Case Report Open Access
False-Negative 99mTc Medi-MIBI Parathyroid Scintigraphies: A Report on the Possible Role of Diagnostic Two-Phase Single-Acquisition CT
| Afzelius P1*, Iyer V1, Lelkaitis G2 and Henriksen SD3 | |
| 1Department of Nuclear Medicine, Aalborg University Hospital, Denmark | |
| 2Department of Pathology, Aalborg University Hospital, Denmark | |
| 3Department of Otolaryngology, Head and Neck Surgery, Aalborg University Hospital, Denmark | |
| Corresponding Author : | Pia Afzelius Department of Nuclear Medicine Aalborg University Hospital Hobrovej 18-22, 9000 Aalborg, Denmark E-mail: pia.afzelius@dadlnet.dk |
| Received March 03, 2013; Accepted March 25, 2013; Published March 28, 2013 | |
| Citation: Afzelius P, Iyer V, Lelkaitis G, Henriksen SD (2013) False-Negative 99mTc Medi-MIBI Parathyroid Scintigraphies: A Report on the Possible Role of Diagnostic Two-Phase Single-Acquisition CT. OMICS J Radiology. 2:112. doi: 10.4172/2167-7964.1000112 | |
| Copyright: © 2013 Afzelius P, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Radiology
Abstract
Introduction: Dual-phase 99mTc-Medi-MIBI parathyroid scintigraphy is often used for preoperative localization of
primary parathyroid adenomas. The overall accuracy has been reasonably high; however, some false-negative cases
occasionally occur. Two such cases are presented, and the advantages of adding two-phased single-acquisition
diagnostic CT to guide the surgeon are demonstrated.
Case presentations: A 54-year old male was admitted due to persistent elevated parathyroid hormone and
calcium concentrations in the blood despite medical treatment consistent with primary hyperparathyroidism. A dualphase
parathyroid scintigraphy performed 6 months earlier in another hospital was unable to confirm the diagnosis.
There was no change over time in levels of parathyroid hormone and calcium in the blood. In the second case, a 46-
year old woman was examined due to the same symptoms and findings; 18 months earlier she also had no retention
of tracer on late images. In this case, the patient also had had a CT performed, which showed morphological signs
of a parathyroid adenoma. We therefore planned dual-phase parathyroid scintigraphy with single-photon emission
computed tomography/computed tomography (SPECT/CT) in the early phase. The low-dose CT was unable to confirm
the impression of slight amounts of tracer uptake and retention at the lower right thyroid pole in both cases. Diagnostic
in both cases, but still with a low dose, the CT revealed a parathyroid adenoma situated in a common parathyroid
location at the lower pole of the right thyroid lobe, where activity retention was seen in late images. The surgeon was
able to perform minimally invasive neck surgery based on accurate anatomical localization of the adenoma.
Conclusion: This case report highlights the potential of two-phase single-acquisition CT as a useful tool in exact
localization of parathyroid adenoma for guiding the surgeon in minimally invasive surgery.
| Keywords |
| Parathyroid scintigraphy; Computed tomography; Primary hyperparathyroidism; false negative |
| Introduction |
| Dual-phase 99mTc- Methoxy-isobutyl-isonitril-Cu(I)-tetrafluoroborate (Medi-MIBI) parathyroid scintigraphy is often used for preoperative localization of primary parathyroid adenomas. The overall accuracy has been reasonably high; however, false-negative cases occasionally occur. We present two cases of initial false-negative scintigraphies. |
| Case Presentation |
| A 54-year old male was admitted due to persistently elevated parathyroid hormone (27.4, normal range 1.3-7.6 pmol/L) and free plasma calcium ion (1.72, normal range 1.18-1.32 mmol/L) concentrations in the blood despite medical treatment consistent with primary hyperparathyroidism. |
| A dual-phase parathyroid scintigraphy performed 6 months earlier in another hospital was unable to confirm the diagnosis. The parathyroid scintigraphy was a false-negative result. There were no changes over time in levels of parathyroid hormone and calcium in the blood. |
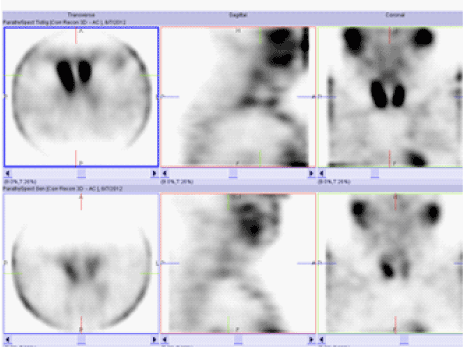
| After injection of 900 MBq 99mTc-Medi-MIBI, early (5 minutes) and late (2 hours) planar image acquisitions were performed [1] with low-dose SPECT/CT (Figure 1). |
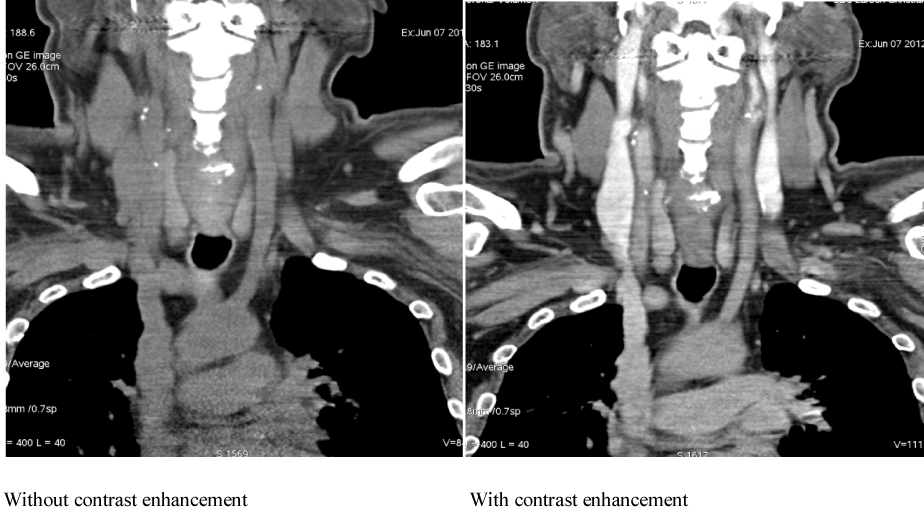
| Diagnostic two-phase (bolus injection after 15 sec and 30 sec.) CT single-acquisition (30 sec) of neck and chest was performed after injection of 25 ml and 60 ml Iomeron (140 mg I/ml) 2 hours after injection of 99mTc Medi-MIBI. |
| Parathyroid scintigraphy gave the impression of increased activity at the lower pole of the right thyroid lobe on early images, still remaining on late images (Figure 1). Low-dose SPECT-CT was not of a quality that convinced the radiologist of the existence of a parathyroid adenoma. Diagnostic CT with contrast enhancement, however, convincingly demonstrated a CT morphological correlate with contrast accumulation in a rounded, approximately 14 mm×5 mm structure situated paravertebrally and paraesophageally behind the lower pole of the right thyroid lobe at the level of the vertebral corpus of C7 (Figure 2). |
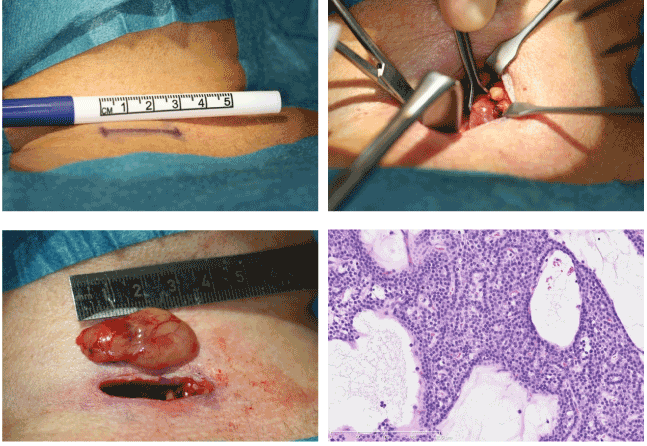
| Minimal neck surgery was performed, and an adenoma was removed at the described location. The concentration of parathyroid hormone dropped peroperatively to 4 pmol/L and of free plasma calcium ion to 1.47 mmol/L immediately after removal and to 1.3 pmol/L and 1.17 mmol/L six days after surgery. A histological examination confirmed the presence of a primary parathyroid adenoma (Figure 3). |
| In the second case, a 46-year old woman was examined because of symptoms of hyperparathyroidism supported by biochemical findings. The patient had been examined 18 months earlier with the same symptoms with no tracer retention found by parathyroid scintigraphy and the finding of a parathyroid adenoma on diagnostic CT. The adenoma was morphologically unchanged after 18 months, and so were biochemical markers and clinical symptoms, but now tracer retention was shown on the late scintigraphy. Minimal surgery was performed, an adenoma was removed, and the biochemical parameters were normalized. |
| Discussion |
| In 2012, Ciappuccini et al. reported that using dual-phase scintigraphy radioisotope technetium-99mwith the ligand methoxyisobutylisonitrile (MIBI) and neck and thorax SPECT/CT in primary hyperparathyroidism enables detection of two thirds of the adenomas [2]. Sensitivity of 92% (95% CI: 80-98) and a specificity of 83% (95% CI: 36-100). The likelihood of finding a parathyroid adenoma on a scintigraphy was associated with levels of concentrations of PTH and calcium [3] and size of adenoma. |
| In nearly 90% of patients with primary hyperparathyroidism, the underlying cause is a solitary adenoma [4]. To minimize the duration of surgery and the risk of complications, a focused approach with unilateral cervical exploration and removal of the preoperatively identified adenoma is preferable. |
| Recently, Hunter et al. demonstrated that a four-dimensional CT lateralized the abnormal glands with 93.7% accuracy (134 of 143), and the accuracy of localization according to quadrant was 86.6% (116 of 134). However, the effective ionizing radiation dose to the patient was rather high; about 27 mSv [5]. |
| Parathyroid scintigraphy and diagnostic CT may be a possible examination alternative prior to surgery, aiding the surgeons with exact localization of adenomas in unusual sites and providing not only the side, but also the upper or lower position of the adenoma. This allows minimally invasive neck surgery to be performed, saving time and causing less inconvenience to the patient due to a more accurate localization of an adenoma. |
| The factor most commonly reported to correlate with falsenegative findings is the size of the parathyroid gland; that is, adenomas are less likely to be detected in smaller glands than in larger glands. In the first presented case, the tumor size may be an explanation, but the calcium and PTH levels, however, did not change over time. |
| 99mTc MIBI consists of lipophilic cationic molecules. After intravenous injection, the molecules are distributed according to blood flow in the body, cross the cell membranes by passive diffusion, and become concentrated intra cellularly in the region of the mitochondria. The ability to detect parathyroid adenomas and hyperplastic parathyroid glands is related to the presence of mitochrondria-rich oxyphil cells [6]. In the cases presented there were no histological signs of oxyphil cells, and the influence of other factors cannot be excluded. Variability of radiotracer uptake in parathyroid adenomas is another factor reported in addition to oxyphil cell content to which differences in perfusion and metabolic activity, P-glycoprotein expression, and multidrug resistance–related protein expression, and cell cycle may be attributed [7-12]. |
| If supplemental morphological examination (CT) had been performed initially in the first case and trusted in both the first and the second case despite false-negative parathyroid scintigraphies, minimally invasive surgery could have been performed at an earlier stage, and the patients in our cases could have been free of symptoms and inconvenience 6 and 18 months earlier. |
| In conclusion, we suggest that when available, two-phased parathyroid scintigraphy is supplemented with SPECT-CT. It remains to be examined whether SPECT with low-dose or diagnostic CT with contrast enhancement is better. We have minimized the effective dose of diagnostic CT with contrast to 4.8 mSv and have planned a prospective consecutive study to rule out this matter. |
References |
|
--
Figures at a glance
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 |
Relevant Topics
- Abdominal Radiology
- AI in Radiology
- Breast Imaging
- Cardiovascular Radiology
- Chest Radiology
- Clinical Radiology
- CT Imaging
- Diagnostic Radiology
- Emergency Radiology
- Fluoroscopy Radiology
- General Radiology
- Genitourinary Radiology
- Interventional Radiology Techniques
- Mammography
- Minimal Invasive surgery
- Musculoskeletal Radiology
- Neuroradiology
- Neuroradiology Advances
- Oral and Maxillofacial Radiology
- Radiography
- Radiology Imaging
- Surgical Radiology
- Tele Radiology
- Therapeutic Radiology
Recommended Journals
Article Tools
Article Usage
- Total views: 14277
- [From(publication date):
March-2013 - Aug 30, 2025] - Breakdown by view type
- HTML page views : 9622
- PDF downloads : 4655
