Verroucas Xanthoma of Faucial Pillar -A Case Report
Received: 26-Aug-2013 / Accepted Date: 21-Sep-2013 / Published Date: 28-Sep-2013 DOI: 10.4172/2161-119X.1000144
Abstract
We present a case of Verruciformxanthoma (VX) occurring on faucial pillar of oral cavity. VX is an uncommon benign mucocutaneous lesion of unknown etiology. It usually appears as single or multiple plaques or papules may be raised or flat with verrocous or pappilary rough surface texture, colour varying from reddish pink to yellowish gray, mainly affecting masticatory mucosa, especially gingiva and hard palate. Histologically, VX is characterized by the presence of parakeratinized epithelium with thin rete ridges and connective tissue papillae extending up to the surface. The papillae characteristically consist of foam cells, also called xanthoma cells. We report a case of VX in the faucial pillar which is not been reported in the literature and discuss their clinical and histopathological findings.
Keywords: Faucial pillar, Xanthoma, Foam cells
254124Introduction
Verruciformxanthoma (VX) is an uncommon non inflamatory benign mucocutaneous lesion of unknown etiology and was first described by Shafer in 1971 [1]. Oral VX usually is an isolated lesion occurring on the mastcatory mucosa chifly gingival and hard palate [2]. The characteristic microscopic feature is the accumulation of foam cells (lipid-laden macrophages) in the connective tissue papillae between the epithelial ridges [3]. Excision is the treatment of choice. However, no potential for malignancy has been reported till date [4].
Case Report
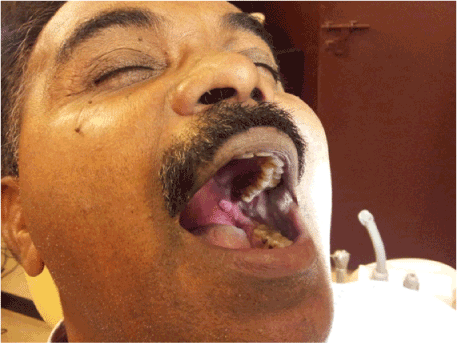
We report a case VX on the left faucial pillar in a 45 year old male patient, he is not a smoker, non alcoholic, no use of tobacco in any form and not suffering from any systemic diseases and not on any medication, the lesion was seen by the patient an year ago (Figure 3), measuring about and it remained of same size even after one year without any symptoms.
On examination rough whitish yellow lesion was noted on the left faucial pillar which was no tender and asymptomatic with rough texture, based on the case history and examination provisional diagnosis of xanthoma was given and as the lesion was small in size excision of the lesion was advised and the specimen was subjected to histopathalogical examination.
Histologically
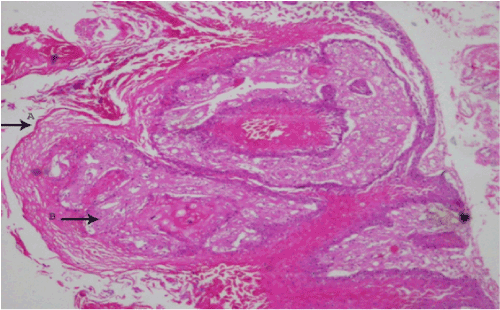
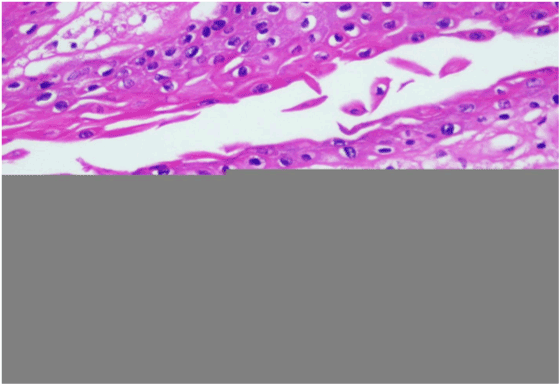
H&E stained section shows epithelium overlying connective tissue stroma. The epithelium is stratified squamous parakeratinized type with flakes of keratin present in focal areas. At the margins the epithelium is thin and atrophic, while at the centre it is hyperplastic showing varying thickness with exophytic finger like papillary projections and acanthotic rete processes in the connective tissue papilla. Focal areas of the epithelium are edematous and show spongiosis with loss of cohesiveness of epithelial cells. The connective tissue papilla contains numerous foamy histiocytes with centrally placed nuclei and granular cytoplasm resembling xanthoma cells which are restricted only to the connective tissue papilla. Just beneath the epithelium nodular areas of chronic inflammatory cells predominantly lymphocytes & plasma cells are seen. The deeper connective tissue stroma is fibrillar with endothelial lined blood vessels and minor salivary glands.
H and E stained section shows epithelium covered by thickened layer of parakeratin with distinctive orange coloration. The connective tissue papillae contained numerous large macrophages with foamy cytoplasm. The overall histopathological features is suggestive was of Verruciform Xanthoma (Figure 1 and 2).
Discussion
VX is an uncommon benign mucocutaneous lesion of unknown etiology. It usually appears as single or multiple plaques or papules may be raised or flat with verrocous or pappilary rough surface texture, colour varying from reddish pink to yellowish gray, mainly affecting masticatory mucosa, especially gingiva and hard palate, and size may vary from 0.2 to 2 cm [5]. There is no gender predilection and most commonly occurs in middle-aged persons with mean age of 40–50 years.
Although in most cases VX tends to occur as an isolated lesion, sometimes it may be associated with erythema multi forma, psoriasis, discoid lupus erythmatosis, lichen planus, graft versuas host diseases, solar keratosis, carcinoma in situ and snuff/tobacco users [6-8].
Multifocal cases of VX involving the upper aero digestive tract have been also reported in a patient with systemic lipid storage disorder [9] possible oral etiologic agents such as wet microenvironment, periodontal pathogens, mechanical stimuli, tobacco, alcohol, drugs, and sensitizing or allergic substances of foodstuffs and dental materials. Viral infection could be associated with the lesion; however, studies have been done with no association found with human papillomavirus. Immune response was also related to VX pathogenesis [10].
Oral mucosal manifestations of chronic Graft Versus Host Diseases (GVHD) are common and include reticular/hyperkeratotic striations and plaques, erythema and ulcerations [11].
Histopathologically, lesions of VX may be flat or slightly raised with a papillomatous or verrucous surface composed of parakeratinized epithelial cells. Elongated epithelial rete ridges extend into the lamina propria at a uniform level or depth. The most characteristic feature is the presence of numerous foam or xanthomatous cells within lamina propria or connective tissue papillae [5]. Sah et al. suggested that the epithelial hyperplasia, elongation of the epithelial rete ridges is illusory. It is not a downward proliferation of epithelial cells but rather results from the upward thursting effect of accumulated macrophages towards the surface epithelium. Hence, it reflects thinning of the epithelium overlying the macrophages in the connective tissue papillae [4].
Xanthomas represent the accumulation of lipid-rich histiocytes (macrophages) known as foam cells. It has also been suggested that degenerative changes in the epithelium lead to the presence of foam cells [12].
Immune reaction associated with matrix metaloprotiens (MMP2&9) has been reasoned for accumulation of foam cells, which degrade basal membrane of the epithelium and promote a reciprocal induction between the mesenchymal and epithelial cells [2].
Three histological subtypes (types A, B, and C) have been described based on the texture of the surface epithelium. Lesions of the verrucous type (A) have hyperparakeratosis, acanthosis, and elongation of the rete ridges. The papillary form (B) has many finger-like projections composed of stratified squamous epithelium containing connective tissue cores. In the flat type (C), mild acanthosis and subtle thin parakeratosis with variable elongation of rete ridges are commonly observed [9,13] (Figure 1 and 2).
Because of the severity of surface keratinization, its color may vary from white to red. Therefore, oral VX may resemble a squamous papilloma, verruca vulgaris, or a mucosal fibroma. These entities do not contain lipid-laden macrophages and they exhibit varying degree of koilocytic change, which are known to be absent in VX. Because of its verrucous nature, verrucous carcinoma should be also added to the list of differential diagnoses and can be distinguished by the presence of invasive epithelial proliferation, cellular atypia, and the lack of foamy histiocytic infiltrate [2,8]. VX is usually treated by a conservative excision. To date, only three cases of recurrence have been reported [2,9].
Conclusion
VX is a multi factorial chronic reactive lesion. The clinical diagnosis may be challenging; however, the histological features are diagnostic and well defined. Its recognition and correct diagnosis is critical because VX can occur in conjunction with systemic and cutaneous inflammatory diseases and to reduce the anxiety in healthy individuals.
References
- Shafer WG (1971) Verruciform xanthoma. Oral Surg Oral Med Oral Pathol 31: 784-789.
- Mete O, Kurklu E, Bilgic B, Beka H, Unur M (2009) Flat type verruciformxanthoma of the tongue and its differential diagnosis. Dermatol Online 15: 5.
- Oliveira PT, Jaeger RG, Cabral LA, Carvalho YR, Costa AL, et al. (2000) Verruciformxanthoma of the oral mucosa. Report of four cases and a review of literature. Oral Oncol 37: 326-331.
- Sah K, Kale AD, Hallikerimath S (2008) Verruciform xanthoma:Report of two cases and review on pathogenesis. J Oral MaxillofacPathol 12: 41-44.
- Hatakeyama M, Alonso J, Guilhermino M, Brandao AA, Sueli A, et al. (2010) Verruciformxanthoma located in anterior gingival. J ClinExp Dent 2: 82-84.
- Regezi, Scuibba Oral pathology: Clinical pathological correlation. 1stedn. pp. 180-82.
- Neville BW, Damm DD, Allen CM, Bouquat JE (2002) Oral and maxillofacial pathology. 2nd ed. Lajpat Nagar, New Delhi: Saunders (An imprint of Elseviers).
- Shafer, Hine, Levy Shaefer's textbook of oral pathology. 6thedn. Noida, India: Elsevier; p. 139.
- Travis WD, Davis GE, Tsokos M, Lebovics R, Merrick HF, et al. (1989) Multifocal verruciform xanthoma of the upper aerodigestive tract in a child with a systemic lipid storage disease. Am J Surg Pathol 13: 309-316.
- Ide F, Obara K, Yamada H, Mishima K, Saito I, et al. (2008) Cellular basis of verruciform xanthoma: Immunohistochemical and ultrastructural characterization. Oral Dis 14: 150-157.
- Treister NS, Cook EF Jr, Antin J, Lee SJ, Soiffer R, et al. (2008) Clinical evaluation of oral chronic graft-versus-host disease. Biol Blood Marrow Transplant 14: 110-115.
- Wall V, Kwast W (1988) Oral Pathology. 1stedn, West Germany: Quintessence Publishing Co. p. 39.
- Philipsen HP, Reichart PA, Takata T, Ogawa I (2003) Verruciformxanthoma-biological profile of 282 oral lesions based on a literature survey with nine new cases from Japan. Oral Oncol 39: 325-336.
Citation: Sathish R, Suhas S, Chandra Shekar L, Praveen K S, Ganeshan S, et al. (2013) Verroucas Xanthoma of Faucial Pillar -A Case Report. Otolaryngology 3:144. DOI: 10.4172/2161-119X.1000144
Copyright: © 2013 Sathish R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 15338
- [From(publication date): 11-2013 - Dec 23, 2025]
- Breakdown by view type
- HTML page views: 10584
- PDF downloads: 4754