Make the best use of Scientific Research and information from our 700+ peer reviewed, Open Access Journals that operates with the help of 50,000+ Editorial Board Members and esteemed reviewers and 1000+ Scientific associations in Medical, Clinical, Pharmaceutical, Engineering, Technology and Management Fields.
Meet Inspiring Speakers and Experts at our 3000+ Global Conferenceseries Events with over 600+ Conferences, 1200+ Symposiums and 1200+ Workshops on Medical, Pharma, Engineering, Science, Technology and Business
Case Report Open Access
A Case of Diffuse Subarachnoid Pneumocephalus after Epidural Injection
| Shahla F Syed* and Ernst Garcon | |
| New York Presbyterian Hospital, Columbia University Medical Center, USA | |
| Corresponding Author : | Shahla F. Syed New York Presbyterian Hospital Columbia University Medical Center, USA E-mail: shahlafs@gmail.com |
| Received March 29, 2013; Accepted April 18, 2013; Published April 22, 2013 | |
| Citation: Syed SF, Garcon E (2013) A Case of Diffuse Subarachnoid Pneumocephalus after Epidural Injection. OMICS J Radiology 2:120. doi: 10.4172/2167-7964.1000120 | |
| Copyright: © 2013 Syed SF, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Radiology
| Introduction |
| There have been rare reports of subarachnoid pneumocephalus after an epidural steroid injection in the literature. To our knowledge, none is reported in the radiology literature while the radiologist may be the first to recognize the condition on cross sectional imaging studies. We report a case of diffuse subarachnoid pneumocephalus after epidural steroid injection utilizing the loss-of-resistance technique with an air-filled syringe. |
| Case Report |
| A 45 year-old obese female with a history of acute on chronic lumbar radiculitis presented for epidural steroid injection. The patient has a history of longstanding left lower extremity pain, with an acute exacerbation three weeks prior while bending to do laundry. There was no bowel or bladder incontinence, and no numbness or weakness. MRI of the lumbar spine revealed herniated nucleus pulposus at L4-L5, with impingement of the left L5 nerve root by possible disk fragment. |
| Past medical history includes a strong history of depression. |
| Due to patient’s obesity, surgical intervention was considered an unfavorable option, especially given neurologically intact status. Epidural steroid injection was planned for treatment. |
| A lumbar epidural was performed with the patient in prone position. A pillow was placed underneath the patient, and the L4-L5 interspace was identified under fluoroscopic guidance. A 20-gauge Tuohy needle was inserted via a midline approach. The epidural space was reached via the loss-of-resistance technique at 12 cm. Aspiration was negative for cerebrospinal fluid or hematologic products. Contrast injection of 0.5 cc revealed good cephalo-caudad epidural spread with no paresthesias elicited. Injection of 80 mg of triamcinolone with 3 cc of Preservative Free Normal Saline (PFNS) followed, and the needle was subsequently removed. |
| Within five minutes of the procedure, the patient reported severe sudden onset of frontal headache, left greater than right, and slight tinnitus in the left ear. The pain worsened with movement of the head and neck, and was not relieved with supine position. |
| On physical examination, vital signs were stable and the patient was alert and oriented to person, place and time. Cranial nerves 2-12 were intact. No vision changes or visual loss was identified. Strength was 5/5 in all extremities. Sensation was grossly intact throughout, with no changes from the pre-epidural condition. |
| The patient was taken to the emergency department for further evaluation. A stat head CT was ordered with the clinical indication of headaches. The images (Figure 1) revealed diffuse subarachnoid pneumocephalus involving the ambient, quadrigeminal plate, interpeduncular and suprasellar cisterns, as well as the anterior interhemispheric fissure and left frontal region. With the limited clinical data available at the time of initial evaluation, the differential diagnoses remain intracranial traumatic injury versus subarachnoid pneumocephalus after epidural steroid injection. The later diagnosis was confirmed by the Emergency Room physician. |
| The patient was admitted for overnight observation. Follow-up imaging one month later revealed the pneumocephalus had completely resolved. |
| Discussion |
| Subarachnoid pneumocephalus (SAP) is the presence of air within the subarachnoid space between the arachnoid membrane and the pia mater covering the cortical layer of the brain. The most common etiology is trauma associated with a fracture at the skull base involving the sphenoid sinus or the mastoid air cells, although a fracture involving any sinus may be causative [1-3]. Infection, often secondary to chronic otitis media or mastoiditis, is also a common cause of SAP [1]. Tension pneumocephalus secondary to subarachnoid pleural fistula has been reported after thoracic spine surgery and posterior chest wall resection [4]. Case reports in anesthesiology, neurosurgery and medical literature have described SAP after epidural injections, even in the absence of dural puncture [5-8]; this may be caused by air entry into the meninges during the procedure by direct injection of air or by a pressure gradient resulting in air flow from atmospheric pressure to the lower pressure epidural space, with resulting injury to the dura and subarachnoid [6-8]. |
| The clinical presentation of SAP is not specific. Headache is the most common presentation, and may be posterior, global or orthostatic [6]. Diplopia and loss of consciousness have also been reported [5,7]. Cross sectional imaging with CT or MRI is indicated to exclude an intracranial hemorrhage or mass. |
| The radiologist should have a high index of suspicion of iatrogenic SAP secondary to epidural injection in a patient with low back pain without recent trauma or spine surgery and CT scan findings of subarachnoid air. The Hounsfield value unit of air is usually approximately -1000. Pneumocephalus can be epidural, subdural, subarachnoid, intraparenchymal or intraventricular [2]. The pattern of distribution of the gas can help predict its location within various intracranial spaces. Subarachnoid air predominantly has a sulcal or cisternal distribution, and tends to move anteriorly when the patient is imaged supine [2]. On CT scan, subarachnoid pneumocephalus is characterized by elongated crescentic foci of air attenuation that outline the gyri; SAP may also have a central distribution within the basal cisterns of the brain [2]. Extension of air into the spinal subarachnoid space is not unusual, and may outline the cord [2]. Although subarachnoid distribution is the most common observation, intraventricular presence of air has also been reported in association with epidural steroid injection [7]. MR is more sensitive for the detection of pneumocephalus; on MR images, the subarachnoid air tends to create field inhomogeneity with small pockets of hypointense signal [6]. These findings are best seen on gradient echo or SWI images, and demonstrate a target-like appearance [6]. |
| Treatment of SAP is supportive and spontaneous, and is hastened by increased concentrations of inspired oxygen; resolution of symptoms typically occurs over the course of several hours, while imaging findings may persist for over 7 days [5,7-8]. |
| Conclusions |
| Epidural injection is a potential cause of subarachnoid pneumocephalus, and should be considered in the presence of such findings on CT or MRI in a patient presenting with back pain. As the imaging findings may closely resemble intracranial traumatic injury, unnecessary investigation to exclude a skull base fracture may be avoided. The radiologist should have a high index of suspicion, ask the appropriate questions and make the correct diagnosis. |
References |
|
Figures at a glance
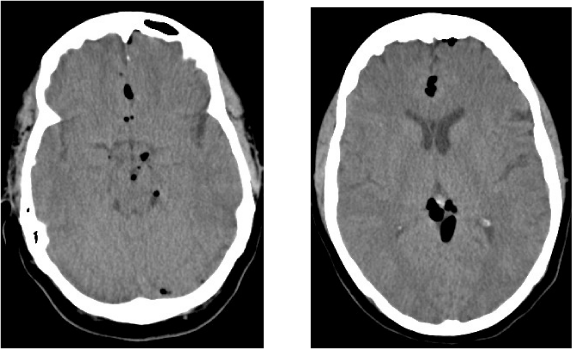 |
| Figure 1 |
Post your comment
Relevant Topics
- Abdominal Radiology
- AI in Radiology
- Breast Imaging
- Cardiovascular Radiology
- Chest Radiology
- Clinical Radiology
- CT Imaging
- Diagnostic Radiology
- Emergency Radiology
- Fluoroscopy Radiology
- General Radiology
- Genitourinary Radiology
- Interventional Radiology Techniques
- Mammography
- Minimal Invasive surgery
- Musculoskeletal Radiology
- Neuroradiology
- Neuroradiology Advances
- Oral and Maxillofacial Radiology
- Radiography
- Radiology Imaging
- Surgical Radiology
- Tele Radiology
- Therapeutic Radiology
Recommended Journals
Article Tools
Article Usage
- Total views: 15412
- [From(publication date):
June-2013 - Aug 23, 2025] - Breakdown by view type
- HTML page views : 10655
- PDF downloads : 4757
