Case Report Open Access
Diagnosis of Cleidocranial Dysplasia: Two Sisters Case Report
Carlos Nicoleta*, Mariajosé Giménezb, María Cristina Henríquezc, Andrea Wernerd and Alfredo Esguepe
Universidad Andrés Bello, Viña del Mar, Chile
- *Corresponding Author:
- Carlos Nicoleta
DDS. Master in Orthodontics
Universidad Andrés Bello, Viña del Mar, Chile
Tel: +56997458630
E-mail: carlos.nicolet.m@gmail.com
Received date: March 17, 2014; Accepted date: May 08, 2014; Published date: May 15, 2014
Citation: Carlos Nicoleta, Mariajosé Giménezb, María Cristina Henríquezc, Andrea Wernerd, Alfredo Esguepe (2014) Diagnosis of Cleidocranial Dysplasia: Two Sisters Case Report. J Interdiscipl Med Dent Sci 2:121. doi:10.4172/2376-032X.1000121
Copyright: © 2014 Nicoleta, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at JBR Journal of Interdisciplinary Medicine and Dental Science
Abstract
Two sisters, ages 8 and 12 years old, were referred to our Orthodontics Department because of delayed eruption and retention of primary dentition. They presented specific physical and oral findings in common, which strongly suggest the idea of an undiagnosed syndrome. Cleidocranial dysplasia (CCD) is a dominant inherited condition with high penetrance and wide variation in clinical expressivity. Some CCD characteristics include maxillary hypoplasia and some dental abnormalities such as retention of primary dentition, multiple supernumerary teeth and delayed or failing eruption of permanents dentition. Dental alterations in CCD frequently result in malocclusion with long and complex dental treatment. CCD is usually under diagnosed because of the relative lack of medical complications in comparison to other syndromes. Early diagnosis of the condition is essential, for approaching to a multidisciplinary treatment. Multiple supernumerary teeth have to be an alert, where family group medical history is essential for inhered condition evaluation. The goal of an accurate diagnosis in patients with multiple syndromic characteristics is the main subject of this paper.
Keywords
Cleidocranial dysplasia; Maxillary hypoplasia; Malocclusion
Introduction
Cleidocranial dysplasia (CCD) is a dominant inherited condition with high penetrance and wide variation in clinical expressivity [1,2].
Some CCD characteristics include short stature, narrow chest and sloping shoulders, clavicular aplasia or deficient formation of the clavicles, delayed closure of cranial fontanels and sutures, brachycephalic appearance, wormian bones. The skull can have parietal and frontal bossing, maxillary hypoplasia and some dental abnormalities such as retention of primary dentition, multiple supernumerary teeth and delayed or failing eruption of permanents dentition. Dental alterations in CCD frequently result in malocclusion with long and complex dental treatment [1-11].
The prevalence is one per million [4,8], with complete penetrance and variable expressivity. The cause of CCD is usually caused by a mutation of the Core Binding Factor-a1 gene (RUNX2, runt-related transcription factor 2), located at chromosome 6p21, which is essential for osteoblast differentiation, maturation of chondrocytes as well as for bone an tooth formation [1-6,12]. However 30 to 40% of the cases appear spontaneously, with no apparent genetic cause. The pathology leads to an early developmental disorder of mesenchyme or connective tissue, with retarded ossification, or in some cases, failure of ossification, in some areas of the skeletal structure [1,5].
Histologic studies have shown abnormal alveolar bone and cementum associated with CCD. Both acellular and cellular cementum are present in deciduous teeth, whereas in permanent teeth, cellular cementum is virtually lacking and acellular cementum partially hyperplastic. The alveolar bone shows abnormal remodeling patterns, with abundant odontogenic epithelium. The aetiology of this failure of eruption is considered to be an abnormality in alveolar bone remodeling as well as fibrosis of the gingival [13-16].
CCD is usually under diagnosed because of the relative lack of medical complications in comparison to other syndromes [4]. Early diagnosis of the condition is essential, for approaching to a multidisciplinary treatment, with cooperation between geneticist, endocrinologist, maxillofacial surgeons and orthodontist. The goal of an accurate diagnosis in patients with multiple syndromic characteristics is the main subject of this paper.
Case Report
Diagnosis and etiology
Two sisters were referred to our Orthodontics Department because of delayed eruption and retention of primary dentition. The older sister was 12-year-old and the younger 8-year-old.
Older sister
The 12 years old girl (Figure 1) was referred to our orthodontic department regarding of prolonged retention of deciduous teeth. Her medical history revealed short stature and a family dental history of supernumeraries.
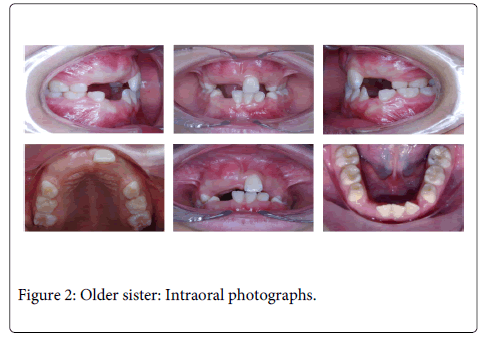
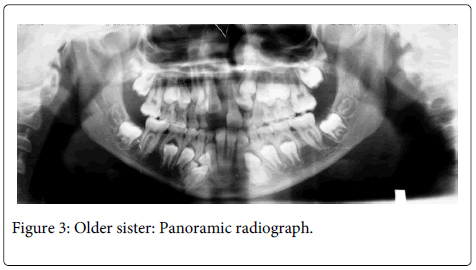
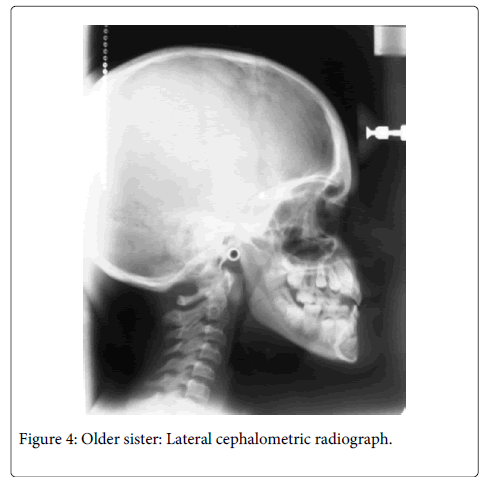
General physical and extraoral examination of the patient showed shorth stature, frontal bossing, depressed and wide nasal bridge, wide nasal base and mid-facial hypoplasia. Intraoral examination showed class III malocclusion, posterior cross bite and retained deciduous teeth (Figure 2). Radiographic findings were multiple unerupted permanent teeth and two supernumerary teeth in the mandibular anterior region (Figure 3). Lateral cephalograph revealed skeletal class III values (Figure 4). Thorax radiographs showed presence of clavicles.
Younger sister
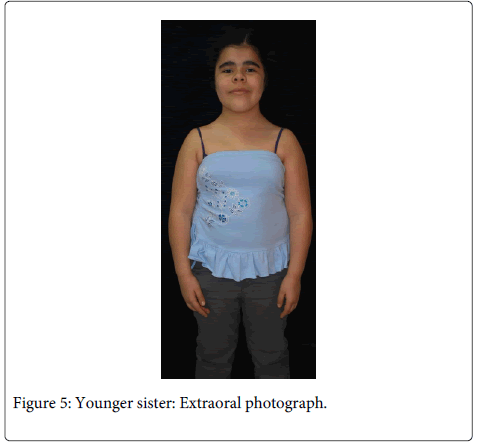
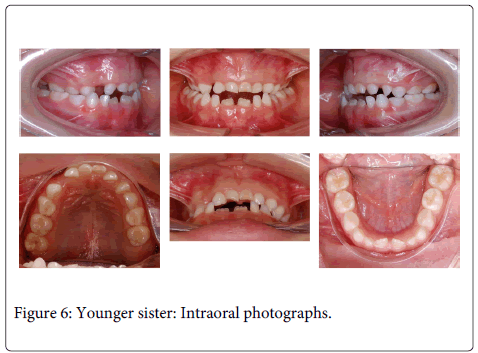
The 8 years old girl (Figure 5) was referred to our department with the chief complaint of delayed eruption of permanent dentition. She had expressed some secondary sexual characters and, because of her short stature, she was under medical treatment in order to prevent early puberty.
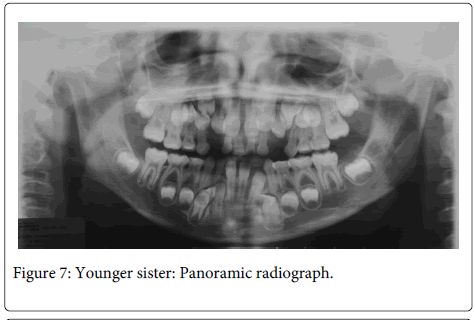
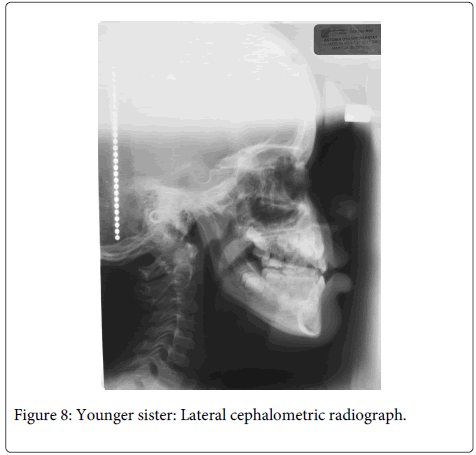
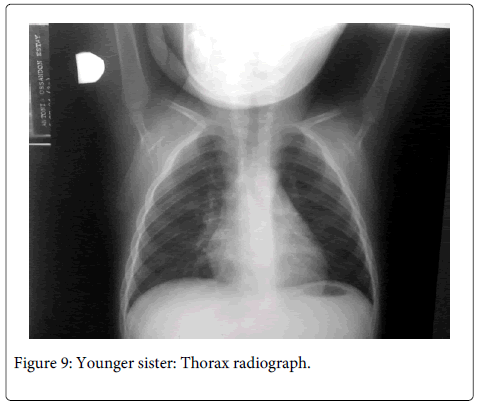
The patient was short statured, narrow chest and sloping shoulders, brachycephalic, with frontal bossing, mid-face hypoplasia, moderate telecanthus and wide nasal bridge and base. Oral findings include mixed dentition, Class III malocclusion with anterior and posterior cross bite and delayed eruption of permanent teeth (two years late in comparison to national standards) (Figure 6). Radiographic findings (Figures 7 and 8) were five supernumerary teeth, three on the upper jaw and two in the mandible. Lateral cephalograph revealed skeletal class III values. Thorax radiographs showed presence of clavicles, but a cone shaped thorax with narrow upper thoracic diameter (Figure 9).
Discussion and Differential Diagnosis
In these two particular cases, we found specific physical and oral findings in common, what suggest the idea of a familial disease or a syndrome. Furthermore, the physical aspects were similar in the rest of the family group (Figure 10).
Short stature, narrow chest and sloping shoulders, frontal bossing, brachycephalic appearance, wide nasal bridge and base and mid-facial hypoplasia, and dental abnormalities (retention of primary dentition, multiple supernumerary teeth and delayed eruption of permanents dentition) strongly suggest CCD (Table 1). Thorax radiographs showed presence of clavicles, but a cone shaped thorax with narrow upper thoracic diameter, especially in the younger sister.
| CLINICAL/RADOGRAPHIC FEATURE | OLDEST SISTER | YUNGEST SISTER |
|---|---|---|
| SHORT STATURE | X | X |
| NARROW CHEST | - | X |
| CLAVICULAR APLASIA/HYPOPLASIA | - | - |
| BRACHYCEPHALIC | X | X |
| WORMIAN BONES | - | - |
| FRONTAL BOSSING | X | X |
| MAXILLARY HYPOPLASIA | X | X |
| RETENTION OF PRIMARY DENTITION | X | X |
| DELAYED ERUPTION OF PERMANENT DENTITION | X | X |
Table 1: Clinical and radiographic CCD features (X=present).
A karyotype test was preformed, with GTG (Trypsin) banding, with no evident structural alteration. Specific test for the RUNX2 gene (sequence analysis and deletion/duplication analysis) weren’t preformed because of the patients’ financial situation and having in consideration that 30 to 40% of the clinical diagnoses are not genetic supported [1,5].
Even though the clavicles are present, CCD with a low expressivity was established as final diagnosis. However, differential diagnosis with other conditions, presenting characteristics in common with CCD, was necessary.
Achondroplasia is the most common process resulting in disproportionate small stature. Affected individuals have short arms and legs, a large head, and characteristic facial features with frontal bossing and midface hypoplasia [17,18].
Achondroplasia can be diagnosed by characteristic clinical and radiographic findings in most affected individuals. In individuals in whom there is diagnostic uncertainty or atypical findings, molecular genetic testing can be used to detect a mutation in FGFR3, the only gene known to be associated with achondroplasia [17,18].
Approximately 80% of individuals with achondroplasia have parents with average stature. The risk to other family members depends on the status of the proband's parents. If a parent is affected, his or her family members are at risk [17,18].
While the family group has similar physical characteristics, the presence of supernumerary and radiographic findings showed no association with achondroplasia.
Multiple supernumerary teeth were the presenting feature in these cases. Supernumerary teeth may be sporadic, familial or condition associated [7,19]. The familial form is inherited as an isolated autosomal dominant trait, with reduced penetrance and variable phenotypic expression [7]. Conditions associated with supernumerary teeth are cleft lip and palate, trichorhinophalangeal syndrome, cleidocraneal dysplasia, and Gardner’s syndrome [7,19].
Gardner’s syndrome is one of the associated polyposis conditions, where the presence of intestinal polyposis is a marker [20]. Familial adenomatous polyposis is associated with a number of extraintestinal manifestations, which include osteomas, dental abnormalities (especially supernumerary teeth and/or odontomas), congenital hypertrophy of the retinal pigment epithelium, soft tissue tumors (specifically epidermoid cysts and fibromas), desmoid tumors, and associated cancers [19-22].
Because of the severity of the associated cancers, thorax radiographs and endoscopy were preformed in the sisters. We found no evidence of signs associated with the characteristics of Gardner’s syndrome in the patients.
In these cases CCD appears to be the best diagnose, even though we didn’t observe hypoplasia or absence of the clavicles, probably due to the variable expressivity of the condition. Further genetic test can be conduced in order of diagnose confirmation.
The timing of diagnosis is not only important for choosing appropriate treatment objectives, but also improves the prognosis [23]. In these cases bone and cement condition are factors to consider in the treatment planning and mechanics.
A team approach to management of dental abnormalities on a long-term basis is necessary. The overall goal is to provide an esthetic facial appearance and functional occlusion by late adolescence or early adulthood. In these particular cases the treatment objectives are:
Older patient: (1) Correct the posterior crossbite with rapid maxillary expansion; (2) Surgically remove supernumerary teeth; (3) Fenestration and traction the retained incisor; (4) Remove deciduous teeth; (3) Surgically expose and traction the permanent maxillary canines and guide them into occlusion; (4) Align; (5) Assess space needs and the Class III skeletal growth pattern; (5) Retain.
Younger patient: (1) Correct the posterior crossbite with rapid maxillary expansion; (2) Maxillary protraction with extraoral forces (3) Surgically remove supernumerary teeth; (4) Fenestration and traction of teeth, if needed (5) Align; (6) Assess space needs and the Class III skeletal growth pattern; (7) Retain.
The orthopedic phase of the treatment should be performed as soon as possible, taking into account the age of the older patient and the risk of premature puberty of the younger patient. Surgical removal of supernumerary teeth, fenestration and traction of permanent teeth, if necessary, must consider the state of root development of permanent dentition.
Summary and Conclusions
CCD is usually under diagnosed because of the relative lack of medical complications in comparison to other syndromes. Diagnosing the condition can be difficult in cases where there are no evident morphological signs
Whenever clinical findings are not conclusive, differential diagnosis must be conduced.
In most CCD cases, the orthodontist easily perceives an alteration in the rhythm of deciduous teeth replacement.
Multiple supernumerary cases have to be an alert to the orthodontist. Family group medical history is essential for inhered condition evaluation.
Early diagnosis of the condition is essential for better approaching to a multidisciplinary treatment, with cooperation between geneticist, endocrinologist, maxillofacial surgeons and orthodontist.
References
- Mendoza-Londono R, Lee B (1993) Cleidocranial Dysplasia. GeneReviews.
- Bufalino A, Paranaíba LM, Gouvêa AF, Gueiros LA, Martelli-Júnior H, et al. (2012) Cleidocranial dysplasia: oral features and genetic analysis of 11 patients. Oral Dis 18: 184-190.
- C N, Shakuntala BS, Mathew S, Krishnamurthy NH, Yumkham R (2012) Cleidocranial dysplasia presenting with retained deciduous teeth in a 15-year-old girl: a case report. J Med Case Rep 6: 25.
- Farronato G, Maspero C, Farronato D, Gioventù S (2009) Orthodontic treatment in a patient with cleidocranialdysostosis. Angle Orthod 79: 178-185.
- Ott CE, Hein H, Lohan S, Hoogeboom J, Foulds N, et al. (2012) Microduplications upstream of MSX2 are associated with a phenocopy of cleidocranial dysplasia. J Med Genet 49: 437-441.
- Suda N, Hamada T, Hattori M, Torii C, Kosaki K et al. (2007) Diversity of supernumerary tooth formation in siblings with cleidocranial dysplasia having identical mutation in RUNX2 : possible involvement of non-genetic or epigenetic regulation. OrthodCraniofac Res 10: 222-225.
- Roberts T, Stephen L, Beighton P (2013) Cleidocranial dysplasia: a review of the dental, historical, and practical implications with an overview of the South African experience. Oral Surg Oral Med Oral Pathol Oral Radiol 115: 46-55.
- Bhat MA, Laway BA, Mantoo S, Choudry K, Kotwal S, et al. (2012) Cleidocranial dysplasia: a rare cause of disproportionate severe short stature. Oman Med J 27: 408-410.
- Kuroda S, Yanagita T, Kyung HM, Takano-Yamamoto T (2007) Titanium screw anchorage for traction of many impacted teeth in a patient with cleidocranial dysplasia. Am J OrthodDentofacialOrthop 131: 666-669.
- Angle AD, Rebellato J (2005) Dental team management for a patient with cleidocranialdysostosis. Am J OrthodDentofacialOrthop 128: 110-117.
- Trigui M, Ayadi K, Elhassan MO, Zribi M, Chabchoub I, et al. (2011) Cleidocranial dysplasia: report of 2 cases and literature review. Arch Pediatr 18: 672-677.
- Mundlos S, Otto F, Mundlos C, Mulliken JB, Aylsworth AS, et al. (1997) Mutations involving the transcription factor CBFA1 cause cleidocranial dysplasia. Cell 89: 773-779.
- Lukinmaa PL, Jensen BL, Thesleff I, Andreasen JO, Kreiborg S (1995) Histological observations of teeth and peridental tissues in cleidocranial dysplasia imply increased activity of odontogenic epithelium and abnormal bone remodeling. J Craniofac Genet DevBiol 15: 212-221.
- Dard M (1993) Histology of alveolar bone and primary tooth roots in a case of cleidocranial dysplasia. Bull Group IntRechSciStomatolOdontol 36: 101-107.
- Gundlach KK, Buurman R (1978) Cleidocranial dysplasia--histological findings in the dental cementum. DtschZahnarztl Z 33: 574-578.
- Migliorisi JA, Blenkinsopp PT (1980) Oral surgical management of cleidocranialdysostosis. Br J Oral Surg 18: 212-220.
- Pauli RM (1998) Achondroplasia. GeneReviews.
- Sberna MT, De Angelis D, Laruffa F, Tettamanti L, Storti E (2012) Oral manifestation of cleido cranial displasia. Minerva Stomatol 61: 421-429.
- Pereira MN, de Almeida LE, Martins MT, da Silva Campos MJ, Fraga MR, et al. (2011) Multiple hyperdontia: Report of an unusual case. Am J OrthodDentofacialOrthop 140: 580-584.
- Jasperson KW, Burt RW (1998) APC-Associated Polyposis Conditions. GeneReviews.
- Herrmann SM, Adler YD, Schmidt-Petersen K, Nicaud V, Morrison C et al. (2003) The concomitant occurrence of multiple epidermal cysts, osteomas and thyroid gland nodules is not diagnostic for Gardner syndrome in the absence of intestinal polyposis: a clinical and genetic report. Br J Dermatol 149: 877-83.
- Davies DR, Armstrong JG, Thakker N, Horner K, Guy SP, et al. (1995) Severe Gardner syndrome in families with mutations restricted to a specific region of the APC gene. Am J Hum Genet 57: 1151-1158.
- Mohan RP, Suma GN, Vashishth S, Goel S (2010) Cleidocranial dysplasia: clinico-radiological illustration of a rare case. J Oral Sci 52: 161-166.
Relevant Topics
- Cementogenesis
- Coronal Fractures
- Dental Debonding
- Dental Fear
- Dental Implant
- Dental Malocclusion
- Dental Pulp Capping
- Dental Radiography
- Dental Science
- Dental Surgery
- Dental Trauma
- Dentistry
- Emergency Dental Care
- Forensic Dentistry
- Laser Dentistry
- Leukoplakia
- Occlusion
- Oral Cancer
- Oral Precancer
- Osseointegration
- Pulpotomy
- Tooth Replantation
Recommended Journals
Article Tools
Article Usage
- Total views: 18369
- [From(publication date):
June-2014 - Sep 04, 2025] - Breakdown by view type
- HTML page views : 13708
- PDF downloads : 4661