Pericardial Tuberculosis-A Case Report
Received: 24-Nov-2016 / Accepted Date: 30-Dec-2016 / Published Date: 06-Jan-2017
Abstract
Pericardial tuberculosis is a rare extra pulmonary manifestation that affects approximately 1 to 2% of patients. Its clinical presentation is variable and nonspecific, which may hinder or delay the diagnostic definition resulting in late complications such as constrictive pericarditis and increased mortality. Imaging tests are noninvasive methods that may aid in presumptive diagnosis, since pericardial effusion is the most frequent sign. The finding of Mycobacterium tuberculosis in pericardial tissue fragment biopsy or culture of pericardial fluid confirms the diagnosis. Therapy is shown to be highly effective with the use of the four-fold antituberculosis regimen for six months. The use of corticosteroids is controversial. The objective of this report is to present a case of pericardial tuberculosis associated with constrictive pericarditis diagnosed in the internal medicine service of a hospital in Ubá-MG, Brazil. It is very important to remember this pathology in cases of pericardial effusion of unknown etiology.
Keywords: Pericardial tuberculosis; Constrictive pericarditis; Extrapulmonary tuberculosis
77176Introduction
The infectious pathogenesis of the pericardium by the bacillus occurs by contiguity, from tuberculosis of the mediastinal ganglia, of adjacent lung focus, miliary dissemination or by reactivation. Symptoms such as dyspnea, anterior chest pain, ventilator-dependent or trunk rotation, and fever, often associated with other findings, such as tachycardia, paradoxical pulse, asthenia, anorexia, weight loss and night sweats. The nature of the symptoms depends on the stage of the infection, degree of pericardial-pericarditis involvement may be the only evidence [1]. In developing countries, tubercolosis remains an important etiology of a lot of clinical manifestations.
Case Presentation
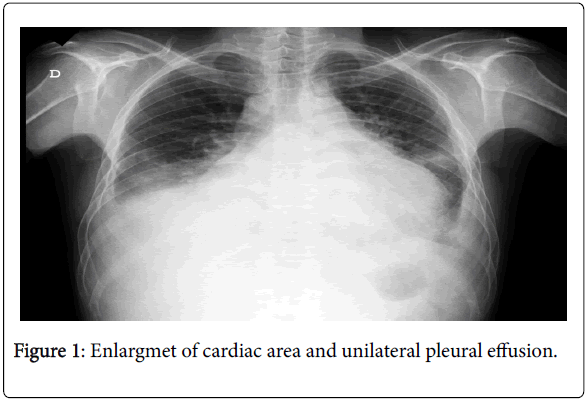
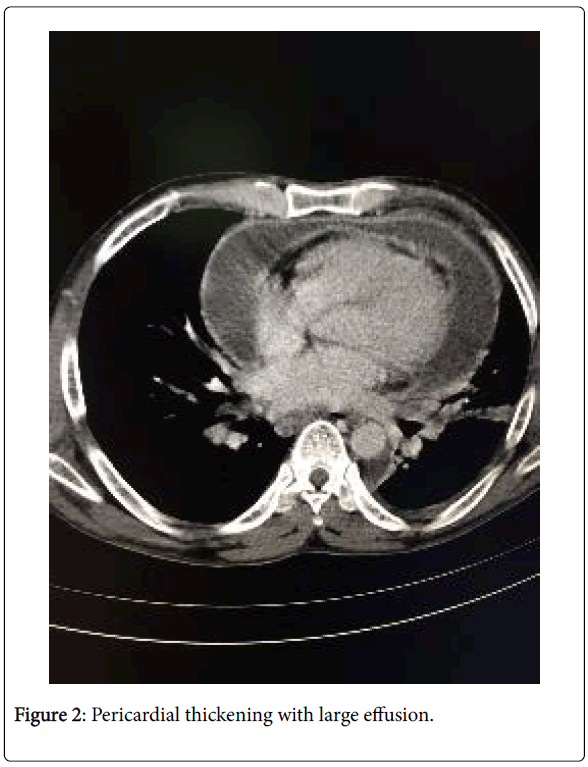
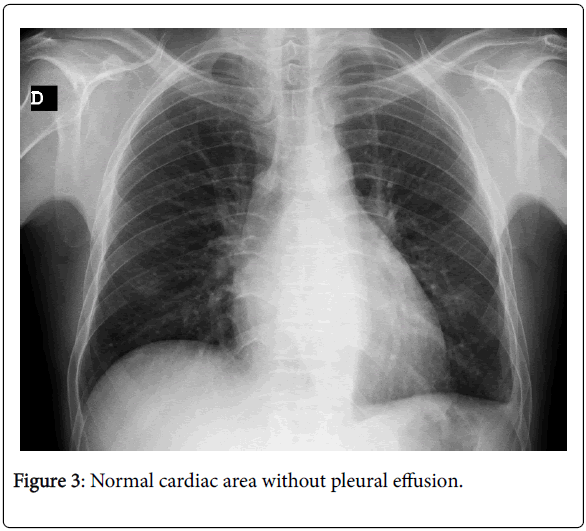
A 40-year-old male, natural and domiciled in Ubá, state of Minas Gerais, Brazil, sought medical care due to dyspnea on exertion, orthopnea, paroxysmal nocturnal dyspnoea and anasarca with significant worsening in the last month prior to consultation. He denied pathologies or previous use of medications. He referred heavy alcoholism and denied smoking. At physical examination, the patient was lucid and oriented, stained, hydrated, acyanotic, with tachypnea in ambient air and afebrile. Cardiovascular apparatus with regular rhythm and hypophontic sounds, arterial pressure of 80 × 60 mmHg. Respiratory apparatus with audible murmurs without adventitious noise, heart rate of 128 bpm. Flaccid and ascitic abdomen. Lower limbs with swelling 3+/4+. He had chest X-ray showing an important increase in the cardiac area and pleural efusion (Figure 1). He had a syndromic diagnosis of congestive heart failure and received clinical support with diuretic therapy. He presented response to therapy with decreased edema, but he maintained dyspnea and evolved with a febrile episode. Computed tomography of the chest showed massive pericardial effusion, pleural effusion and signs suggestive of pulmonary congestion (Figure 2). Three sputum samples with negative BAAR were performed. Pericardiectomy for pericardial biopsy and pericardial fluid that were positive for pericardial tuberculosis. Antituberculin treatment was then instituted and the patient progressed with improvement. After five months, the chest x-ray showed normal cardiac area without pleural effusion (Figure 3).
Discussion
Pericardial tuberculosis (TB) is a rare manifestation of extrapulmonary TB. It presents an estimated incidence of 1% to 4% of cases of pericarditis and usually develops by dissemination of mediastinal lymph nodes, lung, spine, sternum or during miliary infection [1,2]. Tuberculous pericarditis has a variable clinical presentation and should be considered in the evaluation of all cases of pericarditis. Tuberculous pericardial effusion usually develops insidiously, and the predominant symptoms, though nonspecific, are dyspnoea (an early and disabling symptom), cough, chest pain, night sweats, orthopnea, weight loss, and lower limb edema.
The most frequent signs are cardiomegaly, pericardial friction and tachycardia. Paradoxical pulse, hepatomegaly, jugular stasis and pleural effusion may still be included [3]. Pericardial effusion may be the first sign of localized or disseminated tuberculosis and usually results in involvement of the pericardial sac by mediastinal lymph nodes contaminated with mycobacteria. The pericardial fluid is usually a yellow-citrus-like exudate with increased lymphocyte numbers and low glucose. Their culture is not always positive for the bacillus. If it is not effectively emptied, it will result in the formation of fibrin, septations and granulomas with adherence and thickening of leaflets, evolving to chronic constrictive pericarditis [4]. Among the diagnostic methods, chest radiography has an increased cardiac area in more than 90% of the cases, in addition to pericardial calcifications in cases of chronic constrictive pericarditis. Characteristics of active pulmonary TB and pleural effusion may also be observed [5]. The ECG is abnormal in almost all cases of tuberculous pericardial effusion, usually in the form of nonspecific ST wave abnormalities. The Echocardiogram is a non-invasive and useful tool, through which it can be observed the presence of pericardial effusion and cardiac tamponade. The presence of effusion with fibers fibrinated in the visceral pericardium are typical, but not specific for a tuberculous pathogenesis [6]. CT scan of the chest shows typical changes in the mediastinal lymph nodes in almost 100% of the cases. Furthermore, it is possible to accurately delimit and quantify the extent of pericardial involvement [7]. The tuberculous pathogenesis of pericarditis should be established as far as possible by a diligent search for acid-fast bacilli in the sputum, lymph nodes and pericardial fluid [6]. In this case three samples of BAAR with negative result were performed. The diagnosis is confirmed by the finding of the Mycobacterium tuberculosis bacillus in the direct examination and culture of the pericardial fluid, or in a pericardial biopsy specimen. Biopsy leads to a diagnosis that is faster and more sensitive than pericardiocentesis [2]. The therapeutic used is the four-fold antituberculosis regimen (rifampicin, isoniazid, pyrazinamide, ethambutol) for six months. It is known that corticosteroids bring some benefit, making it impossible to recover the fluid, but there are still no data in the literature on the prevention of constrictive pericarditis. The complete and permanent drainage of the effusion fluid would be the best way to avoid future constriction of the cardiac chambers.
Conclusion
Patients with symptoms such as those described and presence of pericardial effusion should be investigated for pericarditis due to tuberculosis. We cannot fail to investigate pericardial tuberculosis in Brazil because although it is a rare disease, Tuberculosis is an endemic disease and its extrapulmonary forms should be included as a differential diagnosis. Early and appropriate treatment decreases the risk of developing into a potentially fatal disease.
References
- Trautner BW, Darouiche RO (2001) Tuberculous pericarditis: optimal diagnosis and management. Clin Infect Dis 33: 954-961.
- Khandaker MH, Espinosa RE, Nishimura RA (2010) Pericardial disease: diagnosis and management. Mayo Clin Proc 85: 572-593.
- Mayosi BM, Burgess LJ, Doubell AF (2005) Tuberculous pericarditis. Circulation 112: 3608-3616.
- Corey GR, Campbell PT, Trigt PV, Kenney RT, O’Connor CM (1993) Etiology of large pericardial effusions. Am J Med 95: 209-213.
- Reuter H, Burgess LJ, Doubell AF (2005) Role of chest radiography in diagnosing patients with tuberculous pericarditis. Cardiovasc J S Afr 16: 108.
- Cherian G (2004) Diagnosis of tuberculous aetiology in pericardial effusions. Postgrad Med J 80: 262-266.
- Golden MP, Vikram HR (2005) Extrapulmonary tuberculosis: an overview. Am Fam Physician 72: 1761-1768.
Citation: Farnetano BDS, Farias ML, Mota GSM, Leao CN, Machareth MMV (2017) Pericardial Tuberculosis-A Case Report. J Tuberc Ther 1: 102.
Copyright: ©2017 Farnetano BDS, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Open Access Journals
Article Usage
- Total views: 10235
- [From(publication date): 0-2016 - May 07, 2026]
- Breakdown by view type
- HTML page views: 8942
- PDF downloads: 1293