Sex-Based Differences in Metabolic Equivalents (METs) After Cardiac Rehabilitation: A Systematic Review
Received: 30-Jun-2021 / Accepted Date: 14-Jul-2021 / Published Date: 21-Jul-2021 DOI: 10.4172/jcpr.1000143
Abstract
Purpose: The purpose of this systematic review is to investigate the differences in peak Metabolic Equivalents (METs) between men and women post myocardial infarction after participating in a Cardiac Rehabilitation (CR) program.
Methods: Four databases were systematically searched through August 2020. Search terms related to cardiac rehabilitation, treatment outcomes, and gender differences were used. Papers were considered relevant if they compared outcomes in cardiac rehabilitation between men and women. Information from the studies was extracted by two independent authors. Risk of bias was assessed using the Downs and Black instrument.
Results: A total of 12,786 records were identified from the search and 8 observational studies were included in the final review. Improvements in absolute METs during CR ranged from 1.1 to 2.0 for women and 0.8 to 2.5 for men. Seven studies reported a statistically significant increase in peak METs for both men and for women after outpatient CR. Three of these studies showed a greater increase in absolute METs in men compared to women that were statistically significant. Four studies showed no sex-based differences before and after. Several of these studies reported significant improvements in both men and women in other outcomes including cholesterol, blood glucose, and BMI.
Conclusion: Both men and women improve functional capacity from CR. The majority of studies reported that there were more men participating in CR programs than women. Given the underrepresentation of women in these studies, it is difficult to speculate if any differences in MET levels reported in these studies are a true representation of sex differences with respect to peak MET levels. Nonetheless, the statistically significant improvement in METs in both sexes suggests that women experience clinical benefit from CR and that efforts should be made for greater referral of women to CR programs.
Keywords: Sex; Cardiac Rehabilitation; Cardiovascular Disease; METs
Background
Worldwide, cardiovascular disease is the leading cause of morbidity for both women and men [1]. In the United States, over 720,000 people experience Myocardial Infarctions (MI) annually [2]. Cardiac Rehabilitation (CR), an evidenced-based multidisciplinary intervention that incorporates health behavior adjustment, patient education, biopsychosocial counseling, and exercise training, has become a standard of care following a MI [3-6]
An increasing body of research demonstrates the broad health outcome benefits of CR. A meta-analysis estimated a 21% to 34% reduction in mortality rate in older coronary patients who underwent CR [7]. Another study noted that CR coupled with medical management is more effective in improving health-related quality of life and reducing future hospitalizations when compared to medical management alone [6]. These benefits are consistent across different adult age groups [8]. Research demonstrates that CR, whether in an inpatient or outpatient setting, is more cost-effective than no CR [9].
While robust evidence favors the use of CR for the medical management of patients after an MI, a significant sex disparity exists for CR participation where women are at a significant disadvantage [10-13]. While this sex disparity is likely complex and multifactorial, differences in CR outcomes between men and women has not been explored in a systematic review. As exercise capacity has been shown to play a significant role in prognosis after an MI, we sought to synthesize the nature of possible differences in post-CR peak exercise capacities between women and men [14-17].
Literature Review
We performed a systematic review examining changes in peak exercise capacity as measured in Metabolic Equivalents (METs). This review was conducted using the criteria established by the PRISMA guidelines [18]. Search strategies were developed in conjunction with a research librarian to answer the following PICO question: In adults that have experienced ischemic heart disease, is there a difference in METs between men and women after phase II CR? Searches of PubMed, SCOPUS, CINAHL, and Cochrane Central Registry of Controlled Trials from inception through August 21, 2020 were performed. In order to maximize search results, we used MeSH headings and free-text terms that included sex, cardiac rehabilitation, cardiovascular disease, and treatment outcomes. Two authors screened titles and abstracts to identify potential articles. Full-text articles were then reviewed by two coauthors to determine eligibility. Co-authors also scanned reference lists of eligible articles and reviews. A third author was used to resolve any discrepancies.
Papers were included if they met the following criteria: (1) Men and women engaged in outpatient, phase II CR after ischemic heart disease (i.e. after sustaining an MI or angina); (2) utilized exercise testing to measure Metabolic Equivalents (METs) as an outcome of CR in both men and women; and (3) peer-review publication in the English language A single MET is defined as the metabolic cost of resting and is understood to be approximately equal to 3.5 ml of oxygen consumed per kilogram body weight. Since METs are measured in ml of oxygen consumed, it is a surrogate measure of the ability of the cardiorespiratory and metabolic systems to support physical activity. Quantifying peak exercise capacity using METs therefore describes the individual’s maximal level of cardiorespiratory and metabolic capacity in terms multiples of the resting metabolic rate [19-21].
We excluded review articles, other systematic reviews, dissertations, and articles that did not specifically look at phase II outpatient CR or did not report before and after differences in physiological treatment outcomes between men and women. Articles that did not measure METs directly and only estimated METs were excluded in order to minimize inflation of the values [22-24].
Quality assessment
Two authors independently assessed study quality using the Downs and Black criteria [25]. Consensus was reached for each item by discussion and a third reviewer was used when consensus was not reached. The Downs and Black scale was selected as it can be used to assess the quality of both observational and randomized clinical trials. We removed the item on power of the study, leaving a total of 26 items. Most items are scored either a 0 for no or 1 for yes if the item was present in the article; however, one item can receive 2 points, resulting in a maximum score of 27 points. The scores for the items were summed and divided by 27 to obtain the final score for each article.
Data extraction and analysis
For each study, two coauthors collected data using a standardized form. Data included answering if the study related to the PICO question, the study design, the population in the study, the cardiac rehabilitation intervention, any comparison intervention, the time points at which the outcomes were measured, and all primary outcome measures including METs. Results are reported as mean (SD) unless noted otherwise.
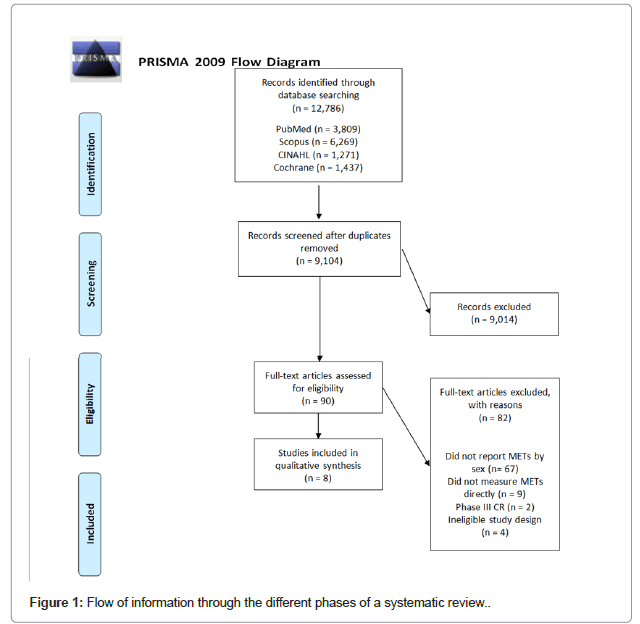
A total of 12,786 records were identified from the search and 8 eligible studies were included in the final review [10, 26-32] (Figure 1). The design of all 8 articles was observational in nature. Of the 8 studies included in the review, 7 directly compared differences in absolute METs between men and women before and after CR [10, 26- 31]. Three of these studies showed a greater increase in absolute METs in men compared to women that was statistically significant [10, 30, 31]. Four studies showed no sex-based differences before and after CR [26-29]. The study design, quality of the studies, characteristics of the subjects, and the duration of the cardiac rehabilitation interventions were comparable between the studies that did and did not demonstrate sex-based differences in METs after cardiac rehabilitation. One study reported changes in METs by sex after cardiac rehabilitation, but they did not directly compare for sex-based differences [32].
Study quality
The mean Downs & Black score of the 8 included studies was 13.75 out of 27 (sd 2.66) or 0.509. The range of the scores was from 10 to 17. Items that were frequently scored lower included those related to random assignment, the accessible population, blinding of participants and outcome assessors, and adverse effects of the interventions.
Participant and study characteristics
Sample sizes of the included studies ranged from 51 to 206 for women and 72 to 652 for men. The total number of subjects in the 8 studies was 3,564 (862 women and 2,702 men). All of the studies, except for Ghashghaei, et al. included more men than women [32].
Seven of the studies reported age by sex; in these studies, the mean age of women ranged from 50 to 63 years, while for men it ranged from 54 to 61 years. The other study provided a mean age of 54.5 years for the total sample, but did not report ages of male and female participants separately [10].
All articles provided descriptions of the CR interventions used. Supervised exercise sessions varied by study, but always included forms of aerobic exercise (i.e. walking on a treadmill) and often resistance exercise training. These exercise regimens were supplemented by other CR components focused on risk factor modification, including nutrition and dietary counselling, biopsychosocial counselling, and smoking cessation.
The total number of sessions for each CR program ranged from 24 to 36 sessions. The exercise sessions typically lasted 40 to 60 minutes; however, Sadeghi, et al. described exercise sessions lasting 60 to 90 minutes [31]. The duration of the programs ranged from 8 to 12 weeks.
Exercise capacity
Improvements in absolute METs during CR, as reported by 8 studies, ranged from 1.1 to 2.0 for women and 0.8 to 2.5 for men. Improvements in percent improvement in METs from baseline, as reported by 4 studies, ranged from 6.1% to 33% in women and 10.6% to 40% in men (Tables 1 and 2). Seven studies reported a statistically significant increase in peak METs for both men and for women after outpatient CR. O’Farrell, et al. was the only study in which a statistically significant improvement for either men or women was not reported after CR [29].
| Authors | Women | |||
| n | Baseline | Post-intervention | Change | |
| Anjo et al 2014 | 85 | 7.6 | 8.7 | 1.2 |
| Cannistra et al 1992 | 26 | 3.7 | 4.8 | 1.1 |
| Caulin-Glaser et al 2007 | 71 | 4.9 | 6.3 | 1.4 (20%) |
| Ghashghaei et al 2012 | 84 | 5.9 | 7.9 | 2 |
| Lavie et al 1995 | 83 | 6.1 | 8.1 | 2.0 (33% increase) |
| O’Farrell et al 2010 | 70 | 4.9 | 5.2 | (6.1% increase) |
| Sadeghi et al 2012 | 121 | 7 | 8.7 | 1.7 |
| Sarafzadegan et al 2007 | 147 | 6.9 | 8.7 | 2.0 (30% increase) |
| Authors | Men | |||
| n | Baseline | Post-intervention | Change | |
| Anjo et al 2014 | 301 | 9.1 | 10.6 | 1.5 |
| Cannistra et al 1992 | 107 | 5.1 | 5.9 | 0.8 |
| Caulin-Glaser et al 2007 | 224 | 6.7 | 8.6 | 1.9 (14%) |
| Ghashghaei et al 2012 | 72 | 8.4 | 10.9 | 2.5 |
| Lavie et al 1995 | 375 | 6.7 | 9.4 | 2.7 (40% increase) |
| O’Farrell et al 2010 | 317 | 6.6 | 7.3 | (10.6% increase) |
| Sadeghi et al 2012 | 464 | 9.4 | 11.9 | 2.5 |
| Sarafzadegan et al 2007 | 400 | 9.7 | 12.2 | 2.5 (21%) |
Table 1: Metabolic equivalents before and after cardiac rehabilitation for women and men.
| Authors | Type of Study | Quality Rating | Participants | Intervention | Outcomes |
|---|---|---|---|---|---|
| Anjo et al, 2014 | Retrospective | 13 (0.46) | 858 patients | Duration: 8-12 weeks | -METs |
| 206 women, 652 men | Sessions: 2x/week | -Metabolic Profile | |||
| 85 women and 301 men were analyzed | Length of session: 60 minutes | -Heart Rate (Resting, recovery, chronotropic index) | |||
| Mean Age | Exercise: Aerobic and strength training with weights | ||||
| Men 59 y with an SD of 10 | Consultations in psychiatry, urology, risk factor modification (i.e. smoking cessation and nutrition) depending on clinical indication | ||||
| Women 50 y with an SD of 10 | |||||
| Cannistra et al, 1992 | Prospective | 16 (0.57) | 225 total patients | Duration: 12 weeks | -METs |
| 51 women, 174 men | Sessions: 3x/week | -Exercise time in minutes | |||
| Mean age | -Heart Rate: Percent max heart rate, Peak rate-pressure product | ||||
| Total sample: 54.4 y (SD=9.9) | Length of sessions: 30 minutes (Participants exercised while maintaining a heart rate between 75% and 85% of their maximal heart rate during 30 minutes of exercise) | -Exercise induced ischemia | |||
| Women: 56 y (SD=10) | -Metabolic Profile | ||||
| Men: 54 y (SD=10) | |||||
| Race: White (84%) | |||||
| Caulin-Glaser et al, 2007 | Retrospective | 14 (0.50) | 348 patients | Duration: 12 weeks | -METs |
| 100 women, 248 men | Sessions: Frequency not reported | -BMI | |||
| Length of sessions: not reported | -Metabolic Profile | ||||
| Mean age | -Biopsychosocial (Depression) | ||||
| Completers 63.9 y (SD=10.6) | Components: Sessions included exercise training, education and extensive behavior modification therapy which included management of diet, cholesterol, blood pressure, stress, and glucose as well as smoking cessation) | ||||
| Non-completers 55.5 y (SD=13.3) | |||||
| Participants must have completed at least 7 weeks. | |||||
| Ghashghaei et al, 2012 | Prospective | 17 (0.61) | 156 total of obese patients | Duration: 2 months long (8 weeks) | -METS |
| 84 women, 72 men | Sessions: 24 sessions, 3x/week | -Weight (body weight, BMI) | |||
| Mean age | -Metabolic profile | ||||
| Women: 57.7 y | Length of Sessions: 90 minutes (10 minutes of warm-up, 60 minutes of aerobic/resistance training, 20 minutes of cooldown) | -Fasting blood sugar | |||
| Men: 54.5 y | |||||
| Components: Included exercise training sessions, nutritional and psychologic consultation, and risk factor management. Each patient had individual dietary instruction by a visiting dietitian during the program. | |||||
| Lavie et al, 1995 | Retrospective Cohort | 10 (0.36) | 458 total | Duration: 12 weeks | -METs |
| -83 women, 375 men | Sessions: 3x/week, total of 36 exercise and educational sessions | -Metabolic Profile | |||
| Mean age | Length of Session: 50-60 minutes (included a 10-minute warm up, 30-40 minutes of upright dynamic exercise, and a 10-min cool down) | -BioPsychosocial outcomes | |||
| Women: 63 y (SD=10) | Type of Exercise: Intensity individualized at 70-85% HRmax | ||||
| Men: 61 y (SD=10) | |||||
| O’Farrell et al, 2010 | Retrospective | 16 (0.57) | 387 total | Duration of program: Three-month program | -METs |
| -70 women, 317 men | Sessions: 2 exercise sessions per week | -Metabolic Risk Factors | |||
| Length of sessions: Exercise sessions included warm-up and 30 minutes of exercise at prescribed HR | -Physical Function (energy expenditure/week) | ||||
| Mean Age | Exercise: Consisted of walking, stationary cycling, rowing, biking | -Biopsychosocial (Mental Health) | |||
| - Men 59 y (SD=10) | Supplement: Varied by individual patient goals (i.e. stress management, smoking cessation, dietary); all had physician-guided risk factor management | ||||
| - Women 61 y (SD=10) | |||||
| Sadeghi et al, 2012 | Retrospective cohort | 14 (0.50) | 585 total patients | Duration: Two months | -METs |
| -121 women, 464 men | Sessions: 24 exercise training sessions | -Metabolic profile | |||
| Mean age | Frequency: 3 x/week | ||||
| Women 58.1 y (SD=8.95) | Length of Sessions: 90 minutes (20 minute warm up and 10 minute cool down, with 60 minutes of aerobic and resistance training between.) Training intensity was 60-85% of HR max. | ||||
| Men 56.2 y (SD=9.94) | Exercise: Using a treadmill, stationary cycles, stationary steppers, stair climbing, rowing, jogging, and some resistance devices. | ||||
| Mean BMI | Data collected from 2000 to 2011 | ||||
| Women 26.29 kg/m2 (SD=2.66) | |||||
| Men 25.45 kg/m2 (SD=2.47) | |||||
| Sarafzadegan et al, 2008 | Retrospective | 10 (0.36) | All patients had documented heart disease | Duration: 8 weeks | -METs |
| 547 patients | Sessions: 24 exercise sessions over 8 weeks | -Weight (BMI, Body weight) | |||
| 147 women, 400 men | Length of Sessions: 60-90 minutes each session | -Metabolic Profile | |||
| Mean Age | Exercise: Intensity of the exercise was calculated according to the determined risk, between 60 and 85% of the maximum HR achieved on the exercise test. | -HR | |||
| 147 women 57.3 y (SD=0.67) | Supplement: All patients received psychological, nutritional and smoking cessation consultations. There were also weekly educational sessions for patients and their families. | -Blood pressure (systolic) | |||
| 400 men 55.2 y (SD=0.47) | -Cardiac variables (LV EF) |
Table 2: Summary of characteristics of included studies.
Three studies showed a greater increase in absolute METs in men compared to women that was statistically significant [10, 30, 31]. Caulin-Glaser, et al., calculated a percentage change from baseline in METs that was relatively similar for both sexes (20% for men, 14% for women). Sarafzadegan, et al., an increase of 2.5 METs in men compared to 1.8 METs in women was noted, which represented a 30% increase from baseline in METs for women and a 21% increase in men [30]. Sadeghi et. al a 2.43 increase in METs in men compared to 1.74 in women [31].
Four studies that compared differences in METs before and after CR found no statistically significant difference between men and women. Two of these studies examined the change in METs as a percentage change from baseline. One, by Lavie et. al, noted a 33% increase from baseline in women and a 40% increase from baseline in men [28]. Cannistra, et al., noted a greater change in women compared to men in terms of METs, but this difference was not statistically significant (P=0.08) [27].
Ghashghaei, et al did not report a direct comparison between men and women [32]. However, this study described similar improvements in METs for both men and women (2.5 in men vs. 2.0 in women) [32].
Other outcomes
AAll studies included in this review reported outcomes in addition to METs. Seven reported outcomes related to lipid profile [10,26,28-32]. Other common outcomes reported included body mass index (BMI) (n=6), blood glucose levels (n=4), and various psychosocial incomes (i.e. depression, tobacco cessation) (n=4).
In the studies which compared lipid profiles, five showed a statistically significant improvement for both men and women before and after cardiac rehabilitation with no statistically significant difference between the two groups [26, 29-32]. Two of these studies, by Cannistra, et al. and Lavie, et al. showed no statistically significant change in total cholesterol in both men and women [27,28].
Six studies investigated BMI changes before and after CR. Three studies noted statistically significant decreases in BMI after CR [10,26,32]. When the changes in BMI between sexes were compared, they were not statistically significant. Sarrafzadegan, et al., noted statistically significant decreases in BMI in both men and women after CR; when these differences were compared, women had a statistically significant greater decrease in BMI compared to men [30]. In contrast, Lavie, et al. noted a statistically significant decrease in BMI in men but not women after CR; these differences were not directly compared [28]. Finally, O’Farrell, et al. noted no statistically significant differences in BMI in both men and women after CR [29].
Discussion
While studies have reported that women specifically benefit from cardiac rehabilitation programs, no systematic review has compared differences in CR outcomes between men and women [33,34]. In this systematic review, we analyzed 8 studies examining typical CR programs conducted in North America, Europe, and the Middle East that reported changes in peak METs in men and women who completed outpatient CR programs. Three of these studies reported statistically greater differences in peak absolute METs following CR completion between men and women, favoring men; four studies reported global improvements in peak METs for both sexes following CR completion, but noted no significant differences in peak MET improvements between men and women [10,26-31]. The other study included did not directly compare changes in METs before and after CR between men and women, though the improvement in METs in both sexes was relatively similar [32]. Strength of the current systematic review was the inclusion of articles which reported MET values as determined from exercise testing. In comparison, MET values as calculated from exercise workloads may be misleading [22,23].
Although our findings suggest that women sometimes experience a smaller magnitude of improvement in peak exercise capacity when compared to men, the majority of the studies in our analysis suggest that women still benefit from CR. While CR may be underutilized post myocardial infarction, it is particularly underutilized in women [8,12]. A recent meta-analysis indicated that women were significantly less likely than men to be referred to CR (39.6% vs. 49.4%, odds ratio 0.68, 95% confidence interval 0.62-0.74) [13].
Women are typically referred to CR only when they present with greater cardiovascular risk than men [26]. Even after referral, women tend to participate at lower rates than men [35,36]. They are also less likely to successfully complete CR programs compared to men [10].
Barriers to CR participation among women are diverse and complex. A recent systemic review identified non modifiable barriers, such as age and diagnosis, and difficult to modify barriers, such as financial constraints and level of education that may be more prevalent among women [37]. Ades, et al. noted that women were significantly more likely than men to encounter transportation problems (32% vs. 16%; P=.01) [38]. Other barriers such as low awareness of CR and lack/lower physician advisement and referral of women to CR are prevalent but modifiable [39]. Research demonstrates that both sets of barriers among women can be addressed with a variety of interventions [37]. Notwithstanding, additional research is still needed to better understand how to close this sex disparity in CR participation. These disparities in referral are compounded by research that suggests that women experience improvements in a wide variety of clinical outcomes [37, 40-42].
Based on these data and the relatively smaller sample sizes of women in the majority of studies, it is difficult to make any definitive conclusion that women or men benefit more from CR than the other in terms of improvements in exercise capacity. Regardless, it is important to note that 7 of the 8 studies in this review found a clinically and statistically significant improvement in exercise capacity in both men and women after CR, underscoring the benefits of CR participation for eligible candidates regardless of sex.
We specifically examined changes in peak METs as a key outcome after completing a CR program because peak exercise capacity has been linked to several important clinical outcomes. From a disability standpoint, both the peak level of exercise capacity and the level of physical activity that can be sustained for a given period of time will determine the types of physical activities one can participate in. According to the work compiled by Ainsworth, et al. the metabolic cost of engaging in general kitchen activities like cooking or washing dishes requires an absolute energy expenditure of approximately 3.3 METs [19-21]. A hypothetical person with a peak exercise capacity of 3.0 METs may find that they are unable to participate in such kitchen activities, and might be considered “disabled,” necessitating assistance from family members or aides to perform such activities. For this person, a seemingly small improvement of 1.0 MET from participating in a CR program would be enough to theoretically enable this person to now perform their own kitchen activities and no longer require the same level of external assistance. Viewed in this light, the seemingly small changes in peak MET levels reported by several of the authors reviewed in this paper may translate to meaningful differences in the participation of daily activities or other meaningful pursuits.
A possible reason why men showed greater improvements in peak METs in some of the studies we examined may be due to underrepresentation of women as men appear to have higher CR completion rates when referred [43,44]. Caulin-Glaser, et al. determined via logistic regression that women had a non-completion odds ratio of 2.52 (p=0.024) compared to men [10]. Factors, such as increased family responsibilities (on average) by women compared to men, may contribute to this disparity [27]. Women referred to CR programs may also start with an average greater baseline cardiovascular risk, an observation highlighted Anjo, et al. O’Farrell et al., and Sadeghi et al. [26, 29, 31]. This could limit the improvement women have in CR, resulting in selection bias that is reflected by poorer outcomes in METs.
The structure of CR programs may explain some of our findings as they appear to be better tailored towards men than women [40, 45]. Other research has suggested that CR programs with flexible, personalized treatment options may be “even more ideally suited for women than for men,” which may provide improved clinical outcomes [37].
Most of the studies included in the review except for one assessed the effect of CR on lipid profile. Five out of these seven studies showed a statistically significant improvement without any statistically significant difference between men and women after CR, suggesting that both experience clinical benefit in terms of risk factor modification due to CR [26, 29-32]. Anjo, et al. concluded that women benefitted from CRP and showed significant improvements in modification of cardiovascular risk factors and other prognostic indiactors, thus increasing the need for increased utilization in women [26]. Similarly, Sadeghi et al., who found a greater improvement in METs in men compared to women after CR, still noted the role that CR plays in improving lipid profile in both sexes [31]. Six studies additionally looked at BMI, with half of them noting statistically significant decreases in BMI after CR in both sexes with no differences between sexes when statistically compared.
Six studies additionally looked at BMI, with half of them noting statistically significant decreases in BMI after CR in both sexes with no differences between sexes when statistically compared [10, 26, 32]. Two of the other studies noted decreases in BMI in at least one sex [28, 30].
Ghashghaei et al., who included obese subjects for their CR intervention, concluded that CR, is an effective tool for modifying both BMI and lipid profiles [32]. Thus, in addition to improvements in metabolic profile, both men and women may experience a reduction in BMI, another clinical benefit of CR for both sexes.
Conclusion
The majority of studies confirm that more men participate in cardiac rehabilitation programs than women. Given the underrepresentation of women in these studies, it is difficult to speculate if any differences in peak MET levels reported in these studies are a true representation of sex differences with respect to peak MET levels. Nonetheless, the statistically significant improvement in METs in both sexes suggests that women experience clinical benefit from CR and that efforts should be made for greater referral of women to CR programs.
Limitations
The majority of the observational studies included were retrospective, which are of lower quality than prospective studies and more prone to selection bias. The studies may have also been prone to selection bias through the inclusion of more men than women. Finally, studies did not specify if they included cis-gendered, trans-gendered, or gender non-binary individuals.
Future Research
Researches with larger, ethnically diverse sample sizes of women are needed to further evaluate different responses to CR between men and women. Future systematic reviews examining other outcomes, such as long-term mortality, would be helpful in evaluating other possible sex- based responses to CR.
Acknowledgements
We would like to thank Tom Harrod of the Himmelfarb Library at GW SMHS for Assistance with the literature searches.
References
- World Health Organization (2014) Global status report on noncommunicable diseases.
- Virani SS, Alonso A, Aparicio HJ, Benjamin EJ, Bittencourt MS, et al. (2021)Heart disease and stroke statistics - 2021 update: A report from the american heart association. Circulation 143: e254-e743.
- Virani SS, Alonso A, Aparicio HJ, Benjamin EJ, Bittencourt MS, et al. (2021)Heart disease and stroke statistics - 2021 update: A report from the american heart association. Circulation 143: e254-e743.
- Balady GJ, Williams MA, Ades PA, Bittner V, Comoss P, et al. (2007) Core components of cardiac rehabilitation/secondary prevention programs: 2007 update: A scientific statement from the american heart association exercise, cardiac rehabilitation, and prevention committee, the council on clinical cardiology; the councils on cardiovascular nursing, epidemiology and prevention, and nutrition, physical activity, and metabolism; and the american association of cardiovascular and pulmonary rehabilitation. Circulation 115: 2675-2682.
- Leon AS, Franklin BA, Costa F, Balady GJ, Berra KA, et al. (2005) Cardiac rehabilitation and secondary prevention of coronary heart disease: An american heart association scientific statement from the council on clinical cardiology (subcommittee on exercise, cardiac rehabilitation, and prevention) and the council on nutrition, physical activity, and metabolism (subcommittee on physical activity), in collaboration with the american association of cardiovascular and pulmonary rehabilitation. Circulation 111: 369-376.
- Piepoli MF, Hoes AW, Agewall S, Albus C, Brotons C, et al. (2016) European guidelines on cardiovascular disease prevention in clinical practice: The sixth joint task force of the european society of cardiology and other societies on cardiovascular disease prevention in clinical practice (constituted by representatives of 10 societies and by invited experts) developed with the special contribution of the European Association for Cardiovascular Prevention & Rehabilitation (EACPR). Eur Heart J 37: 2315-2381.
- Anderson L, Taylor RS (2014) Cardiac rehabilitation for people with heart disease: An overview of Cochrane systematic reviews. Cochrane Database
- Suaya JA, Stason WB, Ades PA, Normand SLT, Shepard DS (2009) Cardiac rehabilitation and survival in older coronary patients. J Am Coll Cardiol 54: 25-33.
- Doll JA, Hellkamp A, Thomas L, Ho PM, Kontos MC, et al. (2015) Effectiveness of cardiac rehabilitation among older patients after acute myocardial infarction. Am Heart J 170: 855-864.
- Wong WP, Feng J, Pwee KH, Lim J (2012) A systematic review of economic evaluations of cardiac rehabilitation. BMC health Serv Res 12: 243.
- Caulinâ€Glaser T, Maciejewski PK, Snow R, LaLonde M, Mazure, C (2007) Depressive symptoms and sex affect completion rates and clinical outcomes in cardiac rehabilitation. Prev Cardiol 10: 15-21.
- Colella TJ, Gravely S, Marzolini S, Grace SL, Francis JA, et al. (2015) Sex bias in referral of women to outpatient cardiac rehabilitation? A meta-analysis. Eur J Prev Cardiol 22: 423-441.
- Pack QR, Priya A, Lagu T, Pekow PS, Berry R, et al. Cardiac Rehabilitation Utilization During an Acute Cardiac Hospitalization: A national sample. J Cardiopulm Rehabil Prev 39: 19-26.
- Samayoa L, Grace SL, Gravely S, Scott LB, Marzolini S, et al. (2014) Sex differences in cardiac rehabilitation enrollment: A meta-analysis. Can J Cardiol 30: 793-800.
- Brawner CA, Abdul-Nour K, Lewis B, Schairer JR, Mod SS, et al. (2016) Relationship between exercise workload during cardiac rehabilitation and outcomes in patients with coronary heart disease. Am J Cardiol 117: 1236- 1241.
- Gulati M, Pandey DK, Arnsdorf MF, Lauderdale DS, Thisted RA, et al. (2003) Exercise capacity and the risk of death in women: The St James women take heart project. Circulation 108: 1554-1559.
- Mora S, Redberg RF, Sharrett AR, Blumenthal RS (2005) Enhanced risk assessment in asymptomatic individuals with exercise testing and framingham risk scores. Circulation 112: 1566-1572.
- Keteyian SJ, Brawner CA, Savage PD, Ehrman JK, Schairer J, et al. (2008) Peak aerobic capacity predicts prognosis in patients with coronary heart disease. Am Heart J156: 292-300.
- Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. Ann Intern Med 151: 264-269.
- Ainsworth BE, Haskell WL, Leon AS, Jacobs Jr DR, Montoye HJ, et al. (1993) Compendium of physical activities: Classification of energy costs of human physical activities. Med Sci Sports Exerc 25: 71-80.
- Ainsworth BE, Haskell WL, Whitt MC, Irwin ML, Swartz AM, et al. (2000) Compendium of physical activities: An update of activity codes and MET intensities. Med Sci Sports Exerc 32: S498-S504.
- Ainsworth BE, Haskell WL, Herrmann SD, Meckes N, Bassett DR, et al. (2011) 2011 Compendium of physical activities: A second update of codes and MET values. Med Sci Sports Exerc 43: 1575-1581.
- Lavie CJ, Milani RV (2007) Metabolic Equivalent (MET) inflation--not the MET we used to know. J Cardiopulm Rehabil Prev 27: 149-50.
- nRoss R, Blair SN, Arena R, Church TS, Després JP, et al. (2016) Importance of assessing cardiorespiratory fitness in clinical practice: A case for fitness as a clinical vital sign: A scientific statement from the American Heart Association. Circulation. 134: e653-e699.
- Savage PD, Toth MJ, Ades PA (2007) A re-examination of the metabolic equivalent concept in individuals with coronary heart disease. J Cardiopulm Rehabil Prev 27: 143-148.
- Downs SH, Black N (1998) The feasibility of creating a checklist for the assessment of the methodological quality both of randomised and non- randomised studies of health care interventions. J Epidemiol Community Health 52: 377-384.
- Anjo D, Santos M, Rodrigues P, Brochado B, Sousa MJ, et al. (2014) The benefits of cardiac rehabilitation in coronary heart disease: A gender issue?. Rev Port Cardiol 33: 79-87.
- Cannistra LB, Balady GJ, O’Malley CJ, Weiner DA, Ryan TJ (1992) Comparison of the clinical profile and outcome of women and men in cardiac rehabilitation. Am J Cardiol 69: 1274- 1279.
- Lavie CJ, Milani RV (1995) Effects of cardiac rehabilitation and exercise training on exercise capacity, coronary risk factors, behavioral characteristics, and quality of life in women. Am J Cardiol 75: 340- 343.
- O’Farrell P, Murray J, Huston P, LeGrand C, Adamo K (2000) Sex differences in cardiac rehabilitation. Can J Cardiol 16: 319-325.
- Sarrafzadegan N, Rabiei K, Kabir A, Sadeghi M, Khosravi A, et al. (2008) Gender differences in risk factors and outcomes after cardiac rehabilitation. Acta Cardiol 63: 763-770.
- Sadeghi M, Ghashghaei FE, Rabiei K, Roohafza H, Afshar H (2012) Is there any difference between non-obese male and female in response to cardiac rehabilitation programs?. J Res Med Sci 17: 787.
- Ghashghaei FE, Sadeghi M, Rabiei K, Roohafza H, Sarrafzadegan N (2012) Gender differences in risk factors of obese patients after cardiac rehabilitation program. Iran J Nurs Midwifery Res 17: 381.
- Arthur HM, Gunn E, Thorpe KE, Ginis KM, Mataseje L, et al. (2008) Effect of aerobic vs combined aerobic-strength training on 1-year, post-cardiac rehabilitation outcomes in women after a cardiac event. J Rehabil Med 39: 730-735.
- Beckie TM, Beckstead JW, Kip K, Fletcher G (2013) Physiological and exercise capacity improvements in women completing cardiac rehabilitation. J Cardiopulm Rehabil Prev. 33: 16.
- Jackson L, Leclerc J, Erskine Y, Linden W (2005) Getting the most out of cardiac rehabilitation:A review of referral and adherence predictors. Heart 91: 10-14.
- Oosenbrug E, Marinho RP, Zhang J, et al. (2016) Sex differences in cardiac rehabilitation adherence: A meta-analysis. Can J Cardiol 32: 1316-1324.
- SupervÃa M, Medina-Inojosa JR, Yeung C, Lopez-Jimenez F, Squires RW, et al. (2017) Cardiac rehabilitation for women: A systematic review of barriers and solutions. Mayo Clin Proc 92: 565-577.
- Ades PA, Waldmann ML, Polk DM, Coflesky, JT (1992) Referral patterns and exercise response in the rehabilitation of female coronary patients aged ≥ 62 years. Am J Cardiol 69: 1422-1425.
- McCarthy MM, Dickson VV, Chyun D (2011) Barriers to cardiac rehabilitation in women with cardiovascular disease: an integrative review. J Cardiovasc Nurs 26: E1-E10.
- Beckie TM, Beckstead JW (2010) The effects of a cardiac rehabilitation program tailored for women on global quality of life: A randomized clinical trial. J. Women’s Health 19: 1977-1985.
- Daniels KM, Arena R, Lavie CJ, Forman DE (2012) Cardiac rehabilitation for women across the lifespan. Am J Cardiol 125: 937-e1.
- Mora S, Redberg RF, Cui Y, Whiteman MK, Flaws JA, et al. (2003) Ability of exercise testing to predict cardiovascular and all-cause death in asymptomatic women: A 20-year follow-up of the lipid research clinics prevalence study. Jama 290: 1600-1607.
- Halm M, Penque S, Doll N, Beahrs M (1999) Women and cardiac rehabilitation: Referral and compliance patterns. J Cardiovasc Nurs 13: 83- 92.
Citation: Duggal NA, Scalzitti DA, Watkins S, Hecht O , Johnson SJ, et al. (2021) Sex-Based Differences in Metabolic Equivalents (METs) After Cardiac Rehabilitation: A Systematic Review. J Card Pulm Rehabil 5: 143. DOI: 10.4172/jcpr.1000143
Copyright: © 2021 Duggal NA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Open Access Journals
Article Tools
Article Usage
- Total views: 5678
- [From(publication date): 0-2021 - Dec 09, 2025]
- Breakdown by view type
- HTML page views: 4762
- PDF downloads: 916