Research Article Open Access
Epidemiology of Pandemic H1N1 in Oman and Public Health Response, 2009
Salah Thabit Al Awaidy1*, Idris Al Obeidani2, Jeffrey V. Singh3, Salim Al Mahrouqi2, Suleiman Salim Al Busaidy4, Said Al Baqlani4 and Robert D. Allison51Office of HE of Health Affairs, Ministry of Health, Muscat, Oman
2Department of Communicable Disease Surveillance & Control, DGHA, Ministry of Health, Muscat, Oman
3Directorate General of Health Affairs, Muscat, Ministry of Health, Muscat, Oman
4Central Public Health Laboratory, DGHA, Ministry of Health, Muscat, Oman
5Johns Hopkins Bloomberg School of Public Health, Baltimore, MD, USA
- *Corresponding Author:
- Salah Thabit Al Awaidy
Office of HE of Health Affairs, Ministry of Health
Muscat, Oman, P.O.Box: 393, Oman
Tel: 968 99315063
E-mail: salah.awaidy@gmail.com
Received date: February 25, 2015; Accepted date: March 30, 2015; Published date: April 03, 2015
Citation: Al Awaidy ST, Al Obeidani I, Singh JV, Al Mahrouqi S, Al Busaidy SS, et al. (2015) Epidemiology of Pandemic H1N1 in Oman and Public Health Response, 2009. J Community Med Health Educ 5:343. doi: 10.4172/2161-0711.1000343
Copyright: © 2015 Al Awaidy ST, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Community Medicine & Health Education
Abstract
A retrospective study of influenza-like illness (ILI) in Oman was completed to describe the epidemiology of pandemic influenza A, subtype H1N1 activity (pH1N1). From June to December 2009, 8,941 specimens were collected nationwide from patients that met the case definition for ILI, of which 6,547 (73%) were tested for pH1N1 by real-time polymerase chain reaction (RT-PCR). Out of these, 4,089 (62%) were found positive for pH1N1 and 712 (11%) were positive for seasonal influenza A. The mean age of patients positive for pH1N1 was 24 years (28 days-74 years). Out of the total patients who met the definition of severe acute respiratory illness (SARI) and required hospitalization, 28.3% were positive for pH1N1. The overall case fatality rate was 1.1 deaths/100,000 populations. Two governorates, Muscat and Dhofar, witnessed the greatest intensity of influenza activity. Mitigation, containment, pharmaceutical and non-pharmaceutical measures were engaged. Based on the experience and lessons learned in Oman, some recommendations were sought in Oman.
Keywords
Pandemics; Influenza A Virus; H1N1 Subtype; Epidemiology; Oman
Introduction
The burden of infectious diseases is felt mainly because of their dissemination in a short span of time resulting in epidemics or outbreaks [1]. Globally, lower respiratory tract infections ranked as the fourth leading cause of death in 2012 and are the most significant infectious causes of death in the world.
Influenza is an acute and highly contagious viral respiratory infection causing significant morbidity and mortality with worldwide public health implications. Seasonal influenza viruses continually circulate in yearly epidemics, while anti-genically novel strains, similar to the re-assorted pandemic H1N1 (pH1N1), emerge sporadically [2,3].
The pH1N1 virus rapidly travelled around the world. As of June 9, 2009, a total of 73 countries had reported more than 26,000 laboratory-confirmed cases, and the World Health Organization (WHO) declared that the situation met the criteria for a phase 6 pandemic. By the time the pandemic had waned in August 2010, virtually all countries had reported laboratory-confirmed cases. While exact figures of the death toll from pH1N1 are unknown, estimates range from 105,700 to 395,600 deaths [4]. The WHO provided early recommendations on administering vaccine to target groups and valuable field assistance to affected countries. WHO efficiently distributed more than 3 million courses of antiviral drugs to 72 countries [4-6].
Surveillance and epidemiologic investigations are critical public health functions during outbreaks, epidemics and pandemics. Thus, timely public health surveillance and epidemiologic investigations are crucial for an effective public health response because they allow public health officials to gather health information, prioritize response activities, and make appropriate public health decisions [7].
Global influenza surveillance has been conducted through the WHO Global Influenza Surveillance and Response System (GISRS) since 1952. The current network is comprised of six WHO collaborating centres, four essential regulatory laboratories and 136 institutions in 106 WHO member states, which are recognized by WHO as national influenza centres [8].
Oman was not spared from the reaches of the pH1N1 and by June 2009 the first pH1N1 cases had been laboratory-confirmed. The Ministry of Health of the Government of Oman stepped-up all the activities related to pandemic influenza management.
This report highlights the 2009 pH1N1 outbreak characteristics and epidemiology, national response and recommendations following response evaluation and lessons-learnt.
Materials and Methods
Background information
An analysis was conducted to describe the epidemiology of the pandemic, and included all cases reported under pH1N1 surveillance in Oman during 2009.
The WHO case-definitions for influenza-like illness (ILI) and severe acute respiratory infection (SARI) were used. ILI was defined as an acute respiratory infection with measured fever of ≥38°C and cough with onset within the last 10 days. SARI is an acute respiratory infection that met the case definition for ILI and required hospitalization [9].
A communicable diseases case notification form was used to collect the data. The following variables were recorded for each patient: age, sex, clinical presentation, travel and treatment history, and laboratory results [10].
The data were entered into a computerized database using Epi Info 2000. The data were analysed statistically using Statistical Package for the Social Sciences (SPSS) version 19. Odds ratio with 95% CI was calculated for signs and symptoms. Other parameters were expressed in proportions. A P value of <0.05 was considered as significant.
Results
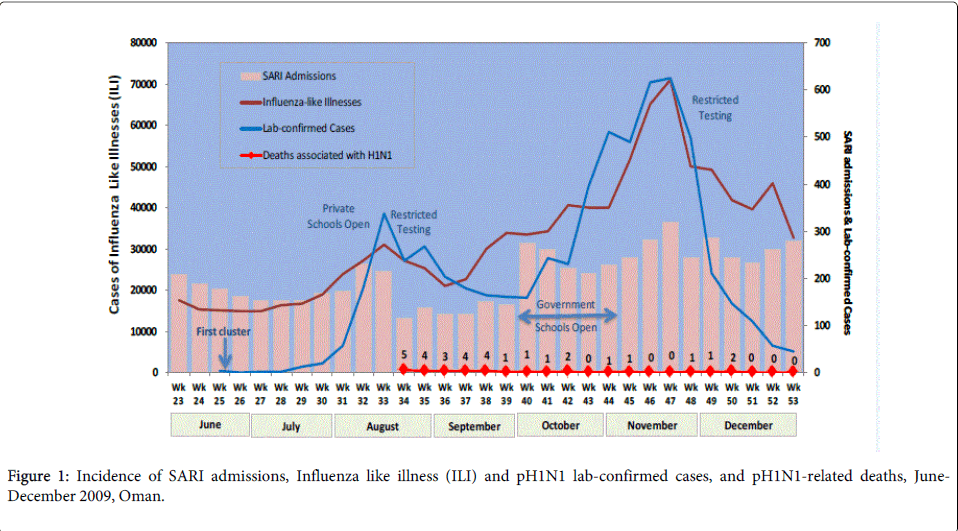
The first 3 cases of confirmed pH1N1 cases occurred amongst students returning from the USA on June 17 (Figure 1). There was then a silent gap of nearly two weeks for other cases to appear. From the first week of July onwards a number of suspect cases tested positive. Almost all of these cases in July were reported from Muscat Governorate and were associated with travel from the USA, Europe and South East Asia. Although initially containment activities were undertaken, by the end of July a transition to mitigation activities was observed. Two governorates of Oman, Muscat and Dhofar, witnessed intense influenza activity. Significant impact was observed in Dhofar governorate closely following the tourist “Khareef season.” The influenza A pH1N1 subtype spread rapidly in Dhofar during this period leading to the first cluster of mortality amongst the population. The diagnostic services at the central public health laboratory were stretched to the limit leading to the first revision of criteria for testing with an announcement that only limited cases within a cluster will be tested.
In the ensuing weeks after July 2009, pH1N1 infections spread to all geographical areas in the country. There was significant increase in the number of cases due to focal outbreaks in expatriate schools in the country. By August the disease was firmly established with widespread distribution. By middle of December the number of cases tested positive among hospitalized patients with SARI had dropped significantly. The timelines for the pandemic in Oman and the actions taken are summarized chronologically as follows Table 1.
| Period | Description | Response |
|---|---|---|
| Apr 26-May 30, 2009 | Preparatory phase | Containment measures adopted |
| Activation of plan | ||
| Preparation of action algorithms | ||
| Port of Entry (PoE) surveillance | ||
| National committee | ||
| Infection control measures | ||
| Community education | ||
| Jun 1-Jun 30, 2009 | Initial cluster investigation | Isolation |
| Antiviral use | ||
| Contact management | ||
| Case management protocol | ||
| Home quarantine | ||
| Jul 1-Jul 31,2009 | Travel associated cases (Muscat Governorate) | Transition to mitigation |
| Aug 1-Sep 30, 2009 | Community spread. | Mitigation measures adopted |
| Cases reported from all regions | Stopped PoE surveillance | |
| Most affected areas: Muscat andDhofar Governorates | Infection control measures | |
| Antiviral use liberalised | ||
| Selective diagnostic testing | ||
| Community awareness campaigns | ||
| Private school outbreaks | ||
| Oct 1-Dec 31, 2009 | Geographically widespread disease | Mitigation |
| Vaccination of high-risk groups | ||
| Vaccine advocacy | ||
| Feedback system | ||
| Government school outbreaks | ||
| Restricted diagnostic testing | ||
| Jan 1-Apr30, 2010 | Downward trend | Reviewing |
| Planning of future Strategies |
Table 1: Analysis of symptoms and signs, pH1N1 lab-confirmed cases, June-December 2009, Oman.
From June to December 2009, a total of 8,941 specimens from patients that met the case definition for influenza-like illness (ILI) were collected, of which 6,547 (73%) specimens were tested for pH1N1 by real-time polymerase chain reaction (RT-PCR) nationwide. Out of these, 4,089 (62%) were found positive for pH1N1, 712 (11%) samples were positive for seasonal influenza A, and 1% of samples tested were inconclusive. The mean age of positive pH1N1 cases was 24 years (28 days-74 years).
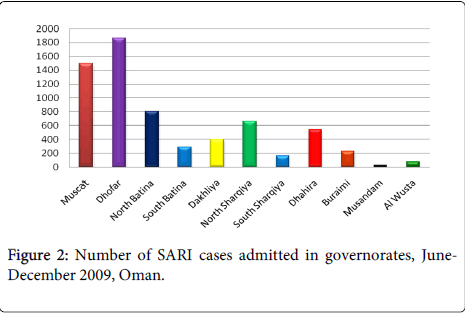
The highest number of samples that tested positive for pH1N1 (June-December 2009) were collected in three major governorates in the following order; Muscat 708 (50.4%), Dhofar 269 (19%) and North Batinah 189 (13.4%).
The influenza A pH1N1 subtype reached Oman with the first cluster of cases reported in week 25.Two governorates of Oman- Dhofar and Muscat-experienced the highest influenza activity and severity. A significant increase in pH1N1 laboratory-confirmed cases was observed in Dhofar Governorate during the tourist “Khareef season” (July-August 2009). Furthermore, the opening of private schools in Dhofar governorate during week 32, facilitated rapid viral spread in the community and led to the first clusters of mortality amongst the population in weeks 34 and 35 Figure 1.
In July-August 2009, the second wave of outbreak was observed in the large Indian schools in Muscat governorate. In response, some schools decided to remain closed. During this period Muscat governorate had the maximum number of cases reported.
Overall clinical symptoms were mild. An analysis of clinical signs and symptoms of 290 patients during the initial period from Muscat governorate was analysed and the analysis are as shown in Table 2. Fever [OR 5.6 (2.9-10.8), p<0.01], headache [OR 1.8 (1.1-5.8), p=0.38] and headache with fever [OR 3.3 (1.5-7.1), p=0.05] were the most common significant symptoms.
| Analysis | Univariate | Multivariate | |||||
|---|---|---|---|---|---|---|---|
| Signs and Symptoms | RT-PCR Result | Crude O.R.* (95% C.I.) | Adjusted O.R.* | 95% C.I. for O.R.* | P-value | ||
| Positive (N=157) | Negative (N=133) | Lower | Upper | ||||
| Fever | 116 | 61 | 5.6 (2.9-10.8) | 8.1 | 3.4 | 19 | <0.001 |
| History of fever | 111 | 71 | 3.3 (1.5-7.1) | 2.7 | 1 | 7.5 | 0.05 |
| Sore throat | 118 | 96 | 1.3 (0.6-2.5) | 1 | 0.4 | 2.8 | 0.94 |
| Rhinorrhoea | 107 | 92 | 0.9 (0.5-1.7) | 0.5 | 0.2 | 1.1 | 0.1 |
| Dry cough | 96 | 70 | 1.5 (0.9-2.6) | 2.1 | 0.8 | 5.2 | 0.13 |
| Productive cough | 41 | 29 | 1.3 (0.7-2.4) | 1.5 | 0.5 | 4.7 | 0.52 |
| Nausea | 26 | 18 | 1.2 (0.6-2.4) | 0.9 | 0.3 | 2.8 | 0.83 |
| Vomiting | 19 | 12 | 1.2 (0.6-2.8) | 0.9 | 0.2 | 3.9 | 0.89 |
| Headache | 81 | 52 | 1.8 (1.1-5.8) | 1.5 | 0.6 | 3.7 | 0.38 |
| Myalgia | 71 | 51 | 1.2 (0.7-2.0) | 0.5 | 0.2 | 1.5 | 0.2 |
| Joint pain | 40 | 24 | 1.6 (0.9-2.8) | 1.9 | 0.6 | 6.5 | 0.3 |
Table 2: Analysis of symptoms and signs, pH1N1 lab-confirmed cases, June-December 2009, Oman.
Severe cases and hospitalization
Out of the total, 6,547 patients met the definition of severe acute respiratory illness (SARI) and required hospitalization in the country. Most of the cases were admitted in Muscat and Dhofar governorates as shown in Figure 2. Patients less than 2 years of age represented the largest group of cases, 2,029 (31%), followed by 12-45 years, 1,833 (28%). Pregnant women with SARI represented 176 (2.7%) of the admissions. Around 25-40% of patients had known risk factors for severe influenza complications and 262 (4%) of admitted cases required ICU admission. The positivity for pH1N1 among admitted cases was 1,833 (28%).
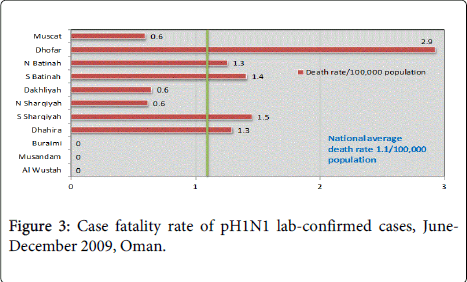
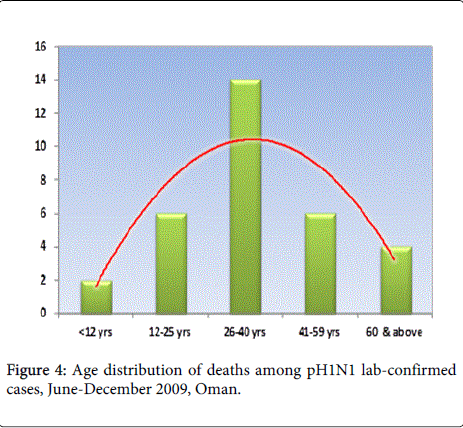
Among the SARI cases, 33 deaths were pH1N1 viral infectionrelated. The overall case fatality rate (CFR) in the country was 1.1 per 100,000 population. The CFR varied significantly in the different governorates: Dhofar governorate had the highest case fatality rate, 2.9/100,000, compared to other governorates as shown in Figure 3. Nineteen (60%) of the deaths occurred in the 12-40 year age group as in Figure 4. There were no gender differences in the mortality rates. Fourteen (44%) of patients who died had co-morbidities including diabetes 6 (45%), a history of transplantation 2 (10%) or, cancer 2 (18%), obesity 1 (6%), smoking 1 (8%) and pregnancy 2 (13%). Six (21%) of the deaths occurred in non-Omani patients, which was consistent with the non-Omani proportion in the population.
Intervention activities adopted by the Ministry of Health, Oman
Port of entry (POE) and airport surveillance: Self-declaration by travellers entering Oman regarding influenza-like symptoms, screening of incoming passengers using thermal scanners and arrangement for isolation of suspect cases was initiated. In addition, information on approaches for seeking medical assistance was provided for travellers.
Quarantine: The initial plan involving isolation of patients in a specific hospital was abandoned due to the rapidly evolving pandemic, thus home quarantine procedures were established. Factors that favoured this change were lack of community cooperation, cultural resistance, stretching of limited human resources and rapid increase in secondary cases.
Health Education and Awareness: Public awareness campaign regarding various aspects related to the influenza pandemic was deployed. Awareness focussed on the various issues related to the influenza pandemic including symptoms, transmission, and treatment. A hotline was established for responding to questions from the public as well as to provide necessary directions for approaching the health care system. Wide publicity through all available media was utilized for awareness on prevention and steps to be taken if symptoms develop as well as focusing on the message that simple hand washing is useful enough to contain virus spread and prevention is better than cure.
Pharmaceutical Measure: A plan using the antiviral drug oseltamivir for treating cases based on clinical guidelines was formulated to ensure rational and optimal use. The national committee decided to involve the private sector and provided oseltamivir free of cost for treating suspect cases in order to avoid over-burdening government capacity. Free dispensing of drug from the private sector with appropriate accounting further strengthened the public-private partnership.
The process of acquiring 2.6 million doses of pH1N1 vaccines was initiated to cover the entire population of Oman and a plan of deployment was developed. The vaccination campaign was launched on the 25th of October 2009, prioritising Hajj pilgrims and healthcare workers. The vaccination of other high-risk groups was expanded to include those in essential services, people with chronic diseases, pregnant women and children under five years old.
Non-pharmaceutical Measures: Though various measures such as school closures, cancellation of mass gatherings, isolation and other social distancing was implemented, the effectiveness of community mitigation measures was difficult to measure and thus no definitive conclusions could be ascertained.
Discussion
This report summarizes the epidemiology and public health responses to the first pandemic Influenza A (H1N1) outbreak ever reported in Oman. The pandemic affected mainly those of younger age, similar to the trend observed worldwide [11-13]. Prior studies have shown a high susceptibility of young age groups to the virus [14,15]. The infection caused severe illness that required ICU admission in 4% and had an overall case fatality rate of 1.1 per 100,000 population. These patients were less likely to have received oseltamivir within 48 hours as compared to those who survived and were not admitted to the ICU (15.3% versus 32.1%) [16].
Fever was the most frequent symptom observed, similar to what has been reported in a number of countries [16,17]. The prevalence of associated medical conditions in our patients was as high (72%), particularly among patients with diabetic mellitus and pregnancy, previously reported in a number of countries [16,18-22].
The high case fatality rate observed in Dhofar governorate might be attributed to late introduction of management interventions as well as a huge load of cases that overwhelmed institutional capacity. Although the cases trend was somewhat similar to seasonal influenza, the major differences noted were the early onset of the pandemic during the peak of summer and a decline earlier in the winter compared to seasonal influenza. The laboratory data illustrate that the pH1N1 virus had completely replaced the other strains of influenza during the pandemic. After the decline, the typical seasonal influenza virus infections started reappearing in the laboratory-tested samples. Similar experiences of 2009 pH1N1 have been reported from several authors around the world [23-27].
Based on the experience and lessons learned, the following recommendations were made by the Ministry of Health and integrated into the Oman pH1N1 Preparedness Plan. These recommendations will be used to create policy and standards that will guide the response to future influenza epidemics in Oman [11]:
More proactive decisions with the aid of a fully equipped command centre and work pathways;
Development of protocol and algorithms to manage any crises and ensure appropriate speed of communications;
Integrating the pandemic plan into the National Disaster Preparedness Plan;
Strengthened disease surveillance with appropriate technological incorporation in decision making;
Training of healthcare workers to understand and internalise rational procedures of managing epidemics/pandemics;
Regular simulations and drills to ensure a strict adherence to the preparedness plan guidelines; and
Strengthening of inter-sectorial co-ordination and international cooperation.
The national data collection was not up to standard by end of December 2009, by which time the number of cases drastically reduced due to exhaustion of the cases and the effect of vaccination. Study limitations encountered were the inclusion of mainly hospitalised patients who may not be representative of patients in the community. Additionally, we could not account for underreporting or differential reporting in different governess.
Conclusion
In response to the pandemic, mitigation, containment, pharmaceutical and non-pharmaceutical measures were engaged. Based on the experience and lessons learned, recommendations were made in Oman for the future pandemic response.
References
- Michael M, Sara M, Viswanath K (2013) The H1N1 pandemic: media frames, stigmatization and coping. BMC Public Health. 13:1116.
- Simonsen L (1997) The global impact of influenza on morbidity and mortality. Vaccine. 17:S3-10.
- Cox NJ, Subbarao K (2000) Global epidemiology of influenza: Past and present. Annu Rev Med 51:407-421.
- Fineberg HV (2014) Pandemic preparedness and response - lessons from the H1N1 influenza of 2009. N Engl J Med 370:1335-1342.
- Simonsen L, Spreeuwenberg P, Lustig R, Taylor RJ, Fleming DM, et al. (2013) Global mortality estimates for the 2009 influenza pandemic from the GLaMOR project: a modeling study. PLoS Med 10: e1001558.
- Dawood FS, Iuliano AD, Reed C, Meltzer MI, Shay DK, et al. (2012) Estimated global mortality associated with the first 12 months of 2009 pandemic influenza A H1N1 virus circulation: a modelling study. Lancet Infect Dis 12:687-695.
- Enanoria WT, Crawley AW, Tseng W, Furnish J, Balido J, et al. (2013) The epidemiology and surveillance response to pandemic influenza A (H1N1) among local health departments in the San Francisco Bay Area. BMC Public Health 13:276.
- http://www.who.int/influenza/gisrs_laboratory/national_influenza_centres/en/
- Human infection with pandemic (H1N1) 2009 virus: updated interim WHO guidance on global surveillance
- Ministry of Health, Oman. Communicable disease surveillance and control. A standard operating procedures manual, 2005, 2nd ed. Muscat.
- Torres JP, O’Ryan M, Herve B, Espinoza R, Acuna G, et al. (2010) Impact of the novel influenza A (H1N1) during the 2009 autumn-winter season in a large hospital setting in Santiago, Chile. Clin Infect Dis 50:860-870.
- Echevarría-Zuno S, Mejía-Aranguré JM, Mar-Obeso AJ, Grajales-Muñiz C, Robles-Pérez E, et al. (2009) Infection and death from influenza A (H1N1) virus in Mexico: a retrospective analysis. Lancet 374:2072-2079.
- Fraster C, Donnelly CA, Cauchemez S, Hanage WP, Van Kerkhove MD, et al. (2009) Pandemic potential of a strain of influenza A (H1N1): early findings. Science 324:1557-1561.
- Hancock K, Veguilla V, Lu X, Zohong W, Butler EN, et al. (2009) Cross reactive antibody responses to the 2009 pandemic H1N1 influenza virus. N Eng J Med 361:1945-1952.
- Centers for Disease Control and Prevention (CDC) (2009) Serum cross reactivity response to a novel influenza A H1N1 virus after vaccination with seasonal influenza vaccine. MMWR Morb Mortal Wkly Rep 58:521-524.
- Al-Lawati J, Al-Tamtami N, Al-QasmiA,Al-Jardani A, Al-Abri S, et al. (2010) Hospitalised patients with Influenza A (H1N1) in the Royal Hospital, Oman: Experience of a tertiary care hospital, July-December 2009 Sultan QaboosUniv Med J10:326-34.
- Swine influenza A H1N1 infection in two children-Southern California. (2009) MMWR Morb Mortal Wkly Rep. 58:400-402.
- Kwong KL, Lung D, Wong SN, Que TL, Kwong NS (2009) Influenza-related hospitalization in children. J Paediatr Child Health 45:660-664.
- Walsh EE, Cox C, Ealsey AR (2002) Clinical features of influenza A infection in older hospitalized persons. J Am Geriatr Soc. 50:498-503.
- Neuzil KM, Maynard C, Griffin MR, Heagerty P (2003) Winter respiratory viruses and health care use: a population based study in the northwest United States. Clin Infect Dis 37:201-207.
- Jamieson DJ, Honein MA, Rassmusen SA, Williams JL, Swerdlow DL, et al. (2009) H1N1 2009 influenza virus infection during pregnancy in the USA. Lancet. 274:451-458.
- Freeman DW, Barno A (1959) Deaths from Asian influenza associated with pregnancy. Am J Obstet Gynecol. 78:1172-1175.
- Ministry of Health, Oman. H1N1 Pandemic Preparedness Plan, 2009.
- Bautista E, Chotpitayasunondh T, Gao Z, Harper SA, Shaw M, et al. (2010) Clinical aspects of pandemic 2009 influenza A (H1N1) virus infection. N Engl J Med. 362:1708-1719.
- Michaelis M, Doerr HW, Cinatl J Jr. (2009) An influenza A H1N1 virus revival - pandemic H1N1/09 virus. Infection. 37:381-389.
- Ison MG, Lee N (2010) Influenza 2010-2011: lessons from the 2009 pandemic. Cleve Clin J Med. 77:812-20.
- Peacey M, Sonnberg S, Ducatez M, Paine S, Nicol M, et al. (2010) Pandemic (H1N1) 2009 and seasonal A (H1N1) influenza co-infection, New Zealand, 2009. Emerg Infect Dis. 16:1618-1620.
Relevant Topics
- Addiction
- Adolescence
- Children Care
- Communicable Diseases
- Community Occupational Medicine
- Disorders and Treatments
- Education
- Infections
- Mental Health Education
- Mortality Rate
- Nutrition Education
- Occupational Therapy Education
- Population Health
- Prevalence
- Sexual Violence
- Social & Preventive Medicine
- Women's Healthcare
Recommended Journals
Article Tools
Article Usage
- Total views: 15860
- [From(publication date):
April-2015 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 11249
- PDF downloads : 4611