Case Report Open Access
Huge Bilateral Mature Cystic Teratoma in Adolescence: A Case Report and Review of Literature
Hamadeh Sameer*, Addas Bishr, Hamadeh Nasreen, Rahman Jessica and Rahman M.S
Obstetrics and Gynaecology Department, King Fahd Hospital of the University, Alkhobar, Kingdom of Saudi Arabia
- *Corresponding Author:
- Dr. Sameer Hamadeh
Obstetrics and Gynaecology Department
King Fahd Hospital of the University
Alkhobar, Kingdom of Saudi Arabia
Tel: 00966502181513
E-mail: sameer_hamadeh@hotmail.com
Received date: June 07, 2016; Accepted date: June 13, 2016; Published date: June 23, 2016
Citation: Sameer H, Bishr A, Nasreen H, Jessica R, Rahman MS (2016) Huge Bilateral Mature Cystic Teratoma in Adolescence: A Case Report and Review of Literature. Adv Oncol Res Treat 1: 108. doi: 10.4172/2572-5025.1000108
Copyright: © 2016 Sameer H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Oncology Research and Treatment
Abstract
Mature cystic teratoma is a benign tumor of the ovary arising from germ cells. It can occur at any age but, commonly in patients between 20 and 40 years. It is usually unilateral. The size of the tumor is relatively small at the time of diagnosis. An unusual presentation of mature cystic teratoma considering age of the patient, diagnosis and features of the tumor, is described, which to our knowledge has not been reported before in the literature.
Keywords
Mature cystic teratoma; Huge; Bilateral; Adolescence
Introduction
The incidence of mature cystic teratoma is 10-20% of all ovarian tumor [1,2]. It is usually unilateral, and bilateral in 10-15% of cases [3], commonly seen in patients between 20 and 40 of age. Size of this tumor rarely exceeds 10 cm [4]. An unusual presentation of bilateral mature cystic teratoma in a young adolescent patient is described.
Case presentation
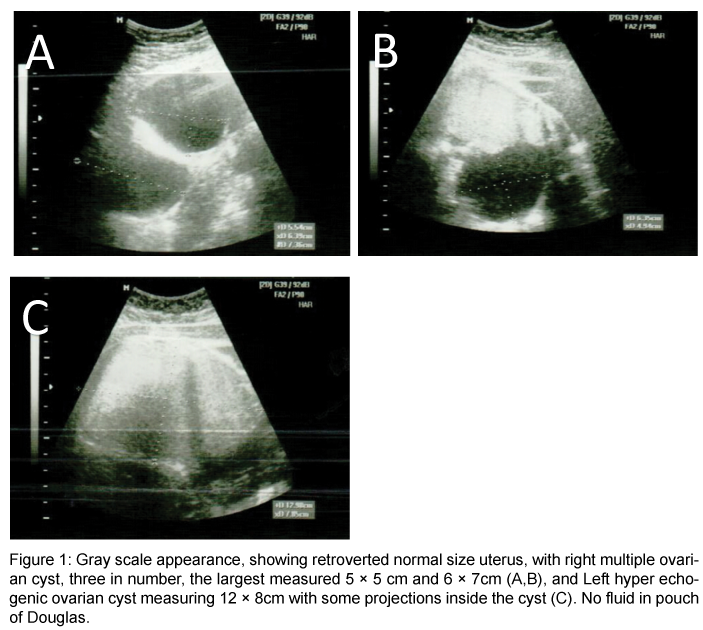
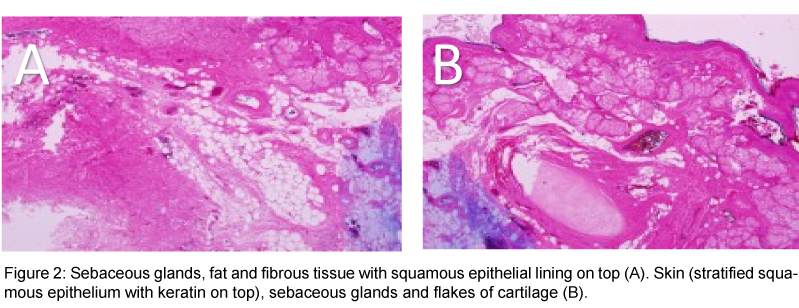
A 13 years old, single female, presented to our emergency room complaining of generalized abdominal pain for two weeks. It was colicky in nature, progressive in intensity over time, with no history of fever, nausea, vomiting, or changes in bowel habits. She did not notice any abdominal distension or changes in weight, but, complained of dysuria for two weeks. Her menarche was two years ago and regular menstruation for the past elven months. The vital signs were within normal. A palpable pelvic-abdominal mass reaching up to the umbilicus, non-tender, mobile with no skin changes was found on abdominal examination. Ultrasound of the abdomen and pelvis revealed a normal, retroverted uterus, three multiple, right sided ovarian cyst, largest measuring 6.3 × 7.3 cm and 5.6 × 6.3 cm, and Left hyper-echogenic ovarian cyst measuring 12.5 × 7.8 cm with some projections inside the cavity. There was no fluid in pouch of Douglas (Figure 1). Abdominal and pelvic CT showed a large, well defined, multiloculated cystic adnexal mass 12.1 × 7.5 × 13 cm in size, most likely arising from left ovary, occupying the whole pelvis and pushing the uterus to the right, antero-laterally and sigmoid colon left laterally, causing left hydronephrosis and hydroureter. The lesion showed mixed component with fat fluid level, and Rokitansky ball seen within it, along with foci of calcification noted in the wall, that represented left ovarian dermoid cyst. Other similar characteristics lesions were noted in higher cuts measuring, approximately 10.5 × 5.6 × 12 cm in size, corresponding to L5 vertebral body and extending superiorly to level of the renal hilum, occupying the right side of the abdomen and pushing the ascending colon posteriorly. No obvious infiltration to adjacent structures was noted. No lymphadenopathy or ascites was noted. Chest x-ray and tumor markers were within normal limits. The guardian of the patient were advised to consent for laparotomy, after full explanation if the possible operative procedures on entering the abdomen, which they agreed and signed. A midline sub-umbilical incision was made to enter the peritoneal cavity. Minimal serous fluid in peritoneal cavity was aspirated and sent for cytology. Bilateral, lobulated, ovarian cysts were found; right one measured 15 × 10 cm, left measured 12 × 9 cm. The uterus and fallopian tubes were normal. Bilateral ovarian cystectomy was carried out with preservation of adequate normal ovarian tissue. The cytology report of peritoneal fluid was negative for malignant cells. Histopathology confirmed bilateral mature cystic teratoma (Figure 2). The patient recovered normally post operation and was discharged home after 5 days. She was followed up in the outpatient clinic for the next two years without complaints or abnormal findings on clinical and ultrasound checks.
Figure 1: Gray scale appearance, showing retroverted normal size uterus, with right multiple ovarian cyst, three in number, the largest measured 5 × 5 cm and 6 × 7cm (A,B), and Left hyper echogenic ovarian cyst measuring 12 × 8cm with some projections inside the cyst (C). No fluid in pouch of Douglas.
Discussion
The incidence of mature cystic teratoma is 20-25% of all ovarian tumors [2]. It is usually unilateral, and bilateral in small percentage of patients [3]. This lesion is commonly seen in young women of childbearing age, and rarely in very young adolescents. Mature cystic teratoma rarely grows more than 10 cm [4]. It can be diagnosed by ultrasound based on its specific features [5]. CT scan may be reserved to visualize the nature of large size tumors, when suspicion of malignancy is present. Mature cystic teratoma is usually asymptomatic and rarely causes symptoms unless it undergoes torsion or pressure symptoms resulting from increasing size of the tumor. The tumor is usually managed by cystectomy or oophorectomy, performed laparoscopically or via laparotomy, depending on the patients age, fertility, cosmetic issues, ovarian tissue reserved and if one or both ovaries affected [6,7]. The preservation of ovarian tissue is highly important in patients with bilateral pathology. The percentage for malignant transformation is 0.2-2% [8]. Mature cystic teratoma at 13 years of age in the patient described, is considered to be rare, especially bilaterally with tumor size >10 cm in each ovary. The lowest age reported was 9 years old in two patients [9,10]. One of them had a unilateral mass and the other was bilateral, with tumor size <10 cm in both cases. Mature cystic teratoma with synchronous immature teratoma in the opposite ovary in a 9-years-old girl has been reported in the literature [10]. Multiple, bilateral ovarian dermoid cyst <10 cm have been reported in the past [11-13]. Bilateral mature cystic teratoma >10 cm in a 35-years old patient has been reported by El-Agwany [14]. CT scan was of great value in the diagnosis of our case because of the size of the cysts and had to be managed by laparotomy. Recurrence may occur 1-15 years after operation [15]. Long term recurrence rate of 4.2% after surgical excision of mature cystic teratoma was reported in one study [16]. Young age, bilaterally, and large cyst size >8 cm were shown to be significant predictive factors. When a patient had all these three factors, the recurrence rate was 21.0% [16]. Our patient was followed up with ultrasoundperiodically and advised to have further checks in the future, considering her age and bilateral tumours more than 10 cm in size.
Conclusion and Recommendations
This case report is a rare presentation of mature cystic teratoma in adolescence which is a definite entity in the differential diagnoses of abdominal pain with pelvic-abdominal mass in young females. Long term fellow up of this patient with significant predictive factors is advised due to higher incidence of recurrence in the future.
Acknowledgement
To the patients who provided us, signed permission to report this case for publications.
References
- Suclly RE, Young RH, Clement PB (1998) Tumor of the ovary, maldeveloped gonads, fallopian tube and broad ligament. Atlas of tumor pathology. Third series, fascile 23. Wahington, DC: Armed Forces Institute of Pathology.
- Peterson WF, Prevost EC, Edmunds FT, Hundley JM Jr, Morris FK (1955) Benign cystic teratoma of the ovary: a clinco-stastistical study of 1007cases with review of the literature. Am J Obstet Gynecol 70: 368-82.
- Einarson JI, Edwards CL, Zurawin RK (2004) Immature ovarian teratoma in adolescence: A case report and review of literature. J Pediatr Adolesc Gynecol 17:187-9
- Comerci JT Jr, Licciardi F, Bregh PA, Gregorgi C, Breen JL (1994) Mature Cystic Trtatoma: a clinicopathologic evaluation of 517 cases and review of literature. Obstet Gynecol 84: 22-28.
- Patel MD, Feldstein VA, Lipson SD, Chen DC, Filly RA (1998) Cystic teratoma of the ovary: diagnostic value of sonography. AJR Am J Roentgenol 17: 1061-1065.
- Zanette G, Ferrari L, Mignini-Renzini M, Vignali M, Fadini R (1999) Laparoscopic excision of ovarian dermoid cyst with controlled intraoperative spillage. Safety and effectiveness. J Reprod Med 44: 815-820.
- Silva PD, Ripple J (1996) Outpatient minilaparotomy ovarian cystectomy for bening teratoma in teenagers. J Pediatr Surg 31: 1383-1386.
- Singh P, Yordan EL, Wilbanks GD, Miller AW, Wee A (1988) Malignancy asscoaited with benign cystic teratomas of the ovary. Singapore Med J 29: 30-34.
- Iwata A, Matsubara K, Umemoto Y, Hashimoto K, Fukaya T (2009) Spontaneous rupture of benign ovarian cystic teratoma in a premenarcheal girl. J Pediatr Adolesc Gynecol 22: e121-123.
- Sai Prasad BV, Md K Faheem N, Indrani G, Vittal Mohan P, Sreedhar Babu KV, et al. (2014) Mature cystic teratoma with synchronous immature teratoma of opposite ovary in a nine year old girl - a varied presentation of common tumor: A case report with review of literature 2: 75-80.
- Pepe F, Lo Monaco S, Rapisarda F, Raciti G, Genovese C, et al. (2014) An unusual case of multiple and bilateral ovarian dermoid cysts. Case report. G Chir 35: 75-77.
- Sinha R, Sethi S, Mahajan C, Bindra V (2010) Multiple and bilateral dermoids: a case report. J Minim Invasive Gynecol 17: 235-238.
- Bournas N, Varras M, Kassanos D, Chrelias Ch, Tzaida O, et al. (2004) Multiple dermoid cysts within the same ovary: our experience of a rare case with review of the literature. Clin Exp Obstet Gynecol 31: 305-308.
- El-agwany A, Moneim AA (2015) Multiple bilateral huge synchronous ovarian mature cytic teratomas: A rarely encountered condition in practice. Egyption J Radiol Nuclear Med 46: 15-197
- Alanbay I, Coksuer H, Ercan M, Karashin E, Keskin U (2011) Multiple recurrent cystic teratoma of the same ovary: Acase report and literature review. Med J Kocatepe 12: 8-12.
- Harda M, Osuga Y, Fujimoto A, Fujimoto A, Fujii T, et al. (2013) Predictive factors for recurrence of ovarian mature cystic teratoma after surgical excisions. Eur J Obstet Gynecol Reprod Biol 171: 325-32 8.
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 15093
- [From(publication date):
June-2016 - Aug 19, 2025] - Breakdown by view type
- HTML page views : 14056
- PDF downloads : 1037