Case Report Open Access
Meconium Peritonitis in a Neonate: Clinical and Radiological Findings
Maciel JMW*, Moritsugu CT and Alvares BRDepartment of Radiology, Universidade Estadual de Campinas Faculdade de Ciencias Medicas, Sao Paulo, Brazil
- *Corresponding Author:
- Joao Marcos Wolf Maciel
Department of Radiology
Universidade Estadual de Campinas Faculdade de Ciencias Medicas
Campinas, Sao Paulo, Brazil
Tel: +5517988125045
E-mail: joaowolfradiofcm@gmail.com
Received date: August 03, 2017; Accepted date: August 16, 2017; Published date: August 21, 2017
Citation: Maciel JMW, Moritsugu CT, Alvares BR (2017) Meconium Peritonitis in a Neonate: Clinical and Radiological Findings. OMICS J Radiol 6:271. doi: 10.4172/2167-7964.1000271
Copyright: © 2017 Maciel JMW, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Radiology
Abstract
Although meconium peritonitis has a low incidence (1 in 35,000 births), when occurs with a late diagnosis it usually leads to a high morbidity and mortality of neonates. This anomaly takes place due to bowel perforation and the consequence is the meconium extravasation into the peritoneal cavity, promoting an exudative inflammatory reaction due to various gastrointestinal pathologies that occurs in neonates or intrauterine. It is worthwhile mentioning that this inflammatory response may result in ascites, fibrosis, and calcification and, in some cases, in cyst formation. Clinical manifestations are non-specific; some of them are: intestinal changes, decrease in the general condition or abdominal physical alterations. In this work, it is described the case of a premature neonate, in which, by physical examination, solid masses in the lower part of abdomen were identified, being afterwards submitted to a thoracic-abdominal x-ray examination. The condition suddenly progressed to sepsis, leading to patient´s death. Bearing all this in mind, this work reports the need of a reinforced standard radiographic image that could be used as a basis in similar cases, helping the diagnosis so that the best treatment strategy may be defined.
Keywords
Meconium peritonitis; Radiography; Neonate
Introduction
Meconium represents material present in the large intestine of the fetus after the fourth month of intrauterine life resulting from the swallowing of amniotic fluid along with mucus, lanugo and epithelial cells. Its presence in the gut during the gestation period contributes to the caliber formation of the intestinal loops [1,2].
Meconium peritonitis represents the result of perforation of the gastrointestinal tract, with extravasation of meconium into the peritoneal cavity, promoting an inflammatory exudative reaction that is a sterile chemical peritonitis. If peritonitis persists after birth, bacterial infection occurs, with a reserved prognosis. Meconium peritonitis may be secondary to meconium ileus, atresia or intestinal stenosis, anal imperforation or intestinal necrosis resulting from intrauterine ischemia [2-4]. Although it is a rare condition, the diagnosis should be made as early as possible so that complications and their morbidity and mortality can be reduced. The simple x-ray of abdomen is one of the most effective, and easy to use, procedure to identify the diagnosis. The most relevant findings of meconium peritonitis are abdominal calcifications with different patterns (intra-abdominal calcification; a mass containing calcification in the context of a meconium pseudocyst) or even calcification in the scrotum. In what follows, a case report of this rare event is described.
Case Report
A middle-aged pregnant woman with hepatic and renal insufficiencies of unknown origin was admitted at the University Hospital with abdominal pains and uterine contractions, and after general exams, the baby was born. The premature neonate was female, small for gestation age, with a Capurro classification estimated at 31 weeks.
The baby was born with severe anoxia, hydrops fetalis and with intense ascites leading to breathing difficulties. She was submitted to a procedure in order to drain the ascites, in the neonate resuscitation room, to allow for adequate respiration.
Even after the initial ventilation strategies, the saturation was low and the patient was unstable, and actions were taken according to the neonate respiratory distress syndrome. Then, ventilation assistance through Continuous Positive Airway Pressure (CPAP) was carried out, however this procedure was not enough to maintain the adequate ventilation, and so, it was necessary an orotracheal intubation.
With the breathing control, the baby was referred to the Neonatology Department of the Hospital where, through a general physical examination, it was observed the presence of solid masses with imprecise limits in the lower abdomen region.
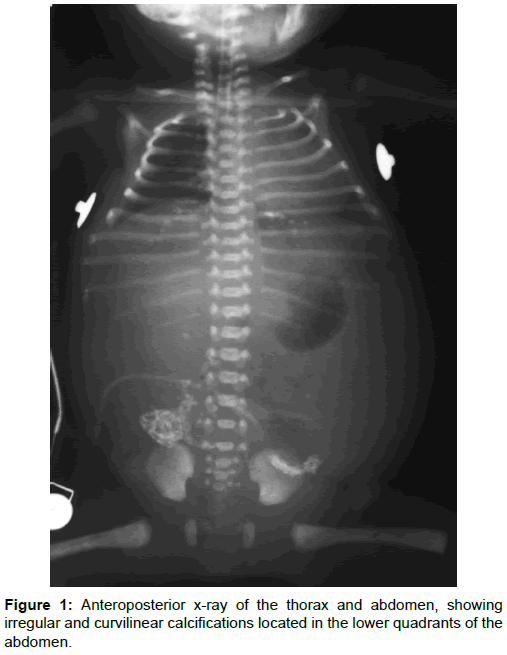
Due to this finding and the respiratory status of the neonate, an anteroposterior x-ray of the thorax and abdomen was carried out, in one single acquisition (Figure 1).
According to Figure 1, abdominal calcifications were observed in the lower quadrants. These calcifications appear to be in the peritoneal structure or to be a pseudo-cyst, and so, meconium peritonitis was diagnosed. Additionally, through clinical evaluation, it was possible to conclude that the baby was with respiratory distress syndrome.
During hospitalization, it was started a conservative treatment for meconium peritonitis, but there was worsening of the baby clinical conditions, with suspect of pulmonary or abdominal complications. Then, a second anteroposterior x-ray of the thorax and abdomen was performed (Figure 2). It was observed an atelectasis of the right upper lobe and the same abdominal findings.
Before taking new therapeutic strategies, the neonate evolved with a pronounced worsening of the general state, a larger breathing difficulty, and alterations in laboratory data, with a septic shock, resulting in death.
Discussion
The meconium peritonitis clinical manifestation is variable, and may be asymptomatic, rare, or, in the majority of cases, non-specific, with abdominal pain, alteration of the patient’s general condition as well as changes of the stool pattern, varying according to the manifestations of the primary event. As clinical changes are variable, the physical examination is unspecific, usually with abdominal distension, abdominal stiffness or even abdominal mass, more commonly in the right lower quadrant (ileum rupture is the most frequent pathology) [3,4].
The meconium peritonitis has an incidence of 1 in 35000 births, being, hence, a rare condition, with a slight male predominance and a survival of 50%. The diagnosis can be done in the gestation phase with Ultrasound (US) or by abdominal x-ray of neonates, with varied images, altering according to the etiology of the obstruction /perforation [3,4].
Through US, there are several findings, isolated or associated, none of which are very specific, but should always raise the suspicion for this pathology: fetus polydraminium, ascites, dilatation of loops and abdominal calcifications (posterior acoustic shadows or echogenic mass). The findings of intestinal pseudocysts and isolated polyhydramnios are more specific for meconium peritonitis, and are almost pathognomonic [2-6].
Abdominal radiographic findings demonstrate abdominal calcifications of a segmental, irregular or curvilinear pattern, suggesting calcification of peritoneal structures. They may also be located in the scrotal pocket or pleural cavity by the passage of meconium from the abdominal cavity through communications between the two cavities. There are other general and very nonspecific radiographic findings, but together they should raise the suspicion for meconium peritonitis, which are: absence of gas in the rectal ampulla, abdominal cysts and dilatation of loops [3,7]. In general, at least four types of meconium peritonitis are recognized, to know: fibro-adhesive (dense mass with calcium deposits caused by chemical reaction), cystic, generalized and healed.
The unfavorable prognosis stems from some frequent complications: development of huge formations of abdominal cysts that may suffer rupture; the formation of ascites that can cause fetal heart failure; and the development of sepsis with rapid evolution due to frequent bacterial colonization after 72 hrs of birth [8].
The treatment should be initiated in the first 24 hrs of life, and may be performed through surgery or conservative therapy with antibiotic alone or associated with abdominal drainage, usually the latter. Surgical intervention is necessary when active peritonitis, intestinal obstruction or pneumoperitoneum is identified. The intrauterine approach is not often used because it may lead to a worse prognosis, but if the fetus begins to develop complications one should opt for intrauterine drainage [3,6].
Among the differential diagnosis of meconium peritonitis, mainly in relation to the imaging findings of intra-abdominal calcifications are meconium pseudocysts, hepatic calcifications, adrenal calcification, and hepatic granulomas [4].
Finally, this pathology is a rare condition with many complications and low survival, which requires specific therapy for each etiology. Therefore, meconium peritonitis should always be suspected in neonates when the US and x-rays present suspicious findings such as calcifications and abdominal pseudocysts. In addition, all these babies should be screened to detect cystic fibrosis, because the association with this pathology is frequent [2].
Conclusion
Meconium peritonitis is an inflammatory reaction caused by the accumulation of meconium in the peritoneum due to a range of gastrointestinal pathologies, making the manifestations non-specific or similar to infection by a specific pathogen. Therefore, it is imperative to maintain a clinical suspicion and to be aware of the most expressive radiological signs, in order to establish an early diagnosis and the rapid application of pertinent clinical procedures, contributing to the reduction of the morbidity and mortality of this pathology.
References
- Alanbuki AH, Bandi A, Blackford N (2013) Meconium periorchitis: A case report and literature review. Can Urol Assoc J 7: 495.
- Chandrasekaran N, Berbardete D, Cariello L, Meraz D (2017) Prenatal sonographic diagnosis of meconium peritonitis from duodenal atresia. BMJ Case Rep bcr2017219208.
- de Amorim MMR, Vilela PC, Santos LC, Neto GHF, Cursino O, et al. (1999) Peritonite meconial como diagnóstico diferencial de ascite fetal: relato de caso. RBGO 21: 353.
- Sharma D, Murki S, Pratap T (2014) Meconium peritonitis: an interesting entity. BMJ Case Reports 2014: bcr2014203536.
- AboEllail MA, Tanaka H, Mori N, Tanaka A, Kubo H, et al. (2015) HDlive imaging of meconium peritonitis. Ultrassound Obstet Gynecol 45: 494-496.
- Kitamura RK, Midulla P, Mirensky T (2016) Meconium peritonitis following intestinal atresia: A case report. J Pead Surg Case Rep 9: 9-10.
- Lee GS, Chandran S, Rajadurai VS (2015) Calcified meconium pseudocyst: X-ray diagnosis of meconium peritonitis at birth. BMJ Case Rep bcr2015211052.
- Dias R, Dave N, Garasia M (2016) Meconium peritonitis: A rare neonatal surgical emergency. Indian J Anaesth 60: 364-366.
Relevant Topics
- Abdominal Radiology
- AI in Radiology
- Breast Imaging
- Cardiovascular Radiology
- Chest Radiology
- Clinical Radiology
- CT Imaging
- Diagnostic Radiology
- Emergency Radiology
- Fluoroscopy Radiology
- General Radiology
- Genitourinary Radiology
- Interventional Radiology Techniques
- Mammography
- Minimal Invasive surgery
- Musculoskeletal Radiology
- Neuroradiology
- Neuroradiology Advances
- Oral and Maxillofacial Radiology
- Radiography
- Radiology Imaging
- Surgical Radiology
- Tele Radiology
- Therapeutic Radiology
Recommended Journals
Article Tools
Article Usage
- Total views: 7556
- [From(publication date):
August-2017 - Aug 31, 2025] - Breakdown by view type
- HTML page views : 6606
- PDF downloads : 950