus, alleviating the damage of the lung tissue. Moreover, another research study by Wen-Jun has suggested that dexamethasone inhibited the activation of transcription factor NF-κB and partially blocked the production of cytokines and adherins, thereby, reducing the damage and inflammation [6]. Hence, we can infer that early administration of glucocorticoid could reduce inflammatory response and edema in local tissue and alleviate the tissue damage mediated by immune system of the host. In this case, the baby was given early administration of meprednisone, which effectively alleviated the airway edema and prevented aggravation of inspiratory dyspnea. The patient did not undergo tracheotomy due to rigorous monitoring.
Early tracheal intubation or tracheotomy
For patients with concomitant inhalation injury, blood oxygen saturation should be routinely monitored. Repeated blood gas analysis should be performed when necessary. For patients with established moderate or severe inhalation injury, tracheal intubation or tracheotomy should be performed within 6 hours. The indications of tracheal intubation or tracheotomy are; 1. Severe burn with acute edema in the face, oral cavity and nasal cavity; 2. Significant edema or armorlike eschar in the neck and/or chest that interferes with breathing; 3. Signs of significant dyspnea after burn, including lip cyanosis, flapping nosewing and positive three-concave sign; 4. Continued hypoxemia which necessitates mechanical ventilation; 5. Concomitant pneumonia, where the patient is unable to cough; 6. Increased airway secretion with exfoliated necrotic mucosa or pseudomembrane, which indicates repeated suction or lavage and 7. Coma with concomitant gastric retention.
Establishment of mechanical ventilation
Generally, patients with mild inhalation injury whose PaO2 is above 8.0 Kpa, or clinically stable patients at recovery phase of a respiratory failure can be given oxygen via nasal catheter. Patients with severe inhalation injury often show progressive hypoxemia, pulmonary edema or bronchopneumonia in early stages. Continuous hypoxemia often necessitates mechanical ventilation. The goal of mechanical ventilation is to help patients survive the acute phase of respiratory failure and increase air-exchange in patients with damaged ventilation thus, making subsequent treatments possible. In this case, sole oxygen support and medicinal therapy were not enough to solve the respiratory failure. To increase air-exchange in patient’s alveoli and improve blood oxygen saturation, we immediately provided bedside tracheal intubation and started assisted mechanical ventilation thereafter. P-CMV mode was first used in assisted ventilation and later switched to SIMV mode when respiratory strength was partially restored. Mechanical ventilation can alleviate hypoxemia of the body in a short period of time, rapidly turn the situation around and can prevent tracheotomy. It also helps restore the patient’s consciousness and relieves the paralysis of respiratory center, while potently enhancing the overall air-exchange saving time for further treatments.
Mechanisms of PEEP
The baby experienced hypoxemia resulting from severe inhalation injury. As hypoxemia in this case was mainly caused by increased pulmonary shunt flow, general mechanical ventilation was not desirable and hence, Positive End-Expiratory Pressure (PEEP) was an appropriate option. The mechanisms of PEEP are as follows: 1. Increases functional residual volume and retains some air in the alveoli at the end of expiration and prevents alveoli from collapsing. It also reopens collapsed alveoli and increases ventilation/ perfusion ratio; 2. Improves pulmonary compliance constantly expanding the alveoli and increases lung capacity. It also helps maintain surface tension in the lung and thus, improves pulmonary compliance; 3. Improves overall oxygen delivery and increases oxygen content in the blood. Given constant cardiac output, such an effect improves oxygen delivery; 4. Elevates bronchial vascular resistance which reduces blood flow and alleviates pulmonary edema. PEEP is effective in treating and alleviating pulmonary edema and preventing pulmonary injury related to the collapse of small airways. For patients with respiratory failure, it may also lower respiratory energy consumption. In this case, the baby was given systemic antibiotic therapy via intravenous injection, together with assisted mechanical ventilation, bronchoalveolar lavage by bronchofibroscopy and local injection. One week later, assisted ventilation was removed and pulmonary infection was controlled. Both repeated complete blood count and blood gas analysis revealed normal results.
Methods for anesthesia
The combination of intravenous ketamine and sodium y-hydroxybutyrate is a clinically common anesthetic approach. Laryngeal spasm, a common complication during surgery is, believed to be related to the shallow anesthesia and inappropriate administration of ketamine. Therefore, y-hydroxybutyrate was administrated by intravenous injection, while, propofol was given by injection pump. Meanwhile, isoflurane was administered via face mask. Furthermore, topical anesthesia of laryngeal and bronchial mucosa was induced by 1% decaine under laryngoscope. When anesthesia became shallow, isoflurane was administered via bronchial side-port immediately to increase the depth of anesthesia. The injection rate of propofol was elevated as well to prevent spasm of the larynx and bronchus and to increase the success rate of the operation.
Surgical procedures
We used rigid bronchoscopy and bronchoalveolar lavage by bronchofibroscopy for the removal of foreign body. The bronchofibroscope was first inserted via tracheal intubation. Then, the trachea, bronchus and bronchi of each lobe and segment were examined. Secretions in trachea and bronchi were carefully removed by suction. During the procedure, bronchi of right middle and lower lobes were seen blocked by large amount of white lime powder. Thereby, bronchofibroscope was replaced by rigid bronchoscope 3.5 STORZ and introduced via laryngoscope. Lime was removed by clamps for bronchial foreign body until the obstruction of the bronchi was mostly cleared. Then bronchofibroscope was placed back in position for investigation and alveolar lavage.
Early bronchofibroscopic examination and treatment
Injured trachea, bronchus and lung tissues are a hotbed for infection. By using bronchofibroscopy at an early stage, we can figure out the site and severity of the lesions, give timely treatment and determine prognosis as well. This shortens hospitalization and reduces mortality. During fibroscopic examination, we can directly visualize the pathological changes in nasopharynx, glottis, trachea, bronchus and so forth. Particularly, the pathological changes such as congestion, swelling, hemorrhage, vesicle, ulcer and the amount of airway secretions can be clearly analyzed and determined under direct visualization. Fibroscopy is the best direct approach to determine the severity of inhalation injury and to confirm whether or not bronchi are obstructed. Alveolar lavage by fibroscopy enables removal of secretion under direct visualization, prevents unguided sputum aspiration and consequent injury on airway mucosa. By removing viscous sputum with lavage and suction, secretion in small bronchi and alveoli will be completely cleared and airway obstruction will be resolved. It improves both the effect of antibiotic therapy, the functions of ventilation and air-exchange [7]. In patients with inhalation injury, airway mucosa is erosive and ulcerative to a varied degree. Therefore, during the manipulation, the bronchoscope should be situated in the center of the airway as much as possible so as to avoid rubbing the airway mucosa of the patients with the fibroscope and subsequent damage on the airway mucosa. Friction-related abrasion on the fibroscope can be reduced as well. In patients with inhalation injury, tracheal and bronchial mucosa is often degenerative and necrotic. Cilia could disappear in some cases. Since the natural defense barrier is impaired,and clearance of sputum and bacteria in the airway is weakened, susceptibility to bacteria and chance of airway infection are thereby increased. Bacterial culture and susceptibility test on the secretions obtained under fibroscope, together with continued observation on the clinical status, provides evidence for the selection of antibiotic for lavage and systemic application. As for intra-tracheal lavage, normal saline is the most suitable lavage solution that induces no adverse reactions in the lung and exerts no influence on the absorption or effect of the drugs. It does not impact patients’ ventilation and air-exchange as well. As for the selection of intra-tracheal antibiotics, aminoglycosides and third-generation cephalosporins are the first choice drugs. They are broad-spectrum antibiotics with minimal tissue toxicity, irritation and sensitization on the airway, which makes them well tolerated drugs for the patients [8]. However, given the ototoxicity and nephrotoxicity of aminoglycosides, they should be used with caution in children. Besides locally injected antibiotic, dexamethasone was also added into the lavage solution at the same time in this case. Such combination not only increases the effective drug concentration in local tissues, but also the drug concentration in the lesions to an effective bactericidal level. High-concentration corticoid on local lesions relieves the inflammation, bronchial spasm and counteracts hypersensitivity. Therefore, the combination promotes remission and improvement of the lesions [9]. Further, the addition of diluted epinephrine into the lavage solution reduces the congestion and swelling of bronchial mucosa, favoring the removal of secretion and guarantees an unobstructed airway.
Post-operative treatment
The patient showed significantly better respiration after the first operation. Pulmonary signs were also relieved. Given the possibility of residual lime in bronchi and secondary chemical injury, the patient was sent to ICU and was given positive airway pressure ventilation, antibiotic, corticoid and nebulization. Repeated complete blood count, blood gas analysis and chest X-ray were performed after the operation.
Management and prevention of complications
Inhalation injury is often accompanied by burns elsewhere. It is necessary to monitor the vital signs, hematuria and urine output of the patients. Early administration of adequate fluids, correction of water -electrolyte imbalance, acid-base imbalance and application of antibiotics are important steps in preventing shock, acute kidney failure and pneumonia impeding the development of multiple organ failure and helping the patients survive the crisis. Application of antacid proton pump inhibitor and gastric mucosa protective agent are effective in preventing stress-induced ulcers.
Conclusion
The patient was treated by the comprehensive scheme described above. At week one, assisted ventilation was removed. At day 15, chest X-ray and pulmonary function examination suggested improvement in the patient. At present, the patient is still subject to follow-up. In addition, it has been inferred that the acute phase of inhalation injury is generally 6-48 hours after injury. Therefore, we used BAL for the first time in treating severe inhalation injury, which should be performed within 6-48 hours after injury. Between days 3-5 after injury, with exfoliation of necrotic airway mucosa and increased secretion, the airway is susceptible to obstruction, which makes it the most dangerous moment during the course of the disease. At this point, the second BAL should be performed as soon as possible. This is because of the fact that the clearance of exfoliated mucosa and secretion in the airway is the key step for the treatment in this period. Thereafter, the number of lavage can be decided based on respiration, pulmonary signs and airway secretion. For patients with severe damage on airway mucosa, lavage should be performed every 2-3 days. Between days 10-14 after injury, necrotic tissue is still exfoliating. Sometimes, exfoliated “bronchial tree” can become a flapper valve and cause airway obstruction. In the meantime, mucosa is being repaired by new tissues. At this point, another BAL is necessary. Thereafter, repeated BAL can be given based on clinical status. In our case, the baby underwent a total of 6 BALs, which produced satisfactory treatment outcome.
References
- LI A (2002) Editor in chief Bums of Li AO. Shanghai: Shanghai Science and Technology Press 153.
- Zhu j, He QY, Li P (2003) Clinical Application of Fibrobronchoscope. In: Inhalation Injury. China Journal of Endoscopy 9: 65-66.
- Shi Y, Chen Z (2002) Modern Therapeutics of Respiratory Diseases, Beijing: Beijing People’s Military Medical Press 715-719.
- Zhong N (2001) Respiratory Failure In: Internal Medicine. (5thedn), Beijing: Beijing People’s Military Medical Press 46-61.
- Cao J, Lu T, Wang B (2003) Regulation of Dexamethasone on the Death of Neutrophil. Chinese Journal of Plastic Surgery 19: 2.
- Li W, Yang Z, Ji T, et al. (2002) The Role of NF-?B Activation in the Pathogenesis of Smoke Inhalation Injury and the Effect of Dexamethasone on it. Medical Journal of Chinese People’s Liberation Army 27: 206.
- Zhu L, Niu S (2002) Mechanical Ventilation. Shanghai Science and Technology Press 306.
- Zhang J, Zhang Y (2004) Analysis on Diagnostic and Treatment Scheme to Reduce Complications of Tracheal-Bronchial Foreign Body and Mortality in Children. Chinese Journal of Otorhinolaryngology Head and Neck Surgery 39: 658-662.
- Liu C (2004) Modern Diagnostic and Therapeutic of Fibrobronchoscopy. Beijing People’s Military Medical Press 165-168.
Citation: Liu Db, Qiu Sy, Zhou J, Huang Zy, Zhong Jw (2013) Treatment of an Acute Respiratory Failure Child Caused by Special Airway Foreign Body. Otolaryngology 3:141. DOI: 10.4172/2161-119X.1000141
Copyright: © 2013 Liu Db, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 15920
- [From(publication date): 9-2013 - Oct 02, 2025]
- Breakdown by view type
- HTML page views: 11072
- PDF downloads: 4848