Research Article Open Access
Changes in Stress Reactivity among Stimulant Dependent Adults After Treatment with Mindfulness Based Relapse Prevention: Results from a Pilot Randomized Clinical Trial
Suzette Glasner Edwards1*, Emily E Hartwell2, Larissa Mooney1, Alfonso Ang1, Hélène Chokron Garneau1, Mary-Lynn Brecht1and Richard Rawson11University of California, Los Angeles, Integrated Substance Abuse Programs, USA
2Department of Psychology, University of California, Los Angeles, USA
- *Corresponding Author:
- Suzette Glasner-Edwards
Integrated Substance Abuse Programs
David Geffen School of Medicine at UCLA
Semel Institute for Neuroscience and Human Behavior
1640 S. Sepulveda Blvd., Suite 120, Los Angeles, Canada
Tel: 310 267-5206
Fax: 310 312-0538
E-mail: sglasner@ucla.edu
Received date: August 17, 2016; Accepted date: October 07, 2016; Published date: October 14, 2016
Citation: Edwards SG, Hartwell EE, Mooney L, Ang A, Garneau HC, et al. (2016) Changes in Stress Reactivity among Stimulant Dependent Adults After Treatment with Mindfulness Based Relapse Prevention: Results from a Pilot Randomized Clinical Trial. J Addict Res Ther 7:298. doi:10.4172/2155-6105.1000298
Copyright: © 2016 Edwards SG, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Addiction Research & Therapy
Abstract
Background: In light of recent evidence suggesting the presence of stress processing deficits in stimulant users, coupled with laboratory studies demonstrating an association between stress reactivity and relapse to stimulant use, interventions that target stress-induced craving and stress reactivity may reduce relapse risk in this population.
Objective: This study examines changes in stress reactivity among adults with stimulant use disorders (N=22) in response to an 8 week Mindfulness Based Relapse Prevention (MBRP) intervention.
Methods: Study participants were enrolled in a in a pilot randomized clinical trial, evaluating the efficacy of MBRP, relative to a health education control condition (HE). At baseline and treatment-end, biological and subjective responses to a laboratory psychosocial stress task (i.e., the Trier Social Stress Task) were measured.
Results: MBRP participants evidenced significantly lower levels of salivary cortisol in response to the posttreatment laboratory stress provocation, relative to those in the HE condition. Likewise, HE participants evidenced disproportionately greater increases in subjective stress, anxiety and stimulant cravings in response to the posttreatment stress provocation, relative to those who received MBRP.
Conclusion: Results of this pilot investigation suggest that MBRP effectively attenuates stress reactivity among adults with stimulant use disorders. This approach may have utility as an adjunct to comprehensive programs treating stimulant addiction. Future research evaluating the impact of changes in stress reactivity on post-treatment relapse to stimulant use and the long-term effects of MBRP on stress reactivity is warranted.
Keywords
Stimulants; Mindfulness; Addiction; Stress reactivity
Abbreviations
MBRP: Mindfulness Based Relapse Prevention; HE: Health Education; MINI: Mini-International Neuropsychiatric Interview; TSST: Trier Social Stress Task; RCT: Randomized Clinical Trial
Introduction
Despite the health risks associated with stimulant use, the 2012 National Household Survey on Drug Abuse estimated that 4.7% and 14.3% of the population have tried methamphetamine and cocaine, respectively, in their lifetime (SAMHSA, 2013). Long-term use is associated with neuroadaptive changes in stress processing which can be particularly problematic in addiction recovery [1-7]. Stress dysregulation is associated with relapse in cocaine users; for example, increased cortisol response and cocaine craving in the face of stress provocation predicts heavier cocaine use during follow-up and shorter time to relapse [8].
Despite the paucity of research on interventions targeting stress reactivity among drug users, in one study, a cognitive-behavioral stress management intervention significantly attenuated stress-induced craving and physiological stress response [9]. Mindfulness based relapse prevention (MBRP) is a behavioral intervention that targets stress reactivity, negative affect, and drug cravings. To achieve this, MBRP facilitates awareness of the present through meditation, coupled with cognitive and behavioral coping skills for tolerating discomfort [10]. In a pilot investigation, mindfulness training attenuated anxiety, fear, and anger in response to a personalized stress induction paradigm among alcohol and stimulant users [11]. Nevertheless, no studies to date have examined the effects of MBRP on laboratory-induced stress reactivity among adults with stimulant use disorders.
To investigate the impact of an 8 week MBRP program on stress reactivity, stimulant dependent individuals who were enrolled in a pilot RCT comparing MBRP to a health education (HE) control [12] completed a laboratory stress task at baseline and again at treatmentend. We hypothesized that those who received MBRP would evidence reductions in psychological and physiological indices of stress reactivity from baseline to treatment-end, relative to HE participants.
Methods
Subjects
Participants were 22 stimulant dependent adults who participated in a pilot RCT of an 8-week MBRP intervention, relative to a HE control intervention for stimulant dependence described elsewhere [12]. Treatment-seeking stimulant users age >18 were recruited from the greater Los Angeles area through advertising, referrals and study flyers posted at various treatment facilities. Individuals were excluded if they: exhibited medical or psychiatric impairment that compromised their safety or ability to participate in brief meditation exercises, and/or required primary treatment (e.g. hospitalization); required medical detoxification from any substances.
The present study, conducted using a subset of participant’s who agreed to participate in a laboratory-based stress induction procedure, was approved by the UCLA IRB. After description of the study to participants, informed consent was obtained. Of the 22 participants, 9 were assigned to the MBRP and 13 to the HE condition.
Mindfulness Based Relapse Prevention. MBRP was delivered by a master’s level study therapist weekly in group format over 8 weeks. All sessions were 75 min and began with a guided meditation, followed by homework review and relapse prevention exercises, guided by the MBRP manual [13]. Goals of MBRP include increasing awareness of relapse triggers, interrupting “automatic” behavior sequences to promote mindful responses (versus “reactions”) to triggers and cravings, and practicing non-judgemental awareness of one’s momentto- moment experience. Participants were given meditation exercise CDs for between-session practice and a log to record time spent practicing. The study therapist, who was formally trained prior to this study in Mindfulness Based Stress Reduction, participated in a 2 day, manualized MBRP training seminar and received on-going supervision, including fidelity monitoring over the course of the trial [12].
Health Education, HE participants received 8 weekly manualized, group health psychoeducation sessions of equivalent duration to MBRP. The intervention comprised a multimedia educational program addressing various health and wellness topics including the 6 dimensions of health (e.g. intellectual, social, emotional, physical, environmental and spiritual) and specific topics within these areas, including nutrition, dental care, acupuncture, skin care, cancer screening, sleep hygiene, physical activity, and traffic safety. Content was adapted from a wellness manual [14] used in a study of exercise for smoking cessation. The HE facilitator held a master’s degree in public health, and was a certified health educator.
Procedures and instruments
Trained interviewers conducted assessments at baseline and treatment-end. A demographics questionnaire gathered information about sex, age, education, marital status, and employment. Stimulant dependence was diagnosed at baseline using the Mini-International Neuropsychiatric Interview (MINI) [15], a brief structured diagnostic interview. Participants provided a urine sample at each visit which was analyzed for the presence of amphetamine, methamphetamine, and cocaine metabolites (benzoylecognine; BE) using enzyme immunoassay test (EMIT) procedures. A 300 ng/ml BE cut-off was used to define a positive sample.
The Trier Social Stress Task (TSST), a well-validated stress induction paradigm [16], was administered at baseline and treatment-end. The task includes a 3 min anticipatory period, a 5 min public speaking task and a 5 min mental arithmetic task in front of an evaluative panel of two adults. During the anticipatory period, participants were asked to prepare and deliver a speech about their personal strengths to an evaluative panel of two adults. Following the speech, participants were asked to perform a mental arithmetic task, by subtracting serial 13 s from 1022 as quickly and accurately as possible for 5 min. If they made an error, participants were instructed to start over from the beginning.
Prior to, immediately after, 15, 30 and 60 min following administration of both the baseline and post-treatment TSST, participants were administered the Within Session Ratings Scale [17], which asks participants to rate, on a 10-point visual analogue scale (0=not at all to 10=extremely), subjective stress, anxiety, mood disturbance and craving for stimulants. At the same time points, salivary cortisol was collected using a commercially available competitive immunoassay kit (Quest Diagnostics, West Hills, CA).
Statistical analysis
Chi-square and t-tests were used to analyze group differences (i.e., comparing those who received MBRP versus HE) on key outcome variables at baseline and treatment-end (i.e., changes in indicators of stress reactivity before versus after the TSST). Multivariate logistic regression analyses were employed to examine the effects of group on post-treatment stress reactivity in response to the TSST.
Results
The original sample of participants in the pilot RCT (N=63) was compared with the subset of participants who were included in the current investigation (N=22) using t-tests and chi-square tests for age, education, gender, marital status, route of administration, employment, and baseline stimulant use frequency in the past 30 days. In all analyses, there were no significant differences between the participants in the current study and the original mindfulness RCT sample. See Table 1 for demographic characteristics.
As a primary indicator of stress reactivity, the proportion of individuals whose cortisol increased from the pre-TSST measurement at each of the four time points after the TSST was examined and compared between the MBRP and HE groups. At the baseline TSST administration, the proportion of MBRP versus HE participants whose cortisol increased was no different at any of the post-TSST administration time points (all p-values >0.05). At the post-treatment TSST administration, however, a significantly greater proportion of those in the HE condition evidenced elevations in cortisol at 15 (χ2=5.1, df=1, p<0.05) and 60 min (χ2=4.4, df=1, p<0.05) following the TSST, relative to those who received MBRP, with no significant group differences at the remaining time points (Table 2). In terms of effect sizes, the variance explained by the model in Table 2 for increased response in cortisol level by treatment group at 15 min is 0.29; At 30 min, the variance explained is 0.24.
| Sample (N=22) | Control (n=13) | Mindfulness (n=9) | |
|---|---|---|---|
| Gender, % (N) | |||
| Male | 81.8 (18) | 76.9 (10) | 88.9 (8) |
| Age, M(sd) | 46.6 (8.1) | 47.3 (8.3) | 45.7 (8.2) |
| Yrs education, M(sd) | 13.5 (2) | 13.6 (1.8) | 13.3 (2.2) |
| Ethnicity, %(N) | |||
| Caucasian | 36.4 (8) | 45.5 (5) | 37.5 (3) |
| Hispanic | 13.6 (3) | 16.7 (2) | 11.1 (1) |
| African American | 50 (6) | 50.0 (6) | 55.6 (5) |
| Asian | 13.6(3) | 20.0 (2) | 11.1 (1) |
| Current employment, %(N) | |||
| Full time | 18.2 (4) | 7.7 (1) | 33.3 (3) |
| Part time/Student | 36.3 (8) | 23.1 (3) | 11.1 (1) |
| Unemployed | 45.5 (10) | 38.5 (5) | 55.6 (5) |
| Full time | 18.2 (4) | 7.7 (1) | 33.3 (3) |
| Part time/Student | 36.3 (8) | 23.1 (3) | 11.1 (1) |
| Marital status, %(N) | |||
| Married | 9.1 (2) | 7.7 (1) | 11.1 (1) |
| Divorced/Separated | 31.8 (7) | 38.5 (5) | 22.2 (2) |
| Never Married | 59.1 (13) | 53.8 (7) | 66.7 (6) |
Table 1: Sample characteristics for the total sample and by treatment group.
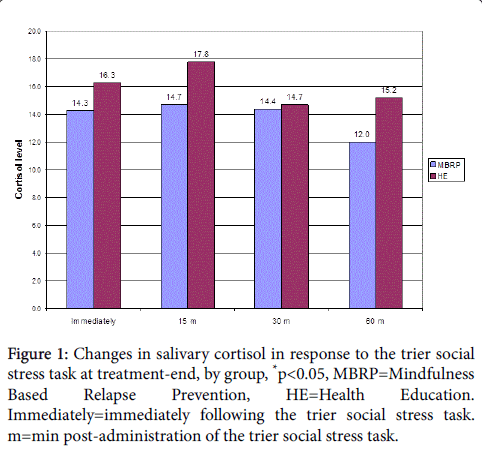
Cortisol values at the post-treatment TSST were examined in a multivariate model controlling for the potential effects of baseline cortisol levels and post-treatment stimulant use (indicated by urine drug screens), revealing significantly higher cortisol levels among those who received HE, relative to MBRP, at 15 (χ2=1.9, df=1, p<0.05) and 60 (χ2=1.9, df=1, p<0.05) min following the TSST. A marginally significant difference in cortisol, favoring the MBRP group was observed immediately after the TSST (χ2=1.7, df=1, p=0.05), with no significant differences at the 30 min time point (Figure 1).
| %Cortisol increase (MBRP) | % Cortisol increase (HE) | c2 | P-value | |
|---|---|---|---|---|
| Baseline TSST: | ||||
| Immediately after TSST | 63.20% | 66.70% | 0.054 | 0.82 |
| 15 min | 55.60% | 71.40% | 1.06 | 0.3 |
| 30 min | 55.60% | 70.00% | 0.849 | 0.36 |
| 60 min | 55.60% | 70.00% | 0.85 | 0.36 |
| Post-Treatment TSST: | ||||
| Immediately after TSST | 14.30% | 45.50% | 1.87 | 0.17 |
| 15 min | 0% | 54.60% | 5.06 | Â 0.02* |
| 30 min | 28.60% | 36.40% | 0.12 | 0.73 |
| 60 min | 0% | 45.50% | 4.41 | Â 0.03* |
Table 2: Percentage of participants for whom cortisol levels increased in response to the trier social stress task at baseline and treatment-end, *P<0.05, Significant difference in % cortisol increase between MBRP and HE, TSST=Trier Social Stress Task.
Figure 1: Changes in salivary cortisol in response to the trier social stress task at treatment-end, by group, *p<0.05, MBRP=Mindfulness Based Relapse Prevention, HE=Health Education. Immediately=immediately following the trier social stress task. m=min post-administration of the trier social stress task.
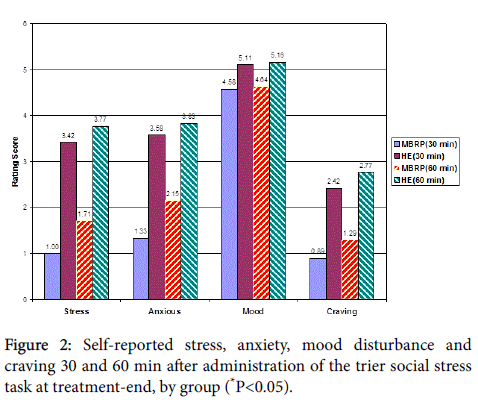
To examine the correspondence of subjective reports of stress reactivity between the MBRP and HE groups with the differences observed using cortisol, the 2 groups were compared on self-reported stress, anxiety, mood, and craving at the post-treatment TSST administration (Table 3). Prior to the post-treatment TSST, there were no significant differences observed in HE versus MBRP participants’ ratings on these 4 dimensions. A significantly greater proportion of HE participants evidenced increases in stress ratings, relative to those in MBRP immediately after, 30 min and 60 min post-TSST. For the subjective response in stress (treatment end) at 30 min, the effect size as measured by variance explained is 0.20 and at 60 min, the variance explained is 0.22. Likewise, a significantly greater proportion of HE participants reported increases in stimulant cravings, as compared to MBRP at 15 and 30 min post-TSST. The HE group experienced disproportionately greater increases in anxiety at 30 and 60 min post- TSST, as well as mood disturbance at 30 and 60 min post-TSST. See Figure 2 for differences in subjective ratings by group.
| % increase (MBRP) | % increase (HE) | c2 | P-value | |
|---|---|---|---|---|
| Stress | ||||
| Immediately after TSST | 5.80% | 19.40% | 4.39 | 0.03* |
| 15 min | 13.00% | 24.20% | 2.37 | 0.12 |
| 30 min | 14.50% | 33.30% | 4.83 | 0.02* |
| 60 min | 15.10% | 33.40% | 4.59 | 0.03* |
| Anxious | ||||
| Immediately after TSST | 8.70% | 19.40% | 2.71 | 0.1 |
| 15 min | 17.40% | 30.30% | 2.55 | 0.11 |
| 30 min | 14.90% | 36.40% | 6.17 | 0.01* |
| 60 min | 19.70% | 43.30% | 5.8 | 0.01* |
| Mood | ||||
| Immediately after TSST | 14.50% | 28.60% | 3.28 | 0.07 |
| 15 min | 17.40% | 30.30% | 2.55 | 0.11 |
| 30 min | 14.50% | 36.40% | 6.13 | 0.01 |
| 60 min | 19.70% | 43.30% | 4.71 | 0.03 |
| Craving | ||||
| Immediately after TSST | 11.80% | 16.70% | 0.91 | 0.34 |
| 15 min | 10.10% | 33.30% | 6.63 | 0.01* |
| 30 min | 13.00% | 30.30% | 4.22 | 0.04* |
| 60 min | 10.60% | 23.30% | 2.87 | 0.09 |
Table 3: Percentage of participants for whom self-reported stress, anxiety, mood and craving increased in response to the trier social stress task at treatment-end, TSST=Trier Social Stress Task; MBRP=Mindfulness Based Relapse Prevention condition; HE=Health Education condition.
Discussion
This study examined changes in laboratory-induced stress reactivity among treatment-seeking, stimulant dependent adults who received MBRP. In this pilot study, MBRP led to reductions in both physiological and subjective indices of stress reactivity, relative to those who received a HE control intervention. MBRP was associated with improvements in stress-induced anxiety, mood disturbance, and stimulant cravings. Correspondingly, MBRP participant’s evidenced reductions in salivary cortisol in response to a laboratory based stress induction from baseline to post-treatment.
This investigation replicates and extends the work of Brewer et al. who found that alcohol and stimulant users who received mindfulness training evidenced attenuated psychological and physiological responses (e.g. heart rate variability) to stress provocation via exposure to personalized imagery scripts [11]. Likewise, we found that subjective and biological indices of stress reactivity were attenuated in response to a well-established psychosocial stress task, to which responses are associated with relapse susceptibility among cocaine users [8]. Taken together, these findings suggest that mindfulness based interventions effectively target stress among adults with stimulant use disorders.
Several limitations of this investigation warrant comment. First, due to the small sample size, findings should be considered preliminary. Second, as a result of limited statistical power, we did not evaluate the contribution of additional factors (e.g. comorbid psychiatric diagnoses, substance use apart from stimulants) that may have influenced stress reactivity. In addition, the stress paradigm used may not generalize to stressful events experienced outside of the laboratory setting, limiting the potential ecological validity of the results. The presence of longterm effects of MBRP on stress reactivity is unknown. Nevertheless, the fact that a number of significant findings emerged despite these limitations is encouraging.
In conclusion, findings from this pilot study suggest that MBRP has promise as a component of addiction treatment for stimulant users, particularly as a means of targeting stress processing and reactivity. Further research is warranted to elucidate the relationship of changes in stress reactivity to post-treatment relapse and the enduring effects of MBRP on stress reactivity.
Acknowledgement
The authors would like to thank Anne Bellows Lee, Hailey Winetrobe, Megan Holmes, Mary Olaer, and all of the research staff at the UCLA ISAP Clinical Research Center, including Al Hasson, Christie Thomas, and Jeff Annon. We also thank Alan Marlatt, Katie Witkiewitz, Neharika Chawla, Sarah Bowen, and Judson Brewer for valuable input in the design and implementation of the RCT. We are grateful to Sudie Back for her valuable input concerning the measurement of stress reactivity. The research presented in this paper was supported by grants R21 DA029255, K23 DA020085 and T32 DA07272-21 from the National Institute on Drug Abuse.
References
- Mantsch JR, Yuferov V, Mathieu-Kia AM, Ho A, Kreek MJ (2003) Neuroendocrine alterations in a high-dose, extended-access rat self-administration model of escalating cocaine use. Psychoneuroendocrinology 28: 836-862.
- Li CS, Sinha R (2008) Inhibitory control and emotional stress regulation: Neuroimaging evidence for frontal-limbic dysfunction in psycho-stimulant addiction. NeurosciBiobehav Rev 32: 581-597.
- Sinha R, Fuse T, Aubin LR, O'Malley SS (2000) Psychological stress, drug-related cues and cocaine craving. Psychopharmacology 152: 140-148.
- Sinha R, Talih M, Malison R, Cooney N, Anderson GM (2003) Hypothalamic-pituitary-adrenal axis and sympatho-adreno-medullary responses during stress-induced and drug cue-induced cocaine craving states. Psychopharmacology 170: 62-72.
- Manetti L, Cavagnini F, Martino E, Ambrogio A (2014) Effects of cocaine on the hypothalamic��?pituitary-adrenal axis. J Endocrinol Invest 37: 701-708.
- Li SX, Yan SY, Bao YP, Lian Z, Qu Z (2013) Depression and alterations in hypothalamic��?pituitary��?adrenal and hypothalamic-pituitary-thyroid axis function in male abstinent methamphetamine abusers. Hum Psychopharmacol 28: 477-483.
- Zuloaga DG, Jacobskind JS, Raber J (2015) Methamphetamine and the hypothalamic-pituitary-adrenal axis. Front Neurosci 9: 178.
- Back SE, Hartwell K, DeSantis SM, Saladin M, McRae-Clark AL, et al. (2010) Reactivity to laboratory stress provocation predicts relapse to cocaine. Drug Alcohol Depend 106: 21-27.
- Back SE, Gentilin S, Brady KT (2007) Cognitive-behavioral stress management for individuals with substance use disorders: A pilot study. J NervMent Dis 195: 662-668.
- Marlatt GA, Chawla N (2007) Meditation and alcohol use. South Med J 100: 451-453.
- Brewer JA, Sinha R, Chen JA, Michalsen RN, Babuscio TA, et al. (2009) Mindfulness training and stress reactivity in substance abuse: Results from a randomized, controlled stage I pilot study. Substance Abuse 30: 306-317.
- Glasner-Edwards S, Mooney LJ, Ang A, ChokronGarneau H, Hartwell E, et al. (2016) Mindfulness based relapse prevention for stimulant dependent adults: A pilot randomized clinical trial. Mindfulness.
- Bowen S, Chawla N, Marlatt GA (2010) Mindfulness-based relapse prevention for addictive behaviors: A clinician��?s guide. Guilford Press.
- Kinnunen T, Leeman RF (2008) Exercise as an adjunct to nicotine gum in treating tobacco dependence among women. Nicotine Tob Res 10: 689-703.
- Sheehan DV, Lecrubier Y, Sheehan KH, Amorim P, Janavs J, et al. (1998) The Mini-International Neuropsychiatric Interview (MINI): The development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry 59: 22-33.
- Kirschbaum C, Pirke KM (1993) The ��?Trier Social Stress Test��?- a tool for investigating psychobiological stress responses in a laboratory setting. Neuropsychobiology 28: 76-81.
- Childress AR, McLellan AT, O'Brien CP ( 1986) Abstinent opiate abusers exhibit conditioned craving, conditioned withdrawal and reductions in both through extinction. Br J Addict 81: 655-660.
Relevant Topics
- Addiction Recovery
- Alcohol Addiction Treatment
- Alcohol Rehabilitation
- Amphetamine Addiction
- Amphetamine-Related Disorders
- Cocaine Addiction
- Cocaine-Related Disorders
- Computer Addiction Research
- Drug Addiction Treatment
- Drug Rehabilitation
- Facts About Alcoholism
- Food Addiction Research
- Heroin Addiction Treatment
- Holistic Addiction Treatment
- Hospital-Addiction Syndrome
- Morphine Addiction
- Munchausen Syndrome
- Neonatal Abstinence Syndrome
- Nutritional Suitability
- Opioid-Related Disorders
- Relapse prevention
- Substance-Related Disorders
Recommended Journals
Article Tools
Article Usage
- Total views: 13270
- [From(publication date):
October-2016 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 12289
- PDF downloads : 981