Case Report Open Access
An Insight to Occult Caries- An Overview with a Novel Approach in the Management
Poornima P1*, Dhanya S. Kumar3, Ashwini2, Nagaveni NB11Pediatric and Preventive Dentistry, College of Dental Sciences, Davangere, India
2Dept of Oral Pathology, College of Dental Sciences, Davangere, India
3College of Dental sciences, Davangere, India
- *Corresponding Author:
- Dr. Poornima P, MDS
Professor and Head of department
Pediatric and Preventive dentistry
College of Dental Sciences, Davangere, India
Tel: +91-8105482841
E-mail: drpoornimas2@gmail.com
Received Date: May 28, 2015 Accepted Date: July 04, 2015 Published Date: July 11, 2015
Citation: Poornima P, Dhanya SK, Ashwini, Nagaveni NB (2015) An Insight to Occult Caries- An Overview with a Novel Approach in the Management . J Oral Hyg Health 3:180. doi:10.4172/2332-0702.1000180
Copyright: © 2015 Dr. Poornima P et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits
unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Oral Hygiene & Health
Abstract
Dental caries appears to be the most prevalent infectious disease in the world. Occult caries/ hidden carious lesions are very challenging for detection as far as dentists are concerned. However, the nature of these lesions, their etiologies and the reasons of why they have eluded early, clinical diagnosis are still unclear. Till date only a very few microbiological studies have been conducted to obtain an insight into the bacteriological profile of these lesions which can also be an etiological factor. The aim of this case report is to present one such case of occult caries which also includes a microbiologic analysis of the lesion. It also includes a novel approach using revascularization for the management of the affected immature tooth.
Keywords
Etiology; Microbiological study; Occult caries; Revascularization
Introduction
In day to day practice very rarely dentist comes across apparently intact, recently erupted tooth which has become abscessed without any history of discomfort or pain. The term occult caries is usually used to refer such lesions. Occult caries is defined as the occlusal caries which cannot be diagnosed clinically because the occlusal surface appears to be ostensibly intact and shows radiolucencies in dentin. The various synonyms are ‘hidden caries’, ‘fluoride bombs’, and ‘fluoride syndrome ’and ‘pre eruptive caries’. The term ‘hidden caries’ or ‘occult caries’ denote those lesions that cannot be detected by clinical examination alone. The terms ‘fluoride bombs’ or ‘fluoride syndrome’ proposes that fluoride is an etiological factor [1,2]. In some teeth, these lesions have been discovered on routine radiographs before their eruption into the oral cavity and these are often erroneously referred to as ‘pre-eruptive caries’, as the tooth when it is completely encased within the crypt is not likely to be infected with cariogenicmicroorganisms. Recently the term ‘Pre-eruptive Intracoronal Resorption’ (PEIR) is used to describe such lesions [2].
Till date only a very few microbiological studies has been conducted to obtain an insight into the bacteriological profile of these lesions which can also be an etiological factor. The aim of this case report is to present one such case of occult caries which also includes a microbiologic analysis of the lesion with a novel approach to the treatment.
Case Report
A 12 year old girl presented to the Department of Pedodontics and Preventive Dentistry, with a chief complaint of pain in the lower right back tooth region since 15 days. She gave a history of pain which was spontaneous, moderate in intensity and of continuous type which aggravated on having food. Her medical history and past dental history were non-contributory. Extra oral examination revealed apparently symmetrical face with no tender lymph nodes.
On intra oral examination, the mandibular right second premolar (45) was tender on percussion with an intact occlusal surface (Figure 1a). There was also the presence of initial buccal pit caries with 36 and 46. An intraoral periapical radiograph with 45 region showed coronal radiolucency centering near the pulp horn of 45, with an intact occlusal enamel. Also widening of periodontal ligamentspace was noted. Radiograph also revealed incompletely formed roots with 45 and an open apex (Figure 1b). The tooth did not respond to cold or electric pulp test. With clinical and radiographic evaluation, the case was diagnosed as Occult caries with acute apical periodontitis in relation to 45.
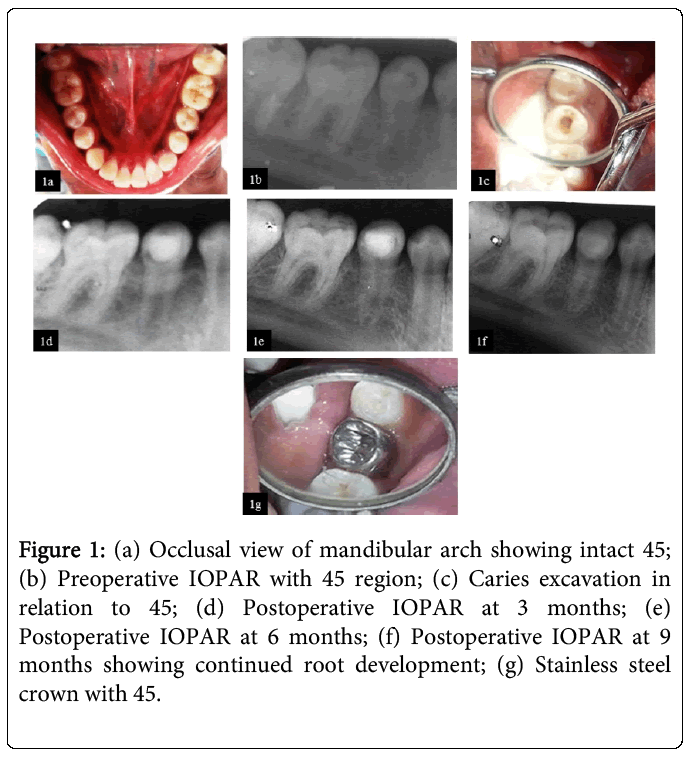
Figure 1: (a) Occlusal view of mandibular arch showing intact 45; (b) Preoperative IOPAR with 45 region; (c) Caries excavation in relation to 45; (d) Postoperative IOPAR at 3 months; (e) Postoperative IOPAR at 6 months; (f) Postoperative IOPAR at 9 months showing continued root development; (g) Stainless steel crown with 45.
Sterile conditions were followed for the entire procedure. Carious lesion when accessed with a sterile round bur, a resorbed empty cavity was observed (Figure 1c). A specimen was obtained from the resorbed area with spoon excavator and was sent for microbiological examination. Access opening when performed; revealed necrotic tissue in the coronal 2/3rd of the canal and a vital pulp tissue in apical portion. This specimen was also sent for microbiologicalexamination. Irrigation with saline was done followed by the placement of Ca(OH)2 mixed with sterile water (3:1 ratio) dressing as a medicament and temporary restoration was done with IRM.
After a week, the tooth was asymptomatic so revascularization with Ca(OH)2 was done. Temporary restoration was removed and the canal was gently irrigated with saline. Taking utmost care of asepsis, bleeding was induced into the canal and was stopped 3mm below the canal orifice. Ca(OH)2 was placed over the arrested bleeding and coronal access was sealed with glass ionomer cement. Reentry and change of calcium hydroxide dressings were not done at the subsequent visits as the coronal restoration was intact and the tooth was asymptomatic. After 1 month follow up, vitality test showed negative response. The 3rd and 6th month follow up showed that the tooth was asymptomatic and there was continued physiologic root development but was negative for both cold and electric pulp test. The 9th month follow up showed delayed response to the vitality test. (Figure 1d), (Figure 1e), (Figure 1f). Tooth was then restored with stainless steel crown and the patient is now under observation (Figure 1g).
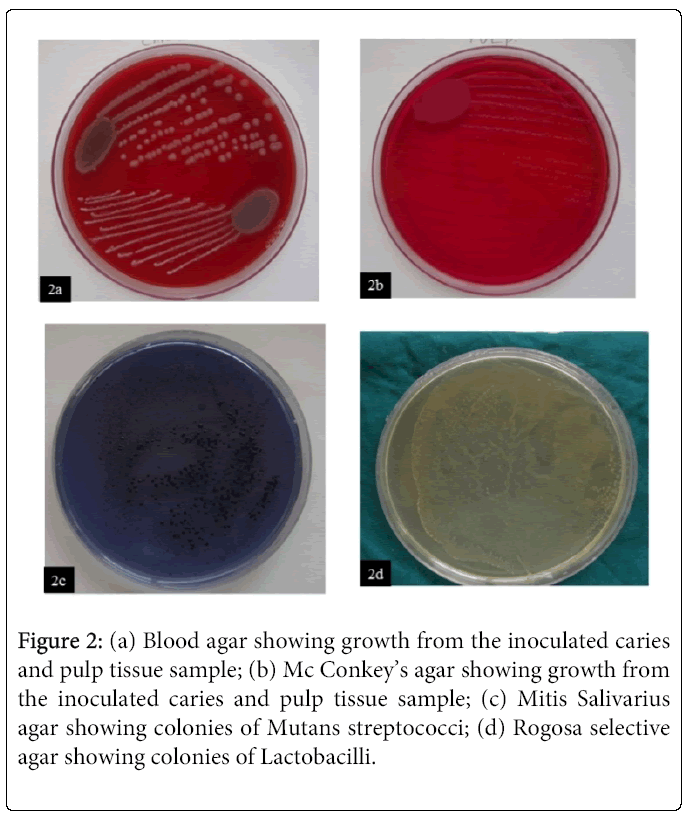
The specimens obtained from the dentin defect and the pulp tissue sample was cultured separately in blood agar (Figure 2a) and Mc Conkey’s agar (Figure 2b). This is followed by the use of selective media Mitis Salivarius agar (MSB) (Figure 2c) and Rogosa Selective Lactobacillus agar (Figure 2d). Microbiologic study showed colonies of Mutans streptococci and Lactobacilli from the dentin defect, whereas the pulp tissue showed the presence of colonies of both Mutans streptococci and Staphylococci.
Figure 2: (a) Blood agar showing growth from the inoculated caries and pulp tissue sample; (b) Mc Conkey’s agar showing growth from the inoculated caries and pulp tissue sample; (c) Mitis Salivarius agar showing colonies of Mutans streptococci; (d) Rogosa selective agar showing colonies of Lactobacilli.
Discussion
The most commonly affected teeth by occult caries are second, third molars and premolars as these teeth are in their pre-eruptive stages when the child normally presents for radiographs. Previous studies have concluded that tooth prevalence is 1-2% and subject prevalence is 2-6% [1].
There are several possible etiologic factors that lead to occult caries. Possibly, all the factors may be correct and a combination of these factors is supposed to be the exact etiology for this condition. In previously conducted studies, it was found that cavitation of the dentine starts only after crown development is complete. Thus, it can be concluded that cavitation is not the result of disturbance of mineralization, but most likely to be due to resorption of dentine [3,4]. Histological examination of affected teeth shows signs of resorption such as osteoclasts and scalloping of the dentine margins, which proves the etiology. However, the origin of the resorption cells is still unclear. It is speculated that the cells arise from undifferentiated cells of the developing dental follicle or from the surrounding bone. They are most likely to enter the dentine through a break in the enamel surface, such as hypoplastic pits or surface cracks or lamellae [5].
Previous studies conducted on the effect of fluoridation and prevalence of hidden lesions concluded that these lesions were less common in fluoridated areas. These findings refute the use of the term ‘fluoride bomb’ to describe these lesions [1]. Infection of the primary tooth has been suggested as another possible factor but is unlikely as many affected permanent teeth do not have primary predecessors. Ectopic eruption can also be an etiologic agent [2]. The local pressure due to ectopic eruption is found to cause damage to the reduced enamel epithelium (REE) at the base of developing fissure, from which resorption could have progressed. Resorptive area is soon invaded by the vascular connective tissue through the defect. But once the tooth erupts into oral cavity, communication with REE is lost which results in loss of vascular supply to the resorbing tissue, which causes the necrosis. The yellowish, `soft material found in the coronal defect of such a lesion is probably the necrotic connective tissue [6].
Till date only very few bacteriological studies on occult caries have been conducted and it has been concluded that less complex microbes were associated with hidden cariouslesionswhen compared to bacterial flora of normal carious lesion suggesting different etiologies for these conditions [7-9]. These lesions are free of microorganisms in the pre-eruptive period but as the tooth erupts, microorganisms ingress into the resorbed cavity and results in large carious breakdown [1]. The present study showed that along with Mutans streptococci and Lactobacilli, few staphylococcal species were also cultured from the samples. Similarly, studies have confirmed the presence of Mutans streptococci in the root canals and the presence of staphylococci in pulp abscess [3].
Bitewing radiographs are efficiently used in detecting such lesions. Whereas other diagnostic aids like panoramic radiographs, are also useful in screening the unerupted teeth [10].
Management depends on the size of the lesion and projected time of tooth eruption. In case of smaller lesions, when teeth are in their eruptive stages it is better to wait and watch after tooth eruption. In case of large lesions when teeth are not yet erupted, surgically exposing the tooth is considered to curette and to restore the lesion [10].
Prognosis depends upon
a) The size of the lesion
b) Pulpal involvement
c) Extent of root development.
In case of a large lesion with pulpal involvement and open apex, extensive endodontic therapyis required to save the tooth but the prognosis is poor. Smaller lesions are managed by restorations alone, where prognosis is found to be good. Also recurrence after treatment is not yet reported [1].
But with the invention of Regenerative Endodontics and newer biocompatible materials, we can expect good prognosis as seen with our case. Revascularization is the procedure to reestablish the vitality in a non-vital tooth to allow repair and regeneration of tissues. The rationale of revascularization is that if a sterile tissue matrix is provided in which new cells can grow, pulp vitality can be reestablished [11]. In our case, Calcium hydroxide was used for the revascularization procedure. According to the previous studies, the typical revascularisation protocol advocates placing antimicrobial agents ( metronidazole, ciprofloxacin , minocycline, or metronidazole, ciprofloxacin or cefeclor or metronidazole with ciprofloxacin [12] or calcium hydroxide [13,14]) for canal disinfection followed by a coronal seal with MTA. The problems seen with triple antibiotic paste arecrown discoloration, resistant strains and allergic reactions[12]. Considering these disadvantages, calcium hydroxide may be a promising alternative for intracanal medication because of its antimicrobial properties, the unlikelihood of crown discoloration , the possible release of growth factors and biomolecules from dentin and the vailability of this medication in routine clinical practice [12,15,16]. But it is speculated that calcium hydroxide would cause necrosis of the tissue with which it is in immediate contact with [17]. Also long term dressing might increase the risk of root fracture [18]. In our present case report, we considered that the cytotoxic effect was negligible as it was placed only in the coronal part of the canal. Concerning leakage of MTA used as a coronal plug material, two bacterial leakage investigations comparing MTA and Fuji Glass Ionomer cement showed no difference between the two types of materials in regard to bacterial penetration [19,20]. Hence taking into account all these factors and cost effectiveness and availability in Indian market, GIC was used to create the coronal seal in the present case. In our case, normal physiologic root development was noticed and root development was completed by 9 months, also the tooth showed a delayed response to vitality test. Thus Calcium Hydroxide could be considered in revascularizationprocedures when cost is the factor but needs further research in its usage.
Conclusion
The accurate diagnosis of the presence or absence of disease is paramount for appropriate care. Early diagnosis of lesion presence, activity and size would significantly improve caries management decisions with respect to operative intervention or preventive care.
References
- Page J (1986) The ‘fluoride syndrome’: occult caries? Br Dent J 160: 228.
- Counihan KP and O'Connell AC (2012) Case report: pre-eruptive intra-coronal radiolucencies revisited. Eur Arch Paediatr Dent. 13: 221-226.
- da Silva LA, Nelson-Filho P, Faria G, de Souza-Gugelmin MC, Ito IY (2006) Bacterial profile in primary teeth with necrotic pulp and periapical lesions. Braz Dent J. 17: 144-148.
- Seow W.K, Hackley D (1996) Pre eruptive resorption of dentin in primary and permanent dentitions. Case reports and literature review Pediatr dent 18: 67-71.
- Walker BN, Makinson OF, Peters MC (1998) Enamel cracks. The role of enamel lamellae in caries initiation. Aust Dent J. 43: 110-116.
- Blackwood HJJ (1958) Resorption of enamel and dentin in the unerupted tooth. Oral surg oral med oralpathol 11: 79-85.
- Loeshe WJ (1986) Role of Streptococcus Mutans in human dental decay. Microbiol Rev 50:353-380.
- Weerheijm L, de Soet J, de Graff J (1990) Occlusal hidden caries: A bacteriological profile. ASDC J Dent Child 57: 428-32.
- de Soet JJ, Weerheijm KL, van Amerongen WE, de Graaff J (1995) A comparison of the microbial flora in carious dentine of clinically detectable and undetectable occlusal lesions. Caries Res. 29: 46-49.
- O’Neal KM, Gound TG, Cohen DM (1997) Pre-eruptive idiopathic coronal resorption: a case report. J Endod 23: 58-59.
- Shah N, Logani A, Bhaskar U, Aggarwal V (2008) Efficacy of revascularization to induce apexification/apexogensis in infected, nonvital, immature teeth: a pilot clinical study. J Endod 34: 919-925.
- Iwaya S, Ikawa M, Kubota M (2011) Revascularization of an immature permanent tooth with periradicular abscess after luxation. Dent Traumatol 27: 55-58.
- Lana PE, Scelza MF, Silva LE, et al. (2009) Antimicrobial activity of calcium hydroxide pastes on Enterococcus faecalis cultivated in root canal systems. Braz Dent J 20: 32-63.
- Chueh LH, Ho YC, Kuo TC, et al. (2009) Regenerative endodontic treatment for necrotic immature permanent teeth. J Endod 35: 160-164.
- Behnen MJ, West LA, Liewehr FR, et al. (2001) Antimicrobial activity of several calcium hydroxide preparations in root canal dentin. J Endod 27: 765-767.
- Graham L, Cooper PR, Cassidy N, et al. (2006) The effect of calcium hydroxide on solubilisation of bio-active dentine matrix components. Biomaterials 27: 2865-2873.
- Banchs F, Trope M. (2004) Revascularization of immature permanent teeth with apical periodontitis: new treatment protocol? J Endod 30: 196-200.
- Andreasen JO, Farik B, Munksgaard EC (2002) Long-term calcium hydroxide as a root canal dressing may increase risk of root fracture. Dent Traumatol 18: 134-137.
- Tselnik M, Baumgartner JC, Marshall JG (2004) Bacterial leakage with mineral trioxide aggregate or a resin-modified glass ionomer used as a coronal barrier. J Endod 30: 782-784.
- John AD, Webb TD, Imamura G, Goodell GG (2008) Fluid flow evaluation of Fuji Triage and gray and white ProRoot mineral trioxide aggregate intraorifice barriers. J Endod 34: 830-832.
Relevant Topics
- Advanced Bleeding Gums
- Advanced Receeding Gums
- Bleeding Gums
- Children’s Oral Health
- Coronal Fracture
- Dental Anestheia and Sedation
- Dental Plaque
- Dental Radiology
- Dentistry and Diabetes
- Fluoride Treatments
- Gum Cancer
- Gum Infection
- Occlusal Splint
- Oral and Maxillofacial Pathology
- Oral Hygiene
- Oral Hygiene Blogs
- Oral Hygiene Case Reports
- Oral Hygiene Practice
- Oral Leukoplakia
- Oral Microbiome
- Oral Rehydration
- Oral Surgery Special Issue
- Orthodontistry
- Periodontal Disease Management
- Periodontistry
- Root Canal Treatment
- Tele-Dentistry
Recommended Journals
Article Tools
Article Usage
- Total views: 23676
- [From(publication date):
July-2015 - Aug 24, 2025] - Breakdown by view type
- HTML page views : 18476
- PDF downloads : 5200