Short Communication Open Access
Alcohol, Depression and Genetic Disposition: The Chicken, the Egg and the Gene Syndrome
Scott Brand*Digital Marketing Inspirations for Youth & Families/Cove Center for Recovery
Visit for more related articles at International Journal of Emergency Mental Health and Human Resilience
Here’s a tough question that perhaps some psychology types may stay up late at night pondering. What comes first: depression or alcoholism? (Figure 1) Well, we finally may have some closure in this age-old debate, thanks to a recent study by the National Institute on Alcohol Abuse and Alcoholism (NIH).
Does depression lead to alcohol abuse?
Nearly one-third of people with major depression also have an alcohol problem, according to one major study conducted by the NIH. The report concluded that in many cases, depression precedes alcohol addiction.
Further research indicates that children, who are depressed, often resulting from a traumatic event such as divorce, abuse, or molestation, are more prone to develop alcohol problems once they reach adolescence. This phenomenon applies to teens as well. In an analysis from the Office of National Drug Control Policy Executive Office of the President: Teens that have had an episode of major depression are twice as likely as those who aren't depressed to start drinking alcohol.
The National Child Traumatic Stress Network conducted a survey of teens, which had experienced physical or sexual abuse/assault and found that they were three times more likely to report past or current substance abuse than those without a history of trauma (Figure 2). In surveys of adolescents receiving treatment for substance abuse, more than 70% of the patients had a history of trauma exposure.
According to the National Child Traumatic Stress Network report, depression usually happens before substance abuse. The study discovered that depression emanates from childhood. These incidents trigger depression, and when the child reaches adolescence or adulthood, he or she can easily find an escape from his or her feelings by using drugs or alcohol.
Now conversely, the study found that children who were not depressed during childhood are less likely to start abusing alcohol or drugs. But there is no hard and fast rule when it comes to teen drug and alcohol abuse.
Sometimes Alcohol Causes Depression
It is important to note that depression leading to alcoholism does not only emanate from childhood, but occurs at adulthood as well. There are innumerable cases where people were sailing through life without any traces of alcohol abuse and then derailed after a traumatic event.
In a recent article by “the fix,” which identifies its online publications as “the worlds leading website about addiction and recovery,” entitled: The Link between Alcohol and Depression, the news piece states that even as adults, depression can lead to alcoholism or addiction.
The fix cited Paul Williams, an original member of the legendary Motown group The Temptations as a prime example of someone who started drugs after depression later in life.
Things began to spiral out of control for him when The Temptations started having creative and financial problems with the Motown label during the late 1960s. According to founding member, Otis Williams, the gravity of the situation mounted for Paul, who replaced his daily glass of milk with booze to self-medicate and drown out his sorrows.
In just a few short years, Williams went from being the alcohol and drug free member of the Temptations to one of the most addicted. When the alcohol impaired Williams' on-stage performance, he was swiftly kicked out of the band, and that's when his drinking problem accelerated, he ultimately committed suicide.
When an adult, like Williams, who never had a history of addiction, is confronted with a catastrophic, life altering event; it is clear to see how easily he or she can fall into the drugs and/or alcohol trap. The reasoning for this sudden turn to an addictive behavior is simple - depression compromises one’s ability to deal with problems. Thus one’s fall back plan is to confront issues through self medication by drinking excessive amounts of alcohol.
There are other instances where depression does not trigger alcoholism. One such example could be a celebrity who reaches the highest pinnacle in his or her career - alcohol free - before succumbing to alcohol abuse. All it takes for a casual drinker is one toxic friend to influence his or her behavior. There does not have to be depression - just exposure to alcohol by hanging out with the wrong crowd.
The Physical Effect of Alcohol To Depres-Sion
According to several studies, alcohol abuse can set off depression because of the neurotoxic effects of alcohol exposure to one's brain. WebMD reports that heavy alcohol consumption may lead to prolonged periods of depression.
The term neurotoxic effect is a medical term that simply means - in layman terms - that alcohol affects the brain in the same way as depression. The parts of the brain that control anxiety, appetite and mood often affected in a depressed person are also influenced by alcohol.
There are several potential social and psychological explanations for the existing link between alcohol and depression. This includes stressful life experiences that can precipitate both depression and alcohol problems.
And Let��?s Not Rule Out The Comorbid Alcohol/Depression Genetic Disposition Theory
Another alternative as to what comes first – alcoholism or depression – does not even involve either an acquired addiction or mental health condition. There are many addiction and mental health experts that contend both alcoholism and affective disorder may stem from a common genetic predisposition or may develop as a completely separate illnesses.
So let’s delve into more of the specifics of this hypothesis. There have been scientists that have discovered that the genes which influence the amount of alcohol people drink may be distinct from those that affect the risk of alcoholism.
And there have been a significant number of studies that have tied genetic predisposition to alcoholism. They deduce that the genes involved in this disorder, combined with environmental factors, influence susceptibility to alcohol dependence and can play an integral part in a person becoming more vulnerable to Alcoholism.
The various genetic pathways affecting alcohol drinking behavior have been investigated by Dr. Boris Tabakoff and his team at the University of Colorado-Denver using both rats and humans (Tabakoff, 2008; 2009).
They compared genes involved in alcohol pathways in rats with human genes, using male study participants throughout the globe to recognize similar genetic causes across species. Alcohol intake among the subjects ran the gamut from abstinence to heavy use, and drinking patterns were recorded.
The researchers found that drinking behavior is linked to the “pleasure and reward” system in the brain. In the journal BMC Biology, they note that the outcomes highlight the significance of exploring at signaling pathways rather than single genes, and show cross-species commonalities in predisposition to alcohol consumption.
Dr. Tabakoff said, “We know that high levels of alcohol consumption can increase the risk of becoming alcohol dependent in those who have a genetic makeup that predisposes to dependence. This is a case of interaction between genes and the environment.”
The report concluded that: “The genetic factors that contribute to the full range of alcohol consumption versus alcohol dependence in humans are distinct.”
To add more fuel to the fire regarding alcoholism and genetic disposition, in 2008, experts from the National Institute on Alcohol Abuse and Alcoholism in Maryland, performed a review of the work done so far on genes and alcohol. Dr. Francesca Ducci and colleagues wrote, “Alcoholism is a chronic relapsing disorder with an enormous societal impact. Understanding the genetic basis of alcoholism is crucial to characterize individuals’ risk and to develop efficacious prevention and treatment strategies.”
They found that genetic factors account for 40 to 60 percent of the variation between people at risk of alcoholism. The genes involved in the vulnerability to alcoholism include both alcoholspecific genes and those that affect neuronal pathways to do with reward, behavioral control and resilience to stress.
Despite the preponderance of evidence leading to a linkage between genetic pre-disposition to alcoholism there some level of obscurity still exists. “The genetic determinants of alcoholism remain to be discovered.”
The experts conclude that, “Although the genetic bases of alcoholism remain largely unknown, there are reasons to think that more genes will be discovered in the future. Multiple and complementary approaches will be required to piece together the mosaic of causation.”
Let’s See if You Can Make Sense of These Possible Scenarios
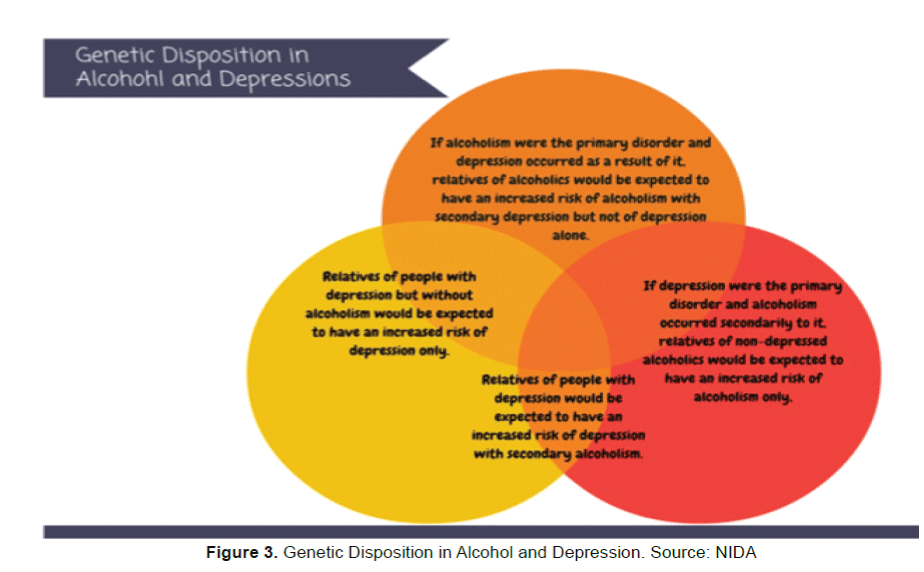
These different hypotheses about the relationship between alcoholism and affective disorders have different implications as the outcomes of each scenario (Figure 3).
Scenario 1 - If alcoholism were the primary disorder and depression occurred as a result of it, relatives of alcoholics would be expected to have an increased risk of alcoholism with secondary depression but not of depression alone.
Scenario 2 - Relatives of people with depression but without alcoholism would be expected to have an increased risk of depression only.
Scenario 3 - If depression were the primary disorder and alcoholism occurred secondarily to it, relatives of non-depressed alcoholics would be expected to have an increased risk of alcoholism only,
Scenario 4 - Relatives of people with depression would be expected to have an increased risk of depression with secondary alcoholism.
One Final Thought – What Should You Treat First? – Depression or Alcoholism
The correct question isn’t what you should treat first – depression or alcoholism- for those with co-existing disorders. A better question would be how you should treat dual diagnosis cases? The appropriate answer isn’t mutually exclusive but all of the above. People in recovery with co-existing disorders should receive various forms of treatment concomitantly including medication and psychotherapy.
There are many effective treatments for depression including interpersonal psychotherapy, cognitive behavioral therapy, supportive counseling and the administration of anti-depressant medications. There are also many effective treatments for addiction including behavioral therapies and counseling, and sometimes, the use of medications.
Perhaps, at this time there is no concrete answer to the question what occurs first depression or alcohol. In some instances a person may be depressed and use drugs and alcohol to escape their troubles. Other times, a person can become addicted and then lose control of everything and fall into a deep depression. And then there is some data to suggest there is a genetic component to alcoholism and/or depression.
About the Author
Scott Brand is the director of digital marketing for Inspirations for Youth, one the nation’s leading Teen Adolescent Addiction Treatment Centers as well as the Cove Center for Recovery, a premier adult drug and alcohol rehab. He spends part of his time performing clinical studies through the collaboration with the clientele and data mining.

Scott Brand during a television interview
References
- DualDiagnosis.org
- Ducci, F. & Goldman, D. (2008). Genetic approaches to addiction: genes and alcohol. Addiction, 103, 1414-1428.
-
National Institute on Alcohol Abuse and Alcoholism (NIH)
National Institute on Alcohol Abuse and Alcoholism in Maryland
Office of National Drug Control Policy Executive Office of the President - Tabakoff, B. et al. (2008). The genomic determinants of alcohol preference in mice.Mammalian Genome, 19, 352-365.
- Tabakoff, B. et al. (2009).Genetical genomic determinants of alcohol consumption in rats and humans.BMC Biology, 7, 70. The National Child Traumatic Stress Network, National Institute of Drug Addiction (NIDA) WebMD
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 17622
- [From(publication date):
March-2015 - Aug 17, 2025] - Breakdown by view type
- HTML page views : 12959
- PDF downloads : 4663