Research Article Open Access
In Vivo Btc-2000™ Measurement of Anterior Vaginal Wall Biomechanical Properties in Prolapse Patients Undergoing Surgical Repair
Elizabeth Mosier1, Rachel Jerome1, Xian-Jin Xie1, Charles CJ Chuong2, J Yan1, Robert C Eberhart2,3 and Philippe E Zimmern1*1Department of Urology, University of Texas Southwestern Medical Center, Dallas, Texas, USA
2Department of Bioengineering, University of Texas at Arlington, Arlington, Texas, USA
3Department of Surgery, University of Texas Southwestern Medical Center, Dallas, Texas, USA
- Corresponding Author:
- Philippe E. Zimmern, MD
UT Southwestern Medical Center, TX, USA
Tel: 214-648-9397
E-mail: philippe.zimmern@utsouthwestern.edu
Received date: November 10, 2011; Accepted date: December 05, 2011; Published date: December 07, 2011
Citation: Mosier E, Jerome R, Xie XJ, Chuong CCJ, Yan J, et al. (2011) In Vivo Btc-2000™ Measurement of Anterior Vaginal Wall Biomechanical Properties in Prolapse Patients Undergoing Surgical Repair. J Biotechnol Biomaterial 1:117. doi:10.4172/2155-952X.1000117
Copyright: © 2011 Mosier E, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Biotechnology & Biomaterials
Abstract
A non-invasive device, the BTC-2000™, used for skin biomechanical measurements, was adapted for vaginal measurements of prolapsed patients, and tested for intra (IaR) and inter-tester (IrR) reliability, in preparation for a clinical measurement series. Following IRB approval, women aged 35 - 85 with symptomatic stage 2-3 anterior vaginal wall prolapse requiring surgical repair were consented. Twenty four consecutive patients were studied. Under anesthesia, the BTC-2000™ with a 10 mm diameter aperture and a suctioning pressure of 150 mmHg was applied to the anterior vaginal wall below the bladder neck, first with the bladder empty and then filled to 300ml. External, suprapubic measurements were taken as controls. All biomechanical parameters displayed by the instrument were assessed for reliability, including: Laxity (mm/%), Elastic Deformation (mm), Modulus (MPa), Energy Absorption (KPa), and Elasticity (mm). Measurements were made in duplicate by the primary surgeon and a separate, randomly chosen tester. Intra-class correlation coefficient (ICC) was calculated to determine IaR and IrR. The feasibility and reliability of all BTC-2000™ measurements was established for this new application. The calculated biomechanical parameters were not statistically different at the two bladder volumes. ICC calculations showed first and second data collections for both IaR and IrR were not statistically different. ICC IaR values were 0.6 or higher, supporting the claim of reliability. IaR and IrR values for the series of secondary testers were less reliable. Demonstrated feasibility and primary operator reliability pave the way for the first detailed in vivo studies of biomechanical properties in this setting.
Keywords
Pelvic organ prolapsed; In vivo biomechanical testing; Measurement reliability
Abbreviations
POP – pelvic organ prolapsed, IrR – inter-rater reliability, IaR – intra-rater reliability, ICC – intra-class correlation coefficient
Introduction
Anterior vaginal wall prolapse, or cystocele, involves descent of the bladder into the vagina, a common form of pelvic organ prolapse (POP) [1-3]. Characterization of the extent of prolapse and the quality of the vaginal tissues is primarily based on physical examination and imaging studies. Typically, vaginal examination is conducted in supine, lateral decubitus, sitting (birthing chair), or standing position. The technique of standing voiding at standardized bladder volumes (cystourethrogram) has allowed reliable grading of cystocele severity, assessment of the size of the hernia defect, and measurement of urethral mobility [1]. This methodology might be extended to provide a more objective documentation of the overall results of bladder prolapse repair [2]. But it tells little about the mechanical properties of the affected tissues, analyses that might permit more convenient preoperative and postoperative assessments. Imaging (pelvic floor MRI and ultrasound) has been recommended to further elucidate levator tears after delivery, as they can be responsible for POP development later in life [3].
Detailed modeling of pelvic anatomy, including vaginal structure and function requires knowledge of tissue mechanical properties. Direct human vaginal tissue data stems from cadaver studies, or from tissue samples harvested in the operating room. Harvested samples from patients are either frozen and then analyzed after thawing [3-4] or, as recently described, tested within two hours of harvest [5]. These techniques rely on a segment of vaginal wall removed at the time of surgery, an important limitation. The information gleaned cannot be part of pre-operative surgical planning (the decision for primary suture repair or mesh interposition), nor can it be used to track disease progression to operation, or postoperative healing.
A direct, in vivo means for quantitative, reproducible evaluation of vaginal wall tissue characteristics could prove useful in surgical decision making [6,7] or in other phases of patient management. For example, such a technology could permit early detection of vaginal tissue breakdown prior to the full development of POP, the monitoring of vaginal tissue changes with aging, or even as a monitor of the healing process. If tissue weakness were detected early on, preventive measures could be considered, to improve pelvic floor tone, limit weight gain, avoid straining factors such as chronic constipation, and maintain adequate hormonal milieu. The effectiveness of such measures could be tested, and thus might prevent or delay the need for reconstructive surgeries later on in life. In short, such a tool could prove very useful clinically, at several levels, for POP prevention, monitoring, and management.
Accordingly, the initial goal of our study was to test the feasibility and reliability of vaginal tissue measurements obtained with a non-invasive device, the BTC-2000™. This instrument was originally applied in plastic surgery to measure skin elasticity. One rationale for adap- tation of this instrument to the pelvic region is the involved pressure excursion range, 150 mm Hg, similar to physiological excursions, e.g., cough, Valsalva, etc. Because this application has not yet been reported, we applied a strict methodology, using repeated intra- and inter-tester measurements at different bladder volumes. To allow repetitive measurements and avoid patient discomfort, a controlled operating room environment was selected, namely the patient under general anesthesia, at the start of the surgical procedure, thereby to minimize any effect of anesthesia on tissue relaxation. Verifications of reliability and reproducibility are necessary to qualify the technology for a new clinical application and subsequent incorporation into multi-centric epidemiological and surgical studies.
Materials and Methods
Women aged 35 to 85 with symptomatic and radiographically-confirmed stage 2 or 3 anterior vaginal wall prolapse requiring surgical repair were consented to participate in this IRB approved study. After induction of general anesthesia and placement in the lithotomy position, a 16 French urethral Foley catheter was placed to drain the bladder. The BTC-2000™ (SRLI Technologies, Nashville TN) was prepared beforehand by wiped down with alcohol solution. The BTC-2000™ probe consists of a trapezoidal hollow glass chamber with a 10 mm diameter aperture at the apex (Figure 1a). A removable sticky pad is placed at the aperture to enhance tissue adhesion and limit air leaks during the ensuing suctioning process. A red laser beam is generated in the probe base and directed to the center of the aperture. The beam reflection from the targeted tissue is directed to a detector in the probe base. Distension of the tissue into the aperture is measured by triangulation of the reflected beam. The centered laser beam appears as a red spot on the tissue during positioning (Figure 1b). A portion of the reflected beam can be observed at the tissue surface during the subsequent test, to ensure stable positioning is maintained. A pump connected to the chamber delivers a modest suction pressure, programmed to increase linearly with time and to reach 150 mmHg in 6 seconds. The suction profile causes a timedependent distension of the exposed tissue into the chamber, during which time the laser triangulation is performed at a 10 Hz repetition rate. The negative pressure in the chamber is then released; during this 2 second period, laser-based measurement of residual distension continues as the tissue returns to, or near, baseline. Measurement of tissue relaxation during this period allows an estimate of viscoelastic properties, simulating early creep behavior. Representative curves are shown in Figure 2.
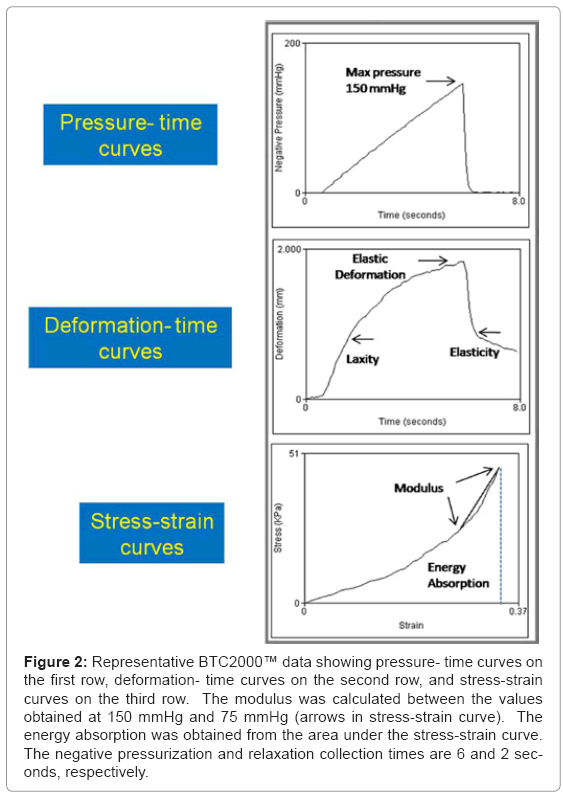
Figure 2: Representative BTC2000™ data showing pressure- time curves on the first row, deformation- time curves on the second row, and stress-strain curves on the third row. The modulus was calculated between the values obtained at 150 mmHg and 75 mmHg (arrows in stress-strain curve). The energy absorption was obtained from the area under the stress-strain curve. The negative pressurization and relaxation collection times are 6 and 2 seconds, respectively.
Although other studies have chosen the face or the forearm as controls, we elected, for this new application, to test the suprapubic skin (one fingertip above the pubic bone, midline region), as it was conveniently available adjacent to the operative field. After control measurements, we tested the anterior vaginal wall just below the bladder neck area, a location easy to recognize by palpation of the balloon of the urethral Foley catheter inflated with 10 cc of water. This location was the only part of the prolapsed anterior vagina that was reproducible between patients. Using the most protruding (bulging) portion of the prolapsed wall would have resulted in too much measurement location variability between patients. Because of the possibility of variations in measurements due to partial distension of the bladder, we performed all our testing cycles with the bladder empty and then filled to 300ml. All measurements were made both by the primary surgeon and by a separate tester. This tester, with no training experience with the device, was chosen at random in the operating room (typically a resident, an operating room nurse, or a medical student).
For both the vaginal and control locations, the data derived from the tissue distension measurements consisted of Laxity (mm/%), Elastic Deformation (mm), Modulus (MPa), Energy Absorption (KPa), and Elasticity (mm/%). We chose to evaluate all these parameters, as there was no a priori cause for exclusion of any one of them. These manufacturer-specified parameters [11] are defined as follows. Laxity is the percentage (%) of acute elastic deformation (mm) that occurs with “very low” pressure or stress. It is defined by a change in the slope of the pressure vs. deformation curve (akin to stress vs. strain, since the baseline aperture area is defined). Elastic deformation (mm) is the amount of deformation obtained at the point of the maximum suction pressure. Modulus is calculated as the slope of the linear portion of the stress vs. strain curve. Energy absorption is the total area beneath this curve (meaning stress vs. strain curve). Elasticity (mm) is the amount of elastic recovery (relaxation of deformation) that occurs immediately upon release of negative pressure: these data are directly compared with the acute elastic deformation to determine the percent elasticity (%).
Intra-rater reliability (IaR) is the degree of agreement among multiple repetitions of a diagnostic test performed by a single rater. Interrater reliability (IrR) is the degree of agreement among different raters. The ICC describes how strongly units in the same group resemble each other, and is used to assess consistency or reproducibility of quantitative measurements made by different observers measuring the same quantity. The Intra-class correlation coefficient (ICC) was calculated to determine IaR and IrR using PASW Statistics Base 17.0 for Windows® [10]. A twenty four patient consecutive cohort was chosen as a convenience sample. A possible “training effect” was tested by comparing the data obtained by the primary surgeon for the first twelve patients and the last twelve (data not shown). Also the effect of age was assessed by calculating a coefficient of variation from the two measurements for each patient and for each variable. Then for each variable, Pearson correlation between this coefficient of variation and age was calculated among the patients.
Results
Twenty-four consecutive patients, the majority being Caucasian (88%) with a mean age (58 ± 17), BMI (26 ± 5) and parity (2 ± 1) were studied. None had prior surgery for prolapse repair. One of 24 primary tester’s attempted vaginal wall measurements failed, due to inability to seal the probe orifice and thus obtain suction when the bladder was full. Two of 24 secondary tester’s attempts failed; one for the same full bladder case and another for an empty bladder case. There were no suprapubic measurement failures.
Table 1 presents the biomechanical result means obtained by the primary tester, tabulated separately for the first and repeat measurements. There were no significant differences in any measurement, at any site. Table 2 compares the primary (IaR) and secondary (IrR) tester’s results, reported as mean values for each location. Again, there were no significant differences in any measurement, at any site. Table 3 presents all ICC mean values for the primary tester. If we take ICC values greater than 0.6 as the threshold for reliable results [14], all but one suprapubic measurement parameter (the modulus) are reliable. By the same criterion the IaR empty bladder vaginal measurements were reliable (the modulus value again excluded). The IaR ICC values for the “filled” bladder measurements declined somewhat, excepting the modulus and elasticity values, suggesting empty bladder measurements are more reliable than “full” bladder measurements. Table 4 presents secondary tester (IrR) ICC values. The numbers are lower across the board, save for suprapubic modulus values, suggesting less reliability by the 0.6 ICC threshold criterion. The 95% confidence intervals for the mean values in Tables 1-4 are broad, but less so for the IaR data than the IrR data. Taking these results together, we claim reliable measurements were obtained by the primary tester; the claim is less certain for the secondary testers. There was no significant change in ICC results for IaR for the first twelve patients tested versus the second twelve, thus arguing against a significant learning curve for the primary tester (data not shown). Intra-rater results for the empty bladder modulus were positively related to age (p <0.03; data not shown).
Discussion
This study established the feasibility and the reliability and reproducibility of a relatively new technology, currently used predominantly in the field of plastic surgery, for in vivo biomechanical prolapsed tissue measurements. These steps were considered critical before embarking on more elaborate clinical pelvic organ studies. Although a null hypothesis was not specified, showing no difference between the frequency of readings and readers on 24 patients provides meaningful evidence that major differences are not likely to exist. Without such an initial investigation, it would be premature to establish a reasonable ‘effect size’ for hypothesis testing.
The ICC is used to assess the consistency, or conformity, of measurements made by multiple observers measuring the same quantity [8]. Thus the ICC fit our data scenario very well in measuring the interrater and intra-rater correlations. A single measure random effect model was used for calculating the ICC [9]. Negative values for ICC at the 95% confidence interval were observed as shown in Table IV. Given the sample size of 17 and the method of interval calculation in this instance, it is acceptable that the lower bound of the 95% confidence interval is negative [10].
A similar instrument, the Cutometer® (Courage & Khazaka Electronics GmbH, Cologne, Germany) is used in dermatologic research for the evaluation of skin elasticity. The reliability of the Cutometer® has been tested on normal skin [12] and on patients with scleroderma lesions [13]. There are several other clinical reports of the use of the Cutometer® or cutometer-like devices to examine eyelid laxity, laser resurfacing, burns and scar formation and other skin conditions [11].
Use of a cutometer-like device has been reported in prior pelvic organ prolapse studies. In one study the DermaLab USB skin probe (Cortex Technology, Hadsund, Denmark) was applied to the left vaginal sidewall, 2cm proximal to the hymeneal remnant. Measurements were performed before and 6 weeks after sacrocolpopexy by the same operator, not blinded to the pre or post-operative status of the patient [6]. Another study from the same group compared two probes, the Cutometer ® MPA versus the Dermalab USB, both with 2 mm apertures. Three cycles were used for each measurement but again, all tests were done by the same tester without information on intra-rater reliability [10]. Intra- and inter-rater reliability were tested in the study of skin scarring with the Cutometer® MPA 580 [12]. No data relating to reproducibility of vaginal wall measurements were mentioned in this report.
The BTC-2000™ relies on mild suction, applied for a short period of time to achieve a modest deformation of tissue. It is thus unlikely to induce disruptive tissue changes. It is akin to a physiological vaginal stressor, like a Valsalva abdominal straining effort. Prior studies on skin diseases have reported on its safety and lack of pain during the measurements [12,13], observations that could not be confirmed in this study, as it was done under anesthesia.
Regarding feasibility, the probe used in this study was easy to handle. But because of its size, it could not be pushed inside the vagina, thus limiting its usefulness to patients with prolapse coming to or outside the vaginal introitus. The probe aperture was set at 10 mm. Other probe aperture sizes (2mm and 6mm) have been reported in prior studies [7]. The probe needs to be placed in direct contact with the vaginal wall. The vagina has to be kept dry to avoid losing the required seal effect during suctioning. Our original concern had been that the pressure of the probe needed to hold the device in place during each measurement would induce great variability, making the measurements unfeasible, but it did not. Also, the instrument protocol supports proper application of the probe: unless there is good suction pressure in the glass chamber, the device will not perform the prescribed measurement. If the seal is lost (as determined by the pressure profile), the laser is turned off, immediately interrupting the measurement. The whole process must be restarted, since partial tracings are not kept in computer memory. Thus BTC-2000™ operation guarantees that a consistent negative pressure history is provided throughout the 8 second event period. We feel that this “all or none” feature allowed fairly consistent recordings, and adds to the feasibility of the measurements.
We adopted a strict methodology for all patients, including general anesthesia to avoid the patient anxiety factor, and a precise location of the probe so that the study could be made reproducible. One could argue that the measurements should have been made at the point of maximum prolapse protrusion. However, such a location would have varied from patient to patient and might also be influenced by bladder distension. Therefore, for purpose of standardization, the measurements were taken from the anterior vaginal wall at a consistent location, just below the level of the bladder neck area, a site easily identified by all testers, and based on the location of the Foley balloon. The balloon was not placed in tension at the time of measurement, to avoid interfering with the measurements.
Table 1 summarizes all the data for the same tester, a critical step before assessing the inter-operator variability (Table 2). The intra-class correlation coefficient is the preferred statistical test to assess the scatter effect or measurement variability when testing a new device. The closer the ICC value to 1, the lesser the observed scatter and the more reliable the device measurement. Although there is no accepted cutoff value for ICC-based reliability determinations, we elected to follow the recommendation of Streiner. “we should expect that correlations among measures of the same attribute should fall into midrange of 0.4- 0.8”. The main limitation of the ICC method is its dependence on the variance of the population. If the population is homogeneous as sug-gested in this case, e.g., patients presenting for surgery, ICC values may be expected to be lower. Heterogeneous populations, e.g., all women in the age range, irrespective of disease, may be expected to yield higher ICC values on the basis of a broader range of parameter values. Thus we chose to apply an ICC value of 0.6 as the threshold for reliability. The IaR values (Table 3) met this criterion. The IrR values were lower, but still fell in the range cited. It is reasonable to expect that learning curves would exist for the independent raters, and thus ICC values would be lower than those obtained by the primary rater.
| IaR | n | Maximum Pressure (mmHg) | Laxity (mm) | Percent Laxity (%) | Elastic Deformation (mm) | Modulus (MPa) | Energy Absorption (KPa) | Elasticity (mm) | Percent Elasticity (%) |
| Supra Pubic 1 | 24 | 147.6 ±1.0 | 147.6 ±1.0 | 74.7 ±17.5 | 2.0 ± 0.5 | 0.30 ± .08 | 5.5 ± 1.3 | 1.2 ± 0.6 | 55.5 ±16.9 |
| Supra Pubic 2 | 147.5±0.9 | 1.5 ± 0.5 | 77.7 ± 11.2 | 1.9 ± 0.4 | 0.35 ± 0.11 | 5.0 ± 1.4 | 1.2 ±0.5 | 61.2 ± 15.4 | |
| Empty Bladder 1 (0 ml) | 147.8 ± 1.0 | 1.4 ± 0.7 | 53.7 ± 14.1 | 2.4 ± 1.0 | 0.14 ± 0.07 | 9.9 ± 3.4 | 0.6 ± 0.3 | 28.7 ± 5.3 | |
| Empty Bladder 2 (0 ml) | 147.8 ± 1.0 | 1.4 ± 0.7 | 53.7 ± 14.1 | 2.4 ± 1.0 | 0.14 ± 0.07 | 9.9 ± 3.4 | 0.6 ± 0.3 | 28.7 ± 5.3 | |
| Filled Bladder 1 (300 ml) | 22 | 147.6 ± 0.7 | 1.5 ± 0.8 | 58.2 ± 14.1 | 2.5 ± 1.0 | 0.15 ± 0.08 | 9.7 ± 3.8 | 0.6 ± 0.2 | 28.6 ± 13.2 |
| Filled Bladder 2 (300 ml) | 147.4 ± 0.9 | 1.1 ± 0.5 | 54.4 ± 11.8 | 1.9 ± 0.8 | 0.18 ± 0.08 | 7.8 ± 3.2 | 0.6 ± 0.2 | 36.5 ± 15.3 |
Table 1: Data from BTC-2000™ for Intra Rater Reliability (IaR). Each measurement reported is the mean of all the measurements, with standard deviation, in that location.
| IaR vs IrR | n | Maximum Pressure (mmHg) | Laxity (mm) |
Percent Laxity (%) | Elastic Deformation (mm) | Modulus (MPa) | Energy Absorption (KPa) | Elasticity (mm) | Percent Elasticity (%) |
| IaR | |||||||||
| Supra Pubic | 24 | 147.5 ± 0.9 | 1.5 ± 0.5 | 76.2 ± 13.4 | 2.0 ± 0.4 | 0.33 ± 0.09 | 5.3 ± 1.3 | 1.2 ± 0.5 | 58.3 ± 15.4 |
| Empty bladder (0 ml) | 24 | 147.7± 0.9 | 1.2 ± 0.7 | 53.3 ± 12.1 | 2.2 ± 1.0 | 0.16 ± 0.07 | 8.9 ± 3.2 | 0.6 ± 0.2 | 33.0 ± 14.8 |
| Filled bladder (300 ml) | 23 | 147.5 ± 0.7 | 1.2 ± 0.6 | 55.4 ± 11.0 | 2.2 ± 0.9 | 0.16 ± 0.08 | 8.7 ± 3.2 | 0.6 ± 0.2 | 32.5 ± 13.8 |
| IrR | |||||||||
| Supra Pubic | 20 | 147.4 ± 0.7 | 1.5 ± 0.4 | 77.4 ± 9.8 | 2.0 ± 0.5 | 0.33 ± 0.11 | 5.2 ± 1.8 | 1.2 ± 0.5 | 62.2 ± 14.2 |
| Empty bladder (0 ml) | 17 | 147.4 ± 0.3 | 1.1 ± 0.8 | 55.5 ± 14.6 | 1.8 ± 1.0 | 0.20 ± 0.09 | 7.0 ± 3.0 | 0.6 ± 0.3 | 39.0 ± 15.0 |
| Filled bladder (300 ml) | 17 | 147.2 ± 0.5 | 1.2 ± 0.7 | 53.6 ± 11.8 | 2.1 ± 0.8 | 0.17 ± 0.10 | 8.3 ± 2.9 | 0.6 ± 0.2 | 35.7 ± 14.8 |
Table 2: Comparison of BTC-2000™ measurements between the primary surgeon (IaR) and another tester chosen at random in the operating room (IrR). Each measurement reported is the mean of measurements, with standard deviation, in that location.
| Intra Rater Reliability (IaR) | Laxity | Elastic Deformation | Modulus | Energy Absorption | Elasticity | |
| Supra Pubic (N = 24) | ||||||
| ICC | Estimate (95% CI) | 0.82 (0.63, 0.92) | 0.83 (0.65, 0.92) | 0.58 (0.24, 0.79) | 0.82 (0.64, 0.92) | 0.91 (0.80, 0.96) |
| Empty Bladder (N = 23) | ||||||
| ICC | Estimate (95% CI) | 0.68 (0.39, 0.85) | 0.75 (0.50, 0.89) | 0.50 (0.13, 0.75) | 0.65 (0.34, 0.83) | 0.78 (0.56, 0.90) |
| Filled Bladder 300mL (N = 22) | ||||||
| ICC | Estimate (95% CI) | 0.57 (0.21, 0.79) | 0.67 (0.36, 0.85) | 0.78 (0.55, 0.90) | 0.60 (0.26, 0.81) | 0.84 (0.66, 0.93) |
Table 3: ICC values for intra-rater (IaR) reliability measurements, including 95% confidence intervals (CI).
Tables 3 and 4 indicated higher ICC values overall for intra-rater than for inter-rater measurements. Therefore, based on the reported findings, we have chosen at our center to use the data from the same operator in future studies, with occasional quality control evaluation with duplicate measurements performed from time to time. Also, to simplify the procedure, all our measurements are now done with an empty bladder, since there was very little data difference between empty and full bladder. A likely explanation for this observation is that the vaginal wall deformation induced by the suction device is very superficial, affecting only 1-1.5 mm, as shown by the laxity data.
| Inter Rater Reliability (IrR) | Laxity | Elastic Deformation | Modulus | Energy Absorption | Elasticity | |
| Supra Pubic (N = 19) | ||||||
| ICC | Estimate (95% CI) | 0.51 (0.09, 0.77) | 0.59 (0.21, 0.82) | 0.78 (0.52,0.91) | 0.68 (0.34, 0.86) | 0.69 (0.37, 0.87) |
| Empty Bladder (N = 17) | ||||||
| ICC | Estimate (95% CI) | 0.62 (0.23, 0.84) | 0.52 (0.08, 0.79) | 0.47 (0.01, 0.77) | 0.41 (-0.07, 0.73) | 0.81 (0.55, 0.92) |
| Filled Bladder 300mL (N = 17) | ||||||
| ICC | Estimate (95% CI) | 0.42 (-0.05,0.74) | 0.42 (-0.04, 0.74) | 0.67 (0.31, 0.87) | 0.38 (-0.09, 0.72) | 0.67 (0.30, 0.86) |
Table 4: ICC values for inter-rater (IrR) reliability measurements, including 95% confidence intervals (CI).
Several additional technical issues are worth reviewing, although their impact on results is not clearly defined at this stage. Differences in aperture have been studied before with 2, 6 and 10 mm aperture probes [11,14]. It is not known if the findings differ or are comparable between a large aperture size, theoretically allowing more tissue deformation with suctioning, or a smaller one. We chose to use only the 10mm aperture, as it is the largest available, enabling surveillance of the deepest possible tissues deemed important for purposes of measurement reliability. Localization of tissue measurements (lateral vaginal wall as opposed to the more elastic anterior vaginal wall where the disease progresses) may also provide differing information. Likewise, whether a reference point allowing calculation of a ratio to compare patients in between themselves is necessary and if so which location to choose remains debatable. We found that the suprapubic region was easy to measure and very reliable. As observed in skin diseases, decay in tissue elasticity with age could have affected our results. However, the only statistically significant positive correlation with age was noted for the modulus with an empty bladder. Another operational choice would be to use the device in the time vs. strain mode, when an increasing or decreasing vacuum is applied for a chosen period, as opposed to the fixed time, linearly increasing vacuum pressure employed in this study. Manipulation of the two modes of operation would enable broader probing of the viscoelastic properties of the tissue.
It is important to point out that this study is not normative, since a normal control group cannot be studied with the current probe. It has only to do with the reproducibility of measurements under specific conditions, at well-specified measurement sites, that can be reproduced by other investigators using the same commercially available instrument. Refinements in the probe shape, and operational characteristics of the device will be needed before it can be applied to patients with no or limited prolapse, or in older patients with a narrow vaginal opening.
In summary, biomechanical measurements on the human prolapsed anterior vaginal wall with the BTC-2000™ instrument were shown to be feasible on a large series of patients undergoing cystocele repair. Intra-operator variability was sufficiently low that reliability was established. Demonstrated feasibility and primary operator reliability pave the way for more detailed in vivo studies of biomechanical properties in this setting.
Acknowledgements
We would like to extend our sincere appreciation to Dr. Spencer Brown, Matt Ruff, and Angela Smith from the UTSW Plastic Surgery Department for the use of the BTC-2000™.
References
- Showalter PR, Zimmern PE, Roehrborn CG, Lemack GE (2001) Standing cystourethrogram: an outcome measure after anti-incontinence procedures and cystocele repair in women. Urology 58: 33-37.
- Gilleran JP, Zimmern P (2009) Abdominal mesh sacrocolpopexy for recurrent triple-compartment pelvic organ prolapse. BJU Int 103: 1090-1094.
- Cosson M, Lambaudie E, Boukerrou M, Lobry P, Crépin G (2004) A biomechanical study of the strength of vaginal tissues. Results on 16 post-menopausal patients presenting with genital prolapse. Eur J Obstet Gynecol Reprod Biol 112: 201-205.
- Goh JT (2002) Biomechanical properties of prolapsed vaginal tissue in pre- and postmenopausal women. Int Urogynecol J Pelvic Floor Dysfunct 13: 76-79
- Zimmern PE, Eberhart RC, Bhatt A (2009) Methodology for biomechanical testing of fresh anterior wall vaginal samples from postmenopausal women undergoing cystocele repair. Neurourol Urodyn 28: 325-329.
- Epstein LB, Graham CA, Heit MH (2008) Impact of sacral colpopexy on in vivo vaginal biomechanical properties. Am J Obstet Gynecol 199: 664 e1-6.
- Epstein LB, Graham CA, Heit MH (2007) Systemic and vaginal biomechanical properties of women with normal vaginal support and pelvic organ prolapse. Am J Obstet Gynecol 197: 165 e1-6.
- Shrout PE, Fleiss JL (1979) Intraclass correlations: uses in assessing rater reliability. Psychol Bull 86: 420-428.
- McGraw KO, Wong SP (1996) Forming inferences about some intraclass correlation coefficients. Psychological Methods 1: 30-46.
- PASW Statistics Base 17.0 for Windows®.
- Koch RJ, Cheng ET (1999) Quantification of skin elasticity changes associated with pulsed carbon dioxide laser skin resurfacing. Arch Facial Plast Surg 1: 272-275.
- Draaijers LJ, Botman YA, Tempelman FR, Kreis RW, Middelkoop E (2004) Skin elasticity meter or subjective evaluation in scars: a reliability assessment. Burns 30: 109-114.
- Enomoto DN, Mekkes JR, Bossuyt PM, Hoekzema R, Bos JD (1996) Quantification of cutaneous sclerosis with a skin elasticity meter in patients with generalized scleroderma. J Am Acad Dermatol 35: 381-387.
- Hendriks FM, Brokken D, Oomens CW, Bader DL, Baaijens FP (2006) The relative contributions of different skin layers to the mechanical behavior of human skin in vivo using suction experiments. Med Eng Phys 28: 259-266.
Relevant Topics
- Agricultural biotechnology
- Animal biotechnology
- Applied Biotechnology
- Biocatalysis
- Biofabrication
- Biomaterial implants
- Biomaterial-Based Drug Delivery Systems
- Bioprinting of Tissue Constructs
- Biotechnology applications
- Cardiovascular biomaterials
- CRISPR-Cas9 in Biotechnology
- Nano biotechnology
- Smart Biomaterials
- White/industrial biotechnology
Recommended Journals
Article Tools
Article Usage
- Total views: 16900
- [From(publication date):
December-2011 - Dec 05, 2025] - Breakdown by view type
- HTML page views : 12103
- PDF downloads : 4797