Preliminary Study on the Application of Upper: Airway Model Construction with 3DMIA in OSAHS of Children
Received: 30-Aug-2014 / Accepted Date: 30-Sep-2014 / Published Date: 10-Oct-2014 DOI: 10.4172/2161-119X.1000175
Abstract
Objective: To investigate the applicability of 3DMIA1 software to upper airway modeling in children with
obstructive sleep apnea hypopnea syndrome (OSAHS).
Methods: A total of 30 children diagnosed with OSAHS by polysomnography were included in this study. Data regarding upper airway structure were collected via spiral CT while sleeping and awake, from which a threedimensional model of the upper respiratory tract from the nasopharynx to the supraglottic region using 3DMIA software was constructed. The upper airway olume and airway minimum cross-sectional area were measured employing software algorithms.
Results: The upper airway volume and airway minimum cross-sectional area of the 30 children during sleep were significantly less than while awake (P <0.01).
Conclusions: 3DMIA software modeling and software algorithm measurement were more objective than
traditional radiology (e.g. Fujioka) with respect to evaluation of the extent of the upper airway narrowing in OSAHS
Keywords: Obstructive Sleep Apnea Hypopnea Syndrome (OSAHS); Computer; Modeling; Children
258686Introduction
Obstructive Sleep Apnea Hypopnea Syndrome (OSAHS) affects multiple systems and multiple organs of children, and it is a syndrome which combines multiple subjects with its own specific etiological factor, pathology, physiology, clinical features and therapy. At present, those basic studies on OSAHS of children are limited on its influences on sleep structure, incretion and the neural development during the growing process of children. However, as a sleep apnea disease featuring at upper respiratory tract obstruction, upper airway structure and morphous factor is publically regarded as one of those important morbidity factors for OSAHS. So, to accurately acquire the data of the upper airway structure and the function condition is the foundation to choose appropriate treatment for OSAHS patients. On the above basis, accurate location of the upper airway stegnosis of the OSAHS patients is necessary to guide the surgery. Since this subject was established in January of 2011, we have conducted 3-dimensional model construction study of the CT data of those children who were diagnosed with OSAS by PSG with 3DMIA software to discuss the possibility of acquiring more accurate upper airway morphous of OSAS children by using software to construct models of upper airway.
Materials and Methods
General data
We chose 30 OSAHS children (18 boys and 12 girls, age of 5-14 years old, average age of 9.5 years old) in our hospital (from 2011-01 to 2012-01). Those OSAHS children were diagnosed according to the Diagnosis standard of OSAHS of children, 2005 made by Stephen et al [1] those children were monitored and observed by PSG, and the diagnosis standard included: apnea hypopnea time>2 respiratory cycle, OAI (Obstructive Apnea Index)>1/h, AHI (apnea hypopnea index) ≥ 5/h, LSa02(Lowest Oxygen Saturation)< 92; among those children, 30 cases were detected with OAI 1.4-15hAHI 7.3-422hLSaO264-91; all cases were observed with snore during sleep, buccal respiration, wheeze and oppression.
Methods to collect CT data
We used brilliance ct 256-channel scanner to conduct scanning. Scanning method: the patient was set in the dorsal position (The body part below the neck was wrapped by clothing made of lead) and the head of the patient was sent into the scanner first; the patient should hold the breath; the line connecting the external auditory foramen and the inferior border of nasal wing on the same side was set as the basal line; data of the volume of the respiratory passage from nasopharynx to the area above glottis; we used double window presentation, and the width of the soft tissue window was 200Hu with the window position of 40Hu, while the width of the bone window was 1200Hu with the window position of 600Hu; digital images were acquired (for detailed scanning parameters see Table 1). After we adjusted the patient’s position, we suggested the patient to take eupnea and we performed spiral CT scanning. After the scanning was finished, we administrated chloral hydrate to the patient for oral use. After the patient was asleep, we adjusted his or her position and at the same time, performed CT scanning quickly to ensure that this CT scanning was performed during sleep cycle of the patient. Informed consents were obtained from the relatives of all children enrolled in this investigation. This research was approved by the Ethic Committee of our hospital.
| Cases | Upper airway volume (mm3) | Minimum cross section areas of air duct (mm2) | Cases | Upper airway volume (mm3) | Minimum cross section areas of air duct (mm3) | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| Awake | Asleep | Awake | Asleep | Awake | Asleep | Awake | Asleep | |||
| 1 | 18 | 15 | 43 | 22 | 16 | 26 | 18 | 66 | 38 | |
| 2 | 25 | 20 | 57 | 24 | 17 | 30 | 23 | 116 | 88 | |
| 3 | 25 | 17 | 59 | 27 | 18 | 14 | 10 | 64 | 51 | |
| 4 | 13 | 9 | 63 | 45 | 19 | 17 | 14 | 39 | 25 | |
| 5 | 13 | 12 | 66 | 29 | 20 | 22 | 17 | 70 | 39 | |
| 6 | 25 | 23 | 63 | 29 | 21 | 16 | 13 | 122 | 108 | |
| 7 | 21 | 12 | 74 | 46 | 22 | 33 | 24 | 147 | 103 | |
| 8 | 31 | 19 | 132 | 48 | 23 | 11 | 8 | 59 | 49 | |
| 9 | 15 | 10 | 118 | 102 | 24 | 13 | 9 | 87 | 45 | |
| 10 | 21 | 19 | 66 | 44 | 25 | 25 | 20 | 67 | 34 | |
| 11 | 27 | 16 | 155 | 75 | 26 | 21 | 15 | 78 | 32 | |
| 12 | 12 | 10 | 60 | 31 | 27 | 22 | 18 | 92 | 75 | |
| 13 | 24 | 15 | 55 | 19 | 28 | 15 | 10 | 82 | 71 | |
| 14 | 29 | 21 | 97 | 76 | 29 | 23 | 20 | 72 | 48 | |
| 15 | 27 | 15 | 201 | 188 | 30 | 29 | 15 | 101 | 77 |
Table 1: Scanning Parameters
Method to establish model
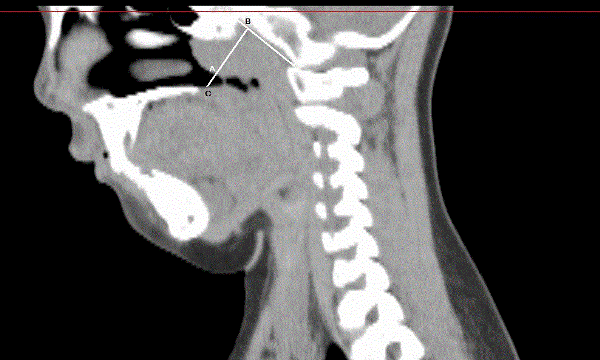
When we constructed the model of upper airway, we adopted the 3DMIA software automatically developed by the Computer School of South China Normal University (the code number of software copyright: 2008SR18799, 2008SR18798). We inserted the data sequence which was consistent with DICOM standard to the automatically developed medical imaging processing software 3DMIA, and used the software to perform important procedures such as imaging division, 3-dimensional reconstruction, and data measuring, etc. We performed imaging division of the CT data by using progress division as a dynamic self-adaptation region developing method [2]. We performed 3-dimensional surface rendering to those divided imaging by the Marching Cubes method. The free edge of soft palate, staphyle, the free edge of tip of the epiglottis and glottis were taken as identification markers. We identified the following parts as the key parts of the upper airway model: the postzone of soft palate, the staphyle zone, the postzone of tongue, the postzone of epiglottis and air tube. After we identified those key parts, we extracted centrage in appropriate region chosen in the upper airway 3-dimensional model mentioned above. Without changing the topology of upper airway, we simplified the 3-dimensional information to the central axis of upper airway to make it convenient to automatically calculate the cross section area along the centrage. By doing the above, we could offer references to analyze and estimate the stegnosis or the obstruction of the upper airway [3]. Through the above calculation method, we extracted from the model the upper airway volume and the minimum air duct cross section area of those children before and after they fell asleep respectively. We used traditional A/N method to acquire A/N ratio: a tangent line was made in the basilar clivus out of the skull, and the most prominent point of the adenoid B was taken to make a vertical line to the tangent line with A being the crossover point; the distance of A and B was measured as the value of A; AB line was prolonged and reached the juncture C in the pars palatalis through pharyngonasal cavity and air passage; the distance of AC was measured as the value of N (Figure 1).
Statistical method
We used SPSS 11.0 to conduct statistical analysis; we used t-test of paired samples for measurement data; P<001 meant statistical significance.
Results
We completely collected the upper airway CT volume data of those 30 children and successfully finished 3DMIA software model construction. We also acquired the upper airway volumes and the minimum cross section areas of those children before and after falling asleep respectively by the calculation method of the software. The results showed that: the upper airway volumes and the cross section areas of those children when they were asleep were significantly lower than when they were awake and the differences showed statistical significance (t=9.392, P < 0.01; t=9.256, P < 0.01, Table 2). The average A/N ratio was 0.67, and there were 14 patients whose A/N ≥ 0.67, accounted for 0.47% among all children with the disease.
| kV | mAs | Thickness | HP | Width of the reconstructed layer | S-F0V |
|---|---|---|---|---|---|
| 120 | 75 | 0.3×32 | 21 | 2~3mm | S |
Table 2: Showing statistical significance.
Discussion
At present, studies on OSAHS of children are limited on its influences on sleep structure, incretion, the neural development and other aspects during the growing process of children. In clinical, there still existed some doubts and confusions about it, for example: most scholars took PSG as the golden standard for the diagnosis of OSAHS children, however, as researches on the sleep mechanism and OSAHS went deeper, we found it difficult for sleep monitoring to reflect the sleep parameter of OSAHS children at normal times; except for some children showing more obvious First Night Effect (FNE), most children couldn’t adapt to the complex sleep monitoring device and relatively uncomfortable sleep progress, thus leading to the distortion of monitoring results; besides, some children had high risks factors such as obesity, jaw facial deformity and so on, these children were too little and had so many complications, so if we performed sleep monitoring to this type of children, the risks would increase significantly and at the same time, the whole progress couldn’t be completed mostly. If we could acquire more diagnosis parameter through noninvasive imaging data to act as subsidiary way for the diagnosis of the above children, we would increase the diagnosis of OSAHS of children to a new high. For the treatment of the disease, operations to relieve local blockage was taken as the first choice publically. However, for OSAHS which was a sleep-respiratory disease featuring at blockage of upper airway, operation to relieve anatomical abnormity was publically known as an important principle to treat OSAHS [4]. However in clinical practices, we could often observe that some children could show clinical features and physical signs which were not in consistent with the blockage degree described in books. To study the reasons, according to many clinical studies [5-7], the airflow obstruction planes included multiple planes such as nasopharynx, oropharynx, laryngopharynx and so on. The whole upper airway above the glottis was almost included. So, to acquire more accurate data of upper airway morphous and function condition and to precisely locate the upper airway stagnosis of OSAHS children to provide reference for operation were necessary conditions to further optimize operation plan and choose reasonable treatment method for OSAHS patients.
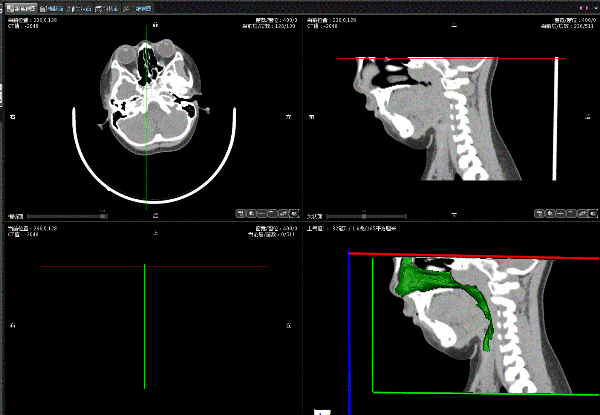
At present, there are many methods in clinical to evaluate patients’ local stegnosis of upper airway.. All of the above examination methods have their own advantages and disadvantages respectively and the information they acquire show different emphasizes. In recent years, with the widely used computer simulation technology, powerful calculation capacity of computers and leading in of finite element analysis, we could reconstruct the airway structure and morphous with volume data collected by CT. Using related software to perform accurate data comparison and measurement of the model was more and more used in the studies on the morphous and functions of upper airway. In this study, the imaging data were obtained by 256-slice CT. The dosage of X-ray was decreased by 60% to 80% compared with that used by previous equipments and the potential clinical ethic issue was properly avoided. Software 3DMIA adopted in this study was a medical image processing software with great functions automatically developed by the Computer School of South China Normal University, it could be used to progress various plane images, reconstruct 3-dimensional model and measure data of multiple medical image data. The produced 3-dimensional model in STL form could act as the foundation for continuous studies. Semi-auto calculation of the minimum cross section area of upper airway could accurately and quickly find the stegnosis in multiple planes of the patients. By using this 3-dimensional visualization method, we could analyze the 3-dimensional anatomical structures of OSAHS children before operation, and in the aspects of operation value concerns, risk evaluation and other aspects, this methods had more significant advantages than those methods adopted in other related studies. (Figure 2)
At present, studies on this aspect were mostly based on the plane image measurement by X-ray, CT and etc. As for this point, Major and other scholars [8] pointed out in the study that children’s upper airways were complex 3-dimensional structure; for children with OSAHS, with the influences left by diseases, their morphous of upper airways had variations to some extent, so when turned to 2-dimensional images, some information would be lost. In this study, we used software to perform 3-dimensional model construction and could acquire relatively accurate data of upper airway morphous and the relative correlation between each anatomical structure. Compared with those current studies based on data collected by CT, our study processed the data by surface-rendering, and the 3-dimensional model we produced were totally with complete virtual physical characteristics and space information other than the volume-rendering model acquired by adjusting CT value. In the models we established, through the specific functions of software, we could, within a specific space range, perform local maximization, rotation, transition and other operations to the model, which was beneficial to identify specific morphous, range and direction of upper airway stegnosis and this was the advantage other domestic studies didn’t have.
In identifying the stegnosis location of airways of children with OSAHS, most studies were concentrated in cavum nasopharyngeum and taking the size of adenoid as the study direction. Conventional tests, such as nasopharyngeal X-ray from a lateral view have been adopted to measure the size of adenoid in children, as an evaluation criterion for the degree of the upper airway stenosis. However, there are various limitations and disadvantages including magnification error caused by varying focus-slice distance and measurement error resulting from inaccurate selection of measurement point. Meantime, nasopharyngeal X-ray from a lateral view displays an overlap image, easily intervened by the ascending branch of mandible. In addition, it fails to display the structures of nose and nasopharynx in details.
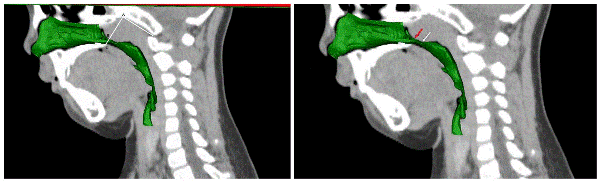
In our study, we adopted the centrage extraction calculation method of the software, located the minimum cross section area of pars nasalis pharyngis with computer and measured in 3-dimensional vision. We found that among those 30 OSAHS children, when they were asleep, only 11 children showed that the most prominent point of pars nasalis pharyngis, namely the point with biggest A value, was in the same plane with the minimum cross section area of pars nasalis pharyngis along the centrage of airway, accounted for 37% of the total. The other 63% children showed that, the narrowest position of pars nasalis pharyngis was not in the same plane with the most prominent point of adenoid. So we might not correctly identify the stegnosis degree of children’s upper airways according to the traditional A/N ratio. As for the reasons, we analyzed and thought that, from the 3-dimensional morphous view, the morphous of OSAHS children’s upper airways in pars nasalis pharyngis were often in wedge cube or trapezoid cube shape; although at most times, the anteroposterior diameter between the most prominent point of adenoid and pars palatalis was the narrowest, the left-to-right diameter namely the distance between the left and right lateral pharyngeal wall might not be the narrowest, so the area was not the smallest (Figure 3, Figure 4). We haven’t got a relatively public received method or standard in evaluating the stegnosis degree of OSAHS children’s upper airways till now, but if we see the trend, we will find that it is accepted by most scholars step and step that we should evaluate the relative volume of stegnosis tissue to upper airway volume other than only evaluate the absolute volume of soft tissue [9]. By using fluid mechanics theories, Powell et al. [10] had proved among adults that in narrow and irregular upper airways, the air current shear stress born by stegnosis tissue significantly increased. This process might cause progressive injuries to the mechanics recipients of upper airway and other recipients that coordinated the contraction of diaphragmatic muscle and respiratory muscles. So, we thought that there existed some defects in our traditional way of evaluating the illness stage and operation indications of OSAHS children by simply measuring the volume of adenoid. Using 3DMAX software to construct model to evaluate the morphous of children’s complete upper airways, and measuring the minimum airway area through computer would be more beneficial to make objective diagnosis to the illness of OSAHS children.
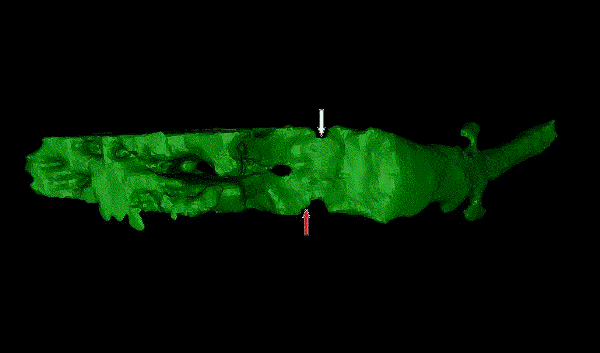
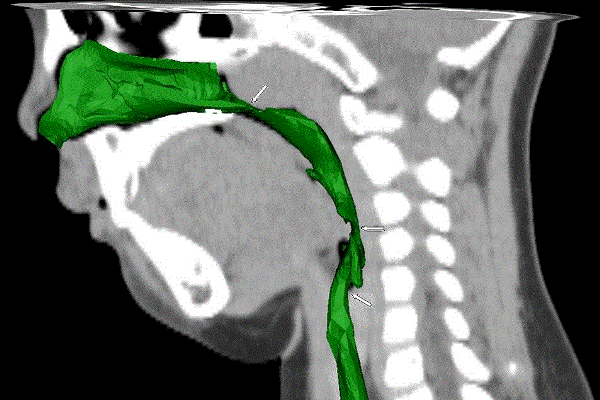
During quantitative study on the constructed model we found that most OSAHS children’s upper airway stegnosis appeared in multiple planes from choana narium along laryngopharynx and formed a discontinuous stegnosis, and the narrowest part often located in the nasopharynx or oropharynx plane (Figure 5). This morphous characteristic was not mentioned in other domestic studies, and this was the advantage brought by 3-dimensional model which could provide more information than traditional 2-dimensional image. Besides, compliances change of upper airways was also regarded as an important morbidity factor for OSAHS. On the basis of constructing model, we measured and compared the upper airway volumes and found that upper airway volume of children was significantly bigger when they were awake breathing than they were asleep breathing, and the minimum cross section area of airway was also larger than they were asleep. Differences showed statistical significance. However, when normal individuals were breathing, the upper airway distension muscular tension was in a dynamic balance with pharyngeal cavity negative pressure to ensure the openness and smoothness of pharyngeal cavity. Result of this study could indicate that the compliance of pharyngeal wall of OSAHS children increased which would easily lead to collapse and obstruction when the children inspired air. This change could reflect the difference of upper airway compliances of airways when the children were awake and asleep to some extent, and could objectively reflect the position, range and extent of the stegnosis and the collapse. In the past, we often diagnosed severe cases of OSAHS children by clinical symptoms and sleep monitoring in clinical practice, but we were lack of good methods to pre-judge the specific stegnosis or the illness degree. This 3-dimensional model method would provide more anatomical references for the diagnosis of severe cases. As for treatment, for those severe cases of OSAHS children, operation was still the major treatment method. However, as those OSAHS children often had stegnosis in multiple planes, if we performed operation to solve the problem in only one plane we couldn’t achieve satisfactory results. And for these patients, the operation was more difficult, anaesthesia status was difficult to control, complication rate during the perioperative process was high, post-operation outcomes were not quite satisfactory, so to choose a correct interference method was always the challenge we had to face in clinical practice. By 3-dimensional model construction, we could precisely locate the stegnosis and collapse point, the range and extent of the children’s upper airways. By comprehensively judging and evaluating these factors and appropriately choose multiple treatment methods such as CAPA, we could improve the therapeutic outcomes of those severe cases of OSAHS children. In this regard, the 3-dimensional reconstruction of upper airways and volume measurement had unique advantages.
With our measurement by using 3-dimensional model construction technology, we could directly reflect the airway volume changes of airway compliances, observe the position, range, extent and direction of the stegnosis and collapse of upper airway, and could study the morphous and functional features of upper airways of OSAHS children. The maneuverability and effectiveness were primarily proved in this study and this method was a relatively good way to study on the morphous and function of upper airway. In the following studies, we would enlarge the sample size and add control groups to make more systematical and exquisite studies on the morphous and functions of upper airways of OSAHS children.
1Software Specifications: the 3-dimensional reconstruction software adopted in this research was 3DMIA, automatically developed by the Computer School of South China Normal University (the code number of software copyright: 2008SR18799, 2008SR18798). The software could be used in the following areas: registering, segmentation (level set, region growing), volume-rendering, 3-dimensional reconstruction (including the adjustments of window width and window level) and surface rendering 3-dimensional reconstruction. Each part of the model could be used to observe the tissue. The tissue could be grouped randomly to be observed and be randomly amplified or diminished. Transparent observation could be set randomly. The produced document was in the form of STL, and could be opened and viewed with 3DMAX and other ordinary 3-dimensional production software but could not be measured.
References
- Stephen H. Sheldon, Richard Ferber, Meir H. Kryger (2005) Principles and Practice of Pediatric sleep medicine. Elsevier Science Health Science div. 207.
- Jiahui Pan, Chao Cheng, Susu Bao, Dabo Liu, Jianping Ye (2013) Study of Computer-aided Diagnosis Method of Childhood Obstructive Sleep Apnea Syndrome. J Comput Biol 9: 5837- 5844.
- Jiahui Pan, Susu Bao (2010) One Biliary Tract Virtual Surgery Simulation System; Application Research of Computers (02) .
- Section on Pediatric Pulmonology, Subcommittee on Obstructive Sleep Apnea Syndrome American Academy of Pediatrics. (2002) Clinical practice guideline: diagnosis and management of childhood obstructive sleep apnea syndrome. Pediatrics 109: 704-712.
- Redline S1, Tishler PV, Schluchter M, Aylor J, Clark K, et al. (1999) Risk factors for sleep-disordered breathing in children. Associations with obesity, race, and respiratory problems. Am J Respir Crit Care Med 159: 1527-1532.
- Morales-Angulo C, Gallo-Terán J, Azuara N, Rama Quintela J (2006) [Otorhinolaryngo logical manifestations in patients with Down syndrome]. Acta Otorrinolaringol Esp 57: 262-265.
- Erler T, Paditz E (2004) Obstructive sleep apnea syndrome in children: a state-of-the-art review. Treat Respir Med 3: 107-122.
- Major MP, Flores-Mir C, Major PW (2006) Assessment of lateral cephalometric diagnosis of adenoid hypertrophy and posterior upper airway obstruction: a systematic review. Am J Orthod Dentofacial Orthop 130: 700-708.
- Ruoff CM, Guilleminault C (2012) Orthodontics and sleep-disordered breathing. Sleep Breath 16: 271-273.
- Powell N, Guilleminault C (2009) Abnormal pharyngeal airflow in obstructive sleep apnea using computational fluid dynamics: Feasibility study. Proceeding of the 9th World Congress on Sleep.Apnea (Seoul, Korea).
Citation: Liu D, Cheng C, Pan J, Bao S (2014) Preliminary Study on the Application of Upper: Airway Model Construction with 3DMIA in OSAHS of Children. Otolaryngol (Sunnyvale) 4:175. DOI: 10.4172/2161-119X.1000175
Copyright: © 2014 Liu D .et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 15017
- [From(publication date): 10-2014 - Aug 16, 2025]
- Breakdown by view type
- HTML page views: 10388
- PDF downloads: 4629