Tuberculous Mastoiditis: Report of an Uncommon Case in Morocco
Received: 12-Jul-2012 / Accepted Date: 30-Jul-2012 / Published Date: 03-Aug-2012 DOI: 10.4172/2161-119X.1000119
Abstract
Although tuberculosis is a major problem of public health in Morocco, the tuberculous mastoiditis remains extremely rare, and its diagnosis is often delayed. We report here the case of a 3-year-old child who had unusual chronic left mastoiditis and retro-auricular fistula, associated with spontaneous discharge of bony sequestrum. CT scan of temporal bones showed complete destruction of left mastoid cells. A left mastoidectomy confirmed the tuberculous mastoiditis diagnosis after histopathological examination. The clinical outcome was favorable after anti-tuberculosis treatment. Otologic tuberculosis of the ear is well described in the literature and symptoms include chronic otorrhea with audio-vestibular symptoms. The specificity of this case is that the child had an isolated involvement of the mastoid with spontaneous bony sequestrum discharge, but without otorrhea.
Keywords: Tuberculosis, Tuberculous mastoiditis, Bony sequestrum, Fistula, Mastoidectomy
251538Introduction
In Morocco, tuberculosis is a major public health problem. It is a contagious infection with endemic and epidemic transmission. According to WHO, about 10 million people are infected in the world and 3 million die every year mainly in developing countries [1,2].
The main germ “mycobacterium tuberculosis” becomes very aggressive when associated with local and/or general immune deficiency. The main risk factors include elderly, malnutrition and HIV infection [1,3].
Common infections are mainly located in the pulmonary system, lymph nodes and visceral organs. Middle ear infections and tuberculous mastoiditis are rare manifestations. They represent less than 0.1% of all chronic suppurative otitis media [1,2].
The most common tuberculous mastoiditis may be secondary to spread of infection through the Eustachian tube, the haematogenous route or the tympanic membrane [1,2,4]. The diagnosis of tuberculous mastoiditis can be difficult for a number of reasons including the wide range of symptoms. This often results in prolonged delays between the onset of symptoms and the diagnosis [1]. We present here a case report of tuberculous mastoiditis which underlines some of the diagnosis difficulties and potential complications.
Case report and Clinical Examinations
A 3-year-oldboy, vaccinated at birth, with no medical or surgical history, presented to our ENT department with left retro-auricular fistula, as a result of a progressive swelling for the past five months. There was no history of tuberculosis exposure. The child complained of hearing loss. There was no otorrhea, vertigo, facial nerve palsy or fever. The evolution was marked by spontaneous discharge of bony sequestrum from the retro-auricular fistula.
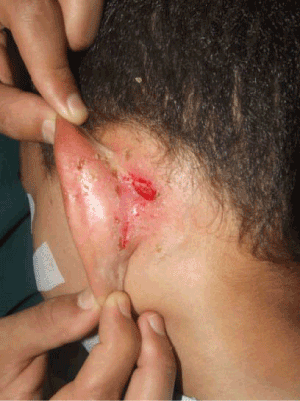
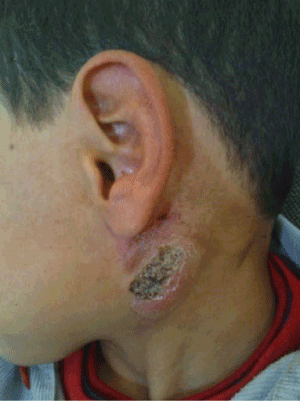
Clinical examination showed a painful left mastoiditis fluctuant to palpation, with a cutaneous purulent fistula discharging bony sequestrum (Figure 1).
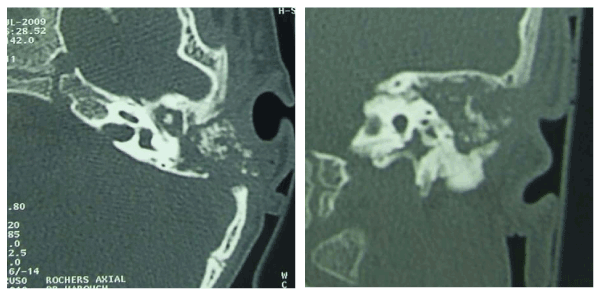
Otoscopy showed an inflammatory bulging tympanic membrane without purulent secretions or perforations. The Ear, Nose and Throat (E.N.T) examination was normal, with no right ear abnormalities or lymph nodes. Neurological and pulmonary examinations were strictly normal. Biological results revealed hyperleukocytosis at 25000/ μl, with 39% of lymphocytes. The C-reactive protein (CRP) was 30 mg/l. Chest X-ray was normal. The audiogram showed a left ear conductive loss (35 dB), with an air bone-gap of 25 dB. CT scan of the temporal bones showed left middle ear filling cavities associated with irregular destruction in mastoid air cells and bony sequestrum, but no intracranial expansion (Figure 2).
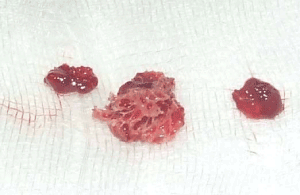
In regards to the atypical clinical presentation, a left mastoidectomy was therefore performed. Granulomatous inflammation of mastoid mucosa was found and a bony sequestrum was removed (Figure 3). Histological examination of the resected material revealed the presence of a tuberculous granuloma with caseous necrosis, confirming the diagnosis of tuberculous mastoiditis.
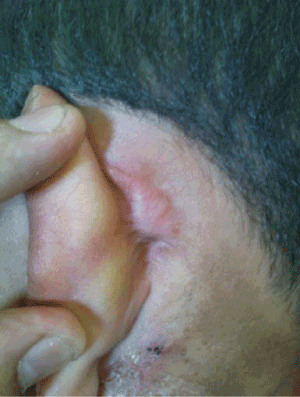
Anti-tuberculosis treatment including rifampicin, isoniazid, pyrazinamide and ethambutol, was started. At follow-up two months later, clinical examination showed the disappearance of the fistula, the complete healing of the mastoid wound and the normalization of the tympanic membrane (Figure 4), but the patient showed tuberculous cervical lymph nodes with necrosis (Figure 5). The complete healing was observed by the end of the anti-tuberculosis treatment maintained for 9 months. Today, the child is declared cured, at 30 months followup.
Discussion
This case highlights a number of potential issues leading to the delay in diagnosis, which is a hallmark of tuberculous mastoiditis. Although rare, the classical description of tuberculous otitis, reported in literature, includes painless otorrhea, facial palsy and multiple perforations [1,3,5,6]. Contrary to this classical description, in our case there was no evidence of otorrhea or facial paralysis, and any perforation was observed by otoscopy. However, the patient was suffering from hearing loss. In literature, it might range from moderate conductive hearing-loss tocophosis [1].
One or multiple perforations in the tympanic membrane, with polypoid middle ear mucosa are typical of the disease. Our patient had an inflammatory bulging of the tympanic membrane, without perforations.
At an advanced stage of the disease, the eardrum or the atrium can present a granulomatous or necrotic aspect, and bony sequestrum occurs frequently [4]. The occurrence of pre-auricular or cervical lymph nodes is not uncommon, and development of retro-auricular fistulais usual [1-4]. Our patient had a mastoiditis associated with left retro-auricular fistula and cervical lymph nodes.
Tuberculous mastoiditis may cause serious complications. When the infection spreads from the ear canal to the nearby tissues such as the skull base or the tegmen tympani, tuberculous mastoiditis could lead to skull base osteomyelitis or tuberculous meningitis [1].
According to the study reported by Rho et al. [7], CT scan of the temporal bones showed, in most cases, soft tissue attenuation in the entire middle ear cavity, preservation of the mastoid air cells without sclerotic change, and soft tissue extension to the external auditory canal (EAC) or mucosal thickening of the bony EAC. In our case, the CT scan showed total destruction of mastoid air cells with multiple bony sequestrae, and bone cavities filled in the left middle ear. Table 1 resumes some CT scan results reported in literature.
| Reference | n | Age (years) |
Gender | Symptoms | Otoscopy | CT-scan | |
|---|---|---|---|---|---|---|---|
| Hamouda et al. (2008)(3) |
1 | 13 | F | Otorrhea and cervical lymph node | Polypoid of the external auditory meatus | Filled mastoid | |
| Chmielik et al. (2007)(2) | 1 | 4 | M | Acute otitis media with fever | Inflammatory bulging of the eardrum | Filled mastoid and bone erosion | |
| Saunders et al(2002)(4) | 1 | 7 | F | Reccurent otorrhea | Anterior retraction of eardrum | Filled mastoid without bone erosion | |
| Vital and Al (2002)(6) | 4 | 19-56 | 3F-1M | Otorrhea | Multiple perforations of eardrum | - | |
| Meher et al (2006)-10 |
5 | 3-13 | 2F-3M | Retroauricular swelling (3) Retroauricular fistula (1) Facial palsy (1) |
Eardrum perforation, polypoid and granulation | - | |
| Our patient (2010) | 1 | 3 | M | Retroauricular swelling and fistula Spontaneous discharge of bony sequestrum |
Bulged eardrum with inflammation | Filled mastoid and destruction with bony sequestrum | |
Table 1: Main cases of auricular tuberculosis reported in literature.
According to Samuel and Fernandes [8], the incidence of bony sequestrum could reach 30% of cases. Therefore, CT scan is the imaging tool of choice to identify the bony sequestrum and the extent of the disease before surgical intervention. MRI can be also used for diagnosis; it helps identifying intracranial extension, but has a limited role for various complications of otologic tuberculosis [9]. Tuberculosis of the middle ear and mastoid may be associated with pulmonary involvement in 50% of cases; therefore a chest X-ray may facilitate the diagnosis [1,3,7]. Finally, laboratory diagnosis can be problematical. The tuberculin intradermal test (also known as Mantoux test) is usually positive, but a negative test does not exclude the diagnosis. The diagnosis of tuberculous mastoiditis remains difficult, and is discussed and confirmed during the pre and post-operative period by bacteriological and histological findings [6].
The treatment is mainly medical, based on anti-tuberculosis drugs for a period ranging from 6 to 12 months. The role of surgery in the treatment of tuberculous mastoiditis is limited. Indeed, surgery is indicated only for loco regional complications, such as subperiosteal abscess evacuation or bony sequestrum removal. In the case of a suspected diagnosis, surgical exploration could be proposed for biopsy [4,5]. Finally, in case of facial paralysis, surgical decompression of the facial nerve may be beneficial, although this issue remains under debate [4]. However, the evolution of the facial paralysis is generally favorable under treatment.
Conclusion
Tuberculous mastoiditis is a rare clinical manifestation but potentially dangerous. The diagnosis is difficult therefore frequently delayed. In otologic infections when imaging results show significant destruction of mastoid air cells and presence of bony sequestrum, tuberculous mastoiditis should be suspected. The anti-tuberculosis therapy remains the main stay of treatment for mastoid and middle ear tuberculosis. Surgery aims to provide the samples required for bacteriological and histological examinations, allowing subsequently early diagnosis.
References
- Duclos JY, Darrouzet V, Ballester M, Bebear JP, Bebear CM (1999) Tuberculose de l’oreille moyenne ; Encycl Med Chir ( Elsevier,Paris ), Oto-rhino-laryngologie, 20-235-A-10, 4 p.
- Chmielik LP, Ziolkowski J, Koziolek R, Kulus M, Chmielik M (2008) Ear tuberculosis: clinical and surgical treatment. Int J Pediatr Otorhinolaryngol 72: 271-274.
- Hamouda S, Opsomer H, Delattre A, Thumerelle C, Flammarion S, et al. (2008) Tuberculous otitis media. Med Mal Infect 38: 608-611.
- Saunders NC, Albert DM (2002) Tuberculous mastoiditis: when is surgery indicated? Int J Pediatr Otorhinolaryngol 65: 59-63.
- Singh B (1991) Role of surgery in tuberculous mastoiditis. J Laryngol Otol 105: 907-915.
- Vital V, Printza A, Zaraboukas T (2002) Tuberculous otitis media: A difficult diagnosis and report of four cases. Pathol Res Pract 198: 31-35.
- Rho MH, Kim DW, Kim SS, Sung SY, Kwon JS, et al. (2007) Tuberculous otomastoiditis on high-resolution temporal bone CT: comparison with nontuberculous otomastoiditis with and without cholesteatoma. Am J Neuroradiol 28: 493-496.
- Samuel J, Fernandes CM (1986) Tuberculous mastoiditis. Ann Otol Rhinol Laryngol 95: 264-266.
- Munoz A, Ruiz-Contreras J, Jimenez A, Maté I, Calvo M, et al. (2009) Bilateral tuberculous otomastoiditis in an immmunocompetent 5-year-old child: CT and MRI findings. Eur Radiol 19: 1560-1563.
- Meher R, Singh I, Yadav SP, Gathwala G (2006) Tubercular otitis media in children. Otolaryngol Head Neck Surg 135: 650-652.
Citation: Abada RL, Nadef N, Elkhiati G, Rouadi S, Mahtar M, et al. (2012) Tuberculous Mastoiditis: Report of an Uncommon Case in Morocco. Otolaryngology 2:119. DOI: 10.4172/2161-119X.1000119
Copyright: © 2012 Abada RL, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 18783
- [From(publication date): 8-2012 - Nov 25, 2025]
- Breakdown by view type
- HTML page views: 13992
- PDF downloads: 4791