Tympanosclerosis - a Beginner's Worry: a Case Series and Review of Literature
Received: 06-Apr-2013 / Accepted Date: 04-May-2013 / Published Date: 11-May-2013 DOI: 10.4172/2161-119X.1000133
Abstract
Introduction: The aim of the present study is to study cases of tympanosclerosis retro-prospectively in regards to their clinical presentation and also their surgical management.
Materials & Methods: 73 cases of tympanosclerosis were studied over a period of two years. Patients were also classified as those operated by the consultant surgeon and the resident surgeon.
Results: The surgical procedure commonly carried out was Type 1 Tympanoplasty, with no significant difference seen with partial or complete removal of tympanosclerotic plaques with regards to the graft uptake or the post operative hearing thresholds. A difference was observed in the number of complications in cases operated by the consultant surgeon as against the resident surgeon.
Conclusion: Though the symptoms of tympanosclerosis may not be a dramatic it does pose a significant dilemma especially to a novice otologist with regards to its complete resection.
Keywords: Sclerosis, Hearing loss, Tympanoplasty, Tympanic membrane
253729Introduction
Tympanosclerosis is an abnormal condition of the middle ear cleft in which there are calcerous deposits in the tympanic membrane, tympanic cavity, involving the ossicular chain and occasionally in the mastoid. It is considered as a long term sequlae of Chronic Otitis Media (COM).
The aetiopathogenesis of tympanosclerosis is obscure but many theories have been put forth to explain its origin. The widely accepted view is that it is an end product of the healing process in which the collagen in fibrous tissue gets hyalinized due to the inflammatory process of COM leading to calcium deposits in different parts of the middle ear. Although the pathogenesis is not clear, a prerequisite appears to be COM followed by healing.
Tympanosclerosis though a relatively benign condition causes predominantly a conductive type of hearing loss. But this loss usually depends on the extent of the tympnosclerotic plaques and their location. However the exact extent of tympanosclerosis can be judged only after formal exploration of the middle ear and it being its only definitive treatment.
In our study cases of tympanosclerosis were studied pre operatively with thorough history and clinical examination. Cases were operated and the type of surgery decided according to the type of defect and also followed up post operatively with respect to hearing improvement and successful graft uptake.
Materials and Methods
A retro prospective study of 73 cases of tympanosclerosis in COM was carried out from Oct 2009 to Sept 2011 seen at Sanjeevan Medical Foundation E.N.T. Post Graduate Institute, Miraj, Maharashtra, India. All of these 73 cases had undergone some form of middle ear surgery to treat their chronic ear problem. 43 cases were operated by the consultant and 30 cases by the third year post graduate resident. The results from both the groups were analyzed taking into account the hearing outcome, graft uptake, post operative complications.
To avoid spurious results the following exclusion criteria was considered and taken into account before selecting the cases for this study.
1) Patients with traumatic tympanic membrane perforation.
2) Previous otologic surgery
3) Use of systemic or local ototoxic drugs in the past
4) Patients having any congenital ear anomalies
5) Patients having hereditary cause of hearing loss
6) Patients using hearing aid
The diagnosis of chronic otitis media was based on presence of or history of otorrhoea, ear blockage, and tinnitus as well as clinically certain pathology. The presence of hearing loss was also taken into account. Tympanosclerosis is diagnosed as being chalky, white patches in the tympanic membrane or the middle ear structures. Ears were examined with otoscope and microscopic examination was done in all cases in pursuit of excellence.
Meticulous ear, nose and throat examination, general and systemic examination of all patients were done. After clinical examination all cases were screened for audiologic profile using pure tone audiometery.
Appropriate type of surgery was decided based upon the extent of disease and involvement of ossicles. Eg with pars tensa perforation and ossicular chain intact only a Type 1 Tympanoplasty was done.
Operative findings of all cases which underwent surgery were noted. Middle ear status was examined. During surgery, the ossicular mobility, status of the middle ear mucosa and degree of tympanosclerosis in middle ear and ossicles were inspected.
All patients had to undergo a strict follow up at the end of 6 weeks to check the uptake of graft and post operative pure tone audiometry.
Results
Of the 73 cases studied 37 patients were in the age group 16-30 yrs (48%) of all the cases having a male to female sex ratio of 1.14:1.
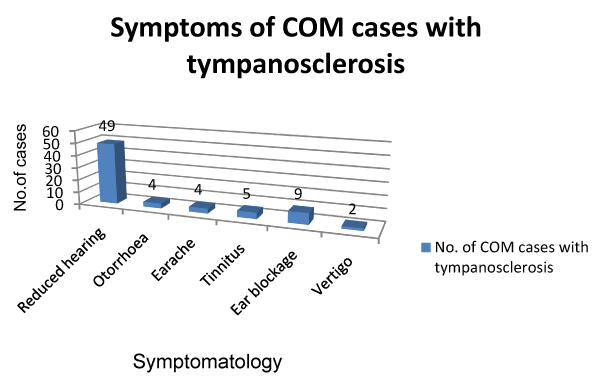
The commonest presentation of tympanosclerosis in our study was in the form of hearing impairment with 67.1% cases (Figure 1).
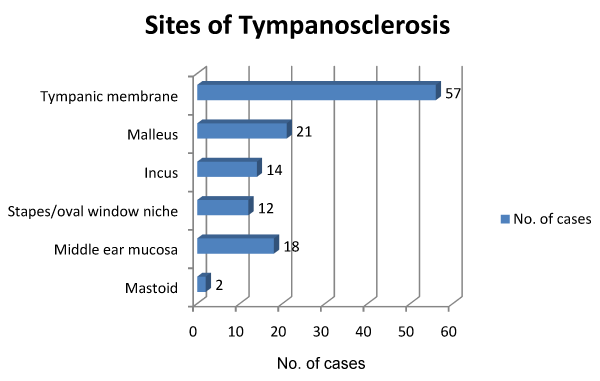
39 cases (53.4%) of Tympanosclerosis showed a central perforation in the tympanic membrane (Figure 2). 62 cases in our study had pure conductive hearing loss and had the following intra operative findings (Figure 2). Tympanosclerotic plaques were in the tympanic membrane in majority of cases which were 75.3% and in the middle ear the plaques were maximum around the malleus which was 27.4% of all tympanosclerosis cases.
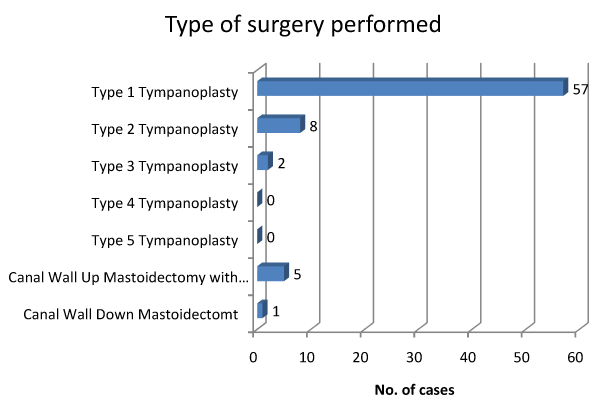
57 cases had to undergo Type 1 tympanoplasty (Figure 3). Of these 57 cases 30 cases were operated by consultant and 27 by the post graduate resident. A standard post auricular incision was used and underlay technique was used to graft placement following exploration of the middle ear and resecting as much of tympanosclerotic plaques as practical. Intra operative findings were recorded and also any intra or post operative complications. Strict follow up was advised at 6 weeks. Intra operative complications (Table 1) were managed accordingly. Result of Graft Uptake in cases where Type 1 Tympanoplasty was done was studied statistically using chi square test and the degree of freedom (df=1) the chi square value was 0.401 and the p value was 0.5267 which is not significant as p>0.05 (Table 2).
| COMPLICATIONS | OPERATED BY CONSULTANT | OPERATED BY RESIDENT |
|---|---|---|
| Malleo incudal joint dislocation | ------------ | 1 |
| Incudo stapedial joint dislocation | 1 | 3 |
| Stapes dislocation | --------- | ---------- |
| Facial Nerve paresis/palsy | ---------- | 1 |
| Sensorineural hearing loss | --------- | ----------- |
Table 1: Intra Operative Complications.
| Tympanosclerotic plaques | No. of cases | No. of cases in which graft uptake was successful | Graft uptake success rate |
|---|---|---|---|
| Completely removed from the tympanic membrane (n=46) | 46 | 44 | 95.6% |
| Partially removed from the tympanic membrane (n=11) | 11 | 10 | 91% |
Table 2: Result of Graft Uptake in Type 1 Tympanoplasty.
The decision to completely or partially remove the plaques from the tympanic membrane was taken on the operating table. Of the 57 cases which were studied as the ones following Type 1 Tympanoplasty in 46 cases, plaques were completely removed from the tympanic membrane whereas in 11 cases they were partially removed. Of the 46 cases with complete removal, 26 were having plaques only in the tympanic membrane, 11 around the malleus, 4 around the incus and 5 in the middle ear mucosa. 11 cases where partial removal was done, 8 cases had plaques only in the tympanic membrane, 5 around the malleus, 6 in the middle ear mucosa and 1 around the stapes.
Pure tone audiometry results (Table 3) after Type 1 Tympanoplasty in cases where different degree of tympanosclerotic plaques removal is done (complete or partial) at 6 weeks follow up and the results studied statistically using non parametric Mann- Whitney test as the data was ordinal data. Using this test the results can be interpreted as the difference between the two parameters was not significant as the p value is more than 0.05
| Removal of Tympanosclerotic plaques | Pre-operative Pure Tone Audiogram (dB) | Post operative Pure Tone Audiogram (dB) |
|---|---|---|
| Complete (46 cases) Mean ± SD |
35.95 ± 12.37 | 26.70 ± 10.17 |
| Partial (11 cases) Mean ± SD |
38.36 ± 9.62 | 28.55 ± 7.64 |
| p value | 0.083(NS) | 0.441(NS) |
Table 3: Pure tone audiometry results.
Discussion
Tympanosclerosis is a long term sequlae of chronic otitis media. There was a slight predominance towards males (53.4%) of all cases of tympanosclerosis with a male to female ratio of 1.1:1. Bhaya et al. [1] and Yabe et al. (1995) had reported a male to female ratio of 1.6:1 and 1.8:1 respectively whereas Pal et al. [2] in their study had described the ratio to be roughly 1:1. This variation in the data was said to be due to the extremely random selection of patients in the various studies.
In present study the commonest presenting symptom was hearing impairment in 72.6% cases with conductive loss being the commonest in 85% of varying degree. Pal et al. [2] in their series had found that about 60% of their cases had deafness as their presenting symptom of which 83.3% had a conductive loss. The impairment of hearing was due to involvement of middle ear conductive system due to the inflammatory process leading to tympanosclerosis (Sorensen & True, 1978).
Clinically, a feature of tympanosclerosis has been lack of suppuration in the affected ear, especially if it is affected over a long period. Being true to this otorrhoea was only seen in 4 of the 73 cases of tympanosclerosis, making it only 5.5% of the cases. Asiri et al. [3] in their series had found otorrhoea as a chief complaint in only 13 of 90 cases whereas the incidence of dry ears in their study was 86%. Wu et al. [4] in their study too found the incidence of dry ears to be significant at 77.78%
In the case series of Pal et al. [2] 27 patients of 50 had a central perforation that made it 54% of all the patients of tympanosclerosis. In our study the cases of tympanosclerosis with central perforation were 39 out of 73 making it 53.4%. Whereas a healed perforation was seen in 10 of 73 cases (13.7%). These results compare favorably to those in literature where the open type is four to five times more common than the closed variety (Austin et al. and Tos et al.) [5,6] and that perforations are invariably sited in the pars tensa (Plester and Kamal) [7,8].
Only 1 case of cholesteatoma was seen of the 73 cases showing tympanosclerosis. Asri et al. 1999 in their series found only 2 cases of cholesteatoma and they concluded that association of choleasteatoma and tympanosclerosis may be regarded uncommon and coincidental. Plester (1972) considered it to be purely coincidental. Gibb (1979) also had a similar opinion [7].
The type of hearing loss seen in majority of cases was pure conductive hearing loss with 62 cases (85%). Remaining 11 cases showed sensorineural hearing loss, of the 11 cases 2 cases showed pure sensorineural hearing loss and 9 cases had mixed hearing loss. Gibb et al. (1971) had suggested that sensorineural hearing loss may occur due to involvement of the inner ear by tympanosclerosis. Uripin et al. (2000) in their study of 26 cases of tympanosclerosis found all of them to have conductive or a mixed loss.
The tympanic membrane is the commonest site where the tympanosclerotic plaques are seen. In 75.3% cases the plaques were seen in the tympanic membrane. According to Sade and Tos and Bak Pedersen [9] the tympanosclerotic plaques occur in areas where the number of mucus glands is lowest and the ciliary activity is least and thus the stagnation of inflammatory exudates is favored. The head of malleus and the body of incus both lodged in the attic are the commonest sites in the middle ear which are affected by tympanosclerosis and this being the main cause of the higher degree seen when the middle ear is involved.
57 patients out of 73 with tympanosclerosis had to undergo Type 1 Tympanoplasty by the post aural incision and underlay grafting technique was used in all cases. Only 1 patient with cholesteatoma was to undergo Canal Wall Down Mastoidectomy for the disease. The decision to completely remove the tympanosclerotic plaques or to keep them in situ was taken on the operating table and in 46 cases out of 57 undergoing Type 1 Tympanoplasty the plaques were removed completely while in rest few plaques were not touched especially around the stapes and the facial nerve. However, the decision varied among the consultant surgeon and the resident surgeon.
The most serious complication which occurred was facial nerve paresis (House Brackman 3) in the case done by the resident. The patient was managed conservatively with steroids and physiotherapy. The facial nerve recovered to HB 1 at 6 weeks follow up. No patient had sensorineural hearing loss or stapes dislocation. The incudostapedial joint dislocations were also on the higher side in cases (3 cases) done by the resident which was corrected using auto incus in 2 cases and in 1 case supporting with gelfoam sufficed.
All the patients were followed up at the end of 6 weeks to note the uptake of graft and also a post operative pure tone audiometry was done. The uptake of graft was seen in 54 cases undergoing Type 1 Tympanoplasty of 57 patients (94.7%) who underwent the surgery. graft uptake rate in cases; where tympanosclerotic plaques were completely removed was 95.6% and it was 91% in those cases where tympanosclerotic plaques were either partially removed or left as such. There was no significant difference in the graft uptake rate as the p value was 0.5267.
Prasad et al. [10] in their series had also not found any statistical significance between the groups where the plaques were completely removed or partially removed.
Also the hearing which was assessed at the end of 6 weeks was studied statistically and no significant difference in hearing was seen (p value was 0.441) which was more than 0.05 and hence statistically not significant. Thus tympanosclerostic plaques, if removed as far as practicable have no effect on post operative hearing status in patients undergoing underlay myringoplasty [10].
Summary and Conclusion
After collecting the data and after its analysis the following conclusions can be drawn:-
• Tympanosclerosis is a clinicopathological entity most commonly seen in COM with central perforation. It is slightly more common in males and occurs in a relatively younger age group of 16-30 years of age.
• It can affect almost any part of the middle ear cleft. Conductive hearing impairment being the most common and majority of patients suffered from a moderate hearing loss.
• Surgery being its only definitive treatment and often the exact extent of the disease can be accurately judged only on formal exploration of the middle ear.
• Removal of all the tympanosclerotic plaques is not fraught of the danger such manoeuvres may possess and should be done judiciously as the complete or partial removal of the tympanosclerotic plaques does not significantly affect the graft uptake or even the post operative hearing. A heroic surgery with an aim to remove all the tympanosclerotic plaques especially be a otologist early in his/her career may unnecessarily put the patient at risk from the dreaded complications of the surgery itself like a facial nerve palsy or even sensorineural hearing loss.
References
- Bhaya MH, Schachern PA, Morizono T, Paparella MM (1993) Pathogenesis of tympanosclerosis. Otolaryngology Head Neck Surg 109: 413-420.
- Pal Indranil, Sengupta A (2005) Clincopathological and audiological study of tympanosclerosis Indian journal of Otolaryngology 57: 235-239.
- Saad Asiria, Alaa Hashama, Fatma A Anazy, Siraj Zakzouka and Adel Banjar (1999) Tympanosclerosis: Review of literature and incidence among patients with middle ear infection. Journal of Laryngology and Otology 113: 1076-1080.
- Wu Y, Yin S, Zhu H, Zhang S (2006) Tympanosclerosis incidence among patient with chronic suppurative otitis media. Lin Chuang Er Bi Yan Hou Ke Za Zhi 20: 1016-1017.
- Austin DF (1988) Reconstructive techniques of tympanosclerosis. Ann Otol Rhinol Laryngol 97: 670-674.
- Mirko Tos, Torben Lau, Helge Arndal and Søren Plate (1990) Tympanosclerosis of the middle ear: late results of surgical treatment. Journal of Laryngology and Otology 104: 685-689.
- Plester D (1972) Tympanosclerosis. Australian Journal of Otolaryngology 3: 325-326.
- Kamal SA (1997) Surgery of tympanosclerosis. Journal of Laryngology and Otology 111: 917-923.
- Tos M, Bak Pederson K (1974) Middle ear mucosa in Tympanosclerosis. J Laryngol Otol 88: 119-126.
- Prasad PL, Bhattarai H (2009) Influence of Tympanosclerosis on Graft Uptake and Hearing Status in Patients Undergoing Underlay Myringoplasty J Nepal Health Res Counc 7: 116-119.
Citation: Asarkar A, Gosavi S (2013) Tympanosclerosis – a Beginner’s Worry: a Case Series and Review of Literature. Otolaryngology 3:133. DOI: 10.4172/2161-119X.1000133
Copyright: © 2013 Asarkar A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 20097
- [From(publication date): 6-2013 - Nov 09, 2025]
- Breakdown by view type
- HTML page views: 15368
- PDF downloads: 4729