Risk Factors for HIV Infection among Thai Young Men Aged 21-23 Years
Received: 21-May-2014 / Accepted Date: 31-May-2016 / Published Date: 07-Jun-2016 DOI: 10.4172/2161-1165.1000248
Abstract
Background: Young men are a highly susceptible group for HIV infection. This study aimed to identify HIV risk factors among Thai young men aged 21-23 years for appropriate preventive interventions.
Methods: A case control study was conducted among 240 HIV positive and 240 HIV negative young men matched for residential areas, using a 6-part questionnaire booklet, consisting of demographic data, addictive behaviors, sexual behaviors, HIV/AIDS knowledge and attitude, condom knowledge, attitude and practice and psychosocial data. The SPSS version 10 software were used for data analysis.
Results: From univariate analysis, the significant risk factors were: urban housing area (OR=1.61); labor occupation (OR=1.70); income of more than 2000 Baht/month (OR=1.74); early secondary level of education and lower (OR=2.71); smoking (OR=2.46); alcohol use (OR=1.61); marijuana use (OR=4.57); amphetamine use (OR=3.44); heroin use (OR=9.32); alcohol use before sex (OR=1.74); drug use before sex (OR=3.76); IDU (OR=6.02); needle sharing (OR=5.80); first sex with female sex workers (FSWs) (OR=3.52); having more than 3 lifetime sex partners (OR=2.14); history of anal sex (OR=2.25); history of STDs (OR=2.80); HIV risk perception (OR=1.61); high speed driving preference (OR=2.73); unability of safe sex talk with partners (OR=1.78); unworrying about HIV (OR=2.28). From multiple logistic regression analysis, the variables found to be predictive of HIV positivity were: income of more than 2000 Baht/month (OR=1.94, 95% CI=1.13, 3.31); heroin use (OR=4.18, 95% CI=1.03, 16.89); drug use before sex (OR=2.20, 95 % CI=1.13, 4.29); first sex with FSWs (OR=3.47, 95 % CI=1.69, 7.13); HIV risk perception (OR=1.86, 95% CI=1.07, 3.25); unworrying about HIV (OR=1.88, 95% CI=1.16, 3.07).
Conclusions: The HIV risk factors can be used for intervention programs for HIV prevention and develop a risk assessment scale to indicate which young men are at-risk for HIV infection and should be educated or counseled to reduce their risks.
Keywords: Risk factors, HIV infection, Thai, Young men
164688Introduction
HIV/AIDS problem is one of the greatest challenges to global public health with variable patterns of transmission and impact among world regions [1]. Primary prevention through education which can result in decreased risk-taking behaviors, especially changes in sexual behavior and condoms use which can reduce HIV seroprevalence in high-risk populations, are the most effective methods of avoiding HIV [2]. It was recognized that HIV transmission was associated with multiple risk factors. A combination of biological, behavioral, and social factors may account for the influence of primary prevention on the HIV epidemic. HIV prevention measures can be focused on each of these factors and young people are a focus of the national AIDS program [3]. The first AIDS case in Thailand was diagnosed in 1984 [4]. It was estimated that there were nearly 520,000 people (ages 15-49) living with HIV and AIDS, Thailand has the highest adult HIV prevalence in the South East Asia region in 2010 [5]. Sexual behavior patterns within Thai society have been the most important contributions to the disease transmission [6]. Young men are a highly susceptible group for HIV infection. Typically, the young recruit on a weekend pass has both the time and motivation, particularly under the influence of peer pressure, to indulge in high-risk behaviors [7].
Thai army conscripts come from young Thai men aged 21-23 years, chosen by lottery system according to Thai laws from all 21 year old of Thai men to work in the military service, mostly in the Royal Thai Army (RTA). There are approximately 60,000 new conscripts every year to work for two years in the army, divided into two groups; the first group enters the army in May and the second in November. All of them have been tested for HIV in the first month of their entry since 1989 for readiness of the strong troops and appropriate work. The HIV infection rate in army conscripts have reflected the infection rate of young Thai men, since such information are derived from the HIV testing in the cohort of Thai men at age of 21-23 years. The infection rates tended increase from 0.5% to peak at 3.7% in 1993, and gradually declined [8]. The conscripts are considered to include in 3 high-risk groups of HIV infection according to their unique demographic characteristics, i.e. men, young people and mobile population. Among Thai army conscripts, there is a high rate of HIV risks [9-12]. The results from the 1996 sexual behavior survey of them showed that there is reduction in risk sexual behaviors, but the change was unsatisfactory because they still had high risk sexual behaviors [13] which meant that they might contract HIV.
Essentially, all new HIV infections can be prevented if people can be helped to make changes in sexual and drug use practices. Perhaps the most difficult area of HIV prevention lies in the area of behavior change. Biomedical based behavioral research has concentrated on special risk groups. From a behavioral public health perspective, those less researched and understood are the residual categories of people potentially “at risk” and young men are among them. A comprehensive behavior change intervention strategy must be designed to address specific target groups in which HIV is being transmitted [14], to take account of the stage and the progress of the epidemic. There is often a gap between knowledge and behavior, and it requires considerable assistance and support to change risky patterns. There are many studies that show the associations between risk factors and HIV infection. These risk factors are: low education level, not living with parents/wife, low economic status, HIV misconception, low perceived risk of HIV, smoking, substance use, risk taking behaviors (e.g. non-use of seatbelt, helmet), early age at first sex, no condom use at first sex, having sex with female sexual workers (FSWs), having sex with men, multiple sex partners, history of STDs [15-19]. Other risk factors are condom misconception, low perceived benefit of condom [20,21]; substance use, alcohol use before sex [10,22-24]; low self-efficacy and other psychosocial factors [25,26]. Some experts claim that single marital status may associate with risk factors [27]. From those risk factors, the level of association with HIV infection can be studied for specific risk factors for more effective HIV prevention among young Thai men.
Methods
The association between risk factors and HIV serostatus was determined by using case control studies. The sample size was obtained from the formula:
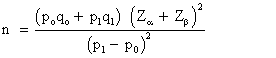
The sample size will be at least 38 conscripts for each risk factor. This study includes 6 risk factors. Then, the sample size is 38 × 6=228. The sample size should be 240 in each group.
The instrument was 6-part questionnaire. All items of the questionnaire were modified to dichotomous answers. It was pretested among 20 HIV positive and 40 HIV negative conscripts and revised before data collection, yielding a 6-part questionnaire booklet. It is composed of demographic factors (7 items), addictive behaviors (8 items), sexual behaviors (8 items), HIV/AIDS knowledge and attitude (8 items), condom knowledge, attitude and practice (4 items) and psychosocial factors (18 items). HIV testing was performed by using ELISA for screening and Western blot for confirmatory test. The results of HIV positive conscripts will be sent to the counselors.
240 HIV positive conscripts and 240 HIV negative conscripts, matched for working in the same army units, were recruited as participants to complete a questionnaire booklet. Verbal consent was obtained and the trained HIV/AIDS counselors, working in the RTA hospitals, were responsible for data collection. Data collection was performed between 1999 and 2001. The complete data for analysis were obtained from 234 HIV negative and 203 HIV positive conscripts.
The crude Odds Ratio (OR) and the difference between groups were obtained by using the social science statistical software in univariate analysis. Then, the logistic regression was applied for controlling confounders and evaluating the effect of risk variables on HIV infection. The variables that were significant (p<0.05) and the corresponding p-values (p<0.1) were entered into the logistic regression model and the adjusted OR’s of significant risk factors were obtained.
Results
The samples were 203 HIV positive conscripts and 234 HIV negative conscripts. The average age, marital status, residence, education, occupation before being conscripts were analysed (Table 1).
| Chracteristics | HIV+n(%) | HIV-n(%) | Total n(%) |
|---|---|---|---|
| Number | 203 | 234 | 437 |
| Age (years) | |||
| 21-22 | 153 (75.4) | 178 (76.1) | 331 (75.7) |
| 23 and over | 50 (24.6) | 56 (23.9) | 106 (24.3) |
| Total | 203 (100) | 234 (100) | 437 (100) |
| Mean | 21.9±1.2 | 21.9±1.1 | 21.9±1.1 |
| Marital status | |||
| Single | 151 (75.5) | 182 (78.4) | 333 (77.1) |
| Married | 22 (11.0) | 37 (15.9) | 59 (13.6) |
| Divorced | 4 (2.0) | 1 (0.4) | 5 (1.2) |
| Widowed | 7 (3.5) | 1 (0.4) | 8 (1.8) |
| Illegal wife* | 16 (8.0) | 1 (4.7) | 27 (6.2) |
| Total | 200 (100) | 232 (100) | 432 (100) |
| Native area | |||
| North | 41 (20.1) | 55 (23.5) | 96 (22.0) |
| Northeast | 44 (21.6) | 57 (24.4) | 101 (23.1) |
| Central | 69 (33.9) | 72 (30.8) | 141 (32.3) |
| South | 49 (24.1) | 50 (21.4) | 99 (22.6) |
| Total | 203 (100) | 234 (100) | 437 (100) |
| Education | |||
| Elementary and lower | 70 (34.6) | 58 (24.9) | 128 (29.4) |
| Early secondary | 70 (34.6) | 48 (20.6) | 118 (27.1) |
| Late secondary | 50 (24.8) | 81 (34.8) | 131 (30.1) |
| Vocational/subbachelor | 8 (4.0) | 35 (15.0) | 43 (9.9) |
| Bachelor and higher | 4 (2.0) | 11 (4.7) | 16 (3.7) |
| Total | 202 (100) | 233 (100) | 435 (100) |
| *Note: Illegal wife means the woman who lives with a man and behaves as wife and husband, but no legal registration. | |||
Table 1: Demographic characteristics of sample conscripts.
After univariate analysis, the significant association between risk factors and HIV infection included urban housing area, labor occupation, income of more than 2000 Baht/month, early secondary level of education and lower, smoking, alcohol use, marijuana use, amphetamine use, heroin use, alcohol use before sex, drug use before sex, first sex with FSWs, having more than 3 lifetime sex partners, history of anal sex, history of STDs, HIV risk perception, high speed driving preference, inability of safe sex talk with partners and unworrying about HIV (Tables 2-8).
| Characteristics | HIV+ n(%) | HIV-n(%) | Total n(%) |
|---|---|---|---|
| Housing area | |||
| Urban | 84 (45.2) | 74 (33.8) | 158 (39.0) |
| Rural | 102 (54.8) | 145 (66.2) | 247 (61.0) |
| Total | 186 (100) | 219 (100) | 405 (100) |
| Previous occupation | |||
| None | 4 (2.0) | 3 (1.3) | 7 ( 1.6) |
| Agriculture | 42 (21.0) | 53 (23.1) | 95 (22.1) |
| Fisherman | 3 (1.5) | 3 (1.3) | 6 (1.4) |
| Government officials | 2 (1.0) | 1 (0.4) | 3 (0.7) |
| Private organization | 34 (17.0) | 35 (15.3) | 69 (16.1) |
| Laborers | 70 (35.0) | 55 (24.0) | 125 (29.1) |
| Students | 34 (17.0) | 67 (29.2) | 101 (23.5) |
| Commerce | 10 ( 5.0) | 12 (5.2) | 22 ( 5.1) |
| Sex workers | 1 (0.5) | - | 1 ( 0.2) |
| Total | 200 (100) | 229 (100) | 429 (100) |
| Monthly income | |||
| 1,000 B and less | 40 (20.1) | 74 (32.0) | 114 (26.5) |
| 1,001-2,000 | 7 (3.5) | 13 ( 5.6) | 20 ( 4.6) |
| 2,001-3,000 | 24 (12.1 ) | 26 (11.2) | 50 (11.6) |
| 3,001-4,000 | 40 (20.1) | 29 (12.6) | 69 (16.0) |
| 4.001-5,000 | 39 (19.6 ) | 32 (13.8) | 71 (16.5) |
| 5,001 and over | 49 (24.6) | 57 (24.7) | 106 (24.6) |
| Total | 199 (100) | 231 (100) | 430 (100) |
Table 2: Demographic characteristics of sample conscripts (continued).
| HIV+ n (%) | HIV- n (%) | Crude OR (95% CI) | p-value | |
|---|---|---|---|---|
| N | 203 | 234 | ||
| Age (Mean) | 21.9 | 21.9 | ||
| Single marital status | ||||
| Yes | 151 (74.4) | 182 (77.8) | 0.83 (0.52. 1.32) | 0.47 |
| No | 52 (25.6) | 52 (22.2) | 1.00 | |
| Total | 203 (100) | 234 (100) | ||
| Urban housing area | ||||
| Yes | 84 (45.2) | 74 (33.8) | 1.61 (1.06.2.44 ) | 0.01 |
| No | 102 (54.8) | 145 (66.2) | 1.00 | |
| Total | 186 (100) | 219 (100) | ||
| Early secondary education or lower | ||||
| Yes | 140 (69.3) | 106 (45.5) | 2.71 (1.78.4.11) | 0.000 |
| No | 62 (30.7) | 127 (54.5) | 1.00 | |
| Total | 202 (100) | 233 (100) | ||
| Labor occupation | ||||
| Yes | 70 (34.5) | 55 (23.5) | 1.71 (1.102.67) | 0.015 |
| No | 133 (65.5) | 179 (76.5) | 1.00 | |
| Total | 203 (100) | 234 (100) | ||
| Monthly income 2,000 Baht and above | ||||
| Yes | 152 (76.4) | 144 (62.3) | 1.74 (1.16, 2.61) | 0.005 |
| No | 47 (23.6) | 87 (37.7) | 1.00 | |
| Total | 199 (100) | 231 (100) | ||
| Mostly not living with parents/wife | ||||
| Yes | 36 (17.7) | 52 (22.2) | 0.75 ( 0.45, 1.24) | 0.29 |
| No | 167 (82.3) | 182 (77.8) | 1.00 | |
| Total | 203 (100) | 234 (100) | ||
Table 3: Comparison of demographic characteristics of HIV+ and HIV- conscripts.
| Variables | HIV+ n(%) | HIV-n(%) | Crude OR (95% CI) | p-value |
|---|---|---|---|---|
| N | 203 | 234 | ||
| Smoking | ||||
| Yes | 129 (63.5) | 97 (41.4) | 2.46 (1.49,4.26) | 0 |
| No | 74 (36.4) | 137 (58.5) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Alcohol use | ||||
| Yes | 101 (49.8) | 89 (38.0) | 1.61 (1.08,2.41) | 0.009 |
| No | 102 (50.2) | 145 (62.0) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Marijuana use | ||||
| Yes | 15 (7.4) | 4 (1.7) | 4.57 (1.43,19.25) | 0.003 |
| No | 188 (92.6) | 230 (98.3) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Amphetamine use | ||||
| Yes | 27 (13.3) | 10 ( 4.3) | 3.44 (1.53,7.88) | 0.001 |
| No | 176 (86.7) | 224 (95.7) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Heroin use | ||||
| Yes | 22 (10.8) | 3 (1.3) | 9.32 (2.74,49.39) | 0 |
| No | 181 (89.2) | 231 (98.7) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Thinner use | ||||
| Yes | 8 (3.9) | 7 (3.0) | 1.33 (0.43,4.20) | 0.38 |
| No | 195 (96.1) | 227 (97.0) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Alcohol use before sex | ||||
| Yes | 136 (67.0) | 126 (53.8) | 1.74 (1.15,2.63) | 0.003 |
| No | 67 (33.0) | 108 (46.2) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Use drug before sex | ||||
| Yes | 61 (30.0) | 24 (10.3) | 3.76 (2.16,6.56) | 0 |
| No | 142 (70.0) | 210 (89.7) | 1 | |
| Total | 203 (100) | 234 (100) | ||
Table 4: Comparison of addictive behaviors between HIV+ and HIV- conscripts.
| Variables | HIV+ n (%) | HIV-n (%) | Crude OR (95% CI) | p-value |
|---|---|---|---|---|
| N | 203 | 234 | ||
| First sex with FSWs | ||||
| Yes | 46 (22.7) | 18 (7.7) | 3.52 (1.89, 6.61) | 0 |
| No | 157 (77.3) | 216 (92.3) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Nonuse condom in first sex | ||||
| Yes | 113 (55.7 ) | 140 (59.8) | 0.84 (0.56, 1.26) | 0.43 |
| No | 90 (44.3) | 94 (40.2) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Had sex with FSWs last year | ||||
| Yes | 27 (13.3) | 15 (6.4) | 2.24 (1.10, 4.60) | 0.02 |
| No | 176 (86.7) | 219 (93.6) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Nonuse condom last time with non-wife | ||||
| Yes | 68 (33.5) | 64 (27.4) | 1.34 (0.87, 2.06) | 0.19 |
| No | 135 (66.5) | 170 (72.6) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| More than 3 lifetime sexual partners | ||||
| Yes | 100 (49.3) | 74 (31.6) | 2.10 (1.39,3.17) | 0.0002 |
| No | 103 (50.7) | 160 (68.4) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Ever had sex with men | ||||
| Yes | 13 (6.4) | 6 (2.6) | 2.59 (0.90,8.49) | 0.08 |
| No | 190 (93.6) | 228 (97.4) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Had anal intercourse | ||||
| Yes | 22 (11.1) | 12 (5.2) | 2.25 (1.02,5.01) | 0.04 |
| No | 177 (88.9) | 217 (94.8) | 1 | |
| Total | 199 (100) | 229 (100) | ||
| Ever had STDs | ||||
| Yes | 42 (21.1) | 21 (9.1) | 2.66 (1.46,4.89) | 0.001 |
| No | 157 (78.9) | 209 (90.9) | 1 | |
| Total | 199 (100) | 230 (100) | ||
Table 5: Comparison of sexual behaviors between HIV+ and HIV- conscripts.
| Variables | HIV+n (%) | HIV-n (%) | Crude OR (95% CI) | p-value |
|---|---|---|---|---|
| N | 203 | 234 | ||
| You can be infected with HIV by traveling with HIV-infected persons. | ||||
| Incorrect | 56 (27.6) | 48 (20.5) | 0.68 (0.42, 1.08) | 0.11 |
| Correct | 147 (72.4) | 186 (79.5) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| The mosquito can carry HIV to infect you by biting. | ||||
| Incorrect | 159 (78.3) | 184 (78.6) | 0.98 (0.60, 1.60) | 0.97 |
| Correct | 44 (21.7) | 50 (21.4) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| You can be infected with HIV by using the same toilet with HIV-infected person. | ||||
| Incorrect | 166 (81.8) | 188 (80.3) | 1.10 (0.66, 1.83) | 0.79 |
| Correct | 37 (18.2) | 46 (19.7) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| In the present time, AIDS can be completely cured. | ||||
| Incorrect | 133 (65.5) | 159 (67.9) | 0.90 (0.59, 1.37) | 0.66 |
| Correct | 70 (34.5) | 75 (32.1) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Good-looking woman cannot be HIV-infected person. | ||||
| Incorrect | 132 (65.0) | 151 (64.5) | 1.02 (0.67, 1.55) | 0.99 |
| Correct | 71 (35.0) | 83 (35.5) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Homosexual men are not only one group that are HIV risky. | ||||
| Incorrect | 115 (56.7) | 162 (69.2) | 1.72 (1.14, 2.66) | 0.008 |
| Correct | 88 (43.3) | 72 (30.8) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| AIDS can happen to me. | ||||
| Yes | 150 (73.9) | 149 (63.7) | 1.61 (1.04, 2.50) | 0.02 |
| No | 53 (26.1) | 85 (36.3) | 1 | |
| Total | 203 (100) | 234 (100) | ||
Table 6: Comparison of knowledge and attitude of HIV/AIDS between HIV+ and HIV- conscripts.
| Variables | HIV+ n (%) | HIV- n (%) | Crude OR (95% CI) | p-value |
|---|---|---|---|---|
| N | 203 | 234 | ||
| Do you think putting a condom on penis would interrupt sex? | ||||
| Yes | 129 (63.5) | 156 (66.7) | 0.87 (0.57, 1.32) | 0.56 |
| No | 74 (36.5) | 78 (33.3) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Have you ever talked with your friends or else about condom? | ||||
| No | 34 (16.8) | 28 (12.1) | 1.47 (0.83,2.63) | 0.2 |
| Yes | 168 (83.2) | 204 (87.9) | 1 | |
| Total | 202 (100) | 232 (100) | ||
| When you had sex with nonsteady partner in the last 12 months, did you use condom? | ||||
| No | 114 (56.2) | 115 (49.1) | 1.33 (0.89, 1.97) | 0.17 |
| Yes | 89 (43.8) | 119 (50.9) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Do you think most of your friends use condoms when having sex with nonsteady partner? | ||||
| No | 99 (49.7) | 116 (50.4) | 1.02 (0.69, 1.52) | 0.98 |
| Yes | 100 (50.3) | 114 (49.6) | 1 | |
| Total | 199 (100) | 230 (100) | ||
Table 7: Comparison of knowledge, attitude and practice of condoms between HIV+ and HIV- conscripts.
| Variables | HIV+ n (%) | HIV- n (%) | Crude OR (95% CI) | p-value |
|---|---|---|---|---|
| N | 203 | 234 | ||
| I do things my own way, irrespective of what my friends think. | ||||
| Yes | 34 (16.7) | 39 (16.7) | 1.01 (0.59, 1.72) | 0.91 |
| No | 169 (83.3) | 195 (83.3) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| If I do not have sex with lots of lovers, I would feel unattractive. | ||||
| Yes | 39 (19.2) | 36 (15.4) | 1.71 (0.77, 2.23) | 0.35 |
| No | 164 (80.8) | 198 (84.6) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| I do not worried about contracting HIV. | ||||
| Yes | 110 (54.2) | 80 (34.2) | 2.28 (1.51, 3.43) | 0 |
| No | 93 (45.8) | 154 (65.8) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| I believe it is possible for me to practice safer sex. | ||||
| No | 39 (19.2) | 32 (13.7) | 1.50 (0.87, 2.59) | 0.15 |
| Yes | 164 (80.8) | 202 (86.3) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| If a condom is not available, it would be worth the effort to discontinue sexual activityto obtain a condom. | ||||
| No | 25 (12.3) | 18 (7.7) | 1.69 (0.85, 3.36) | 0.14 |
| Yes | 178 (87.7) | 216 (92.3) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| You worry every time you meet the strangers. | ||||
| Yes | 12 (5.9) | 12 (5.1) | 1.16 (0.47, 2.86) | 0.88 |
| No | 191 (94.1) | 222 (94.9) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| When you are asked to do something, you are always anxious. | ||||
| Yes | 23 (11.3) | 16 (6.8) | 1.74 (0.85, 3.60) | 0.14 |
| No | 180 (88.7) | 218 (93.2) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| You are easily angry when you face disappointed situation. | ||||
| Yes | 58 (28.6) | 61 (26.1) | 1.13 (0.73, 1.77) | 0.63 |
| No | 145 (71.4) | 173 (73.9) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| You like driving a car or riding a motorcycle with high velocity. | ||||
| Yes | 115 (68.5) | 178 (85.6) | 2.73 (1.60,4.70) | 0.0001 |
| No | 53 (31.5) | 30 (12.8) | 1 | |
| Total | 168 (100) | 234 (100) | ||
| When you drive car / ride motorcycle, do you often use seatbelt/helmet | ||||
| Yes | 35 (17.2) | 46 (19.7) | 0.85 (0.51, 1.43) | 0.6 |
| No | 168 (82.8 | 188 (80.3 | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Did you feel as if your life had been a failure? | ||||
| Yes | 41 (20.6) | 35 (15.1 | 1.46 (0.86, 2.49) | 0.17 |
| No | 158 (79.4) | 197 (84.9) | 1 | |
| Total | 199 (100) | 232 (100) | ||
| You cannot sleep well. | ||||
| Yes | 50 (25.0) | 61 (26.2) | 0.94 (0.59, 1.49) | 0.86 |
| No | 150 (75.0) | 172 (73.8) | 1 | |
| Total | 200 (100) | 233 (100) | ||
| Did you feel lonely? | ||||
| Yes | 73 (36.5) | 72 (30.9) | 1.24 (0.84, 1.96) | 0.26 |
| No | 127 (63.5) | 161 (69.1) | 1 | |
| Total | 200 (100) | 233 (100) | ||
| Would you be able to refuse sex if your partner did not want you to use condom? | ||||
| Yes | 84 (41.4) | 103 (44.0) | 0.90 (0.60,1.34) | 0.64 |
| No | 119 (58.6) | 131 (66.0) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Can you stop and look for condom even if you are sexually aroused? | ||||
| Yes | 50 (24.6) | 52 (22.2) | 1.14 (0.71,1.83) | 0.63 |
| No | 153 (75.4) | 182 (77.8) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Would you use condoms even if you had been drinking or using drugs? | ||||
| Yes | 70 (34.5) | 65 (27.8) | 1.37 (0.89,2.11) | 0.15 |
| No | 133 (65.5) | 169 (72.2) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Do you think you will use condom when having sex with your nonsteady partners? | ||||
| Yes | 35 (17.2) | 32 (13.7) | 1.32 (0.75,2.30) | 0.36 |
| No | 168 (82.8) | 202 (86.3) | 1 | |
| Total | 203 (100) | 234 (100) | ||
| Are you sure you can talk about safe sex with your sexual partner? | ||||
| Yes | 88 (44.2) | 71 (30.9) | 1.78 (1.17,2.69) | 0.006 |
| No | 111 (55.8) | 159 (69.1) | 1 | |
| Total | 199 (100) | 230 (100) | ||
Table 8: Comparison of psychosocial characteristics between HIV+ and HIV conscripts.
After multivariate analysis was applied, 6 variables were found to be related to HIV infection: (1) income of more than 2000 Baht/month (OR=1.94), (2) heroin use (OR=4.18), (3) drug use before sex (OR=2.20), (4) first sex with FSWs (OR=3.47), (5) perception of HIV risk (OR=1.86), and (6) unworrying about HIV (OR=1.88) (Tables 9-11).
| Risk Factors | Crude OR | 95% CI | p value |
|---|---|---|---|
| Urban housing area | 1.61 | 1.06, 2.41 | 0.013 |
| Labor occupation | 1.7 | 1.10, 2.64 | 0.01 |
| Income > 2000 Baht/month | 1.74 | 1.16, 2.61 | 0.002 |
| Early secondary education and lower | 2.71 | 1.78, 4.11 | 0 |
| Smoking | 2.46 | 1.49, 4.26 | 0 |
| Alcohol use | 1.61 | 1.08, 2.41 | 0.009 |
| Marijuana use | 4.57 | 1.43, 19.25 | 0.003 |
| Amphetamine use | 3.44 | 1.53, 7.88 | 0.001 |
| Heroin use | 9.32 | 2.74, 49.39 | 0 |
| Alcohol before sex | 1.74 | 1.15, 2.63 | 0.003 |
| Drug use before sex | 3.76 | 2.16, 6.56 | 0 |
| First sex with FSWs | 3.52 | 1.89, 6.61 | 0 |
| More than 3 sex partners | 2.14 | 1.44, 3.17 | 0.0003 |
| History of anal sex | 2.25 | 1.12, 4.71 | 0.03 |
| History of STDs | 2.8 | 1.60, 5.02 | 0.0004 |
| HIV risk perception | 1.61 | 1.04, 2.50 | 0 |
| High speed driving preference | 2.73 | 1.60, 4.70 | 0.001 |
| Unability of safe sex talk with partner | 1.78 | 1.17, 2.69 | 0.006 |
| Unworrying about HIV | 2.28 | 1.51, 3.43 | 0 |
Table 9: Summary of risk factors for HIV infection among Thai army conscripts from univariate analysis.
| Variables | β | SE | Wald | OR | 95% CI | Sig |
|---|---|---|---|---|---|---|
| Income (>2000 vs. others) | 0.661 | 0.2739 | 5.8235 | 1.94 | (1.13, 3.31) | 0.0158 |
| Heroin use (yes vs. no) | 1.4299 | 0.7127 | 4.0254 | 4.18 | (1.03,16.89) | 0.0448 |
| Drug use before sex (yes vs. no) | 0.79 | 0.34 | 5.3969 | 2.2 | (1.13, 4.29) | 0.0202 |
| First sex with FSWs (yes vs. no) | 1.2434 | 0.3676 | 11.4433 | 3.47 | (1.69, 7.13) | 0.0007 |
| HIV risk perception (yes vs. no) | 0.6248 | 0.2833 | 4.8635 | 1.86 | (1.07, 3.25) | 0.0274 |
| Unworry about HIV (yes vs. no) | 0.6331 | 0.2489 | 6.4685 | 1.88 | (1.16, 3.07) | 0.011 |
Table 10: Logistic equation based on the data in phase 1.
| Risk Factors | Adjusted OR | 95% CI |
|---|---|---|
| Income more than 2000 Baht/month | 1.94 | 1.13, 3.31 |
| Heroin use | 4.18 | 1.03, 16.89 |
| Drug use before sex | 2.2 | 1.13, 4.29 |
| First sex with FSWs | 3.47 | 1.69, 7.13 |
| HIV risk perception | 1.86 | 1.07, 3.25 |
| Unworrying about HIV | 1.88 | 1.16, 3.07 |
Table 11: Risk factors for HIV infection among Thai army conscripts from multivariate logistic regression analysis.
Discussion
This study demonstrated 6 significant risk factors for HIV infection among Thai army conscripts: (1) income of more than 2000 Baht/ month (demographic factor), (2) heroin use (addictive behavior), (3) drug use before sex (addictive behavior and sexual behavior), (4) first sex with FSWs (sexual behavior), (5) perception of HIV risk (attitude to HIV and psychosocial factor), and (6) unworrying about HIV (attitude to HIV and psychosocial factor).
It should be noted that almost all of the 6 risk factors of this study are related to behavior, i.e. addictive behavior, sexual behavior and psychosocial behavior. Psychosocial behavior played a role in the control of addictive and sexual behaviors. Addictive behavior could also influence psychosocial and sexual behaviors to take HIV risks.
In this study, most of the risk factors obtained from the logistic regression analysis are behavioral factors of hosts or conscripts, i.e. addictive behavior, sexual behavior and psychological behavior. Only income more than 2,000 Baht/month is not directly risk behavior but it is indirectly related to risk behavior.
The income of 2000 Baht/month or over was found to significantly associate with HIV infection. The reasons may be that the more money the subjects had, the more occasions they could buy alcohol, drugs and sex, which facilitated HIV transmission.
The use of heroin was the strongest predictor of HIV infection in this study. The reason is people who use heroin usually inject it and share syringes or needles, which may be contaminated with HIV22, [28].
Alcohol and other drug use are risk-taking behaviors for HIV because mood-altering drugs can impair judgment and lead to risky behavior. In other words, when someone uses drugs, such as marijuana, amphetamine, before having sex, they may forget safe sex and can contract HIV [29].
The sexual behavior of first sexual intercourse was related to protective behavior in the later behavior. A study showed that youths who used a condom from the onset of sexual activity were more likely to have used a condom in the most recent intercourse occasion, less likely to be diagnosed with a STD and less likely to combine substance use with sexual activity [30]. This is the clue for HIV prevention.
It was demonstrated that the conscripts who perceived the risk of HIV were more likely to be HIV positive. The Health Belief Model theory can be used to explain the association. These basic components include subjective perceptions of: (1) vulnerability to the negative event, (2) severity of the negative event, (3) benefits of specific preventive actions, and (4) barriers to performing preventive actions. Perceived personal vulnerability is usually depicted as a necessary (but not sufficient) motivator of precautionary behavior. In addition, emotionality may influence person’s perception of threat. Risk perception is not enough for a person to practice preventive behaviors [31]. HIV risk perception is also demonstrated to be unrelated to injecting or sexual behaviors and previous history of STDs [28]. Focus group discussions revealed that the risk perception for acquiring HIV was decreased by never knowing a person with HIV, because FSWs had health certificates for STD-free, and by the belief that HIV/AIDS could be cured or prevented with folk medicines [32]. This made some conscripts underestimate the risk of HIV infection, remain unconcerned about HIV/AIDS and perform HIV- related risk behavior.
Many studies showed that some but not all beliefs about HIV have changed over time. In 1986, the survey revealed that 46% of people worried about becoming infected with HIV and 9% thought it likely they will get AIDS in their lifetime. In 1988, the proportion of respondents doubled who indicated that they were worried about AIDS (74%) and who thought it likely they will get AIDS in their lifetime (18%). There has been significant increase in the perceived likelihood of sexual transmission from 1988 to 1991 [33]. Adolescents’ worry of STDs and HIV had different sets of correlates. Recent history of STDs was associated with HIV worry and partner-specific barriers were related to HIV worry [34]. Unworrying about HIV/AIDS may make the conscripts careless and engage in drug use and unprotected sexual behaviors.
Surprisingly, in this study, nonuse of condom both in first sex and last time with FSWs did not associate significantly with HIV infection. It was the same as the study in the north of Thailand [16] that showed no protective effect of condom use in commercial sex. This is understandable in the context of condom promotion and changing condom use patterns. The men at highest risk may have been the first to adopt condom use. However, with the rapid spread of HIV, many were unknowingly infected before making any behavioral change. In addition, some may have been less than consistent in their condom use at first. This would make condom in the early stages of the epidemic a proxy for risk behavior, explaining the higher HIV levels in those reporting condom uses. However, the use of latex condom is accepted to reduce the risks of STDs, including HIV. In this study, some risk factors were associated with inconsistent condom use that can lead to HIV infection, i.e. drug use before sex and unworrying about HIV.
Some risk factors in this study were significantly associated with HIV infection by univariate analysis but not significantly related after multiple logistic regression analysis. For example, the demographic characteristics that significantly associated with HIV infection only in univariate analysis were urban housing area, labor occupation and finishing early secondary school or lower. For residential areas, it should be noted that the conscripts are not in their natural social environment during military service, since they are living in military camps with only occasional home visits.
Addictive behaviors significantly associated with HIV infection in univariate analysis were smoking, alcohol use, marijuana use, and amphetamine use, alcohol use before sex, IDUs, heroin use, and drug use before sex. Only the last 2 variables were demonstrated to associate with HIV infection in multivariate analysis.
Considering sexual behaviors and related factors, the history of STDs was significantly associated with HIV infection in univariate analysis; this was compatible with other studies [16,18,35] but it was not in multivariate analysis. The history of having sex with men and anal sex are associated with HIV infection in univariate analysis; this was the same as in another study [18], but it was not in multivariate analysis. Having sex with FSWs in the previous year and more than [3] lifetime sex partners were also significantly related to HIV infection in univariate analysis. In many studies, visiting FSWs is the most important factor influencing new HIV infections [18,36].
This study showed that there was no statistical difference concerning the knowledge of HIV/AIDS and condom use between conscripts with different HIV serostatus. There were a lot of studies that showed this fact, such as the study in sexually active Thai men in 1989 which showed that more than 90% possessed knowledge about HIV transmission modes, but only one-third to half of them had ever used a condom [37]. There are a number of reasons why knowledge may have had a limited effect on behavior change. Firstly, where knowledge is universally high there may be insufficient variance to produce statistically significant relationships with other variables, such as change in HIV/AIDS related risk behavior. Secondly, an alternative theoretical explanation is that knowledge only predicts stages in the process of behavior change but not behavior change itself. For example, the precaution adoption model consists of five stages: (1) unaware of the issue; (2) aware of the issue and personally engaged; (3) engaged and deciding what to do; (4) planning to act and not yet having acted; and (5) acting. The provision of information affects decision- making only in the first two stages. Thus the lack of consistent effects due to knowledge may be due to the selection of the wrong outcome variables. Finally, the failure of increased HIV/AIDS knowledge to facilitate appropriate changes in behavior may be due to the type of information provided or the characteristics of the person who perceives it [38].
However, the Thai HIV epidemic has not been static, it has evolved. The behavioral risk factors of young Thai men have been changed over time [39]. As the impact contribution of direct commercial sex was reduced by the country’s efforts, other modes of transmission assumed more visibility and importance. Husband-wife transmission became the dominant route of infection for women. As brothels were increasingly perceived as high risk, commercial sex shifted to indirect sites, many of which were more difficult to identify than brothels. Feelings of safety by the clients at these sites reduced the pressure to use condoms.
There are a lot of research questions in order to change HIV risk behaviors among heterosexual adolescents, such as, whether risk reduction behavioral skills can be increased, whether interventioninduced behavioral change can be sustained, whether the behavior of high-risk populations can be changed and which kinds of interventions are most effective. It is concluded that carefully designed theory-based interventions that take into account the characteristics of the particular population or culture can cause positive changes in adolescents’ HIV-risk behavior, but boundary conditions for their effectiveness still need to be identified [40].
Conclusions
The objective of this study is to identify HIV risk factors in the group of Thai army conscripts which represent Thai young men. There were 19 risk factors from univariate analysis. After removing of confounders by multiple logistic regression, the obtained risk factors were: income more than 2000 Baht/month, heroin use, drug use before sex, first sex with FSWs, perception of HIV risk, and unworrying about HIV.
From these risk factors, the targeted intervention by risk assessment can be implemented and the HIV risk assessment scale can be developed to identify at-risk individuals for appropriate HIV preventive programs in this special group.
References
- Essex M (1997) The human immunodeficiency virus (HIV) as a newly evolving pathogen. Southeast Asian J Trop Med Public Health 28: 127-130.
- Choi KH, Coates TJ (1994) Prevention of HIV infection. AIDS 8: 1371-1389.
- UNAIDS (1998) HIV/AIDS emerging issues and challenges for women, young people & infants (2nd edn.)Geneva.
- Limsuwan A, Kanapa S, Siristonapun Y (1986) Acquired immune deficiency syndrome in Thailand. A report of two cases. J Med Assoc Thai 69: 164-169.
- Havanon N, Bennett A, Knodel J (1993) Sexual networking in provincial Thailand.Stud Fam Plann 24: 1-17.
- UNAIDS (1998) AIDS and the military: UNAIDS point of view. UNAIDS Best Practice Collection. Geneva: UNAIDS
- Mason CJ, Kitsiripornchai S, Markowitz LE, Chanbancherd P, Supapongse T, et al. (1998) Nationwide surveillance of HIV-1 prevalence and subtype in young Thai men. J Acquir Immune DeficSyndr Hum Retrovirol 19: 165-173.
- Celentano DD, Nelson KE, Suprasert S, Wright N, Matanasarawoot A, et al. (1993) Behavioral and sociodemographic risks for frequent visits to commercial sex workers among northern Thai men. AIDS 7: 1647-1652.
- MacQueen KM, Nopkesorn T, Sweat MD, Sawangdee Y, Mastro TD, et al. (1996) Alcohol consumption, brothel attendance, and condom use: normative expectations among Thai military conscripts. Med Anthropol Q 10: 402-423.
- Saengdidtha B, Suppadit W (2001) HIV risk behavior among young men in the Royal Thai Army: the challenge for military preventive medicine.
- Saengdidtha B, Sathityudhakarn O, Wongba N, Muangya C, Suppadit W (2001) Addictive behaviors and prevalence of HIV risk related behaviors among conscripted young Thai men: implications for surveillance and intervention.
- Saengdidtha B, Lapparat G,Torugsa K, Suppadit W, Wakai S (2002) Sexual behaviors and Human Immunodeficiency Virus infection among Thai army conscripts between 1992 and 1998. Mil Med 167: 272-276.
- Kahn JG (1996) The cost-effectiveness of HIV prevention targeting: how much more bang for the buck?Am J Public Health 86: 1709-1712.
- Renzullo PO, McNeil JG, Levin LI, Bunin JR, Brundage JF (1990) Risk factors for prevalent human immunodeficiency virus infection in active duty army men who initially report no identified risk: a case-control study. J Acquir Immune DeficSyndr 3: 266-271.
- Nelson KE, Celentano DD, Suprasert S, Wright N, Eiumtrakul S, et al. (1993) Risk factors for HIV infection among young adult men in Northern Thailand. JAMA 270: 955-960.
- Catania JA, Binson D, Dolcini MM, Stall R, Choi KH, et al. (1995) Risk factors for HIV and other sexually transmitted diseases and prevention practices among US heterosexual adults - changes from 1990 to 1992. Am J Public Health 85: 1492-1499.
- Celentano DD, Nelson KE, Suprasert S, Eiumtrakul S, Tulvatana S, et al. (1996) Risk factors for HIV-1 seroconversion among young men in northern Thailand. JAMA 275: 122-127.
- Page-Shafer K, Veugelers PJ, Moss AR, Strathdee S, Kaldor JM, et al. (1997) Sexual risk behavior and risk factors for HIV-1 seroconversion in homosexual men participating in the TricontinentalSeroconverter Study, 1982-1994. Am J Epidemiol 146: 531-542.
- Catania JA, Coates TJ, Stall R, Turner H, Peterson J, et al. (1992) Prevalence of AIDS-related risk factors and condom use in the United States. Science 258: 1101-1106.
- Weir SS, Roddy RE, Zekeng L, Ryan KA (1999) Association between condom use and HIV infection: a randomised study of self reported condom use measures. J Epidemiol Community Health 53: 417-422.
- Choopanya K, Vanichseni S, Des Jarlais DC, Plangsringarm K, Sonchai W, et al. (1991) Risk factors and HIV seropositivity among injecting drug users in Bangkok. AIDS 5: 1509-1513.
- Ruiz I, Hernandez-Aguado I, Rebagliato M, Avini MJ, Perez-Hoyos S, et al. (1996) Determinants of condom use among intravenous drug users in Spain. Eur J Public Health 6: 270-274.
- Duncan SC, Strycker LA, Duncan TE (1999) Exploring associations in developmental trends of adolescent substance use and risky sexual behavior in a high-risk population. J Behav Med 22: 21-34.
- Kelly JA, St Lawrence JS, Brasfield TL, Lemke A, Amidei T, et al. (1990) Psychological factors that predict AIDS high-risk versus AIDS precautionary behavior. J Consult ClinPsychol 58: 117-120.
- Perkins DO, Leserman J, Murphy C, Evans DL (1993) Psychosocial predictors of high-risk sexual behavior among HIV-negative homosexual men. AIDS EducPrev 5: 141-152.
- VanLandingham MJ, Suprasert S, Sittitrai W, Vaddhanaphuti C, Grandjean N (1993) Sexual activity among never-married men in northern Thailand. Demography 30: 297-313.
- Crisp BR, Barber JG, Ross MW, Wodak A, Gold J, et al. (1993) Injecting drug users and HIV/AIDS: risk behaviours and risk perception. Drug Alcohol Dpend33: 73-80.
- Tapert SF, Aarons GA, Sedlar GR, Brown SA (2001) Adolescent substance use and sexual risk-taking behavior. J Adolesc Health 28: 181-189.
- Lawrence JS, Scott CP (1996) Examination of the relationship between African American adolescents, condom use at sexual onset and later sexual behavior: implication for condom distribution program. AIDS EducPrev 8: 258-266.
- Gerrard M, Gibbons FX, Bushman BJ (1996) Relation between perceived vulnerability to HIV and precautionary sexual behavior.Psychol Bull 119: 390-409.
- Sweat MD, Nopkesorn T, Mastro TD, Sangkharomya S, MacQueen K, et al. (1995) AIDS awareness among a cohort of young Thai men: exposure to information, level of knowledge, and perception of risk. AIDS Care 7: 573-591.
- Strunin L, Hingson R (1993) Adolescents. In: AIDS and the heterosexual population. Sherr L Chur: Harwood Academic Publishers pp:125-137.
- Crosby R, DiClemente RJ, Wingood GM, Sionéan C, Harrington K, et al. (2001) Psychosocial correlates of adolescents' worry about STD versus HIV infection: similarities and differences. Sex Transm Dis 28: 208-213.
- Cohen MS (1998) Sexually transmitted diseases enhance HIV transmission: no longer a hypothesis. Lancet 351 Suppl 3: 5-7.
- Nopkesorn T, Mastro TD, Sangkharomya S, Sweat M, Singharaj P, et al. (1993) HIV-1 infection in young men in northern Thailand.AIDS 7: 1233-1239.
- Swaddiwudhipong W1, Nguntra P, Lerdlukanavonge P, Chaovakiratipong C, Koonchote S (1990) A survey of knowledge about AIDS and sexual behavior in sexually active men in Mae Sot, Tak, Thailand. Southeast Asian J Trop Med Public Health 21: 447-452.
- Ross MW, Kelaher M (1993) Knowledge, attitudes and behaviour in heterosexual men and women: the research evidence. In: AIDS and the heterosexual population. Sherr L Chur: Harwood Academic Publisherspp. 253-262.
- Celentano DD, Nelson KE, Suprasert S, Eiumtrakul S, Galai N, et al. (1995) Dynamics of risk behavior for HIV infection among young Thai men. J Acquir Immune DeficSyndr Hum Retrovirol 10: 477-483.
- Jemmott JB, Jemmott LS (2000) HIV risk reduction behavioral interventions with heterosexual adolescents. AIDS 14 Suppl 2: S40-52.
Citation: Saengdidtha B, Rangsin R, Kaoaiem H, Sathityudhakarn O (2016) Risk Factors for HIV Infection among Thai Young Men Aged 21-23 Years. Epidemiology (Sunnyvale) 6:248. DOI: 10.4172/2161-1165.1000248
Copyright: © 2016 Saengdidtha B, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 11757
- [From(publication date): 6-2016 - Jul 30, 2025]
- Breakdown by view type
- HTML page views: 10816
- PDF downloads: 941
