Make the best use of Scientific Research and information from our 700+ peer reviewed, Open Access Journals that operates with the help of 50,000+ Editorial Board Members and esteemed reviewers and 1000+ Scientific associations in Medical, Clinical, Pharmaceutical, Engineering, Technology and Management Fields.
Meet Inspiring Speakers and Experts at our 3000+ Global Conferenceseries Events with over 600+ Conferences, 1200+ Symposiums and 1200+ Workshops on Medical, Pharma, Engineering, Science, Technology and Business
Case Report Open Access
Extraskeletal Ewing’s Sarcoma in Conus Medullaris: A Case Report and Review of the Literature
| Xi-fu Wang, Gui-xiang Zhang*, Kang-an Li, Yu-jie Li and Lin-feng Zheng | |
| Department of Radiology, Shanghai Jiaotong University Affiliated First People’s Hospital, Shanghai 200080, China | |
| Corresponding Author : | Guixiang Zhang Department of Radiology Shanghai Jiaotong University Affiliated First People’s Hospital Shanghai 200080, China E-mail: guixiangzhang@sina.com |
| Received March 13, 2013; Accepted August 16, 2013; Published August 20, 2013 | |
| Citation: Wang XF, Zhang GX, Li KA, Li YJ Zheng LF (2013) Extraskeletal Ewing’s Sarcoma in Conus Medullaris: A Case Report and Review of the Literature. OMICS J Radiology 2:139 doi: 10.4172/2167-7964.1000139 | |
| Copyright: © 2013 Wang XF, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Radiology
| Introduction | |
| Extraskeletal Ewing’s sarcomas (EES) are a rare soft tissue sarcoma that arises in extraskeletal sites. To the best of our knowledge, so far, EES has been described that it mostly involves the paravertebral region, lower extremities, chest wall, and pelvis [1-3], however, few cases of primary intramedullary EES in spinal canal have been documented [4,5]. Herein, this paper describes a case of EES in conus medullaris in a 16-years-old girl, which has not been reported in previous literature. | |
| Case Report | |
| A previously healthy 16-year-old girl presented with a 3-weeks history of progressive low back pain radiating to lower extremities under no obvious predisposing causes, and became worse particularly at night. Unfortunately she felt no better in clinical symptoms than before after acupuncture and massage. Physical examination showed reeling gait, grade 4 in the right lower extremity, grade 3 in the left one with hypalgesia and hypothermoesthesia, and positive heel-tap reflex and knee jerk. | |
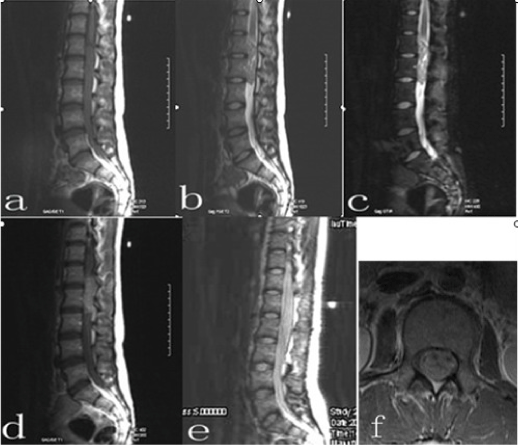
| Imaging studies were all performed in our own department of radiology. Lumbar plain film showed no abnormality. Magnetic resonance (MR) imaging of lumbar spine revealed a well-demarcated mass in conus medullaris, which was 1.8 cm×5.6 cm×2.0 cm in size. The mass was isointense to muscle on T1-weighted images, hyperintense to muscle on T2-weighted images and short tau inversion recovery (STIR) images. It demonstrated slightly inhomogeneous, moderate enhancement with many small noncontrast-enhanced cystic areas on T1-weighted images after intravenous administration of Gd-DTPA (Figure 1a-f). The adjacent nerve roots were compressed by the mass without destructive or sclerotic change of vertebrae. The widening of neural foramina, intervertebral foramen and lymphadenopathy were not demonstrated. On the basis of these findings, the preoperative diagnosis of the mass in conus medullaris was ependymoma. Postoperative imaging confirmed that the tumor completely disappeared (Figure 1e). | |
| The patient underwent laminectomy with the entire tumor removed soon after radiologic tests. A long-round, soft, red-togray mass measuring 1.5 cm×5.0 cm×2.0 cm was seen in the conus medullaris | |
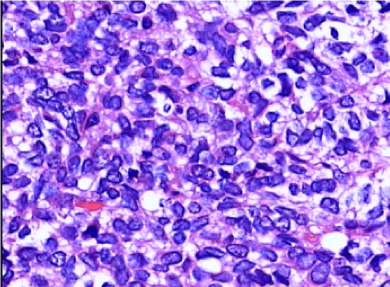
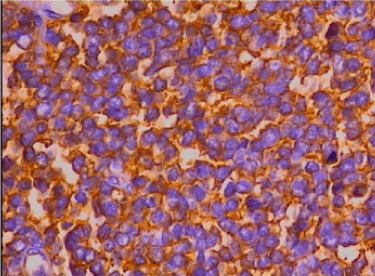
| On histopathological examination, the neoplasm consisted of sheets of small, blue round cells in the capillary network stroma, with oval nuclei, small nucleoli and a small amount of ill-defined cytoplasm (Figure 2). A periodic acid-Schiff stain (PAS) showed abundant intracytoplasmic glycogen. Immunohistochemical analysis revealed negative staining for leukocyte common antigen (LCA), desmin (Des), epithelial membrane antigen (EMA), muscular specific antigen(MSA), and positive expression for vimentin, neurone specific enolase (NSE) and CD99 (Figure 3). The final diagnosis of EES was thus made. | |
| The patient underwent immediately local postoperative radiotherapy (4196 cGy/22F×/47day), followed by adjuvant chemotherapy with dacarbazine (DTIC) 200 mg d1-5; THP 60 mg d1; ifosfamide (IF0)2.0 d1-3. After multimodal therapies, her neurologic functions were recovered perfectly, and metastasis was not detected clinically . | |
| Discussion | |
| EES was first reported in 1969 by Tefft [6]. The histopathological characteristics were described in 1975 by Anhgervall and Enzinger [1], in accordance with the diagnostic criteria for Ewing’s sarcoma. Subsequently, this new kind of soft tissue sarcoma was defined as EES as a result of a distinct clinicopathologic entity with unknown mesenchymal origin. | |
| EES is a rare condition, but it has the tendency of increasing incidence over the past few years. The patients between the ages of 10 years and 30 years are predominantly affected, with a median age of 20 years old, and most series have shown no gender predilection. Clinically, the median interval between symptom onset and diagnosis was only 2 to 3.5 months. Patient with EES presents with a rapidly enlarging swelling which is usually less painful than its skeletal counterpart. | |
| There may be no abnormal findings for intradural EES of spinal canal on routine radiograph, neither osteolytic nor osteosclerotic changes were seen in the vertebral bodies. On MR imaging, intradural EES was isointense to muscle on T1-weighted images, hyperintense to muscle on T2-weighted images and STIR images [4]. The tumor enhanced irregularly with gadolinium, but these MR findings of intradural EES were nonspecific. At the site of conus medullaris, therefore, ependymoma, astrocytoma and swannoma should be included in differential diagnosis [7]. Ependymomas are often cited as the most frequent in adults (65%), especially at the conus medularis and filum terminal. It arises from ependymal cell lining the central canal or its remnants and from the cells of ventriculus terminalis in the filum terminale. Occuring in the cauda equina region in adults is a special variant, named the myxopapillary ependymoma. Astrocytoma is the most common intramedullary tumor in children (59%), diffusely expanding the spinal cord, occasionally involving the entire length of the spinal cord. Swannoma of nerve sheath tumors is usually in middle decades, appearing as an encapsulated, well-demarcated round or oval tumor with cystic degeneration and hemorrhage. In our case, the neoplasm was misdiagnosed as ependymoma, even though MR imaging revealed exactly that it was located in conus medullaris of spinal canal. | |
| The final diagnosis of EES is made primarily on the basis of the combination of light and electron microscopic features, and immunohistochemistry. Histopathological examination shows sheets of small blue round cells tumor (SBRCT) with oval nuclei, small nucleoli and scanty cytoplasm. Microscopic findings of SBRCT were no specific, as SBRCT included lymphoma, neuroblastoma, Wilms tumor, rhabdomyosarcoma, small cell osteosarcoma, Merkel cell carcinoma, small cell carcinoma and Ewings family of tumors (osseous Ewing sarcoma, EES and primitive neuroectodermal tumor (PNET)). Therefore, it seems difficult to distinguish these entities only by means of microscopy. However positive staining for CD99 on immunohistiochemistry become gold standard for diagnosis of EES. In our case, ESS was confirmed dependent on CD99. | |
| Entire resection of EES followed by adjunctive chemotherapy and radiotherapy has greatly improved the prognosis of EES. Ahmad et al. [8] reviewed retrospectively twenty-four patients with EES treated with modern multimodal therapies and concluded that age and surgical treatment were found to be important prognostic variables in the treatment of EES. With multimodal therapeutic approach, a 9.3- year disease-free survival has been achieved. No other variables, such as tumor size, tumor location, stage of disease, or radiation therapy, were found to improve survival. In our case, her neurologic functions were recovered perfectly after entire resection of the mass combined with adjunctive chemotherapy and radiotherapy. | |
| In conclusion, although extremely rare, EES should be included in the differential diagnosis of intradural soft tissue mass lesions of spinal canal. | |
References |
|
|
|
Figures at a glance
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 |
Post your comment
Relevant Topics
- Abdominal Radiology
- AI in Radiology
- Breast Imaging
- Cardiovascular Radiology
- Chest Radiology
- Clinical Radiology
- CT Imaging
- Diagnostic Radiology
- Emergency Radiology
- Fluoroscopy Radiology
- General Radiology
- Genitourinary Radiology
- Interventional Radiology Techniques
- Mammography
- Minimal Invasive surgery
- Musculoskeletal Radiology
- Neuroradiology
- Neuroradiology Advances
- Oral and Maxillofacial Radiology
- Radiography
- Radiology Imaging
- Surgical Radiology
- Tele Radiology
- Therapeutic Radiology
Recommended Journals
Article Tools
Article Usage
- Total views: 13750
- [From(publication date):
September-2013 - Aug 18, 2025] - Breakdown by view type
- HTML page views : 9156
- PDF downloads : 4594
