Clinical images Open Access
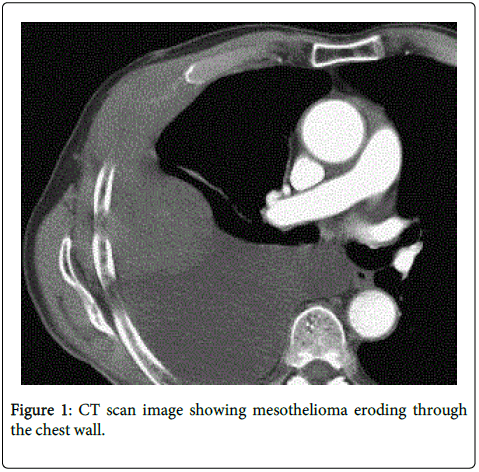
Mesothelioma Eroding through the Chest Wall
MacLeod N1,2*, Klepstad P3,4, Fallon M1,5 and Laird B1,2,51Edinburgh Cancer Research UK Centre, University of Edinburgh, Crewe Road South, Edinburgh EH4 2XR, UK
2Beatson West of Scotland Cancer Centre, 1053 Great Western Rd, Glasgow, G12, UK
3Department of Anaesthesiology and Emergency Medicine, St Olavs University Hospital, Trondheim N-7006, Norway, UK
4Department of Circulation and Medical Imaging, Norwegian University of Science and Technology (NTNU), 7006 Trondheim, Norway, UK
5Western General Hospital, Crewe Road South Edinburgh, EH4 2XU, UK
- Corresponding Author:
- MacLeod Nicholas
Edinburgh Cancer Research UK Centre
University of Edinburgh, Crewe Road South
Edinburgh EH4 2XR, UK
Tel: 0044 141 301 7679
Fax: 0044 141 301 7604
E-mail: Nicholas.macleod@ggc.scot.nhs.uk
Received Date: June 26, 2014 Accepted Date: June 27, 2015 Published Date: June 29, 2015
Citation: Macleod N, Klepstad P, Fallon M, Laird B (2015) Mesothelioma Eroding through the Chest Wall. J Palliat Care Med 5:i102. doi: 10.4172/2165-7386.1000i102
Copyright: © 2015 Macleod N, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Palliative Care & Medicine
Clinical Image
A 68-year-old man presented to his local hospital with severe right-sided chest pain and breathlessness. He had worked as an apprentice carpenter in the shipbuilding industry many years ago. A chest X-ray was performed which showed a right-sided pleural effusion and pleural thickening. A Computerised Tomograph (CT) scan, including a CT guided biopsy, was done with pathology confirming MPM of sarcomatoid type. Treatment options were discussed with the patient. Chemotherapy was discussed but this was declined by the patient due to low likelihood of benefit. The patient agreed that treatment would be symptomatic only. The gentleman described his pain as “stabbing and shooting”, suggesting a neuropathic component. He also stated that it was severe in intensity.
Prior to admission, he had been taking tramadol (400 mg daily) and gabapentin (300 mg three times daily). During his admission, he was commenced on 40 mg of Morphine Sustained Release Tablets (every 12 hours), 15 mg of Immediate release Morphine Tablets when needed for pain, and a lidocaine patch applied over the chest wall. Tramadol was discontinued.
Pain continued to be problematic and when his morphine dose was escalated, he developed signs of opioid toxicity (muscle jerks and pseudo-hallucinations). He was therefore switched to Oxycodone Sustained Release Tablets (30 mg twice daily). With this, his opioid toxicity improved though was still present. His gabapentin was increased to 600 mg TDS and he remained on a lidocaine patch. Despite all this, his pain remained poorly controlled. At this point, he received radiotherapy with the aim of improving his pain. Twenty Gy in 5 fractions of radiotherapy were administered which brought about a temporary improvement in his pain but six weeks after treatment, his pain was as severe as it was prior to his radiotherapy. Following this, he was considered for cordotomy but unfortunately died before he was able to receive this.
This case illustrates some of the difficulties patients with MPM face in terms of pain management. Despite multiple analgesics and palliative radiotherapy, his pain remained poorly controlled. Not all cases of MPM are as challenging as this.
--Relevant Topics
- Caregiver Support Programs
- End of Life Care
- End-of-Life Communication
- Ethics in Palliative
- Euthanasia
- Family Caregiver
- Geriatric Care
- Holistic Care
- Home Care
- Hospice Care
- Hospice Palliative Care
- Old Age Care
- Palliative Care
- Palliative Care and Euthanasia
- Palliative Care Drugs
- Palliative Care in Oncology
- Palliative Care Medications
- Palliative Care Nursing
- Palliative Medicare
- Palliative Neurology
- Palliative Oncology
- Palliative Psychology
- Palliative Sedation
- Palliative Surgery
- Palliative Treatment
- Pediatric Palliative Care
- Volunteer Palliative Care
Recommended Journals
- Journal of Cardiac and Pulmonary Rehabilitation
- Journal of Community & Public Health Nursing
- Journal of Community & Public Health Nursing
- Journal of Health Care and Prevention
- Journal of Health Care and Prevention
- Journal of Paediatric Medicine & Surgery
- Journal of Paediatric Medicine & Surgery
- Journal of Pain & Relief
- Palliative Care & Medicine
- Journal of Pain & Relief
- Journal of Pediatric Neurological Disorders
- Neonatal and Pediatric Medicine
- Neonatal and Pediatric Medicine
- Neuroscience and Psychiatry: Open Access
- OMICS Journal of Radiology
- The Psychiatrist: Clinical and Therapeutic Journal
Article Tools
Article Usage
- Total views: 13841
- [From(publication date):
July-2015 - Aug 30, 2025] - Breakdown by view type
- HTML page views : 9245
- PDF downloads : 4596