Unilateral Submandibular Gland with False PET Positive Uptake in a Patient with Breast Cancer: Case Report and Review of the Literature
Received: 13-Jul-2011 / Accepted Date: 05-Nov-2011 / Published Date: 10-Nov-2011 DOI: 10.4172/2161-119X.1000106
Abstract
Unilateral submandibular gland aplasia is a rare entity with only thirteen cases reported in the literature. Most of the published patients were asymptomatic on presentation without any associated facial anomalies.We present a patient with a history of breast cancer with an incidental finding of unilateral submandibular gland aplasia presenting with asymmetric uptake of fluoro-2-deoxy-glucose (FDG) in the remaining submandibular gland on a positron emission tomography/computed tomography (PET/CT). Multiple options exist for imaging of the salivary glands which include plain radiographs, Tc-pertechnatate scintigraphy, sialography, ultrasonography, magnetic resonance imaging, and computed tomography. There are certain characteristics found in each category that would warrant further diagnostic inquiry. For combined PET/CT of the head and neck, there is inherent variable uptake of FDG due to the anatomy and structures involved in this region. Both the otolaryngologist and radiologist should work closely in assessing suspicious salivary gland tissue within PET/CT of the head and neck and correlating these findings clinically to consider further investigation.
Keywords: Unilateral submandibular gland aplasia, Ultrasonography, Positron emission tomography, Computed tomography.
247524Introduction
Aplasia or agenesis of the salivary glands is an uncommon disorder. Gruber first described a case of bilateral submandibular gland aplasia in 1985 and Bruno first described a case of unilateral submandibular gland aplasia in 1894. Since 1894, only thirteen cases of unilateral aplasia of the submandibular gland have been published within the literature. All previously reported cases of unilateral submandibular gland were incidentally found on imaging studies or cadaver dissection. In this case report, we present the fourteenth case of unilateral submandibular gland aplasia and the first associated with positivity of the unilateral submandibular gland on combined positron emission tomography/ computed tomography (PET/CT) scan in a patient with breast cancer.
Case Report
A 48 year old female with a past medical history of T2 N0 M0, ER positive, PR positive, HER-2/neu negative intermediate grade infiltrating ductal carcinoma of the right breast presented to the Otolaryngology clinic for evaluation of a PET/CT with increased fluoro-2-deoxy-D-glucose (FDG) uptake in the right submandibular gland. She was otherwise healthy and first became aware of minor fullness in the right neck four years ago without any change in size and other associated symptoms, including a history of sialoadenitis, dryness of the mouth, or dysphagia. She did not have any prior neck surgeries or other significant medical conditions.
On otolaryngic physical exam, she had minimal fullness in the region of the right neck, consistent with a right submandibular gland. Bimanual palpation of the left neck could not locate the left submandibular gland. The oral mucosa and submandibular papilla were normal appearing with good dentition.
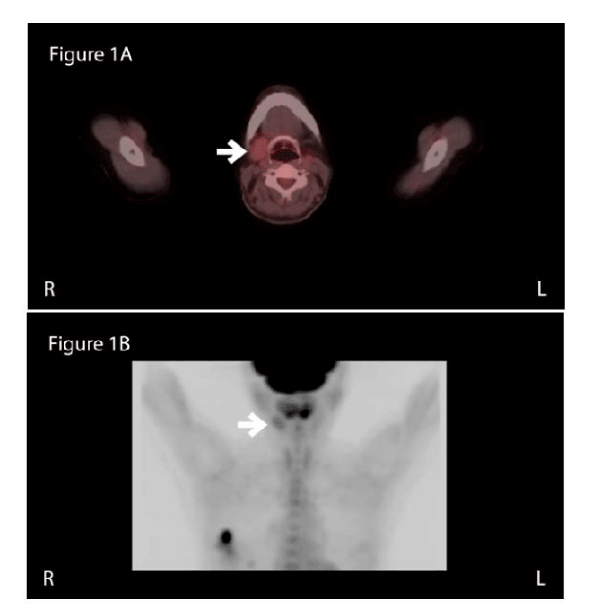
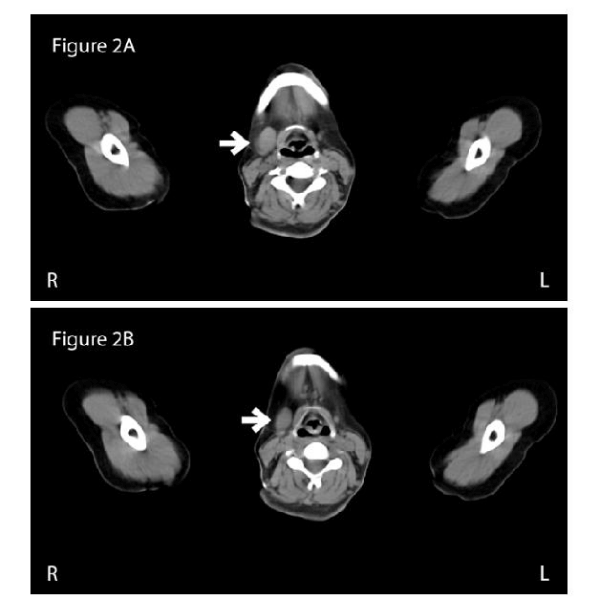
PET/CT performed earlier that week revealed a large area of increased FDG uptake in the region of the right superolateral breast consistent with known breast carcinoma. Additionally, she had a smaller focus of increased uptake further inferiorly within the right breast and another area of increased FDG uptake was visualized in the region of the right submandibular gland (Figure 1). CT scan correlation identifies a 2.8 cm X 1.9 cm right submandibular gland and absence of the left submandibular gland (Figure 2).
Figure 1: (A) Axial fused PET/CT scan showing increased FDG uptake in the right submandibular gland (arrow) and absence of left submandibular gland. (B) Coronal PET scan with increased FDG uptake in the right submandibular gland (arrow) and significant FDG uptake in the right superolateral breast consistent with known malignancy.
She was referred for ultrasound evaluation of the right submandibular gland and possible FNA. She was evaluated with ultrasonography which revealed a slightly prominent right submandibular gland, homogeneous, slightly hyperechoic echotexture typical of a normal submandibular gland. No abnormal enlarged lymph nodes, vascularity, calcification, or nodules noted within or surrounding the right submandibular gland. Left submandibular gland was not visualized and aplastic. FNA was not deemed necessary since multiple imaging studies revealed a completely normal appearing right submandibular gland with associated left submandibular gland aplasia. She had further follow up with repeat ultrasonography in six months which revealed no changes in the right submandibular gland.
The left submandibular gland aplasia resulted in asymmetrical FDG uptake on PET/CT resulting in a false positive scan with a slightly prominent, normal appearing right submandibular gland.
Discussion
The major salivary glands develop between the fourth and eight week of gestation through an expansion of the oral epithelium into a solid cord of cells into the underlying mesenchyme. The solid cords branch, expand in size and later develop lumens. The proximal ends of these cords become the main salivary duct and the distal end form the secretory acini. The first gland to develop is the parotid gland around the fourth week of gestation. Around the sixth week, the submandibular glands appear as paired primordium near the midline of the tongue. The last of the salivary glands to develop in the ninth week is the sublingual gland which arises between the tongue and the mandibular arch. Aplasia of the salivary gland may be partial or complete; the etiology is believed to be due to disruption during early fetal development [1].
Most of the forty reported cases of major salivary gland aplasia involved congenital absence of all major salivary glands or congenital absence of the parotid gland. Patients with aplasia of multiple salivary glands usually have associated facial anomalies such as atresia of the lacrimal puncta, mandibulofacial dysostosis (Treacher-Collins syndrome), first or second branchial arch abnormalities, or congenital malformations of the temporomandibular component [1]. Currently, there are two published case reports describing bilateral submandibular gland aplasia, both found incidentally, both asymptomatic, and neither associated with facial anomalies [2,3].
Isolated unilateral submandibular gland aplasia is an extremely uncommon finding. The true incidence of congenital submandibular gland aplasia is unknown and is confounded by the asymptomatic nature in most patients. Patients with aplasia of the salivary gland can present with symptoms such as dry mouth, dysphagia, or dental caries which may be due to erosion of enamel. Most patients presenting with unilateral submandibular gland aplasia are asymptomatic and none of the previously published patients had accompanying developmental disorders. The asymptomatic nature of unilateral submandibular gland aplasia is probably due to compensatory secretions from other salivary glands [1,4]. In previous presentations, sialography was attempted and revealed partial visualization of the remaining Wharton's duct with a club-like terminal branch [1].
The etiology of unilateral aplasia of the submandibular gland can be a result of iatrogenic causes (surgical resection), congenital developmental abnormality, or chronic sialolithiasis causing chronic inflammation resulting in atrophy of the involved salivary gland [5]. Thorough physical examination of these patients include: bimanual palpation, inspection of the oral cavity for mucosal dryness, dental caries, and facial anomalies. Imaging of the salivary glands include: plain radiography, Tc-pertechnatate scintigraphy, sialography, ultrasonography (USG), magnetic resonance imaging, computed tomography, and positron emission tomography [6].
Using PET for tumor staging, restaging, monitoring of treatment, and predicting the prognosis in patients with head and neck cancers is clearly established. Due to the variable physiologic uptake of FDG in the head and neck, particularly those of glandular origin, accurate interpretation of PET scans in these patients can be very difficult and can lead to false-positive results [7]. Unilateral aplasia of a salivary gland can result in hypertrophy of the opposite gland [1,8]. Our patient had mild prominence of the remaining submandibular gland as seen on ultrasonography (USG) and this may account for the asymmetrical uptake of FDG on PET/CT imaging. The normal patterns and variability in the extent of tracer uptake is measured in standardized uptake value (SUV). In the submandibular gland, the SUV has been shown to be 2.16 +/- 0.57 in males and 2.06 +/- 0.58 in females [10]. Our patient had a maximal SUV of 2.7 in the remaining right submandibular gland, while the known cancer of the right breast had an SUV of 11.0. Given the unilateral nature of the submandibular gland in our patient and the variable uptake of FDG in salivary glands, a false PET positivity was identified since the uptake was asymmetrical.
In order to evaluate the PET positive submandibular gland, an USG was completed. Due to the superficial position of the major salivary glands, most are accurately accessible by high-resolution transducers. USG is widely available, cost-effective, and safe with the ability to correctly differentiate malignant from benign lesions in 90% of cases. This diagnostic modality is able to distinguish glandular from extraglandular masses with an accuracy of 98% and confirm the clinical suspicion of a mass [11]. If a tumor is suspected, the cervical lymph nodes are also examined. Characteristics of malignant tumors found on USG include lesions with irregular borders, heterogeneous echoic patterns, irregular necrosis, and a higher degree of vascularization [12]. Intraglandular metastases most often present as multiple, round, sharp-bordered lesions, and color Doppler usually displays hypervascularization [13]. Our patient had several benign appearing lymph nodes in the neck and the remaining right submandibular gland was found to possess benign characteristics. Since no discrete masses were seen on USG, a biopsy was not undertaken; additionally, repeat USG in another six months revealed no significant changes. Yanir et al. [14] performed a fine needle aspiration (FNA) in the remaining unilateral submandibular gland with benign features and was found to be acellular.
In conclusion, unilateral submandibular gland aplasia is an extremely rare entity and is usually asymptomatic and has not been associated with other facial developmental abnormalities. Several imaging options are available to assess major salivary glands including USG, MRI, CT, and PET. FDG uptake on PET by the remaining submandibular gland in unilateral submandibular aplasia concerning for metastasis from breast cancer should be evaluated carefully. If the gland appears normal, additional testing may be unnecessary.
Acknowledgements
The authors wish to thank Ryan DeMelo, MD in the Radiology department of University of Missouri-Columbia for his input and evaluation of the PET-Scan.
References
- Yilmaz MD, Yucel A, Derekoy S, Altuntas A (2002) Unilateral aplasia of the submandibular gland. Eur Arch Otorhinolaryngol 259: 554-556.
- Mathison CC, Hudgins PA (2007) Bilateral submandibular gland aplasia with hypertrophy of sublingual glands. Otolaryngol Head and Neck Surg 138: 119- 120.
- Ahmed M, Strauss M, Kassaie A, Shotelersuk V, DeGuzman R (2009) Bilateral submandibular gland aplasia with clinic-radiological mass due to prolapsing sublingual salivary tissue through mylohyoid boutonniere: a case report and review. Dentomaxillofac Radiol 38: 121-124.
- Srinivasan A, Moyer JS, Mukherji SK (2006) Unilateral submandibular gland aplasia associated with ipsilateral sublingual gland hypertrophy. AJNR 27: 2214-2216.
- Koo BS, Lee SW, Lee YM, Lee JD, Koh YW (2009) Sialolithiasis in a stump of Wharton's duct of an aplastic unilateral submandibular gland. Int J Oral Maxillofac Surg 38: 93-95.
- Burke CJ, Thomas RH, Howlett D (2010) Imaging the major salivary glands. Br J Oral Maxillofac Surg 49: 261-269.
- Cook GJ, Fogeman I, Maisley MN (1996) Normal physiological and benign pathological variants of 18-fluoro-2-deoxyglucose positron-emission tomography scanning: potential for error in interpretation. Semin Nucl Med 26: 308-314.
- Shipchandler TZ, Lorenz RR (2008) Unilateral submandibular gland aplasia masquerading as cancer nodal metastasis. Am J Otolaryngol 29: 432-434.
- Gupta N, Palacios E, Barry S (2009) Unilateral submandibular gland aplasia: a rare phenomenon. Ear Nose Throat J 88: 818-820.
- Nakamoto Y, Mitsuaki T, Hammoud D, Christian C, Medhat M O, et al. (2005) Normal FDG distribution patterns in the head and neck: PET/CT evaluation. Radiology 234: 879-885.
- Martinoli C, Derchi LE, Solbiati L, Rizzatto G, E Silvestri, et al. (1994) Color doppler sonography of salivary glands. AJR 163: 933-941.
- Gritzman N, Rettenbacher T, Hollerweger, Macheiner P, E Hübner A (2003) Sonography of the salivary glands. Eur Radiol 13: 964-975.
- Yanir Y, Fleiman G, Cohen-Kerem R (2009) Aplasia of the submandibular gland with compensatory sublingual gland hypertrophy: a case report. Int J Pediat Otorhinolaryngol 4: 77-79. Submit
Citation: Nguyen SB, Paik YS, Khan U, Jorgensen JB (2011) Unilateral Submandibular Gland with False PET Positive Uptake in a Patient with Breast Cancer: Case Report and Review of the Literature. Otolaryngol 1:106. DOI: 10.4172/2161-119X.1000106
Copyright: © 2011 Nguyen SB, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 16258
- [From(publication date): 11-2011 - Oct 06, 2025]
- Breakdown by view type
- HTML page views: 11453
- PDF downloads: 4805