Case Report Open Access
Oral Thrush in an Infant: A Case Report with Treatment Modalities
Sachdeva SK1*, Dutta S2, Sabir H3and Sachdeva A41Reader, Department of Oral Medicine and Radiology, Surendera Dental College and Research Institute, Rajasthan, India
2Professor and Head, Department of Oral Medicine and Radiology, Maharana Pratap College of Dentistry and Research Centre, Madhya Pardesh, India
3Private Practitioner, Raj Multispeciality Dental Clinic, Madhya Pardesh, India
4Senior Lecturer, Department of Prosthodontics, JCD Dental College, Haryana, India
- *Corresponding Author:
- Sachdeva SK
Associate Professor, Surendera Dental College and Research Institute
Sriganganagar, Rajasthan, India
Tel: 0154- 2440071/2440072
E-mail: drsureshsachdeva7184@gmail.com
Received date: March 20, 2016; Accepted date: March 24, 2016; Published date: March 30, 2016
Citation:Sachdeva SK, Dutta S, Sabir H, Sachdeva A (2016) Oral Thrush in an Infant: A Case Report with Treatment Modalities. Pediatr Dent Care 1:106.doi:10.4172/pdc.1000106
Copyright: © 2016 Sachdeva SK. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Neonatal and Pediatric Medicine
Abstract
Oral thrush or acute pseudomembranous candidiasis is a fungal infection of the oral mucosa with Candida albicans. Clinically, it appears as a white curd like plaque, which on removal leaves a red base. Oral thrush is an opportunistic infection of the oral cavity, which may be seen in newborn infants, the source of which may be from the birth canal, candidal infected skin of the mother’s nipple or a pacifier. Here a case of oral candidiasis is presented in an infant, who responded well to the treatment.
Keywords
Acute; Candidiasis; Thrush; Infants
Introduction
Oralthrushor acute pseudomembranous candidiasisis opportunistic infection, may affect any person. The various risk factors include oral dryness, antibiotics, immunosuppression, diabetes, HIV, steroids, nutritional deficiency, Radiation/Chemotherapy. Oral thrush is caused by yeast-like fungus, candida. C. albicans is a normal commensal of the mouth and generally causes no problems in healthy people. Overgrowth of this organism in the oral cavity may lead to local discomfort, altered taste sensation, dysphagia. The diagnosis of the oral thrush is essentially clinical. Clinically, it may appear as a white curd-like plaque, which adheres to whole of the oral mucosa including tongue, buccal mucosa, palate, gingiva, and oropharyngeal areas. When these areas are scrapped off, there may be pain or slight bleeding [1]. In infants, the source of infection may be from the birth canal, candidal infected skin of the mother’s nipple or a pacifier [2]. Fisher- Hoch and Hutwagner reported that during 1980-1989, the rate of neonatal oropharyngeal candidiasis has increased 4.7 times. They also reported that number of pediatric deaths secondary to oropharyngeal candidiasis has increased 5-folds during this period [3]. Therefore, it is important for the clinicians to be aware of the risk factors, diagnostic aspects and treatment of oral candidiasis within infants. Here a case of oral candidiasis is presented in an infant, who responded well to the treatment.
Case Report
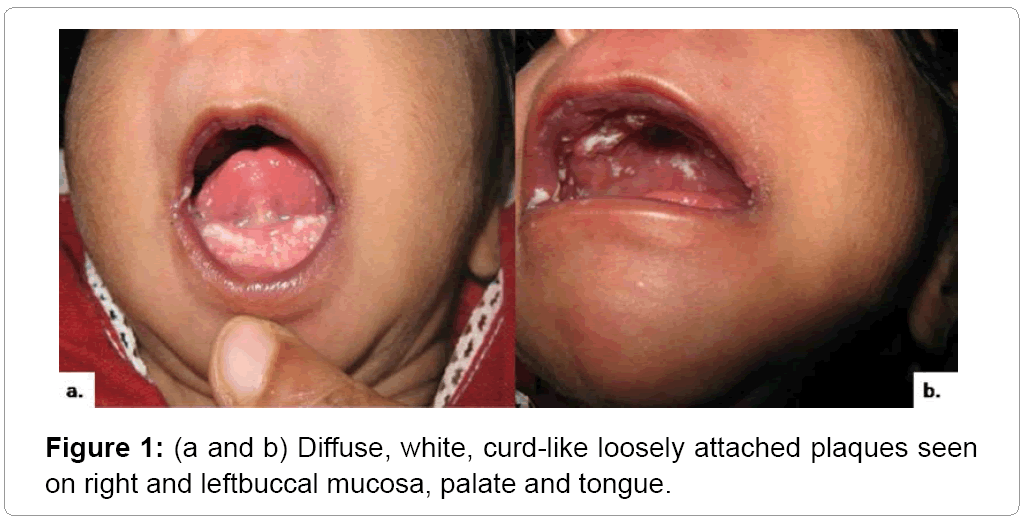
A ten-days old male patient visited the department with a chief complain of white deposits in the whole oral cavity, as reported by mother. On history, whitish deposits were present since birth without any other problem. Past medical, dental and family history was non contributory and patient was not on mother’s milk. On general examination, patient was moderately built, conscious and slightly uncooperative. On local examination of the oral cavity, diffuse, white curd-like plaques were observed over right and left buccal mucosa, palate and tongue. These plaques were scrapable and showed erythematous mucosa on scraping. This finding supported the straight forward clinical diagnosis of pseudomembraneous candidiasis. The patient was advised topical application of clotrimazole (1%) 3-4 times daily with maintenance of good oral hygiene. Within 3 days of treatment, the infant responded well and oral cavity was completely cleared off the white plaques (Figure 1).
Discussion
Candida organism is ubiquitous as it is commonly found on skin and mucosal surfaces. It is estimated that 5-7% of babies less than one month old generally develops oral thrush. In general, the oral microbial flora and the body defenses keep this organism under control. But, when the body’s defenses are compromised (such as HIV,cancer, chemotherapy/radiotherapy treatment, immunosuppression, or use of broad spectrum antibiotics, etc.), then the colonization of this organism takes place [1].
Predisposing factors for oral thrush in infants may include damage to the skin of the nipple, mastitis, long-term use of antibiotics prior to pregnancy or after the delivery, and a history of vaginal thrush. It can also cause an infection in a woman’s nipples, which can then be transmitted to an infant’s mouth during breastfeeding but our patient’s mother did not give the history of breastfeeding [4]. In the present case, oral thrush might be the results of immature immune response and infection was probably acquired during passage through the birth canal.
Earlier the treatment of oral thrush was with gentian violet, an aniline dye. Now, this dye is not used because of resistance developing and side effects, such as staining of the oral mucosa. Treatment of oral thrush is usually by topical antifungal agents, such as 1 ml of 100,000 units of nystatin (mycostatin) divided equally in 2 drops, 4 times/daily for 10-14 days. Nystatin is not systemically absorbed, so it is safe with no drug interactions. Nystatin is more effective in pastille (lozenge) form, due to prolonged contact time, but due to risk of aspiration, it is not used in infants. Systemic antifungal therapy is used in patients intolerant or refractory to topical treatment and those at high risk of developing systemic infections. In cases, where systemic treatment is needed, topical therapy should continue as this reduces the dose and duration of systemic therapy. Other antifungal agents which are effective in the treatment of oral thrush include amphotericin B, clotrimazole, fluconazole, and ketoconazole. Clotrimazole (10 mg/ml) oral suspension can be used 4 times/daily for 2 weeks. Ketaconazole is not recommended for the infant, due to risk of liver toxicity [2,5]. Culture and sensitivity testing should be undertaken if initial therapy is unsuccessful [6].
Treatment for mother’s infected breast is use of fluconazole for atleast 2-week. Moreover the breast-feeding of the infant should not be stopped. In addition, the vaginal candidiasis in the third trimester and postpartum should be done aggressively [7]. Other adjunctive treatment modality for the oral thrush is use of live-cultured yogurt containing acidophilus bacteria, in infants at least 6 months of age [8]. Orally administered Lactobacillus casei subspecies rhamnosus significantly reduces the incidence and the intensity of enteric colonization by Candida among very low birth weight neonates [9]. 5% Cranberry (Vaccinium macrocarpon Ait) can be used for the treatment its proanthocyanidins prevents the Candida albicans adherence and biofilm formation [10].
Conclusion
As oral thrush is increasing in infants, and it may lead to the death, it is important for the general practitioner to be familiar with its clinical appearance. The successful management of oral thrush involves treatment of secondary mother’s breast skin infections and maintenance of pacifier hygiene along with appropriate use of antifungal agents.
References
- Samaranayake LP, Lamey PJ (1988) Oral candidosis: Clinicopathological aspects. Dent Update 15: 227-228, 230-1.
- Darwazeh AM, Al-Bashir A (1995) Oral candidal flora in healthy infants. J Oral Pathol Med 24: 361-364.
- Fisher-Hoch SP, Hutwagner L (1995) Opportunistic candidiasis: an epidemic of the 1980s. Clin Infect Dis 21: 897-904.
- Zöllner MS, Jorge AO (2003) Candida spp. occurrence in oral cavities of breastfeeding infants and in their mothers' mouths and breasts. Pesqui Odontol Bras 17: 151-155.
- Epstein JB, Polsky B (1998) Oropharyngeal candidiasis: a review of its clinical spectrum and current therapies. Clin Ther 20: 40-57.
- Akpan A, Morgan R (2002) Oral candidiasis. Postgrad Med J 78: 455-459.
- Hartung de Capriles C, Mata-Essayag S, Azpiróz A, Ponente A, Magaldi S, et al. (2005) Neonatal candidiasis in Venezuela: clinical and epidemiological aspects. Rev Latinoam Microbiol 47: 11-20.
- Petti S, Tarsitani G, D'Arca AS (2001) A randomized clinical trial of the effect of yoghurt on the human salivary microflora. Arch Oral Biol 46: 705-712.
- Manzoni P, Mostert M, Leonessa ML, Priolo C, Farina D, et al. (2006) Oral supplementation with Lactobacillus casei subspecies rhamnosus prevents enteric colonization by Candida species in preterm neonates: a randomized study. Clin Infect Dis 42: 1735-1742.
- Feldman M, Tanabe S, Howell A, Grenier D (2012) Cranberry proanthocyanidins inhibit the adherence properties of Candida albicans and cytokine secretion by oral epithelial cells. BMC Complement Altern Med 12: 6.
Relevant Topics
- About the Journal
- Birth Complications
- Breastfeeding
- Bronchopulmonary Dysplasia
- Feeding Disorders
- Gestational diabetes
- Neonatal Anemia
- Neonatal Breastfeeding
- Neonatal Care
- Neonatal Disease
- Neonatal Drugs
- Neonatal Health
- Neonatal Infections
- Neonatal Intensive Care
- Neonatal Seizure
- Neonatal Sepsis
- Neonatal Stroke
- Newborn Jaundice
- Newborns Screening
- Premature Infants
- Sepsis in Neonatal
- Vaccines and Immunity for Newborns
Recommended Journals
Article Tools
Article Usage
- Total views: 20456
- [From(publication date):
specialissue-2016 - Aug 19, 2025] - Breakdown by view type
- HTML page views : 18992
- PDF downloads : 1464