Make the best use of Scientific Research and information from our 700+ peer reviewed, Open Access Journals that operates with the help of 50,000+ Editorial Board Members and esteemed reviewers and 1000+ Scientific associations in Medical, Clinical, Pharmaceutical, Engineering, Technology and Management Fields.
Meet Inspiring Speakers and Experts at our 3000+ Global Conferenceseries Events with over 600+ Conferences, 1200+ Symposiums and 1200+ Workshops on Medical, Pharma, Engineering, Science, Technology and Business
Research Article Open Access
Evaluation of Mean Glandular Dose during Diagnostic Mammography Examination for Detection of Breast Pathology, in Ethiopia
| Seife Teferi Dellie1*, A. Durga Prasada Rao2, Daniel Admassie3 and Atnatiwos Zeleke Meshesha4 | |
| 1Department of Radiology, College of Health Sciences, Addis Ababa University, Ethiopia | |
| 2Department of Nuclear Physics, College of Science and Technology, Andhra University, Visakhapatnam, India | |
| 3Department of Radiology, College of Health Sciences, Addis Ababa University, Ethiopia | |
| 4Acting Director for Ethiopian Radiation Authority, Addis Ababa, Ethiopia | |
| Corresponding Author : | Seife Teferi Dellie Medical Physicists, Department of Radiology College of Health Sciences Addis Ababa University, Ethiopia E-mail: seifeteferi@yahoo.com |
| Received July 18, 2012; Accepted August 27, 2012; Published August 30, 2012 | |
| Citation: Dellie ST, Durga Prasada Rao A, Admassie D, Meshesha AZ (2012) Evaluation of Mean Glandular Dose during Diagnostic Mammography Examination for Detection of Breast Pathology, in Ethiopia. OMICS J Radiology. 1:109. doi: 10.4172/2167-7964.1000109 | |
| Copyright: © 2012 Dellie ST. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Radiology
Abstract
Background: A mammography examination facilitates the early detection of breast cancer. However, the potential risk of radiation-induced carcinogenesis is also increased with such a procedure. Thus assessment of the breast dose is important.
Objectives: The objectives of this study were to investigate the techniques currently used for diagnostic
mammography in Ethiopia, thereby to estimate the mean glandular dose (MGD) for Ethiopian women.
Materials and methods: A cross-sectional study was conducted on breast cancer patients between 40-64 years of age having compressed breast thickness (CBT) greater than 2 cm. Five mammographic units and 386 women having a total of 1463 mammograms were included in the study period from April 2011-February 2012 in Addis Ababa, Ethiopia.The characteristics of the radiographic equipment and the exposure data of each patient were recorded using designed format. The MGD was calculated from the measured Entrance Surface Air Kerma (ESAK) using appropriate conversion coefficients. The obtained data were analyzed using statistical software.
Results: The range of CBT was 2.2-7.5 cm for CC mammograms with mean ± SD of 4.24 ± 1.1 cm and 2.3-8.0
cm in MLO projection with mean ± SD of 4.64 ± 1.1 cm. The average MGD per exposure was 2.57 ± 2.1 mGy while the respective averages separately for the CC and MLO projections were 2.58 ± 2.2 mGy and 2.57 ± 2.1 mGy, respectively.
Conclusion: The average MGD values recorded in this study were between the limiting value of the Institute of Physical Sciences in Medicine (2.0 mGy) and American College of Radiology (3.0 mGy) recommendation. These ensure that the mammography examination performed in Ethiopia was capable of achieving acceptable dose levels for patient safety.
| Keywords |
| Mammography; Radiation; Compressed breast thickness; Mean glandular dose; Quality control |
| Introduction |
| Breast cancer is the most common type of cancer among women in the majority of the countries in the world and so it is in Ethiopia. Breast cancer represents about 24% of all newly diagnosed cases of cancer rate in Bulgaria and is the second reason for death from oncological diseases [1]. In Israel this is somewhat lower, reaching 13.1 % among Jewish women [2]. X-ray mammography is the method of choice for early detection of breast cancer. Although mammography examination is associated with a very low dose to the breast tissue there exist some risk of cancer induction [3-5]. While there is a certain risk of radiation-induced cancer associated with mammography, this risk is considered acceptable compared to the expected benefits, especially when modern equipment and techniques are used for minimising the dose to the breast [3]. |
| In any radiographic procedure, it is imperative that the radiation dose is as low as reasonably practicable, while maintaining an adequate image quality. This is particularly important in radiography of sensitive organs such as breast and in screening programs where the exposed population is showing no evidence of diseases. It is generally accepted that the glandular tissue of breast is the most radiation-sensitive tissue [5-12]. Therefore, the suggestion that the mean glandular dose (MGD) is the most appropriate dosimetric quantity to predict the risk of radiation-induced carcinogenesis has been widely accepted [7-9]. The MGD cannot be measured directly, but it can be calculated from ESAK, and using appropriate conversion factors [1,2,5-18], apart from few studies in which the ESD was directly measured using thermo luminescent dosimeters (TLDs) positioned on the breast [19]. |
| It should be stressed that, in the present literature, no study regarding diagnostic mammography techniques and radiation dose either in private or government hospitals/clinics in Ethiopia was found. Such data are necessary to formulate recommendations to minimize radiation doses without compromising the image quality, and for the development of national reference doses as recommended by the International Commission on Radiological Protection ICRP [20]. Furthermore, no formal national screening programme has been introduced in our country yet. The objectives of this study were therefore: (1) to investigate the examination techniques currently used both in public and private mammographic units in Ethiopia, (2) to estimate the ESAK and MGD so as to establish a baseline radiation dose database for Ethiopian women, (3) to analyse the effect of clinical factors such as the age and technical factors such as tube potential (kV) and tube loading (mAs) on ESAK and MGD, and finally (4) to compare the results with those of the recent literature. |
| Materials and Methods |
| Mammography equipment |
| In Ethiopia there are seven Mammography units recognized by Ethiopian Radiation Authority. Out of which, six of them are found in Addis Ababa the capital city of Ethiopia. |
| A total of five mammographic units were included in the study, four of which were situated in private diagnostic units (private units BZ, BH, KA and SI) and the remaining one unit government (BL). |
| Initially, a self administered questionnaire regarding the mammography unit including manufacturer, model, focal spot size (FSS, [mm]), film type, cassette size, film processor make/model, source image distance (SID, [mm]), Applied Mode of exposure (AME), kVp and mAs range was prepared in English and distributed to the radiographers working in the study mammography units. The completed questionnaires were checked for completeness and consistency and collected from respective mammography units. |
| All tube output (O/P) reproducibility , half value layer (HVL) measurements, kVp accuracy and reproducibility were performed with a new calibrated digital dosimeter (Mult-O-Meter Unfors, model 535L, Sweden) using exposures of 32 and 80 mAs for the range of kV selections used in the clinical practice. The detector was positioned on the breast support table midways along the direction perpendicular to the anode–cathode axis at 4.8 cm from the image receptor holder, 6 cm from the chest wall edge with the compression plate positioned half way from the detector in place to account for the exposure reduction and beam hardening introduced by the compression plate. The half value layers (HVLs) of each mammography unit were measured for kVp values (24 to 32 kVp with increment of 1 kV). To reduce the effects of scattered radiation, the beam size was limited to the size of the detector sensitive area using magnification slit. For measuring HVL; high purity (99.9%) aluminium (Al) foils were used. The Al foils (0.2– 0.5 mm thick) were positioned on the compression device to intercept the whole radiation field. |
| Patient data |
| This is a cross-sectional study conducted on breast patients between 40-64 years of ages whose CBTs are greater than 2 cm. In order to find sufficient data’s for specified ages and CBTs values a total of 518 breast patients of all ages and all CBT values were selected from all five mammography units including none-respondents. |
| Compressed breast thickness was measured on government unit BL and private unit BH with a ruler and on private units KA, SI and BZ by reading the displayed compressed thickness on the X-ray set (Table 1). The accuracy of the displayed compressed breast thickness was verified by applying a typical force to rigid material of known thickness. ESAK without backscatter on patient’s skin was calculated for each exposure by multiplying the tube loading and the measured tube output for the relevant tube voltage with correction for the distance to the patient’s skin surface. Before conducting the study, the research project was ethically cleared by faculty of Medicine Institute of Review Board (IRB). Ethical clearance and permission was also obtained from the respective mammography units. All participants were informed about the purpose of the study and confidentiality of information. Finally, verbal consent was obtained from each participant. |
| Estimation of MGD |
| The standard method of estimating the MGD dose on patients undergoing mammography X-ray examinations is derived by Dance [17] making use of entrance surface air kerma (ESAK) and tabulated conversion factors. |
| MGD = ESAK gcs |
| where ESAK is the entrance surface air kerma (in the absence of scatter) at the upper surface of the breast. The factor g corresponds to the glandularity of 50%. The factor c corrects for any difference in composition from 50% glandularity, and the factor s corrects for differences due to the choice of X-ray spectrum. The g and c factors were interpolated for age groups, according to the breast thickness, the HVL and the anode/filter combination used. For all mammography units the mean, standard deviation, range of MGD was calculated using (SPSS 16.0). Finally the results of calculated ESAK and MGDs were compared with a similar study. A linear regression analysis with the least squares method was used to determine the correlation between compressed breast thicknesses and ESAK values. Correlations of mAs and MGD were evaluated with Pearson’s correlation coefficient. Comparisons of mean compressed breast thicknesses, and MGD in different imaging projections were performed using the Student’s t test. Bivariate analysis was applied to explore association of explanatory variables with ESAK and MGD. Level of statistical significance was set at P<0.05. |
| Results |
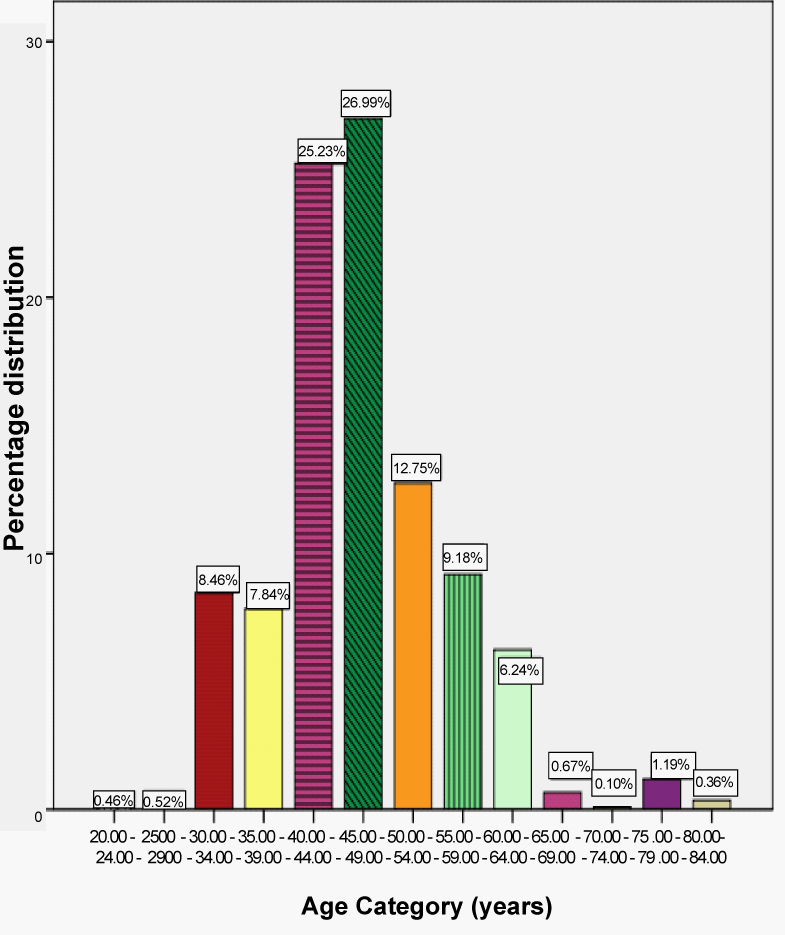
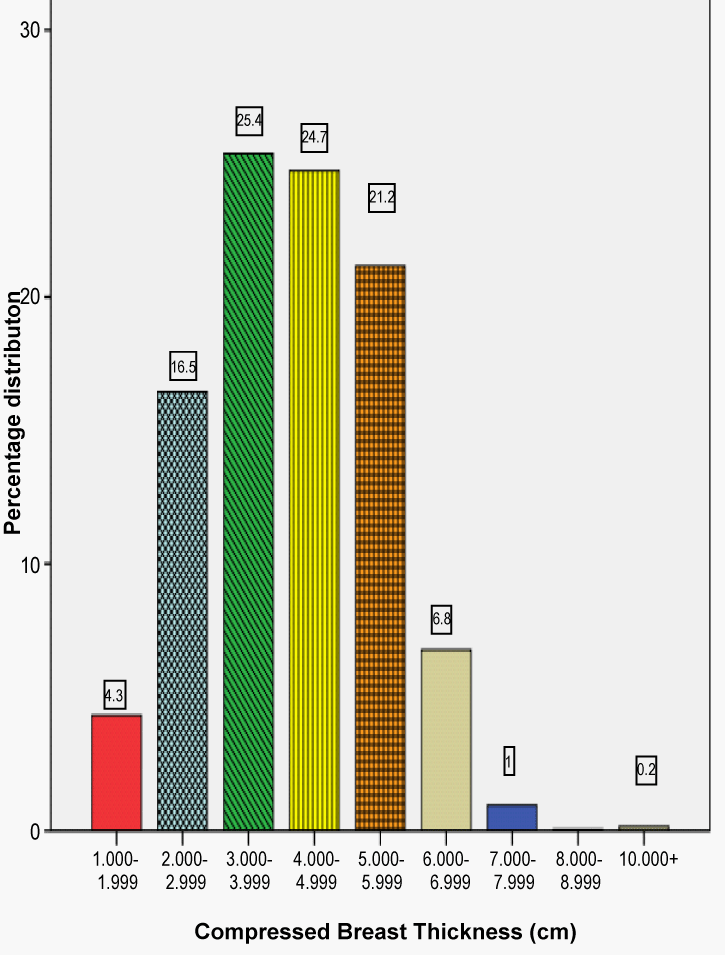
| Out of the 518 selected study subjects, 510 respondents gave valid response, making the overall response rate for the study to be 98.5%. From the distribution of the women examined according to their age given in Figure 1 it can be seen that about 52.2% of the patients were within the age interval 40-49 which was one of the intervals for the age dependent conversion factors and 28.1% were between 50 and 64 years old. The remaining 17.3% and 2.4% were for ages below and above 40 and 64 years of age respectively. The 17.3% part of the patients was in the age interval in which it was considered that the breast contains high glandular tissue having high density. This high density can make mammograms more difficult to interpret and can thus lead to missed diagnoses, as well as increased rates of false-positive findings. During data collection a very wide range of CBT values resulted, whose distribution is given in Figure 2. In order to use Dance [17] conversion factors for estimation of MGD, out of 510 breast patients a total of 124 breast patients of 466 mammograms whose CBT and ages were not between (2 -11) cm and (40-64) years respectively were excluded. Each of the remaining three hundred and eighty six (386) patients had a diagnostic mammographic examination, which usually involved one vertical view (craniocaudal, CC) and one oblique view (mediolateral oblique, MLO) projection in each breast. In some occasions only one projection on each breast was performed while in a few cases only one breast was examined. The distribution of breast thickness was well represented by a normal distribution as shown in Figure 2. |
| All units use manual film processor with eye inspection method. As shown in Table 2, private SI was indeed the only unit where all examinations included two CC and two MLO projections per patient. The same value of tube voltage and mAs were used for both CC and MLO projection in almost all mammography units except KA unit. While in KA unit the kVp and mAs was adjusted using automatic exposure control. Lowest kVp was observed at BZ and KA mammography units with mean ± SD of 26.1 ± 0.6 and 26.5 ± 0.6 respectively, while the highest kVp was observed at BH with mean ± SD of 31.4 ± 0.9. The mean ± SD of kVp all units in the study period were found to be 28.5 ± 2.3 kVp. Overall, tube potentials of 26 kV and 30 kV were used in 23.9% and 21.4% of the mammograms acquired, respectively. |
| As can be seen in Table 3, the average MGD values for all mammography units except BL unit were very similar. The lowest mean ± SD of MGD were observed both at SI and BZ with values of 1.4 ± 0.32 mGy and 1.46 ± 0.45 mGy respectively, while the highest was observed at BL with values of 6.59 ± 0.75 mGy. Table 3 also shows the calculated mean ± SD of ESAK for all mammography units, with values of 4.97 ± 1.24 mGy for SI and 28.75 ± 4.90 mGy for BL having lowest and highest values in that order. The maximum to minimum ratio of the average MGD recorded in the five units was 4.71. The MGD to breast dose was found to vary from 0.23 mGy to 7.89 mGy, with 16.5% of the dose above the upper limit of American College of Radiology (ACR) recommendation established for the reference medium-sized breast of 4.2 cm CBT, illustrating the need of strict quality control. |
| In bivariate analysis kVp, mAs, CBT and HVL were statistically associated with ESAK and MGD for all automatic, manual and combined manual and automatic projections. However no statistical association was found between age, ESAK and MGD for both manual and combined manual and automatic projections. |
| Discussion |
| This is the first systematic dose survey in both private and public mammography units in Ethiopia, in which no official national protocol for screening programme still exists. |
| In this study (Table 2) the results of the mean CBT for CC and MLO films were 4.24 cm and 4.64 cm, respectively. CBT values for CC and MLO films in the present study were somewhat less than the values recorded by other [5]. The difference in CBT of 8.6% between MLO and CC views is lower than that found 16% in Yazed [5] and 12.1% in Young et al. [12]. This may represent a real difference between the populations, a difference in the compression force used, or a difference in the breast thickness measurement technique [17]. In the current study the greatest difference was found in KA, followed by BZ, SI, BL and then BH, women with values of 17% (3.81 cm vs. 4.59 cm), 11.3% (4.18 cm vs. 4.71 cm), 7.7% (3.58 cm vs. 3.88 cm), 6.5% (4.77 cm vs. 5.1 cm), and 1% (4.85 cm vs. 4.90 cm) respectively. These figures indicate that the breast is thinner on the CC than the MLO view. |
| In our study (Table 3), the mean MGD per film, in both views of CC (2.58 ± 2.19 mGy) and MLO (2.57 ± 2.1 mGy), for the mean CBT of 4.24 ± 1.06 and 4.64 ± 1.12 cm, respectively, were significantly (P<0.05) higher than those reported by [12] 1.96 mGy and 2.23 mGy , [3] 1.2 ± 0.5 and 1.5 ± 0.7 mGy, [5] 1.2 ± 0.6 mGy and 1.63 ± 0.9, and [9] 1.77 mSv and 1.88 mSv, [13] 2.0 mGy and 2.5 mGy [14] 1.54 mGy and 1.82 mGy for CC and MLO views, respectively. From these values it is obvious that the MGD is always lower in the CC than in MLO projection. The inclusion of pectoral muscle in the MLO projection (whose proper imaging is essential for the diagnosis) is denser than the rest of the breast and causes an increase to the mAs and consequently to the MGD. This increase, however, is variable, depending on what part of the AEC chamber this muscle is covering. The result of our study is in disagreement with others [3,5,9,12-14]. This is caused by improper usage of exposure factors such as mAs and kVp for different thickness as seen in the four mammography units (SI, BZ, BL and BH). |
| The operation of a mammography unit requires an explicit choice of the X-ray tube potential used to generate the image. LaVoy et al. [11] shows increasing the kVp from 25 to 26 kVp reduces the mAs and exposure times by about 25%, and reduces the MGD by about 10%. However, as shown in Table 2 and Table 3, during manual selection of parameters, in SI unit, it is observed that the same mAs and kVp were selected for CC and MLO projection having a mAs of 31.12 ± 1.66, 31.12 ± 1.66 and kVp of 29.62 ± 1.76, 29.74 ± 1.84 respectively. As a result MGD of 1.43 ± 0.32 mGy and 1.36 ± 0.32 mGy were observed for CC (3.58 ± 0.93 cm) and MLO (3.88 ± 1.05 cm) projection respectively. Similarly in BZ reduced mAs and kVp were selected for larger breast and vice versa having a mAs of 76.35 ± 20.13 and 75.94 ± 19.96, a kVp of 26.08 ± 0.63 and 26.07 ± 0.59 and MGD of 1.52 ± 0.47 mGY and 1.40 ± 0.42 mGY were observed for CC(4.18 ± 0.86 cm) and MLO (4.71 ± 0.85 cm) projection respectively. Surprisingly higher mAs, kVp and MGD were observed in BL unit with a mAs of 186.49 ± 12.97 and 186.39 ± 13.03 a kVp of 29.43 ± 1.08 and 29.44 ± 1.1 and MGD of 6.73 ± 0.24 mGy and 6.45 ± 0.67 mGy for CC (4.77 ± 0.92 cm) and MLO (5.1 ± 1.19 cm) projection respectively. |
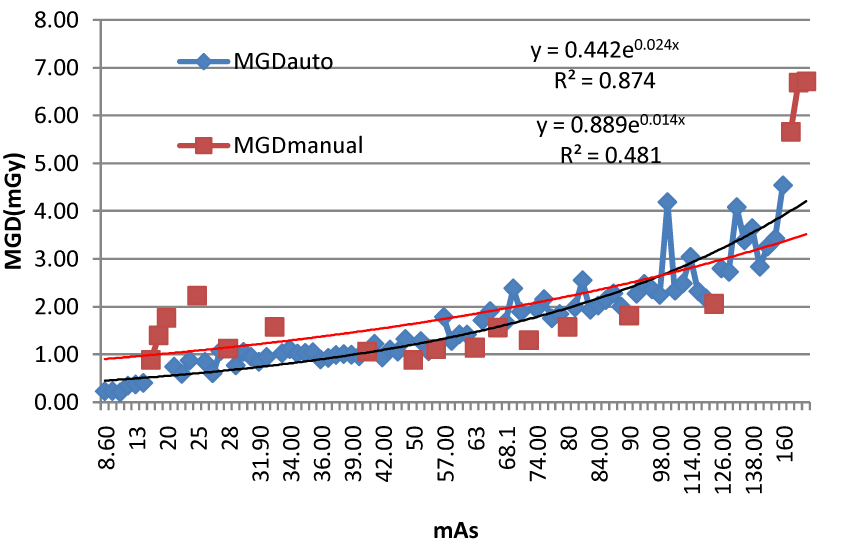
| In contrast to the four mammography units (SI, BH, BL and BZ), KA is using AEC. In this hospital a mAs of 53.74 ± 27.31 and 75.24 ± 35.79, kVp of 26.33 ± 0.57 and 26.74 ± 0.62, and MGD of 1.39 ± 0.63mGY and 1.92 ± 0.88 mGy were observed for CC (3.81 ± 0.98 cm) and MLO (4.59 ± 1.05 cm) projection. This is in agreement with all studies using AEC where the MGD for MLO is higher than CC projection. In both manual and AEC beam selection mAs and MGD were excellently correlated with values of R2=0.4817 and R2=0.8741 respectively (Figure 4). |
| The average MGD found in this study (2.57 ± 2.12 mGy) was higher with the corresponding values found in the recent literature: 1.4 ± 0.6 mGy [3], 1.42 ± 0.8 mGy [5], but the average MGD in this study were below the limit of 3 mGy established for the reference medium-sized breast of 4.2 cm CBT. All mammography units except BL mammography unit participating in this study fulfilled the Quality Criteria Guidelines set by the European Commission in terms of the MGD limiting value of 2 mGy given by the IPEM protocol [15] and the European protocol [16] for standard CBT of 4.5 cm. However, the variety of techniques that was observed during this study, namely the different approaches concerning the setting of the tube potential and mAs revealed the great need for the establishment of a national protocol concerning diagnostic breast examination in Ethiopia. |
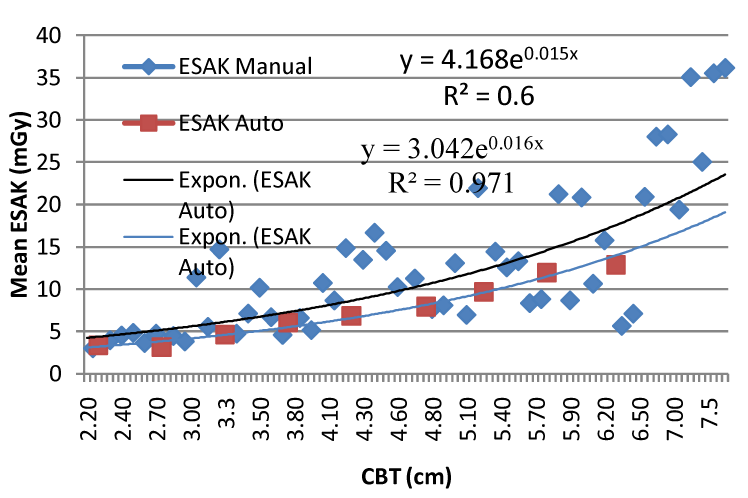
| As shown in Table 4, in bivariate analysis kVp, mAs, CBT and HVL were statistically associated with ESAK and MGD for all automatic, manual and combined manual and automatic projections. However no statistical association was found between age and ESAK and MGD for both manual, automatic projections and for both combined together. This is consistent with the previous finding [1,5,13]. In this survey the correlation between ESAK and CBT found for manual beam selection method (60%) was significantly (P<0.05) less than automatic beam selection method (97.1%) (Figure 3). The difference can partly be explained by the fact that for the same breast thickness there is variation of exposure factors application in manual beam selection method. This substantial variation in the ESAK values for the same CBT in different units can be connected to the fact that no systematic periodical quality controls measurements are carried out in all mammography units in Ethiopia. |
| Numerous studies showed that use of a rhodium (Rh) or tungsten (W) anode tube with an Rh filter in thick or dense breasts provides higher image quality, while resulting in significantly lower dose than a Mo anode tube used with a Mo filter [1-5]. However although four of the units have an alternative target material such as tungsten or rhodium, these are still not used in Ethiopia. |
| A major determinant of image quality and average breast doses was the type of film–screen combination used. In Ethiopia, because of lack of mammography films, it is very difficult to choose the fastest or slowest film-screen combination. The screen Kodak MIN-R 2190, HD, AD mamo fine, Kodak Min-R, AD mamo fine were combined with any type of green sensitive mammography films available in KA, BL, BZ, BH and SI respectively. Because of the potential variation in speed and contrast characteristics it is not recommended to mix screens and films [20]. The results indicate urgent need to introduce annual quality control checks to test image quality and routinely audit the radiation dose to women undergoing diagnostic mammography in all mammography units in Ethiopia. |
| There are many mean glandular dose affecting factors, and their complex interrelations are difficult to control in clinical settings. Well tailoring of kVp/anode/filter combination, selection of faster screens and well matched films are mandatory, in reducing mean glandular dose. However, tailoring of kVp/anode/filter, which should be based on both breast thickness and composition, is difficult to achieve accurately at all times using manual selection. Therefore, automatic beam quality control should replace the manual mode in screen-film mammography practice in order to provide easier and more effective control on mean glandular dose. |
| Acknowledgements |
| We gratefully acknowledge the financial support of Addis Ababa University and Ethiopian Embassy in India, all hospitals that participated in this study and their staff for their cooperation. The authors also express their gratitude to all radiographers who participated in data collection. |
References |
|
Tables and Figures at a glance
| Table 1 | Table 2 | Table 3 | Table 4 |
Figures at a glance
 |
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 | Figure 4 |
Post your comment
Relevant Topics
- Abdominal Radiology
- AI in Radiology
- Breast Imaging
- Cardiovascular Radiology
- Chest Radiology
- Clinical Radiology
- CT Imaging
- Diagnostic Radiology
- Emergency Radiology
- Fluoroscopy Radiology
- General Radiology
- Genitourinary Radiology
- Interventional Radiology Techniques
- Mammography
- Minimal Invasive surgery
- Musculoskeletal Radiology
- Neuroradiology
- Neuroradiology Advances
- Oral and Maxillofacial Radiology
- Radiography
- Radiology Imaging
- Surgical Radiology
- Tele Radiology
- Therapeutic Radiology
Recommended Journals
Article Tools
Article Usage
- Total views: 9139
- [From(publication date):
October-2012 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 4112
- PDF downloads : 5027
