Research Article Open Access
Sensory Processing and Repetitive Behaviors in Clinical Assessment of Preschool Children with Autism Spectrum Disorder
Magda Di Renzo*, Federico Bianchi di Castelbianco, Elena Vanadia, Massimiliano Petrillo, Lidia Racinaro and Monica Rea
Institute of Ortofonologia (IdO), Via Salaria, 30-00198-Rome, Italy
- *Corresponding Author:
- Magda Di Renzo
Institute of Ortofonologia (IdO)
Via Salaria, 30-00198-Rome, Italy
Tel: 0039-068542038
E-mail: m.direnzo@ortofonologia.it
Received Date: Mar 30, 2017; Accepted Date: Apr 19, 2017; Published Date: Apr 27, 2017
Citation: Di Renzo M, Bianchi di Castelbianco F, Vanadia E, Petrillo M, Racinaro L, et al. (2017) Sensory Processing and Repetitive Behaviors in Clinical Assessment of Preschool Children with Autism Spectrum Disorder. J Child Adolesc Behav 5: 342. doi: 10.4172/2375-4494.1000342
Copyright: © 2017 Di Renzo M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Child and Adolescent Behavior
Abstract
Autism is a neurodevelopmental disorder characterized by impairments in social communication and presence of restricted and repetitive patterns of behavior and interests, including abnormal reactions to sensory stimuli. Atypical responses to sensory input are increasingly recognized as a common feature of ASDs. In addition to repetitive patterns of behavior, the inclusion of sensory aspects in the diagnosis of autism in the latest Diagnostic and Statistical Manual of Mental Disorders (DSM-5) is evidence of the prevalence of sensory dysfunctions in this population. There are several tools investigating these areas, mostly rating scales that, far from wishing to replace other methods, allow a better understanding of the alterations presents and help in defining clinical picture and individual trajectory so improving diagnosis and intervention. The purpose of this study was to investigate the relation between sensory and repetitive behavioral characteristics of a sample of 50 preschool children with ASD measured with the Short Sensory Profile and the Repetitive Behavior Scales-Revised. Results are consistent with previous researches describing the co-occurrence of repetitive behaviors and sensory response abnormalities in the ASD population. We found evidence to support that the most frequently dysfunctional sensory areas in ASD children regard tactile hypersensitivity, auditory filtering, hyporeactivity and low energy/weak; while among repetitive behaviors the most common are those stereotyped. Furthermore it emerged that direct assessment with ADOS-2, a gold standard test for ASDs, and indirect assessment with questionnaires converged on the same profiles, so suggesting the usefulness to hold together both ecological and structured observations.
Keywords
Sensory profile; Repetitive behavior; Clinical assessment; Autism spectrum disorder
Introduction
All informations we receive about the world are coming from our sensory system according to an input> process> output model. The sensory processing refers to the way the nervous system receives, interprets and responds to sensory input. This response is determined both by genetic and environmental variables. Dunn [1], starting from the interaction between the neurological threshold of perception of individual stimulus and the behavioral response, identified four basic patterns of responding to sensory events in everyday life. Their characteristics are summarized in his sensory processing model where the neurological threshold indicates the amount of stimulus necessary to the nervous system to react, while the self-regulating strategy indicates the way in which respond in relation to the threshold (Table 1).
| Behavioral Response Continuum | |||
|---|---|---|---|
| PASSIVE (responds in accordance with threshold) |
ACTIVE (responds to counteract the threshold) |
||
| Neurological Threshold Continuum | HIGH (habituation) |
Poor registration | Sensation seeking |
| LOW (sensitization) |
Sensitivity to stimuli | Sensation avoiding | |
Table 1: Relationship between behavioral responses and neurological threshold.
In sensory processing disorders, sensory informations are normally received by receptors, but the brain incorrectly processes them, thus determining hyper-sensitivity or hypo-sensitivity to common stimuli. The levels involved in the disorder are, therefore, the perception, the modulation, the integration and the organization of sensory stimuli [2].
A high incidence of sensory processing difficulties exists in children with ASD who have more sensory-related behavioral symptoms than typically developing controls. Atypical behavioral and physiologic responses to sensory stimuli are reported in various groups with clinical diagnoses, such as Fragile X Syndrome or Attention-Deficit Hyperactivity Disorder [3-5], but few studies compare sensory symptoms across clinical conditions. A better understanding of the similarities and differences in sensory functioning between clinical disorders would be crucial to differential diagnosis and could have a profound impact on treatment planning [6]. According to previous studies, a wide range of sensory disturbances were reported in children with ASD [7-10]. Evidence suggested the profile of atypical sensoryrelated behaviors in children with ASD was different than children with other developmental disorders [11,12]. Rogers, et al. [13], for example, using parent questionnaires, found that toddlers with autism had more deficits in tactile sensitivity, auditory filtering and taste/smell sensitivity, as measured by the Short Sensory Profile, than those with other developmental delays. A specific search of sensory selfstimulation could also be present, as reported by some parents who reported their children need to get under the mattress, roll up in blankets or squeeze into very tight places [14].
Crispiani [15] described a significant perceptual overload, whereby, situations characterized by an excess of visual stimuli (crowded places or with too much light), or auditory stimuli (noisy places or with unusual/unpleasant sounds) may give rise to intolerance so leading to anger and aggressive reactions. The same author also reported the presence of strong visual-spatial discriminative abilities: for example, the tendency to focus on the details enables the autistic person to show good perceptual abilities in space, as the memory of positions and shapes, the discrimination of images and forms, the ability to build puzzles etc. On the other hand this hyper-functioning area often goes to interfere with the central coherence, that is, with the ability to capture the general meaning and totality of the stimuli, by altering the experiences and memories of subjects who have this characteristic approach to reality.
Parents and professionals who treat people with ASD frequently reported abnormalities in their sensory profile. In fact, sensory deficits, along with communication and social difficulties, become highly pervasive in their lives. The difficulties of ASD people in entering the world could therefore be ascribed to hyper or hypostimulation of the various sensory systems (e.g., a weak sound heard with particular intensity or a touch experienced as a strong pressure).
Since the 70s, many researches revealed the presence of sensory disorders in 70-80% of people with autism [16-18]. A more recent study [19] about rating scales for assessment of sensory profiles [20] showed very high percentage (95%) of ASD preschool children with sensory processing disorders. Specifically, the most affected areas appeared to be: the tactile and taste/smell sensitivity, the auditory filtering and the sensory seeking [21]. Furthermore, several significant relationships were found between these impairments and social, emotional and behavioral function [10].
In the psychodynamic approach, Meltzer [22] described, in autistic children, the dismantling mechanism to highlight the lack of integration of the various sensory components which in most cases are intact. Developmental theories showed that the arrest takes place in sensory integration level, making it necessary to pay close attention at how the child structures his presence in the world without being able to use normal sensory integration mechanisms. This is why it is very important to note the different ways in which the child uses various sensory pathways. However, in the previously mentioned tools are examined not only the individual responses in the various sensory channels, but also the behaviors related to proprioception and emotional regulation, since the sensory and affective components are inseparable during development. It is necessary to consider the specificities of different behaviors in order to outline different clinical conditions in symptom’s structuring, especially taking into account that the correlation with age is not significant [23], and then the peculiarity of responses is in relation with the extent of the disease.
The sensory and repetitive behaviors often have a reverse trend in the sense that an increased ritualization expresses an evolution respect to the restricted use of sensory and this is also confirmed by a qualitative analysis that enables to restrict the most involved parts of the body (as for example, body rocking or objects swinging), and the intensity with which movements are performed.
In confirmation of the importance of the role played by the sensory aspects also in the diagnosis, the fifth edition of the DSM [24], among the criteria for ASD, includes atypical sensory behaviors, thus introducing the “hyper or hyporeactivity to sensory input or unusual interest in sensory aspects of environment” (such as apparent indifference to pain/heat/cold, adverse response to specific sounds or textures, excessive smelling or touching of objects, fascination with lights or spinning objects).
In clinical and research settings, then, to integrate the criterial observations required by DSM-5, the various atypical behaviors of children are investigated through questionnaires and tests in order to define a framework that is as representative as possible of sensory difficulties and repetitive behaviors.
Among the most commonly used tests there are the Sensory Profile [20,25] and the Repetitive Behavior Scale [26,27]. The Sensory Profile investigates typical answers in the search for sensory stimulation assuming what already theoretically shared by the scientific community, that is the lack in sensory integration process of the ASD subjects. Ayres [28] described the process of sensory integration as an organization of sensation for use, stating that integration of sensory information was necessary for a child to interact effectively with his world.
Recent research has shown that in autism spectrum disorders an increased sensory integration, often associated to a more functional and symbolic use of the object, is related to a positive evolution of the disorder, so constituting an important prognostic predictor. In restricted and repetitive interests, through difficulties in sharing imaginative play and social game, there could be an awareness of the relationship with each other, albeit with the rigidity that characterizes the mode of staying in relationship that is typical of the autistic child. Similarly, mannerisms do not necessarily preclude relational aspects and may be related to self-regulate and relieve bodily tensions. Unusual interests at segments of sensory experience of self and objects instead prevent the connection between sensory processing and emotions, hindering the awareness of a psychological and emotional relationship with the other [29].
Even the ADOS-2, considered one of the most trusted and recognized worldwide test in the autism assessment, has made a significant change as regards the restricted and repetitive behaviors, including in the final score also quantitative assessment of mannerisms, unusual sensory interests and stereotyped behaviors (previously excluded). The presence, in terms of frequency and intensity of such behaviors, is a key discriminant in the diagnostic classification in addition to being an indicator of the level of severity in autism spectrum disorders.
Measures
Short sensory profile (SSP)
The Short Sensory Profile [20] is a standardized parent questionnaire which measures children’s responses to sensory events in everyday life. It was developed as a screening instrument to identify children with sensory processing difficulties and associated behaviors. Caregivers complete the questionnaire by reporting how frequently their children respond in the way described by each of 38 items item through a 5 point Likert scale (a score of 1 is assigned to behaviors that “always” occur and a score of 5 is assigned to behaviors that “never” occur). The raw scores are used to produce composite scores for seven domains: Tactile Sensitivity, Taste/Smell Sensitivity, Movement Sensitivity, Under-Reactive/Seeks Sensation, Auditory Filtering, Low Energy/Weak muscles, and Visual/Auditory Sensitivity. The total SSP score ranges from 38 to 190, with cutoff points to define classification categories. These cutoff points are based on the normative values collected [1] from 1,200 typically developing children. The validity and reliability of the SSP have been reported in literature. Initial studies on the validity of the SSP demonstrated a discriminant validity of >95% in identifying children with and without sensory modulation difficulties.. The internal reliability for the SSP, calculated using Cronbach’s alpha, ranges from 0.70 to 0.90.. These findings provide support for the use of the SSP as a valid and reliable measure of sensory processing.
Repetitive behavior scale-revised (RBS-R)
The Repetitive Behavior Scale Revised [26,27] is a caregiver questionnaire that captures the breadth of repetitive behaviors in ASD children. It consists of 43 items, rated on a four-point Likert scale ranging from ‘behavior does not occur’ to ‘behavior occurs and is a severe problem’, where higher scores indicate frequent dysfunctional behaviors.
The items are grouped into 6 subscales, which are: (A) Stereotyped behaviors (defined as apparently purposeless movements or actions that are repeated in a similar manner); (B) Self-injurious behaviors (defined as movements or actions that cause or have the potential to cause redness, bruising, or other injury to the body, and that are repeated in a similar manner); (C) Compulsive behaviors (defined as behavior that is repeated and performed according to a rule or involves things being done just so); (D) Ritualistic behaviors (defined as performing activities of daily living in a similar manner); (E) Sameness behaviors (defined as the resistance to change, insisting that things stay the same); (F) Restricted behaviors (defined as limited range of focus, interest, or activity).
Autism diagnostic observation schedule, second edition (ADOS-2)
The Autism Diagnostic Observation Schedule - Second Edition [30,31] is a semi-structured, standardized assessment of communication, social interaction, play, and restricted and repetitive behaviors. It presents various activities that elicit behaviors directly related to a diagnosis of ASD. The ADOS-2 includes five modules, each requiring just 40 to 60 minutes to administer. The individual being evaluated is given only one module, selected on the basis of his or her expressive language level and chronological age:
Toddler Module: For children between 12 and 30 months of age who do not consistently use phrase speech. It provides ranges of concern reflecting the extent to which a child demonstrates behaviors associated with ASD
Module 1: For children 31 months and older who do not consistently use phrase speech
Module 2: For children of any age who use phrase speech but are not verbally fluent
Module 3: For verbally fluent children and young adolescents
Module 4: For verbally fluent older adolescents and adults
Each module engages the individual in a series of activities involving interactive stimulus materials.
With improved algorithms, the ADOS-2 demonstrates strong predictive validity. In Modules 1 to 4, algorithm scores are compared with cut-off scores to provide one of three classifications: autism, autism spectrum, and non-spectrum. Cut-off scores varies depending on the module used and then to the language level of the child.
The ADOS-2, in addition to providing an overall score, also measures the Social Affect domain (SA) and Restricted and Repetitive Behaviors (RRB). The SA includes the evaluation of aspects related to communication and reciprocal social interaction, while the RRB includes unusual sensory interests, mannerisms, repetitive behaviors and stereotyped-idiosyncratic use of words and/or vocalizations.
Leiter international performance scale – revised (Leiter-R)
The Leiter International Performance Scale – Revised [32] is an individually administered instrument designed to assess the cognitive functioning of children and adolescents ages 2 years, 0 months to 20 years, 11 months of age. The Leiter-R was specifically developed for children and adolescents with communications disorders, cognitive delays, hearing impairments, traumatic brain injury, attention-deficit disorder and certain types of learning disabilities as well as other populations (e.g., autism spectrum disorders) for which traditional intelligence tests may not be appropriate or valid. In fact, it is a completely non-verbal scale and consists of two batteries: the first is the Visualization and Reasoning Battery (VR) which includes ten subtests, measuring nonverbal cognitive visuospatial and reasoning skills then generating Brief IQ (ages 2–20), Full Scale IQ (ages 2–20) and Fluid Reasoning Index (ages 2–20); the second,, that is the Attention and Memory Battery (AM), which also consists of ten subtests that enhance the interpretation of the global nonverbal IQ score by providing valuable diagnostic indicators of speed and nonverbal memory. The two batteries can be administered together or separately. Both batteries include unique "growth" scores, which measure small, important improvement in the cognitive skills even of a child with significant cognitive disabilities. The Leiter-R also includes four social-emotional rating scales (Examiner, Parent, Self, and Teacher) that provide behavioral informations, so allowing a multidimensional observation of the examinee. The validity coefficient of the IQ score was calculated for each age group (alpha .92 to .93). The Leiter-R has good evidence of the validity of the studies on the analysis of content, with data from an extensive analysis and various studies relating to the construct. The IQ scores have a mean of 100 and a standard deviation of 15. The intellectual disability is indicated by a composite score that is two standard deviations or more below the average, so that a score of 70 constitutes the limit value.
Procedures
Children with autism spectrum disorder were recruited during the period from 2014 to 2016 at the Institute of Ortofonologia. The Institute works in agreement and accreditation with the National Health System for taking charge of ASD children and their families. The diagnosis of autism of the children involved in the research has been prepared by a group of experts (psychologists, child neuropsychiatrists, speech therapists) and confirmed by an assessment with ADOS-2, according to DSM-5 criteria [24]. Psychologists and child neuropsychiatrists took care of clinical assessment and psychodiagnosis; therapists, who have dealt with the therapy and home-intervention for at least three months, completed SSP and RBSR questionnaires. Parents, in the psychodiagnostic evaluation phase of the child (1 to 4 weeks after the first interview), were informed about the general characteristics of the disease and in particular of their child. When the child began the course of treatment, that is immediately after the diagnostic phase, parents were placed in a counseling program, which included, as needed, also group meetings with other parents or therapy sessions together with their child. This research meets APA’s ethical principles and guidelines. The aims and procedures of the study were explained to the parents of all the participating children and they freely expressed their written informed consent in accordance with the Declaration of Helsinki.
Objectives
The aims of this study were to identify a characteristic sensory profile of ASD children, and to verify the relation between repetitive behaviors and sensory profile. In addition, we was interested to explore the personal variables (age, ADOS-2 score, IQ, therapy duration) that were correlated with the sensory profile and with the repetitive behaviors of ASD children.
Sample
The sample consisted of 50 children, aged between 3 and 6.8 years. When they arrived at the Institute they have received a diagnosis of Autism Spectrum Disorder. At the time of this study, they attended a therapeutic process which provided six hours a week of individual or group rehabilitation activities and parental counseling sessions. Of these children, 12 had been included in therapy for less than one year; 28 children for less than 2 years and 10 children for less than 3 years. According to ADOS-2 scores, 38 children had severe scores and 12 mild scores. The group was composed of 13 females (26%) and 37 males (74%). The M/F ratio was about 3:1, in according with recent publications on autism that indicate a relationship male/female 3:1 [33]. Table 2 reported the descriptive characteristics of the sample. The present study excluded children with brain injuries, genetic or metabolic disorders, sensory disabilities and none of the children involved in this research took drugs.
| Mean | SD | Range | |
|---|---|---|---|
| Age (in years) | 4,66 | 1,05 | 3-6,8 |
| Therapy Time (in months) | 17,44 | 9,4 | 3-39 |
| ADOS-2 scores | 18,0 | 5,2 | 6-28 |
| AS scores | 14,5 | 4,1 | 5-20 |
| CRR scores | 3,6 | 1,9 | 0-8 |
| IQ scores | 67,5 | 20,7 | 36-109 |
| FR scores | 77,36 | 15,3 | 48-110 |
| SES (%) | |||
| low | 4 | ||
| average | 88 | / | / |
| high | 8 | ||
| Siblings (%) | |||
| yes | 54 | / | / |
| no | 46 |
Table 2: Description of sample’s characteristics (N=50).
Results
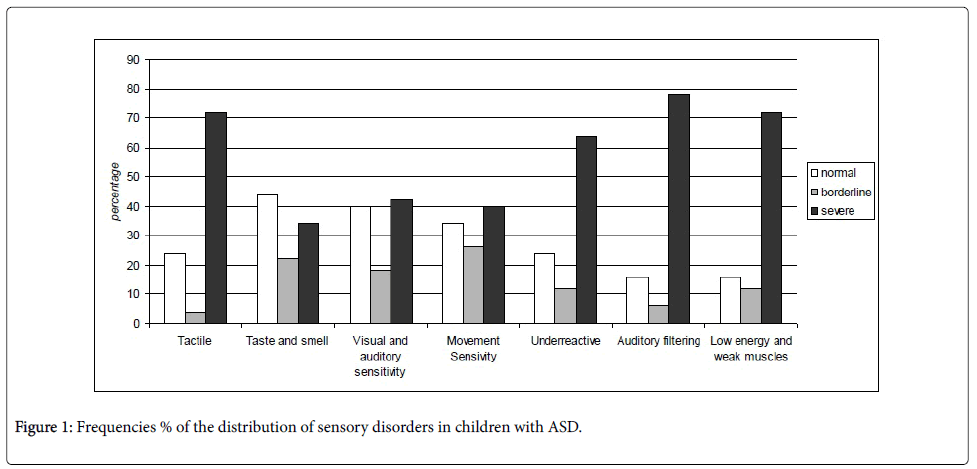
1) Children sensory profile (SSP)
As reported in Figure 1, descriptive analysis showed that in children with ASD the most prevalent sensory processing dysfunctions involved the underreactive/seeks sensation, auditory filtering, low energy/weak and tactile sensitivity domains, in accordance with what has already been demostrated by Watling, et al. [21].
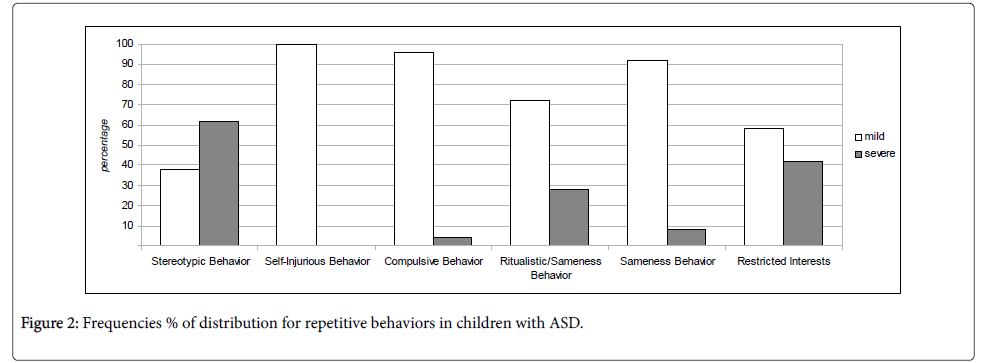
2) Repetitive behaviors (RBS-R)
The evaluation of repetitive behaviors, assessed with the RBS-R, it emerged that those stereotyped and restricted represented the most common behaviors in the majority of children with ASD (Figure 2).
3) Comparisons between sensory profile and repetitive behaviors in ASD children
As shown in the Table 3, statistical correlation analysis showed that children with severe scores in repetitive behaviors were also those who had more severe scores in the majority of the sensory areas as well as in ADOS-2 scores. We considered we considered significant correlations only with a Pearson-r value >0.65. Therefore, a high proportion of variance of tactile sensitivity (48%), of under-reactivity (55%) and of auditory filtering (58%) was explained by stereotypic behavior.
| Tactile | Taste and smell | Movement sensitivity | Under-reactive | Auditory filtering | Low energy and weak muscles | Visual and auditory sensitivity |
|---|---|---|---|---|---|---|
| -,696** | -,229 | -,424** | -,744** | -,760** | -,566** | -,544** |
| -,530** | -,397** | -,380** | -,534** | -,492** | -,238 | -,454** |
| -,293* | -,423** | -,096 | -,218 | -,168 | ,003 | -,076 |
| -,562** | -,059 | -,175 | -,343* | -,179 | -,194 | -,163 |
| -,426** | -,262 | -,184 | -,479** | -,407** | -,051 | -,422** |
| -,497** | -,268 | -,310* | -,781** | -,699** | -,335* | -,625** |
*p<0.01; **p<0.001
Table 3: Correlations between RBS-R and SSP scores.
Furthermore children with severe scores in restricted behaviors are also those who got severe scores on under-reactivity (61% explained variance) and on auditory filtering (49% explained variance)
4) Relationship between sensory profile, repetitive behaviors, personal variables and symptoms in ASD children
Chronological age and therapy duration: Statistical correlation analysis showed that there were no significant correlation between the RBS-R and SSP subscales, the chronological age of children and the therapy duration.
Autistic symptoms
Statistical correlation analysis showed that there were significant correlations between the RBS-R and SSP subscales, the ADOS-2 general scores and the scores of its SA (Social Affect) and RRB (Restricted and Repetitive Behaviors) subscales.
As shown in the following Table 4, children with high ADOS-2 total scores showed high scores (i.e., severe symptoms) in stereotyped (52% explained variance) and restricted behaviors (55% explained variance) and also low scores (i.e., severe symptoms) in almost all the sensory areas, particularly in under-reactivity (51% explained variance) and auditory filtering (59% explained variance). Moreover, children with high SA scores (i.e., severe symptoms) got high scores only in restricted and stereotyped behaviors, and also had low scores (i.e., severe symptoms) in almost all the sensory areas, except for the taste/ smell sensitivity.
| Stereotypic Behavior | Ritualistic/Sameness Behavior | Sameness Behavior | Self-Injurious Behavior | Compulsive Behavior | Restricted Interests | ||
|---|---|---|---|---|---|---|---|
| ADOS-2 total score | ,724** | -,046 | ,321* | ,179 | ,243 | ,741** | |
| SA subscale | ,558** | -,087 | ,273 | ,077 | ,138 | ,553** | |
| RRB subscale | ,795** | ,060 | ,299* | ,326* | ,371** | ,658** | |
| Tactile | Taste and smell | Movement sensitivity | Under-reactive | Auditory filtering | Low energy and weak muscles | Visual and auditory sensitivity | |
| ADOS-2 total score | -,434** | -,089 | -,419** | -,713** | -,769** | -,473** | -,665** |
| SA subscale | -,304* | -,068 | -,379** | -,598** | -,658** | -,459** | -,533** |
| RRB subscale | -,541** | -,100 | -,340* | -,683** | -,706** | -,319* | -,688** |
* p<0.01; ** p<0.001.
ADOS-2 Subscales: SA:Social Affection; RRB: Restricted and Repetitive Behavior
Table 4: Correlations between RBS-R, SSP and ADOS-2 in the ASD sample.
Finally, children with high RRB scores (i.e., severe symptoms) showed high scores in almost all evaluated repetitive behaviors: particularly in stereotyped behaviors (63% explained variance) and restricted behaviors (43% explained variance). In addition, they also had low scores (i.e., severe symptoms) in almost all the sensory areas, particularly in under-reactivity (47% explained variance), auditory filtering (50% explained variance) and Visual and auditory sensitivity (47% explained variance).
Intelligence quotient and fluid reasoning
Statistical correlation analysis showed that there were significant correlations between the RBS-R and SSP subscales, IQ and FR scores of the Leiter-R scale.
As shown in Table 5, although no correlation value was >0.65, children with high nonverbal IQ and FR scores got low scores in the stereotyped, compulsive and restricted behaviors and also have high scores in the tactile, under-responsive, auditory-filtering and visual/ auditory sensitivity domains.
| Stereotypic Behavior | Ritualistic/Sameness Behavior | Sameness Behavior | Self-Injurious Behavior | Compulsive Behavior | Restricted Interests | ||
|---|---|---|---|---|---|---|---|
| IQ | -,553** | -,086 | -,196 | -,232 | -,328* | -,547** | |
| FR | -,524** | -,162 | -,233 | -,336* | -,383** | -,496** | |
| Tactile | Taste and smell | Movement sensitivity | Under-reactive | Auditory filtering | Low energy and weak muscles | Visual and auditory sensitivity | |
| IQ | ,421** | ,100 | ,052 | ,584** | ,503** | ,075 | ,497** |
| FR | ,466** | ,041 | ,000 | ,570** | ,470** | ,054 | ,496** |
*p<0.01; **p<0.001.
IQ: Intelligence Quotient; FR: Fluid Reasoning
Table 5: Correlations between RBS-R, SSP, IQ/FR in ASD children of the sample.
Discussion
Findings from the SSP collected in the current study show a sensory profile that is common to more than 60% of children and that respond to some of the main features of the disorder such as tactile and auditory hypersensitivity, under-responsivity with low energy and sensation seeking. These sensory features translate into those behaviors so commonly observed in children with ASD such as: avoidance of physical contact, difficulties in carrying out activities of daily living related to personal care, low tolerance for some materials and clothing textures, avoidance or extreme reactions to noise; with respect to hyporeactivity, are also typical the lack of responses to name and commands in absence of hearing loss, the predilection for noisy activities (especially in the early years of life), the reduced perception of danger. The situation described is strongly limiting with respect to experiences and, dealing with a neurobiological component of altered perception/sensory integration, these considerations should always accompany the assessment and therapy of people with ASD. Primarily working on the body, on uni/multi-modal sense-perception and on emotion-related feelings/atypical reactions, as evidenced by another research conducted at the Institute [34], it is possible to change many of the dysfunctional behaviors.
The areas that in our research were less dysfunctional, or visualauditory, movement and taste/smell sensitivity, can be interpreted as follows: for what concerns the taste/smell and visual/auditory domains we believe that the combined observation of two sensory channels provided for the questionnaires in some ways reduced the sensitivity of the tool while maintaining the specificity of sensory dysfunction. In fact, many children, with or without ASD, showed high food selectivity, but only when the taste hypersensitivity was associated with the smell it resulted significantly dysfunctional at SSP; the same applied for auditory sensitivity, very frequently noted, that only when coupled with reactions of hyper-responsivity/avoidance of visual stimuli became meaningful. The movement sensitivity, often present in children with sensory processing disorders, did not seem to represent a significant area in the ASD.
Findings from the RBS-R demonstrated that restricted and repetitive behaviors certainly constitute a key feature of ASDs, in fact they are included in diagnostic algorithms of the ADOS-2 and in DSM-5. Our results maintain coherence between what clinically observed, what found with the ADOS and with the RBS-R. The age group we analyzed did not revealed self-injurious behaviors, even in children with lower nonverbal IQ and ADOS-2 scores; these are behaviors that, in clinical practice, more often belong to severe intellectual disabilities and organic syndromes. Ritualistic and compulsive behaviors, they too very rare in our sample regardless of ADOS-2 and nonverbal IQ scores, represent an uncommon element in infancy and childhood, and did not seem significant and/or specific in the sample considered. Furthermore, from the correlations between repetitive behaviors, sensory profile and nonverbal IQ, it could be assumed that the improvement of these areas indicates that the bodymediated therapy promotes the integration of mono-sensory perceptions so that the various segments of the sensory experiences can gradually evolve into emotional experience that activates a process of connecting emotions, sensory processing, motor planning and formation of symbols.
The correlation with the nonverbal IQ indicates that increased sensory integration and therefore greater cognitive potential reduces dysfunctional behaviors in ASD children. In this regard it would be interesting to reflect on behaviors that were not significant in the sample in relation to the therapeutic approach. Probably, a bodilymediated therapy improves movement sensitivity (not significant domain in our sample), promotes emotional regulation and consequently reduces self-injurious behaviors (they too not significant in the current sample) intended as a search for self-satisfaction of an aggressive charge that cannot be invested in the relationship. Given the centrality of these behaviors in the structuring of ASDs, it would be important to illustrate the trend in different therapeutic approaches in order to understand how much they can be attributed to the disorder or to the therapeutic intervention (both in a positive and negative sense).
Conclusion
Findings from this research provide clear support for the presence of sensory processing differences and repetitive behaviors in ASDs as well as for the utility of questionnaires completed by experienced professionals who know the child since at least three months. These tools, in clinical practice, help to better decline the various shades both in terms of difficulties and points of strength on which work during the therapeutic process. Of course, no questionnaire can replace clinical observation or structured testing as the ADOS-2, nor can be considered valid if compiled just by parents who are emotionally involved in the communicative and relational difficulties of their child.
Rather, parents’ evaluation has an important clinical significance if is considered as the result of the image they built by integrating their instinctive responses with the knowledge about the disorder. We noticed also that the reliability of the questionnaires completed by parents increases with the growth of the child, maybe because it gradually becomes possible to reach a greater awareness of the problems related to the disorder. In any case, in clinical setting, the questionnaires are particularly useful, both for parents and operators, to monitor the therapeutic efficacy. Especially professionals can be helped to modulate the intervention by identifying the zone of proximal development in the trajectory of sensory processing and expansion of the behavioral repertoire. In this view, parents can be stimulated to a greater awareness of the abilities achieved or difficulties overcome by the child.
We believe that an important result of this research is the identification of a variability in sensory areas in ASDs (not all areas are compromised, as we often find indicated in the literature), and then the possibility to promote changes through therapeutic intervention. It is therefore evident the need to accompany the initial evaluation with a specific observation of these areas also to allow any differential diagnosis.
The lack of attention to sensory domains during the assessment can neglect, in the therapeutic planning, the serious interferences created by stimuli the child could not receive and this can lead to misinterpretation. A child, for example, who is bothered by visual stimuli can respond with more dysfunctional behaviors, and this could increase the amount of responses difficult to manage in various contexts of the child's life. For repetitive behaviors too it is important to reflect on the fact that the lack of understanding of different correlations with sensory areas could induce the therapist to inhibit child’s behavior through pedagogic directives that risk themselves to become repetitive, monotonous and compulsive so leading to an exacerbation of symptoms. Also aggressive attitudes refer to some characteristics of the disorder but they often could be consequent to therapeutic modalities and / or too rigid educative instructions.
Moreover, the correlation found with the ADOS-2 and the Leiter-R, as well as the correlation between the RBS-R and the SSP, takes value because it emphasizes the importance of an assessment that combines together structured and ecological observations in order to achieve a more complete and respectful clinical picture of the child. Despite the recent recognition of both sensory symptoms and repetitive behaviors as specific aspects of ASDs, they have received less research attention than the social-communicative features of the disorder. But these aspects have a significant relationship with the overall adaptive behavior and impact on participation in daily life.
This is why the present contribute would encourage further study to better define pathology and also to open new frontiers in therapeutic approaches.
References
- Dunn W (1997) The Impact of Sensory Processing Abilities on the Daily Lives of Young Children and Their Families: A Conceptual Model. Infant Young Child 9: 23-35.
- Bundy AC, Lane SJ, Murray EA (2002) Sensory integration: Theory and practice. FA Davis.
- Dunn W, Bennett D (2002) Patterns of sensory processing in children with attention deficit hyperactivity disorder. OTJR: Occup Participation Health22: 4-15.
- Mangeot SD, Miller LJ, McIntosh DN, McGrath-Clarke J, Simon J, et al. (2001) Sensory modulation dysfunction in children with attention-deficit-hyperactivity disorder. Develop Med Child Neurol 43: 399-406.
- Miller LJ, Reisman JE, McIntosh DN, Simon J (2001) An ecological model of sensory modulation: performance of children with Fragile X syndrome, autistic disorder, attention-deficit/hyperactivity disorder, and sensory modulation dysfunction. In: Understanding the Nature of Sensory Integration With Diverse Populations, Roley SS, Blanche EI, Schaaf RC, editors. (San Antonio, Therapy Skill Builders) 57-88.
- Baranek GT, David FJ, Poe MD (2006) Sensory Experiences Questionnaire: discriminating sensory features in young children with autism, developmental delays, and typical development. J Child Psychol Psychiat 47: 591-601.
- Iarocci G, McDonald J (2006) Sensory integration and the perceptual experience of persons with autism. J Autism Develop Disord 36: 77-90
- Ben-Sasson A, Hen L, Fluss R (2009) A meta-analysis of sensory modulation symptoms in individuals with autism spectrum disorders. J Autism Develop Disord 39: 1-11.
- Kern JK, Trivedi MH, Garver CR (2006) The pattern of sensory abnormalities in autism. Autism 10:480-494.
- Baker AEZ, Lane A, Angley MT (2008) The relationship between sensory processing patterns and behavioral responsiveness in autistic disorder: a pilot study. J Autism Develop Disord 38: 867-875.
- Ermer J, Dunn W (1998) The sensory profile: a discriminate analysis of children with and without disabilities. Am J Occupational Ther 52: 283-290.
- Baranek GT, Boyd BA, Poe MD, David FJ, Watson LR (2007) Hyperresponsive sensory patterns in young children with autism, developmental delay, and typical development. Am J Mental Retard 112: 233-245.
- Rogers SJ, Hepburn S, Wehner E (2003) Parent reports of sensory symptoms in toddlers with autism and those with other developmental disorders. J Autism Develop Disord 33: 631-642.
- Grandin T (1995) How people with autism think. In: Learning and cognition in autism, Springer US 137-156.
- Crispiani P (2002) Lavorare con l’autismo [Working with Autism]. Junior, Bergamo.
- Ornitz EM, Guthrie D, Farley AH (1977) The early development of autistic children. J Autism Childhood Schizophrenia 7: 207-229.
- Ornitz EM, Guthrie D, Farley AJ (1978) The early symptoms of childhood autism. Cogn Defects Develop Mental Illness 24-42.
- Volkmar FR, Cohen DJ, Paul R (1986) An evaluation of DSM-III criteria for infantile autism. J Am Acad Child Psychiat 25: 190-197.
- Tomchek SD, Dunn W (2007) Sensory processing in children with and without autism: a comparative study using the short sensory profile. Am J Occup Ther61: 190-200.
- Dunn W (1999) Sensory Profile: Examiner’s manual. Psychological Corporation, San Antonio, TX.
- Watling RL, Deitz J, White O (2001) Comparison of sensory profile scores of young children with and without autism spectrum disorders. Am J Occ Ther 55: 416-423.
- Meltzer D (1975) Adhesive identification. Contemp Psychoanal 11: 289-310.
- Mirenda P, Smith IM, Vaillancourt T, Georgiades S, Duku E, et al. (2010) Validating the repetitive behavior scale-revised in young children with autism spectrum disorder. J Autism Develop Disord 40: 1521-153.
- American Psychiatric Association (2013) Diagnostic and statistical manual of mental disorders (DSM-5®). American Psychiatric Pub.
- Dunn W, Westman K (1997) The sensory profile: the performance of a national sample of children without disabilities. Am J Occup Ther 51: 25-34.
- Bodfish JW, Symons F, Lewis M (1999) The Repetitive Behavior Scale: Test manual. Western Carolina Center Research Reports, Morganton.
- Bodfish JW, Symons FJ, Parker DE, Lewis MH (2000) Varieties in repetitive behavior in autism. J Autism Develop Disord 30: 237-243
- Ayres AJ (1972) Sensory integration and learning disorders. Western Psychological Services, Los Angeles.
- Di Renzo M, Bianchi Di Castelbianco F, Petrillo M, Racinaro L, et al. (2016) The Emotional Contagion In: Children With Autism Spectrum Disorder. Austin J Autism Related Disabil 2: 1020-1027.
- Lord C, Rutter M, Di Lavore PC, Risi S, Gotham K, et al. (2012) Autism diagnostic observation schedule, second edition. Western Psychological Services, Torrance, CA.
- Colombi C, Tancredi R, Persico A, Faggioli R (2013) ADOS-2 – Autism Diagnostic Observation Schedule-Second Edition. Hogrefe, Florence.
- Roid GH, Miller LJ (2002) Leiter-R - Leiter International Performance Scale – Revised. O.S.Organizzazioni Speciali, Firenze.
- Nicholas JS, Charles JM, Carpenter LA, King LB, Jenner W, et al. (2008) Prevalence and characteristics of children with autism-spectrum disorders. Ann Epidemiol 18: 130-136.
- Di Renzo M, Bianchi di Castelbianco F, Vanadia E, Petrillo M, Racinaro L, et al. (2016) From the Emotional Integration to the Cognitive Construction: The Developmental Approach of Turtle Project in Children with Autism Spectrum Disorder. Autism-Open Access 6: 160-169.
Relevant Topics
- Adolescent Anxiety
- Adult Psychology
- Adult Sexual Behavior
- Anger Management
- Autism
- Behaviour
- Child Anxiety
- Child Health
- Child Mental Health
- Child Psychology
- Children Behavior
- Children Development
- Counselling
- Depression Disorders
- Digital Media Impact
- Eating disorder
- Mental Health Interventions
- Neuroscience
- Obeys Children
- Parental Care
- Risky Behavior
- Social-Emotional Learning (SEL)
- Societal Influence
- Trauma-Informed Care
Recommended Journals
Article Tools
Article Usage
- Total views: 9297
- [From(publication date):
specialissue-2017 - Aug 16, 2025] - Breakdown by view type
- HTML page views : 8109
- PDF downloads : 1188