Make the best use of Scientific Research and information from our 700+ peer reviewed, Open Access Journals that operates with the help of 50,000+ Editorial Board Members and esteemed reviewers and 1000+ Scientific associations in Medical, Clinical, Pharmaceutical, Engineering, Technology and Management Fields.
Meet Inspiring Speakers and Experts at our 3000+ Global Conferenceseries Events with over 600+ Conferences, 1200+ Symposiums and 1200+ Workshops on Medical, Pharma, Engineering, Science, Technology and Business
Case Report Open Access
Case Report: Two Cases of Uretero-Iliac Artery Fistula Managed with Endovascular Therapy
| Andy Choy, Jennifer Chang, No Bong Kwak, Mark Kissin* and Igor Lobko | |
| Department of interventional radiology and vascular surgery, Long island jewish medical center, USA | |
| Corresponding Author : | Mark Kissin Department of interventional radiology and vascular surgery Long island jewish medical center, USA Tel: 516-233-3701 E-mail: andchoy@gmail.com |
| Received April 15, 2015; Accepted April 27, 2015; Published April 30, 2015 | |
| Citation: Choy A, Kwak NB, Kissin M, Lobko I (2015) Case Report: Two Cases of Uretero-Iliac Artery Fistula Managed with Endovascular Therapy. OMICS J Radio 4:185. doi: 10.4172/2167-7964.1000185 | |
| Copyright: © 2015 Choy A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Radiology
Abstract
This case report presents two cases of arterial-ureteral fistulas following urological surgical procedures managed with endovascular therapy.
|
Abstract
This case report presents two cases of arterial-ureteral fistulas following urological surgical procedures managed with endovascular therapy.
Case 1
This is an 83 year-old male who was diagnosed with bladder cancer treated with robotic radical cystectomy with bilateral pelvic lymph node dissection and ileal conduit urinary diversion one year ago. The surgery was complicated by urinoma secondary to the right uretero-ileal conduit anastomotic leak. Urinoma was percutaneously drained, and bilateral upside-down nephrostomy catheters acting as the transureteral stents were placed for urinary diversion. However, the patient presented with recurrent urinary tract infection, and interventional radiology was consulted.
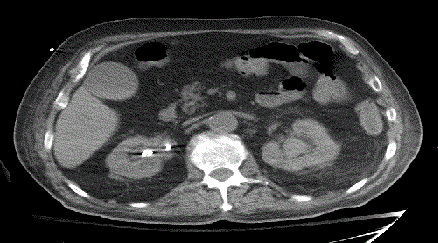
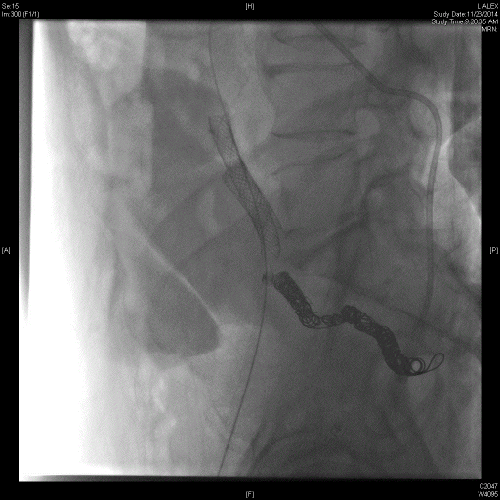
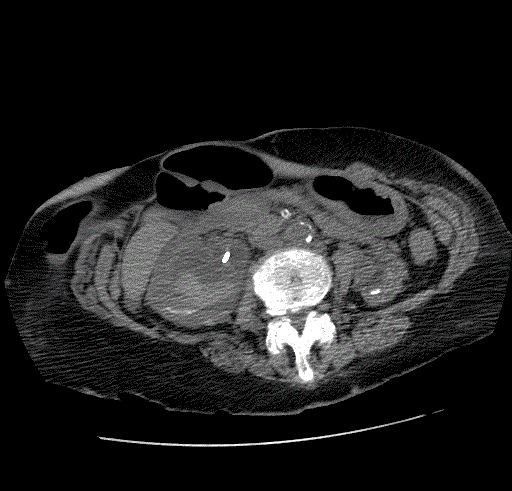
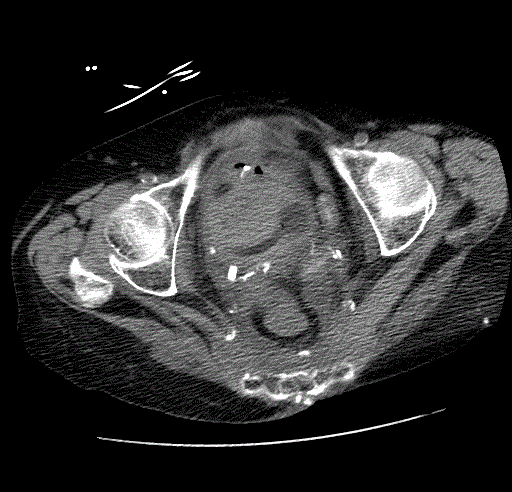
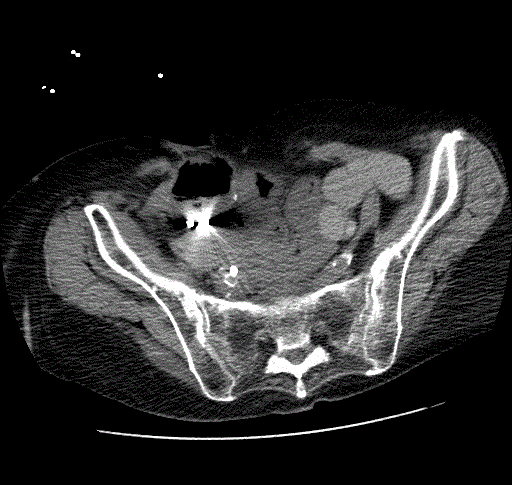
The patient underwent successful placement of bilateral nephrostomy catheters. Removal of the right upside-down nephrostomy catheter was uneventful. However, removal of the left-sided catheter was complicated by brisk pulsatile arterial bleeding from the right lower quadrant ostomy. Based on the review of prior imaging which showed close proximity of the distal left ureter to the right hypogastric artery in the region of the urinoma, the right hypogastric artery was empirically embolized using multiple coils. However, the patient experienced recurrent bleeding overnight in the surgical ICU, and CT angiography was performed demonstrating blood clots in the moderately dilated left renal pelvis (Figure 1A, 1B and 1C) and ureter, and a small pseudoaneurysm of the left distal common iliac artery protruding into the mid left ureter, compatible with an arterioureteral fistula. Conventional angiography confirmed a small contour irregularity (Figure 2) along the anterior wall of the left distal common iliac artery at the site of the pseudoaneurysm seen on the CT angiography (Figure 3). Two stent-grafts were deployed in an overlapping fashion across the fistula followed by balloon dilatation. Case 2
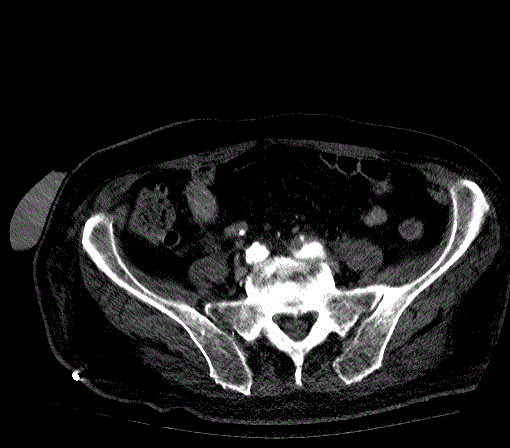
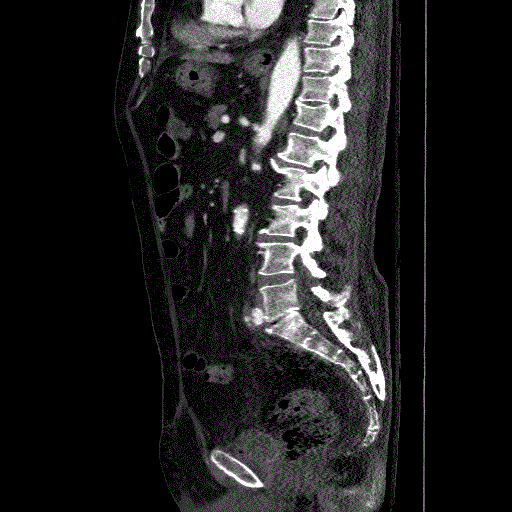
This is a 73 year-old female with a history of uterine cancer status post total abdominal hysterectomy and radiation therapy. The postoperative course was complicated by an enterocutaneous fistula requiring colostomy. The patient previously presented with malignant obstruction of the right ureter which was treated with a tandem right ureteral stent. The patient was lost to the follow-up until she presented with gross hematuria and urinary tract infection. CT scan demonstrated a right ureteral stent with marked hydroureteronephrosis containing blood clots in the right renal pelvis and bladder (Figures 4A, 4B and 5).
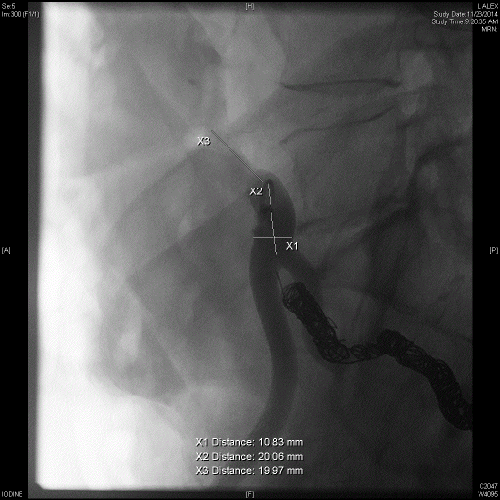
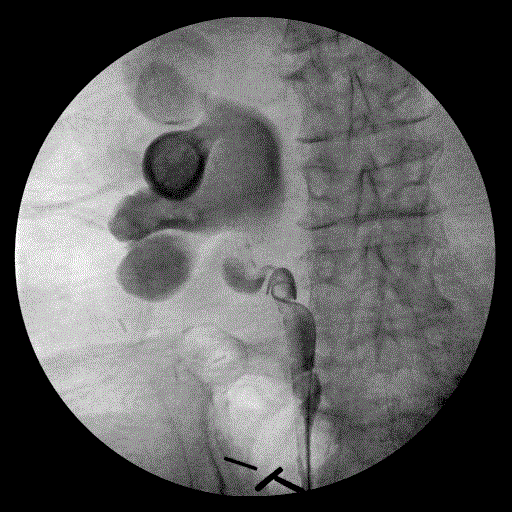
The patient underwent cystoscopy demonstrating a large formed clot in the bladder. Upon removal of the right ureteral stent, there was brisk, pulsatile bleeding from the right ureteral orifice. Compression of the orifice was performed with the resectoscope loop leading to hemostasis. A retrograde pyelogram was then performed showing massive hydroureteronephrosis down to the level of the iliac vessel crossing. A double J ureteral stent was then placed (Figures 6 and 7). Intraoperative vascular surgery consultation was obtained. An on-table angiogram however did not reveal active contrast extravasation in the region of suspected fistula where the ureteral stent crossed the iliac arteries, just distal to the iliac bifurcation. Because of the high suspicion for an underlying AUF, the right internal iliac artery was coil embolized followed by deployment of a stent-graft over the iliac bifurcation. Discussion
Arterioureteral fistula (AUF) is a rare diagnosis that has come into greater spotlight thanks to the recent publication of multiple case reports and literature reviews [1]. AUF is an important cause of gross hematuria and can result in life threatening hemorrhage. Thus, it is important for all clinicians to be aware of this entity.
AUF is defined as an abnormal communication between the ureter and a major artery. Presenting symptoms can range from intermittent to massive hematuria [1,2]. The intermittent nature of the hematuria is thought to be the result of blood clot formation tamponading the bleeding. As in our case, provocative maneuvers such as stent removal can incite episodes of massive hematuria. The diagnosis of AUF is notoriously difficult as angiograms are usually normal. The causes of AUF can be broadly categorized as primary or secondary. Primary causes are usually secondary to aortoiliac aneurysmal disease. Secondary causes represent the majority of cases and include prior pelvic surgery, urinary diversion, pelvic radiation, vascular reconstruction, and use of ureteral catheters/stents [3]. Because of its intermittent nature, the diagnosis of AUF can prove elusive. Diagnostic options include CT angiography, conventional angiography, and ureteroscopy. The sensitivity of these modalities varies. Examination of the patient’s nephrostomy drainage or cystoscopy can help localize the side of bleeding. A technique commonly referred to as “provocative angiography” involves manipulation of a ureteral stent during angiography in order to dislodge any tamponading clot. Some authors have found ureteral contrast studies to have the highest sensitivity. As in the first case, preprocedural CT angiography may facilitate the localization of the pseudoaneurysm or fistula before conventional angiography. As with its diagnosis, there are many options for the treatment of AUF. With the recent advent of endovascular stents, this approach has been employed with favorable outcomes in many published reports [4-6]. Complications of this technique include infection, stent occlusion, refistulization, and recurrent hematuria. A recent study estimated the hematuria recurrence-free rates at 1 and 2 years were 76.2 and 40.6% respectively [7]. Muraoka et al. reported a stent patency rate of over 6 years in one patient. Nevertheless, more investigations will need to be performed to establish long term stent patency rates. Embolization of the internal iliac artery can be employed when it is the source. The placement of coils into the distal ureter with concomitant nephrostomy placement has also been used. Open surgical approaches remain an effective treatment in patients whom the diagnosis or site of AUF is uncertain or in patients where the use of endovascular approaches are contraindicated. Surgical approaches are varied including fistula closure with a patch, vascular ligation, vascular bypass, renal autotransplant and omentoplasty [8]. Nephroureterectomy has also been performed in patients in whom the diagnosis of AUF is suspected. Overall, the diagnosis of an AUF should be considered in any patient with the aforementioned risk factors who presents with hematuria. A multi-disciplinary approach to treatment should be employed with involvement of urology, radiology, and vascular surgery. References
|
Figures at a glance
 |
 |
 |
 |
 |
| Figure 1A | Figure 1B | Figure 1C | Figure 2 | Figure 3 |
 |
 |
 |
 |
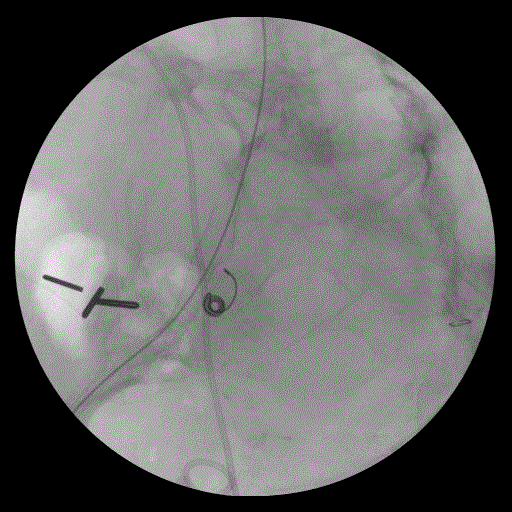 |
| Figure 4A | Figure 4B | Figure 5 | Figure 6 | Figure 7 |
Post your comment
Relevant Topics
- Abdominal Radiology
- AI in Radiology
- Breast Imaging
- Cardiovascular Radiology
- Chest Radiology
- Clinical Radiology
- CT Imaging
- Diagnostic Radiology
- Emergency Radiology
- Fluoroscopy Radiology
- General Radiology
- Genitourinary Radiology
- Interventional Radiology Techniques
- Mammography
- Minimal Invasive surgery
- Musculoskeletal Radiology
- Neuroradiology
- Neuroradiology Advances
- Oral and Maxillofacial Radiology
- Radiography
- Radiology Imaging
- Surgical Radiology
- Tele Radiology
- Therapeutic Radiology
Recommended Journals
Article Tools
Article Usage
- Total views: 13829
- [From(publication date):
April-2015 - Aug 17, 2025] - Breakdown by view type
- HTML page views : 9276
- PDF downloads : 4553
