Research Article Open Access
Kinesiology Taping in Cervical Vertigo Treatment
| Kulczy�?�?ska Katarzyna1, Pawlak-Osi�?�?ska Katarzyna1, Ka�?ºmierczak Henryk3, Pujanek Zuzanna3*, Rzewnicki Ireneusz2 and Ma�?�?gorzata Pyskir4 | |
| 1Department of Hearing and Vestibular Pathophysiology, Collegium Medicum Nicolaus Copernicus University, Bydgoszcz, Poland | |
| 2Department of Otolaryngology, Medical University of Bialystok, Poland | |
| 3Department of Otolaryngology, Head and Neck Surgery and Laryngological Oncology, Jurasz’s Hospital, Poland | |
| 4Departement of Physiotherapy, Collegium Medicum Nicolaus Copernicus University, Bydgoszcz, Poland | |
| *Corresponding Author : | Pujanek Zuzanna Department of Otolaryngology Head and Neck Surgery and Laryngological Oncology Jurasz’s Hospital, Sklodowska-Curie Street 9, 85-094 Bydgoszcz Tel: +48693716894 E-mail: zpujanek@vp.pl |
| Received February 03, 2016; Accepted March 22, 2016; Published March 31, 2016 | |
| Citation: Katarzyna K, Katarzyna PO, Zuzanna P, Ireneusz R, Henryk K, et al. (2016) Kinesiology Taping in Cervical Vertigo Treatment. J Nov Physiother 6:287. doi:10.4172/2165-7025.1000287 | |
| Copyright: © 2016 Katarzyna K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Novel Physiotherapies
Abstract
Introduction: In otoneurological clinical practice, cervical vertigo is one of the most common vestibular disorders.
Purpose: The aim of this study was to evaluate the effectiveness of Kinesiology Taping in patients with cervical vertigo syndrome, based on an objective assessment of spinal conduction from the balance system sensory receptor (SEP test), a postural control based on a cranio-corpography (CCG test) and Freyss’ dynamic stabilometry.
Methods: The research covered 74 patients. Through medical examination all the patients were diagnosed with vertigo of somatosensory etiology (disturbed somatosensory evoked potentials – SEP on a cervical level) or of mixed etiology (disturbed SEP and vasogenic cervical disorders). Kinesiology Taping, using Strips by Nitto Denko Kinesiology Tape / K-Active Tape, was applied to both groups of patients. Somatosensory evoked potential (SEP) test, craniocorpography (CCG), Freyss’ stabilometry test were performed before and after therapy.
Results: The results were compared before and after kinesiotaping in patients and between the patients and control group of healthy subjects. With regard to the SEP test, waves N13, P11 and P27 latency measurement results obtained after rehabilitation did not show any statistically important differences, as compared with the control group. In the case of the CCG examination there was no improvement after rehabilitation. Significant differences were observed on Freyss’ stabilometry under the condition of visual control and comparing the groups of strictly somatosensory and mixed cervical vertigo.
Conclusions: In patients with cervical vertigo, the applied Kinesiology Taping therapy did not have an impact on the objectively measured parameters of SEP, but caused the positive effect on balance coordination measured by stabilometry. Patients with solely somatosensory etiology of balance disorders responded better to the taping therapy than patients from the mixed etiology group.
| Keywords |
| Cervical proprioception; Cervical vertigo; Kinesiology taping; Stabilometry; Somatosensory evoked potentials; Balance disorders |
| Introduction |
| In clinical practice, cervical vertigo is among the most common vestibular disorders. Neuhauser [1] reported that that vertigo/dizziness had a prevalence of 22.9% in the last 12 months and an incidence of 3.1% of respondents in Germany. |
| The definition includes location of dysfunction, which sheds light on the neck as the region of detailed diagnostic tests. Cervical spine consists of subsections whose mechanisms are closely involved in the very balance control [2,3]. Deep sensory conduction disorders seem to be the most important cause. Incredible wealth of proprioceptors proven to exist in soft tissues of cervical spine results in high likelihood of damaging them, which in turn will manifest itself in balance disorders [4,5]. |
| In 1946, Cawthorne [6] and Cooksey [7] established the physical rehabilitation therapy as a form of replacement therapy of the sense of balance, and they applied it in patients after labyrinth surgeries. For decades two rehabilitation trends were mainly used, which referred only to labyrinth damage [8]. With advances in electrophysiological studies, more attention was given to the significance of sight and proprioception in vestibular dysfunction compensatory processes. |
| Cervical vertigo is a peculiar form of vertigo, and a detailed vestibular diagnostics is fundamental for the diagnosis, choosing the type of rehabilitation, and further treatment. The most important goal in terms of improvement should be integration of three canals of the balance system, including a multisensory system effector – a locomotor organ, where the very cervical spine generates afferent vestibular disorders [9,10]. |
| Nowadays, physiotherapy gives access to diverse forms of therapy, helping both the treating and the treated sides to fight system dysfunctions. One of the examples includes Kinesiology Taping, which is now being rediscovered (though the method has been well-known internationally since 1970s), i.e. a therapeutic method developed in Japan, which consists in taping the body with specialist cotton strips designed specifically for this technique [11]. The originality of this technique stems from a highly specialised Kinesio Tex Tape® strip with technological parameters as close as possible to the parameters of human skin (i.e. thickness, weight, flexibility). An incredible advantage of this method is its 24-hour continuity, and it is sometimes described as a round-the-clock presence of the therapist’s hand touch. Kinesiology Taping was developed with the idea of relieving pain and providing support to accelerate recovery of overstrained soft tissues, and its suggested effects include proprioceptive facilitation, inhibition of pain, and normalization of muscle tone, oedema therapy enhancement, and blood circulation improvement [12]. |
| The aim of this study was to evaluate the effectiveness of Kinesiology Taping in patients with cervical vertigo syndrome, based on an objective assessment of spinal conduction from the balance system sensory receptor (SEP test), a postural control based on a cranio-cartography (CCG test), a course of reaction in disturbed somatosensory function based on Freyss dynamic stabilometry and analysis of the impact of the cause of cervical vertigo on the results of applied rehabilitation method. |
| Material and Method |
| Ethics |
| All human subjects studies have been approved by the appropriate ethics committee and have therefore been performed in accordance with the ethical standards of the responsible committee on human experimentation (institutional or regional) and with the Helsinki Declaration of 1975, which was revised in 1983. |
| The research covered 74 patients (50 female, 24 male), aged 18 to 66 suffering from vertigo. There were the patients of The Dpt. of Hearing and Balance Patophysiology, Otolaryngological Clinic. Through medical examination vertigo were classified as being of somatosensory origin (disturbed somatosensory evoked potentials – SEP on a cervical level) or of mixed etiology (disturbed SEP together with vasogenic cervical disorders). Such a division created two groups of subjects depending on a somatosensory component (38 people, 25 female, 13 male, aged from 19 to 64, average age 45,6) and on a cervicogenic mixed etiology (36 people, 25 female, 11 male, aged from 18 to 66, average age 44,8), 24 women and 37 men. The height in both groups was average 162, 7 - 184, 9 cm, weight: 53, 1- 89, 4 kg (BMI<24, 99). |
| The clinical picture for people with somatosensory vertigo obtained (apart from SEP) through radiological examination of cervical spine included: discopathy, spondylosis, ligamentous laxities, bone block, spondyloarthritis, osteophytosis. Also, medical diagnoses indicated post-traumatic and post-neurosurgical conditions in cervical spine. |
| In patients from the mixed etiology group, somatosensory background coexisted with vascular background, particularly of cervical origin, i.e. artheroslerosis of common carotid arteries, blood flow disorders in carotid arteries, narrowing or tortuous arteries, developmental anomalies and systemic vascular diseases: high blood pressure with vascular pathology of the encephalon, angiopathy of small blood vessels, anaemia, arrhythmia, lipidoses. |
| A clinical control group consisted of 61 people (24 female, 37 male, aged 22- 62, average age 47, 0) with no otoneurological disorders. They have never complained about vertigo, balance disorders and hearing loss. The height in control group was 160, 2-183, 5 cm, weight average: from 50, 3-90, 2 kg (BMI<24, 99). |
| All patients were subjected to Kinesiology Taping rehabilitation. Only one physiotherapist was involved in research and application the KT. The physiotherapist completed the kinesiology taping basic course, according to the standards of the K-Active Association in Warsaw 2008 and during the research has got 2 year experience in KT method and five years experience with otoneurological patients. |
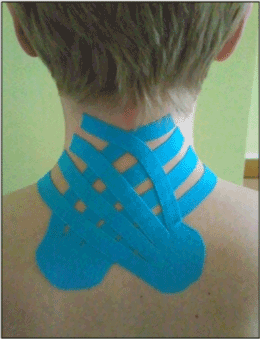
| Strips by Nitto Denko Kinesiology Tape / K-Active Tape were used. One type of application was used – a technique following a whiplash injury, where bases were stuck in the area of upper angles of shoulder blades with the head in a natural position; in bending position tails with a 25% strip tension were applied. The idea was to make the impact on not necessary particular muscles but rather neck area themself, to threat patients with many different causes of cervical vertigo without particular the same etiology. Time of application was between 8 and 15 days (average of 12.6 days). The length of application time was determinate by various frequencies of vertigo episodes among patients, where vertigo incidents have been reported over one to two weeks. Simultaneously the answer from the nervous system as some changes in SEP test was expected to show as a results of trophic and blood circulation improvement and proprioceptive facilitation. It was assumed that such changes might need longer than average time of tape application (Figure 1). |
| To check the efficiency of Kinesiology Taping, a series of specialist tests were performed before launching the rehabilitation and after the therapy. The following tests were carried out: somatosensory evoked potential (SEP) test, craniocorpography (CCG), Freyss’ stabilometry test. |
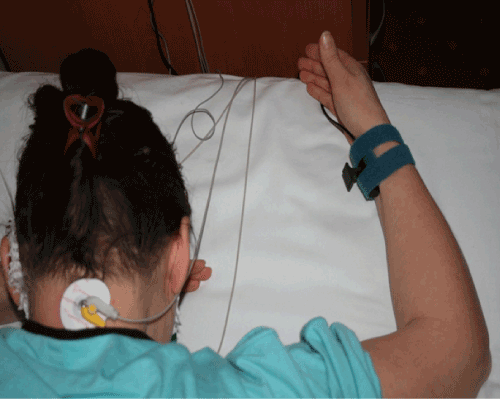
| SEP tests were performed on the Centor- C device (Ratia-Alvar, France), through percutaneous electrical stimulation of the median nerve of the right upper limb in the carpal tunnel. Cathode was placed proximally to the anode. Grounding electrode was placed on a cheek; impedance of electrodes below 5,000 ohms. During the stimulation, the force slightly exceeded the motor excitability threshold assessed based on the thumb movements. |
| The following test parameters were applied: frequency of stimulation – 3.1 Hz, time basis – 60 ms, time of a single impulse 0.1 ms, reception sensitivity – 100 uV, filters – 3.1 Hz and 1.6 kHz, the number of obtained responses for averaging the final record – 300 (according to “Recommendations for the practice of clinical neurophysiology: guidelines of the International Federation of Clinical Neurophysiology, 1999”). |
| Receptive electrodes were located in accordance with the system of EEG electrode assembly 10-20 above the olecranon process C5, the front electrode above point Cz, the parietal electrode above point C3`. |
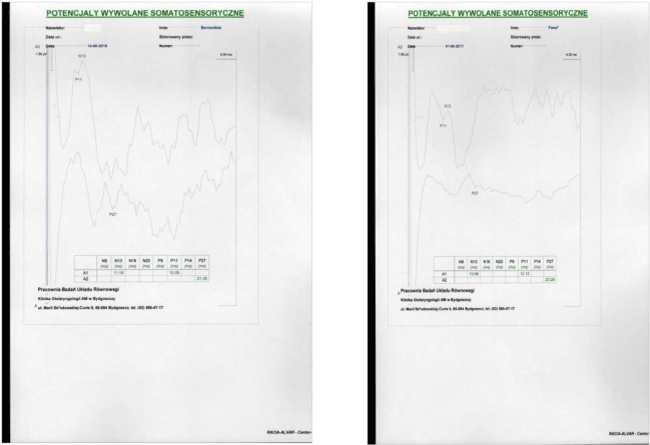
| Latency measurements of waves P11 and N13 were made from above dorsal roots of the spinal cord and postsynaptic potential from the grey matter of dorsal horns, and wave P27 from above the sensory area of parietal cortex. Morphology and time of wave formation was assessed, which determined efficiency or the presence of impaired sensory conduction (Figure 2). |
| Craniocorpography is a quantitative analysis of Romberg’s and Unterberger’s tests, used to assess the performance of the effector sense of balance. It was carried out with the use of Zebris- Win Balance CMS 10 Measuring System for 3D-Motion Analysis device (Zebris Medical GmbH, Germany), where the patient was equipped in 5 movement sensors: 2 on a helmet, 1 on each of the shoulders, 1 on a lumbar spine. |
| During the statistical test, data were obtained on the range of lateral and longitudinal inclinations of the body, the angle of the twist of the neck and the surface area of frontal inclinations (Figure 3). A walk test provided information on the distance walked from the starting point, about the range of lateral inclinations of shoulders during a step, angular deviations from the starting point and the angle of rotation of the entire body. |
| Freyss’ stabilometry tests the ability to maintain balance on an unstable ground. The Synapsys STABILO platform (Schaevitz Accustar Electronic Clinometer, Lucas Control Systems, USA) was used for the analysis. The device consists of a mobile platform placed on a cylindrical base carrying the patient. The analysis covers passive inclinations of ± 15° front-to-back, side-to-side sequence in relation to the level. The maximum and average inclination range is measured and recorded in degrees (A max, Aav), and the average rotating speed of the platform (Vav) is recorded in degrees/s to the nearest 0.1 degree/s. A motion detector is placed on the patient’s head and the measurement of the average rotating speed of the head is taken (Vavh). |
| The test comprises 4 sequences, 20 seconds each. At the first stage, the platform’s mobility was set in the sagittal plane body position. The patient is standing still for 20 seconds with his or her eyes open, and then for 20 seconds with the eyes closed. The third and fourth test sequence considered mobility in the frontal plane; as in the previous case, the test was carried out with and without the visual control. The method allows for recording involuntary, corrective responses, stabilising the posture in disturbed somatosensory conditions, where the value of parameters increases in the case of disturbance. |
| Results |
| The following abbreviations are used in tables: |
| CI – Confidence Interval, C – Confidence, LS – Level of Significance, SD – Standard Deviation, SE – Standard Error, DF – Degrees of Freedom, t – The Value of Statistics According to the Particular Patterns, p – Probability, Min. – Minimal Value, Max. – Maximal Value, Mean – Mean Value, N – Number of Proofs. |
| Somatosensory evoked potentials (SEP) |
| With regard to the SEP test, the normality of the results derivation was checked using the Shapiro-Wilk test. In the patients, the normal derivation was noted for the variables P11 i P27; the variable N13 was not subject to normal derivation. In control group all the variables were not subjected to normal derivation. The variables subjecting to normal deviation were analyzed using t-test (Table 1). |
| There was no statistical differences between latencies of the waves P11 and P27 before and after rehabilitation (at the statistical significance <0,05). |
| The variables that were not subjected to normal derivation were compared using Wilcoxon test (Table 2). |
| There was no statistical difference before and after rehabilitation in the wave N13 latency. |
| The results of the latencies of the SEP in healthy group and in patients were compared using non-parametric statistical Wald- Wolfowitz test (Table 3). |
| There was the significant changes (p<0,05) between the latency of P11 waves . This difference remained after therapy. |
| Craniocorpography |
| The following abbreviations are used for parameters of craniocorpography in tables: the range of lateral (LaSW) and longitudinal (LoSW) inclinations of the body, the angle of the twist of the neck (TA) and the surface area of frontal inclinations (FCA); the distance walked from the starting point (LD), the range of lateral inclinations of shoulders (LSW) during a step, angular deviations (SS) from the starting point and the angle of rotation (AD) of the entire body. |
| Romberg test |
| On Shapiro-Wilk test, in the patients, the normal derivation was noted only for the variable P TA; the others were not subjected to normal derivation. |
| The variables not subjecting to normal derivation were compared using Wilcoxon test (Table 4). |
| There were no statistical differences before and after rehabilitation. |
| Dynamic testing (walk test) |
| The variables not subjecting to normal derivation were compared using Wilcoxon test (Table 5). |
| The parameters did not change significantly after rehabilitation. |
| The variables (AD) with normal derivation were compared using t-test (Table 6). |
| There was no statistical difference before and after rehabilitation. |
| The comparison between control group and patients demonstrated the difference of the lateral inclinations of shoulders (LSW) during the step (dynamic test) after the application of taping. In the control group, its value is significantly lower (better) than in the taping group. The remaining parameters showed no significant differences after rehabilitation. |
| Stabilometry |
| The following abbreviations are used for parameters of stabilometry in the tables: |
| Amax- maximal inclination of the platform, Aav – average inclination of the platform, Vav - average rotating speed of the platform, Vavh - average rotating speed of the head. Stabilometry with eyes open |
| All variables were not subjected to normal derivation during the mobility of the platform both in saggital and frontal planes. They were tested using Wilcoxon test (Table 7). |
| The only statistical difference was noted for the average inclination of the platform (Aav). It was smaller that means better after kinesiotaping (Table 8). |
| The only statistical difference was noted for the maximal inclination of the platform (Amax)- it was better after kinesiotaping (Table 9). |
| Table 9 shows statistically significant differences for the stabilometry test parameters for groups of patients with somatosensory and mixed etymology of vertigo after rehabilitation. |
| The existence of significant statistical differences was observed in cases where the value of parameters changed, where all of them were significantly lower for patients with mixed etymology of vertigo should be higher. Statistically significant differences were obtained with: |
| • Change of the average speed of the platform (Vav). moving in a front-to-back direction, when the patient’s eyes were closed. |
| • Change in the maximum range of platform Amax, with a side to side mobility and eyes open. |
| • Change Amax with a left to right platform mobility, without any visual control. |
| In the case of the remaining parameters, no statistically significant differences were determined (Table 9). |
| In the group of healthy individuals and the research group, parameters (Table 10 excluding Aav and Vavh with a side to side mobility and eyes open) showed significant differences. Statistically significant differences were obtained with: |
| • Amax, Aav, Vav, Vavh with a front-to-back platform mobility, with eyes open and closed |
| • Amax, Vav, with a side-to-side platform mobility and visual control |
| • Amax, Aav, Vav, Vavh with a side-to-side platform mobility and with eyes closed in the control group the values were significantly lower |
| Significant differences were also observed after rehabilitation for the Aav front-to-back parameter, eyes open, where in the taping group its value was significantly lower (better) than in the group of healthy individuals. |
| Discussion |
| The balance analysis in the patients suffering from cervical vertigo seems to be essential due to the high frequency of occurrence of this type of vertigo and because of various efficiency of a variety of therapies and difficulties in objective monitoring of symptoms. |
| Somatosensory evoked potential test shows an objective condition of sensory conduction, and this paper presents the analysis of such conduction on a cervical level. |
| Results did not show any statistically significant changes in the latency of somatosensory potentials when Kinesiology Taping was applied. The primary assumption of this paper that Kinesiology Taping may influence the shaping of spinal response in the place of cervical application turned out to be experimental and did not improve somatosensory potential parameters in the research group. The applied method is relatively innovative and, as demonstrated by the results, its positive assessment is based on subjective impressions of the patient. |
| Academic literature lacks information on the SEP test in patients who had undergone taping treatment, in particular in patients with cervicogenic vertigo. Analysing sensory conduction among sportsmen and in the group of people with sedentary lifestyle, Bulut et al. [13] noticed a decrease in the potential latency values and a simultaneous decrease in their range after workout on a treadmill. Results pointed out to the significance of intense and systematic physical exercise in shaping somatosensory potentials. |
| Literature points out to the impact of other techniques, such as manual therapy, on shaping of sensory evoked potentials. Haavik- Taylor et al. [14] describe a significant decrease in the range of waves N20 and N30 after manipulation treatment on dysfunctional cervical spine joints. It may prove the existence of temporary impact on changes in cortical plasticity, illustrated by a decrease in the range of somatosensory potentials. |
| It may be presumed that Kinesiology Taping influences surface structures of the neck too shallowly to interfere in the structures of the core, as was the case in the manual therapy. May be, the duration of successful taping is essential- we tried to unify the patients’ group for the technique of application, duration of rehabilitation and etiology of vertigo (cervical) – under such circumstances it was difficult to collect adequately numerous subgroups. |
| To obtain a comprehensive assessment of the static and motor efficiency of the balance system, posturographic tests were used [15,16]. In this paper, a combination of the Freyss’ stabilometry with the use of the mobile platform and the CCG test, particularly while marching – seems to give exhaustive answers to questions concerning the condition of ‘multisensory’ balance. |
| Craniocorpography results obtained through this research showed that tested groups differed significantly from the healthy subjects on the base of parameter “lateral inclinations of shoulders during the step”. Its value was significantly better in the control group than in the group treated with Kinesiology Taping. Alpini et al. [17] described the CCG test of mobile sequence in patients diagnosed with whiplash injury, as compared with healthy individuals. They found out that the subjects demonstrated abnormal motor strategies, mainly decreasing head stability, reduced body movement, paradoxal excessive stabilisation, referred to as the collar effect. Soto Varela et al. [18] analysed the CCG of Romberg test in patients with cervical vertigo, labyrinth pathology and in healthy individuals. It turned out that head movements were as much as 67% more frequent for the group with cervical vertigo than in patients with labyrinth pathology (27%) and in healthy individuals (31%). |
| In the case of Freyss’ stabilometry test, when compared with healthy subjects-only one parameter – the average range of platform with front-to-back movement and eyes open after Kinesiology Taping rehabilitation – had a significantly lower value, i.e. a value which was better than in healthy individuals. This variable accompanied by maximal inclination the platform improved when taking into consideration the values before and after rehabilitation in patients’ group. This observation shows positive effect of kinesiotaping on balance coordination providing the proper visual impact. The craniocorpography, demonstrating no influence of taping, was performed under the more difficult circumstances, with eyes closed, so its results were worse than Freyss’ stabilometry. Osinski et al. [19] noted the improvement in posture coordination on Freyss’ platform in patients with proprioceptive vertigo who underwent neurosurgical fixation of the cervical spine, but only in a particular period: from one month to one year after surgery. Open eyes additionally supported the posture control [19]. |
| Sitko et al. [20] describe the results of both physiotherapy and manual therapy in patients with cervicogenic vertigo. After treatments, the tested body stability was statistically characterised by significantly smaller area of inclinations in the sagital plane when patients used visual coordination. These results were similar to our observation. Apart from positive impact of visual control one should regard the better men adaptation to the motion in sagital than in frontal plane. |
| When comparing the values of changes in Freyss’ stabilometry parameters, depending on the cause of vertigo, significant differences were identified in three parameters of the analysis: patients from the somatosensory group reacted slightly better to the taping therapy. It indicates the real effect of kinesiotaping on proprioceptive element of the neck and encourages us to select the patients with strictly somatosensory origin of vertigo for this kind of rehabilitation. |
| Thus, changes in the values of parameters both before undertaking therapy and afterwards show a partial impact of Kinesiology Taping on the vestibular condition. Noree et al. [21] claim that the quality of correct postural reflexes is influenced by a variety of cervical mechanoreceptors, where an abnormal afferent stimuli causes delivery of wrong information on the state of balance. The objective influence on cervical afferent pathway on the base of SEP-analysis was not confirmed in this study. Still, other aspects of Kinesiology Taping may play a role in the observed postural control improvement in patients with purely somatosensory vertigo, as compared to patients from the mixed etymology group. González-Iglesias et al. [22] reported reduced pain and improved cervical spine mobility after this kind of therapy, which can make a difference for shaping the posture and motility in individuals with the organic, but solely bone-joint-muscle cause of the vestibular syndrome. Ozmen et al. [23] noticed maintained flexibility of the muscles that if appeared in the neck might help to correct posture. |
| There’s no denying that a multitude of application methods, noninvasiveness, and high availability of the method as well as broad therapeutic indications make Kinesiology Taping a quite universal tool for combating dysfunctions in multiple systems. Yet, in the case of cervical vertigo therapy, it seems that this method should be considered supportive to primary treatment, at the same time leaving the room for continuation of research and experiment [24]. But it must be underlined that subjective symptoms like vertigo and balance disturbances were reported by our patients to be less annoying. If the method of our study was founded on the Dizziness Handicap Inventory- most frequently used to appreciate the vestibular symptoms- the results of kinesiotaping might be more satisfactory [25]. |
| Conclusions |
| 1. In patients with cervical vertigo, the applied Kinesiology Taping therapy did not have any impact on the shaping of objectively assessed conduction (SEP) from the balance system sensory receptor through the cervical spine up to the sensory cortex. |
| 2. The lack of significantly improved results of the static and dynamic test carried out with the use of CCG was observed after Kinesiology Taping therapy. |
| 3. The results of Freyss’ dynamic stabilometry were better after kinesiotaping when the visual control was preserved. |
| 4. Patients with solely somatosensory etiology of balance disorders responded better to the taping therapy than patients from the mixed etiology group. |
| Acknowledgement |
| Article financed from project INNOSENSE (contract no. STRATEGMED1/248664/7/NCBR/2014). Project co-financed from the funds of National Centre for Research and Development within the framework of STRATEGMED programme. |
References |
|
Tables and Figures at a glance
| Table 1 | Table 2 | Table 3 | Table 4 | Table 5 |
| Table 6 | Table 7 | Table 8 | Table 9 | Table 10 |
Figures at a glance
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 |
Relevant Topics
- Electrical stimulation
- High Intensity Exercise
- Muscle Movements
- Musculoskeletal Physical Therapy
- Musculoskeletal Physiotherapy
- Neurophysiotherapy
- Neuroplasticity
- Neuropsychiatric drugs
- Physical Activity
- Physical Fitness
- Physical Medicine
- Physical Therapy
- Precision Rehabilitation
- Scapular Mobilization
- Sleep Disorders
- Sports and Physical Activity
- Sports Physical Therapy
Recommended Journals
Article Tools
Article Usage
- Total views: 15230
- [From(publication date):
April-2016 - Aug 30, 2025] - Breakdown by view type
- HTML page views : 14139
- PDF downloads : 1091
