Research Article Open Access
Oral and Dental Findings in Patients with End Stage Renal Disease Undergoing Maintenance Hemodialysis in Sulaimani City
Khadija Muhamed Ahmed1*, Mohammed A Mahmood2, Rukhosh H. Abdulraheam2 and Shawbo M Ahmed3
1Department of Oral Diagnosis, University of Sulaimani, Iraq
2Department of Dental Basic Sciences, University of Sulaimani, Iraq
3Department of Operative, University of Sulaimani, Iraq
- Corresponding Author:
- Khadija Muhamed Ahmed
lecturer, Department of Oral Diagnosis
Faculty of Medical Sciences
University of Sulaimani School of dentistry
Street 27, Zone 209, Iraq
Tel: +9647701445804;
Fax: 1-952-658-0178;
E-mail: khadija.ahmad@univsul.edu.iq
Received date: May 31, 2015 ; Accepted date: June 23, 2015 ; Published date: June 25, 2015
Citation: Ahmed KM, Mahmood MA, Abdulraheam RH, Ahmed SM (2015) Oral and Dental Findings in Patients with End Stage Renal Disease Undergoing Maintenance Hemodialysis in Sulaimani City. J Interdiscipl Med Dent Sci 3:182. doi: 10.4172/2376-032X.1000182
Copyright: © 2015 Ahmed KM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at JBR Journal of Interdisciplinary Medicine and Dental Science
Abstract
Background: Patients with improper kidney’s functions requiring maintenance hemodialysis (HD) exhibit an increased prevalence of oral lesions. Since growing numbers of patients with chronic renal failure have been documented worldwide, the dental team has a significant role in providing oral care for patients with such disease.
The objectives of this study were to analyze the prevalence of oral lesions in hemodialysed patients compared to healthy individuals and to find a possible link between different subjective symptoms and objective clinical findings.
Patients and methods: An observational, case-control, cross-sectional study was carried out in 109 patients with end-stage renal disease (ESRD) on maintenance HD in comparison to 154 healthy controls in different health centers of Sulaimani city, Kurdistan region of Iraq. Various oral findings were documented by acknowledged dentist who implements well-known clinical diagnosis criteria for ESRD-associated oral manifestations. The data were analyzed using descriptive and analytical statistical software program to find the association between varibles; a p-value < 0.05 were considered as significant.
Results: The most common prevalent oral manifestations in haemodialysis group of patients were dry mouth (76.1%), coated tongue (73.4%), uremic fetor (66.1%), unpleasant taste (64.2%) and pale oral mucosa (60.6%); while linea alba was the most prevalent finding in healthy group. There was a significant relation with high Odds Ratio between dry mouth with uremic fetor, unpleasant taste, and oral mucosal pain.
Conclusions: Results of the present study indicated that a variety of oral manifestations is shown in patients with ESRD on maintenance hemodialysis in comparison to healthy individuals.
Early detection of these findings is of great importance, as it would allow the dentist to implement therapeutic and preventive measure for patients awaiting a renal transplant.
Keywords
End-stage renal disease; Hemodialysis; Xerostomia; Oral findings
Introduction
Normal kidneys excrete nitrogenous waste product; regulate fluid volume and acid /base balance of plasma; synthesize erythropoietin, 1, 25-dihydroxy-cholecalciferol and rennin are responsible for drug metabolism [1]. Chronic Renal Failure (CRF) is caused by a progressive and irreversible decline in the number of the functional unit of the kidney or the nephrons [2].
Patients develop End-Stage Renal Disease (ESRD) once bilateral deterioration of nephrons passes the point of compensation, therefore; dialysis treatment and kidney transplantation are life-saving procedures in these patients [3].
Worldwide the prevalence and incidence of patients with ESRD appears to be increasing [4,5], and when this coupled with improved rates of survival for renal replacement therapies, it is evident that patients with chronic renal failure will comprise an increasing proportion of dental patients in the near future [6].
Various signs and symptoms are presented in patients with ESRD, reflecting the improper kidney’s functions in every organ system [7,8].
In the oral cavity, a wide variety of oral manifestations have been documented in these patients by several authors [2,8-10]. Determination and identification of these changes in the oral cavity will improve the quality of life in these patients.
Furthermore, it is important to consider patients with ESRD on maintenance hemodialysis (HD) as a candidate of renal transplant in the future. Since the availability of the transplant is unpredictable, and when it occur the time interval of pretransplant preparation is too short to manage all the existing oral infections in HD patients, therefore, it is worth to evaluate and maintain an acceptable oral health status of these dialysis patients at least until successful transplantation [11].
From this viewpoint, the objectives of this study was firstly, to analyse the prevalence of oral lesions in haemodialysed patients compared to healthy individuals; secondly to find possible link between different subjective symptoms and objective clinical findings.
Patients and Methods
This study was designed as an observational, case-control, crosssectional study. Ethical approval to undertake the study was obtained from the Faculty of Medical Sciences, School of Dentistry, University of Sulaimani in Kurdistan region, Iraq.
The study populations were all consecutive end-stage renal failure patients regularly attending the nephrology department of (Chwarbakh, Shar and Shorsh) hospitals for maintenance hemodialysis. Regardless of the etiology of the condition, a total of 109 patients with ESRD undergoing hemodialysis were selected. They were all adult patients above 18 years on maintenance haemodialysis for more than three months and agreed to participate in the study, while patients below 18 years and those with history of smoking and alcoholism that could affect their oral health status were excluded.
The control group populations were randomly selected from (Peramerd hospital, Shorsh center and outside clinics) in Sulaimani province. They were systemically healthy people, with no history of kidney disease, or any other chronic debilitating illness, or habit of smoking or drinking, and/or not receiving any medication that could affect oral health, but who were seeking treatment due to dental problems.
All the examinations were carried out by one author (oral medicine specialist) who used acknowledged clinical diagnosis criteria for ESRDassociated oral manifestations reported by Proctor et al. [4].
All subjects were informed about the procedure and their agreements were taken to participate in the study. For all patients, the existed oral and dental findings were registered using simple dental instruments and for patient’s convenience, all examination was performed at the bed side during HD session.
Changes in the oral cavity were followed on the entire mucosal surface recording ESRD- associated signs, symptoms, and oral lesion absence or presence. Signs and symptoms identification was objectively searched for, and /or reported by the patients. A diagnosis of xerostomia was made when the patients reported dry mouth and during oral inspection dental instrument was sticking to the oral mucosa. Uremic fetor was recorded as a urine-odorbreath and unpleasant taste as loss of sensation of different tastes in food. Subjective feeling of mucosal pain and burning sensation especially on the dorsal surface of the tongue were also reported by asking the patients about their existence or disappearance.
Oral lesions, when present, were diagnosed according to the history and clinically accepted criteria. Dry and fissured lips were recorded when smaller or larger squamous formations on the mildly erythematous vermilion surface were observed. Coated tongue was registered as dirty white plaque formations on the dorsal surface which could be easily removed and also elongated filiform papillae were present. Uremic stomatitis was registered as a form of irregular easily erythematosus areas covered with grayish white pseudomembranes localized on lateral borders and dorsum of the tongue or buccal mucosa, accompanied with painful sensations. Gingival enlargements were observed in the region of marginal gingival and interdentally papilla. Enamel hypoplasia was recorded once a defect of the teeth (in which the enamel is hard but thin and deficient in amount) was seen. Bleeding tendencies were suspected if petechiae and ecchymose'swere observed in the mucosal surface of the oral cavity of the participant individuals. Other lesions like paleness of oral mucosa due to anemia and oral candidiasis particularly erythematous candidiasis and angular cheilitis were all diagnosed according to the criteria described by Proctor et al. and Haider et al. [4,10].
Statistical Analysis
The data was entered into a Microsoft© Excel spreadsheet 2010©, after collection of data; the data was transported into SPSS© (Statistical Package for the Social Sciences- version 21.0). Descriptive statistics (number and percentage) were calculated, as well as analytical statistics was done to find the relations between variables. Chi-square and Ttest were used for calculation of P value and coefficient of relation. A P-value < 0.05 was considered as significant.
Results
The demographic features of the study participants are shown in Table 1. There were 109 hemodialysis patients compared to 154 healthy controls, more females found than males in both groups. The mean age of the hemodialysis group was 52.55 years to 29.72 years in healthy controls. The most common causes of chronic renal failure were chronic glomerulonephritis followed by hypertension and diabetes mellitus and the majority of the hemodialysis patients took antihypertensive medications.
| Variable | Haemodialysispatients (no.=109) | Healthy controls(no.=154) |
|---|---|---|
| Male | 51 | 51 |
| Female | 58 | 103 |
| Mean age ± SE | 52.55 ± 1.45 | 29.72 ± 0.84 |
| Causes of Renal Failure | ||
| Chronic glomerulonephritis | 85 (78%) | 0 (0%) |
| Hypertensive nephropathy | 54(49.5%) | 0 (0%) |
| Diabetic nephropathy | 33(30.5%) | 0 (0%) |
| Others or Unknown | 29(26.6%) | 0 (0%) |
| Medications used by the patients | ||
| Antihypertensive | 79(72.5%) | 5 (3.25%) |
| Diuretics | 30 (27.5%) | 0 (0%) |
| Calcium carbonate | 73 (67%) | 0 (0%) |
| Anti platelet agents | 17 (15.6%) | 0 (0%) |
| Multi-vitamins | 73 (67%) | 0 (0%) |
| Others | 23 (21.1%) | 7 (4.55%) |
Table 1: Demographic features including, sex, age (mean age), types of drugs and the underlying cause of ESRD and hemodialysis patients in comparison to healthy adults.
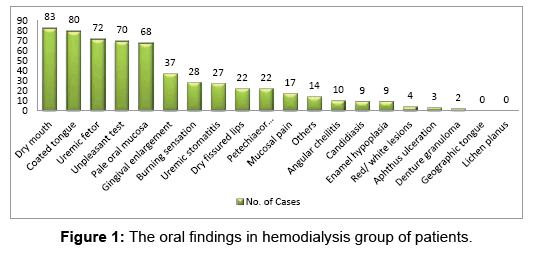
Table 2 (Figure 1) revealed the list of oral findings in the studied groups. Subjective feelings of xerostomia were reported by eightythree haemodialysis patients and the coated tongue was the most frequent objective findings (80 patients) in those patients, while nearly a comparable numbers of the patients complains of uremic fetor and unpleasant taste (72 and 70 haemodialysis patients). Pale oral mucosa, gingival enlargement and uremic stomatitis demonstrated by (66, 37and 27 patients respectively). In the healthy group the major oral findings was white lesions in the form of linea alba followed by pseudomembranous candidiasis and unpleasant taste (30, 14 and 12 patients respectively); details of the other findings are shown in Table 2.
| Variable | Haemodialysispatients (no.=109) | Healthy individuals (no.=154) |
|---|---|---|
| Uremic Fetor | 72(66.1%) | 4(2.6%) |
| Unpleasant taste | 70(64.2%) | 12(7.79%) |
| Dry mouth | 83(76.1%) | 5(3.25%) |
| Burning sensation | 28(25.7%) | 3(1.95%) |
| Mucosal pain | 17(15.6%) | 4(2.6%) |
| Pale oral mucosa | 66(60.6%) | 0 (0%) |
| Dry Fissure lips | 22(20.2%) | 0 (0%) |
| Coated tongue | 80(73.4%) | 9 (5.84%) |
| Candidiasis Erythematous/thrush | 9(8.3%) | 14 (9.09%) |
| Petechiae or ecchymoses | 22(20.2%) | 0 (0%) |
| Uremic stomatitis | 27(24.8%) | 0 (0%) |
| Red/ white lesions Leukoplakia/linea alba | 4(3.7%) | 30 (19.5%) |
| Angular cheilitis | 10(9.2%) | 2 (1.3%) |
| Gingival enlargement | 37(33.9%) | 6 (3.9%) |
| Enamel hypoplasia | 9(8.3%) | 1 (0.65%) |
| Aphthous ulceration | 3(2.8%) | 3 (1.9%) |
| Geographic tongue | 0 (0%) | 2 (1.3%) |
| Denture granuloma | 2(1.8%) | 0 (0%) |
Table 2: Oral findings in hemodialysis and healthy individuals.
The associations between the observed findings in hemodialysis group of patients in comparison to healthy individuals are demonstrated in Table 3. Nearly all variables were significantly differed in the studied groups except oral candidiasis, aphthous ulceration, geographic tongue and denture granuloma.
| Variable | Haemodialysis patients |
Healthy controls |
P value | |
|---|---|---|---|---|
| Mucosal pain | Yes | 17 | 4 | < 0.001 |
| No | 92 | 150 | ||
| Pale oral mucosa | Yes | 68 | 0 | < 0.001 |
| No | 41 | 154 | ||
| Dry fissured lips | Yes | 22 | 0 | < 0.001 |
| No | 87 | 154 | ||
| Candidiasis | Yes | 9 | 14 | 0.81 |
| No | 100 | 140 | ||
| Petechiaeorecchymoses | Yes | 22 | 0 | < 0.001 |
| No | 87 | 154 | ||
| Red/ white lesions | Yes | 4 | 30 | < 0.001 |
| No | 105 | 124 | ||
| Angular cheilitis | Yes | 10 | 2 | 0.003 |
| No | 99 | 152 | ||
| Gingival enlargement | Yes | 37 | 6 | < 0.001 |
| No | 72 | 148 | ||
| Enamel hypoplasia | Yes | 9 | 1 | 0.001 |
| No | 100 | 153 | ||
| Aphthous ulceration | Yes | 3 | 3 | 0.67 |
| No | 106 | 151 | ||
| Geographic tongue | Yes | 0 | 2 | 0.23 |
| No | 109 | 152 | ||
| Denture granuloma | Yes | 2 | 0 | 0.09 |
| No | 107 | 154 | ||
| Uremic Fetor | Yes | 72 | 4 | < 0.0001 |
| No | 37 | 150 | ||
| Unpleasant taste | Yes | 70 | 12 | < 0.0001 |
| No | 39 | 142 | ||
| Dry mouth (xerostomia) | Yes | 83 | 5 | < 0.0001 |
| No | 26 | 149 | ||
| Coated tongue | Yes | 80 | 9 | < 0.0001 |
| No | 29 | 145 | ||
| Uremic stomatitis | Yes | 27 | 0 | < 0.0001 |
| No | 82 | 154 | ||
| Burning sensation | Yes | 28 | 3 | < 0.0001 |
| No | 81 | 151 | ||
Table 3: Oral findings and association between variables in hemodialysis and healthy individuals.
The relation between dry mouth with subjective symptoms and objective findings in hemodialysis group of patients are shown in Table 4 and Table 5. There was a significant relation between dry mouth with each of uremic fetor, unpleasant taste and oral mucosal pain (OR = 4.7, OR = 5.2, OR = 5.9 respectively). On the other hand, there was a relatively low association between dry mouth and the other observed oral findings.
| Dry Mouth | P value | |||
|---|---|---|---|---|
| Yes | No | |||
| Uremic Fetor | Yes | 62 | 10 | 0.001 |
| No | 21 | 16 | ||
| Unpleasant test | Yes | 61 | 9 | < 0.001 |
| No | 22 | 17 | ||
| Burning sensation | Yes | 24 | 4 | 0.13 |
| No | 59 | 22 | ||
| Mucosal pain | Yes | 16 | 1 | 0.047 |
| No | 67 | 25 | ||
| Dry fissured lips | Yes | 16 | 6 | 0.43 |
| No | 67 | 20 | ||
| Gingival enlargement | Yes | 27 | 10 | 0.37 |
| No | 56 | 16 | ||
| Angular cheilitis | Yes | 23 | 3 | 0.442 |
| No | 76 | 7 | ||
| Coated tongue | Yes | 58 | 22 | 0.107 |
| No | 25 | 4 | ||
| Candidiasis | Yes | 5 | 4 | 0.136 |
| No | 78 | 22 | ||
Table 4: Relation between dry mouth and other oral symptom and signs in haemodialyse's group of patients.
| Variable | OR(95%CI) | P value |
|---|---|---|
| Uremic fetor | 4.724(1.8-12) | 0.001 |
| Unpleasant test | 5.237(2.04-13.4) | 0.001 |
| Mucosal pain | 5.970(0.75-47.4) | 0.091 |
Table 5: The Odds Ratio of uremic fetor, unpleasant test, and mucosal pain in relation to dry mouth.
Discussion
To begin with hemodialysis, means the kidneys functions impaired toward 5-10% of the original capacity. ESRD is the final sequel to several primary renal diseases, and systemic diseases with renal involvement, causing kidney function loss. The condition is incompatible with life unless the patient starts chronic dialysis treatment or kidney transplantation [12].
It is generally accepted that patients with ESRD undergoing haemodialysis exhibit an increased prevalence of oral lesions which could be related to the medical , psychological, and socioeconomic characteristics of these patients [13], since identification and maintaining good oral health in HD patients will help to diminish sources of infection foci during dialysis session, which inturn minimize the risk of unfavorable outcomes, this study aimed to determine the prevalence of these oral complication in comparison to healthy individuals.
The results of this study clearly indicated that there was significant difference in the types and nature of oral lesions presented in healthy and heamodialysis group of patients, and we were unable to make a meaningful comparison. The following augments the most prevalent oral manifestations in HD patients relevant to other researches in this field.
Our data revealed that the vast majority of HD patients were complainedof dry mouth (about 76% of all HD patients). Similar findings were observed by other investigators. Dry mouth resulted from a combination of direct gland involvement, water restriction, mouth breathing and the use of xerostomic medication as explained by [1,6,14]. In addition, Epstein et al. suggested that, salivary function (salivary flow) be used as a diagnostic index to aid in maintaining appropriate fluid balance levels in patients with ESRD on maintenance hemodialysis [14,15].
The results also showed that uremic odor and unpleasant taste were nearly comparable in HD patients (about 64-66% of all of HD patients), this was agree with the outcome of Belazelkovska et al., on the other hand lower proportion (about 34%, 48%, 50%) were detected by other researchers [2,12,16].
It is well known that uremic individuals have a characteristic halitosis (uremic fetor), which is explained by the fact that compromised kidney’s function results in an increase in the levels of urea in the blood and also in the saliva, where inturn to ammonia by the action of urase-splitting oral organisms. Additional factors for this characteristic halitosis include oral health and xerostomia. There was a positive relation between xerostomia and uremic fetor.
Contrary to previous researches that showed removal of urea and other toxin via dialysis results in improved taste function [5,17] however; a high proportion of our HD patients were still complained from altered taste sensation.This couldbe related to the persistence of high levels of urea, food avoidance (especially for animal proteins), low zinc levels (due to the malabsorption derived from gastrointestinal disorders). Additional possible causes are xerostomia, increased phosphate concentrations and changes in saliva pH, which led to unpleasant or metallic taste. Our results indicate that there was a significant positive relation between xerostomia and unpleasant taste.
The occurrence of burning sensation and mucosal pain reached (25.7% and 15.5% of all HD patients respectively). This result was fairly similar to that reported by Patil et al. and Kho et al.) [2,16].
Since the statistical analysis revealed a significant relation between oral mucosal pain and xerostomia, we hold the concepts that dry mouth may be the major forerunner of other subjective symptoms in HD patients however; there was a weak association between dry mouth and the other subjective and objective findings.
Our results also relate well to the previous reports of ESRD predisposing to oral lesions [8,12,14]. The most frequent oral lesions were coated tongue followed by pale oral mucosa, gingival enlargement, and uremic stomatitis.
Coated tongue was most frequently encountered lesion among our HD patients (about 73%). This figure was higher than that reported by de la Rosa-García et al. [12] and Chuang et al. and lower than that reported by Belazelkovska et al. [8]. Coated tongue is caused by retention of desquamated epithelial cells and dead leucocytes on filiform papillae and by volatile sulfurous compounds produced by anaerobic bacteria on the tongue surfaces. Poor oral hygiene, low saliva flow and even emotional condition of the dialysis patients have an impact on its occurrence.
Mucosal pallor was the second most frequent lesions in the HD group of patients (about 60%). This result is consistent with a similar study performed by de la Rosa-García et al and Belazelkovska et al. [8,12]. The appearance of pale oral mucosa in ESRD patients explained mainly by anemia caused by erythropoietin and folic acid deficiencies, hemolysis and hemodialysis complications resulted in the progression of the disease associated with the loss of renal functions.
Despite the fact that our patients were examined at bed side during HD session, however, gingival enlargements were noticed in (33.9% of all HD patients) by the naked eye. According to Proctor et al. and Martí Álamo et al. gingival enlargement is a relevant manifestation in renal transplant patients secondary to drug therapy, while in haemodialysis group of patients reflecting the usually poor oral hygiene, so deposits of calculus and plaque may be increased [1,4].
The etiology of uremic stomatitis to a large extend remain poorly understood. Clinically it may manifest as localized or generalized white, red or gray areas of the oral mucosa. The erythematous type coved pseudomembranous exudates leaving, on removal, an intact or ulcerated mucosa.
The relatively high proportion of HD group of patients presented with uremic stomatitis, this results contradicting other published results in HD and CRF patients. This might represent a high level of urea in the blood particularly before HD session or due to it is a relation with uremic odor.
It is well established that haemodialysis predispose to petechiae, ecchymosis and hemorrhage in the oral cavity due to factors depending on the disease itself, alteration in platelet aggregation and due to dialysis that diminish platelet recount due to mechanical damage and heparin anticoagulation during HD process. In the present study nearly (20% of HD patients) manifest petechiae and/ or ecchymosis in the oral cavity. In contrast to our finding Belazelkovska et al. demonstrate that about 90% of their HD patients showed petechiae and/ or ecchymosis. Meanwhile lower value was detected by other researchers [2,12].
In the current study, although the oral candidal infection was not confirmed by swab and histopathological diagnosis, nevertheless, the oral candidiasis and angular cheilitis were prevalent in both healthy and HD group of patients. It was a little surprising to observe oral candidiasis in healthy individuals; however, the majority of cases were occurred under dental prosthesis, indicating the underlined causes of oral candidiasis. In hemodialysis group of patients, it is accepted that compromised immune system due to uremia, malnutrition, and dysfunction of cellular and humoral immunity will increase the risk for opportunistic candidal infection. Furthermore, candidiasis may occur secondary to xerostomia, low saliva flow, poor oral hygiene, systemic diseas diseases like diabetes mellitus and medication that might affect salivary secretion. In agreement with previous investigators, oral candidiasis and angular cheilitis were associated with dry mouth.
It is important to point out that angular cheilitis has been found to be associated with candidal infection and anemia. In this investigation about (9% of HD patients) were revealed angular cheilitis, this results was in conflict with results of other researcher who reported a lower value [2,12,18].
The prevalence of dry fissured lips in this investigation like de la Rosa-García et al. study’s reached nearly 20% of all HD patients [8]. Higher prevalence was reported by Belazelkovska et al. and there was a weak association between fissured lips and xerostomia [12].
Regarding the other findings in HD group of patients, it is generally accepted to be associated with the direct or indirect effect of raised circulatory and salivary urea levels.
Finally, in the current study we found that lineaalba was the most common findings in healthy individuals. Linea alba is a bilateral raised white line on the buccal mucosa extending from commissure to the last molar teeth along their occlusal plain. Linea alba is asymptomatic and generally considered as a normal variation than pathological, therefore, no treatment required as documented by Anura A [19].
Conclusion
Results of the present study indicated that a variety of oral manifestations are presented in patients with ESRD on maintenance haemodialysis in comparison to healthy individuals, and there was strong relation of uremic fetor, unpleasant taste and oral mucosal pain with xerostomia in these patients.
Early detection of these findings is of great importance, as it would allow the dentist to implement therapeutic and preventive measure in patients awaiting a renal transplant.
References
- Álamo SM, Esteve CG, Pérez M (2011) Dental considerations for the patient with renal disease. J ClinExp Dent 3: e112-e119.
- Patil S, Khaandelwal S, Doni B, Rahuman F, Kaswan S (2012) Oral manifestations in chronic renal failure patients attending two hospitals in North Karnataka, India. Oral Health Dent Manag 11: 100-106.
- DaÄŸ A, Firat ET, KadiroÄŸlu AK, Kale E, Yilmaz ME (2010) Significance of elevated gingival crevicular fluid tumor necrosis factor-alpha and interleukin-8 levels in chronic hemodialysis patients with periodontal disease. J Periodontal Res 45: 445-450.
- Proctor R, Kumar N, Stein A, Moles D, Porter S (2005) Oral and dental aspects of chronic renal failure. J Dent Res 84: 199-208.
- Manley KJ, Haryono RY, Keast RS (2012) Taste changes and saliva composition in chronic kidney disease. Renal Society of Australasia Journal 8: 56-60.
- Bots CP, Brand HS, Poorterman JH, van Amerongen BM, Valentijn-Benz M, et al. (2007) Oral and salivary changes in patients with end stage renal disease (ESRD): a two year follow-up study. Br Dent J 202: E3.
- Summers SA, Tilakaratne WM, Fortune F, Ashman N (2007) Renal disease and the mouth. Am J Med 120: 568-573.
- Belazelkovska A, Popovska M, Mirjana S, Goce B, Zlatanka M, et al.(2013) Oral changes in patients with chronic renal failure. Romanian Journal of Oral Rehabilitation 5: 104-112.
- Akar H, Akar GC, Carrero JJ, Stenvinkel P, Lindholm B (2011) Systemic consequences of poor oral health in chronic kidney disease patients. Clin J Am SocNephrol 6: 218-226.
- Haider SR, Tanwir F, Momin IA(2013) Oral Aspects of Chronic Renal Failure. Pak Oral Dent J 33: 87.
- Chen LP, Chiang CK, Chan CP, Hung KY, Huang CS (2006) Does periodontitis reflect inflammation and malnutrition status in hemodialysis patients? Am J Kidney Dis 47: 815-822.
- de la Rosa García E, Mondragón Padilla A, ArandaRomo S, Bustamante Ramírez MA (2006) Oral mucosa symptoms, signs and lesions, in end stage renal disease and non-end stage renal disease diabetic patients. Med Oral Patol Oral Cir Bucal 11: E467-473.
- Souza CM, Braosi AP, Luczyszyn SM, Casagrande RW, Pecoits-Filho R, et al. (2008) Oral health in Brazilian patients with chronic renal disease. Rev Med Chil 136: 741-746.
- Kao CH, Hsieh JF, Tsai SC, Ho YJ, Chang HR (2000) Decreased salivary function in patients with end-stage renal disease requiring hemodialysis. Am J Kidney Dis 36: 1110-1114.
- Epstein SR, Mandel I, Scopp IW (1980) Salivary composition and calculus formation in patients undergoing hemodialysis. J Periodontol 51: 336-338.
- Kho HS, Lee SW, Chung SC, Kim YK (1999) Oral manifestations and salivary flow rate, pH, and buffer capacity in patients with end-stage renal disease undergoing hemodialysis. Oral Surg Oral Med Oral Pathol Oral RadiolEndod 88: 316-319.
- Middleton RA, Allman-Farinelli MA (1999) Taste sensitivity is altered in patients with chronic renal failure receiving continuous ambulatory peritoneal dialysis. The Journal of nutrition 129: 122-125.
- Klassen JT, Krasko BM (2002) The dental health status of dialysis patients. J Can Dent Assoc 68: 34-38.
- Anura A (2014) Traumatic oral mucosal lesions: a mini review and clinical update. Oral Health Dent Manag 13: 254-259.
Relevant Topics
- Cementogenesis
- Coronal Fractures
- Dental Debonding
- Dental Fear
- Dental Implant
- Dental Malocclusion
- Dental Pulp Capping
- Dental Radiography
- Dental Science
- Dental Surgery
- Dental Trauma
- Dentistry
- Emergency Dental Care
- Forensic Dentistry
- Laser Dentistry
- Leukoplakia
- Occlusion
- Oral Cancer
- Oral Precancer
- Osseointegration
- Pulpotomy
- Tooth Replantation
Recommended Journals
Article Tools
Article Usage
- Total views: 17007
- [From(publication date):
June-2015 - Jul 15, 2025] - Breakdown by view type
- HTML page views : 12219
- PDF downloads : 4788