Case Report Open Access
Extensive Involvement of the Dorsal Spine by Tuberculous Infection and Surgical Treatment with Percutaneous Spinal Instrumentation
| Joaquim Soares Do Brito1*, António Tirado2 and Pedro Fernandes3 | ||
| 1Orthopaedic and trauma resident – Hospital de Santa Maria, Portugal | ||
| 2Orthopaedic and trauma specialist – Hospital de Santa Maria, Portugal | ||
| 3Head of Spine Surgery Unit – Orthopaedic and trauma department – Hospital de Santa Maria, Portugal | ||
| Corresponding Author : | Joaquim Soares do Brito Orthopaedics and Trauma Resident – Orthopaedic and Trauma department – Hospital de Santa Maria Avenida Professor Egas Moniz, 1649-035, Lisbon, Portugal Tel: 351 21 780 5000 E-mail: joaquimsoaresdobrito@gmail.com |
|
| Received June 02, 2014; Accepted June 14, 2014; Published July 20, 2014 | ||
| Citation: Brito JSD, Tirado A, Fernandes P (2014) Extensive Involvement of the Dorsal Spine by Tuberculous Infection and Surgical Treatment with Percutaneous Spinal Instrumentation. J Infect Dis Ther 2:156. doi: 10.4172/2332-0877.1000156 | ||
| Copyright: © 2014 Brito JSD, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.. | ||
Related article at Pubmed Pubmed  Scholar Google Scholar Google |
||
Visit for more related articles at Journal of Infectious Diseases & Therapy
Abstract
Purpose: Tuberculosis can be responsible for extensive spinal lesions. Despite the efficacy of medical treatment surgery is indicated to avoid or correct significant deformity, instability and neurological involvement. The authors present a clinical case of total dorsal spine involvement with posterior and anterior major abscess, discussing the management options and outcome obtained.
Clinical case: 24 years old male patient, admitted with severe dorsal pain and fluctuating posterior left hemithorax mass with no neurological impairment. CT-Scan and MRI showed extensive lytic lesions from T2 to T12 with gross instability in T8-T9.
The patient was surgically treated after 15 days of antibiotic therapy, having a continuous drainage from the left posterior hemithorax superinfected with Staphylococcus aureus. A posterior percutaneous unilateral T5-T12 pedicular instrumentation plus anterior debridement and T7-T10 arthrodesis with vascularized rib graft was performed. Left pedicular instrumentation was postponed to the third week to allow healing of the superinfected area over the left hemithorax where skin was all detached from rib cage. At 24 months follow up, the patient regained complete and normal functional activity with no recurrence of infection, showing a solid fusion over the thoracic area with no deformity.
Discussion: Extensive involvement and pyogenic abscess superinfection makes this case a significant therapeutic challenge. In our opinion, anterior-posterior surgery and staged posterior percutaneous instrumentation were favourable related with the excellent outcome.
| Keywords | |
| Spinal tuberculosis; Surgical treatment; Percutaneous instrumentation; staged surgery | |
| Presentation of Clinical Case | |
| A 24-year-old male, original from Guiney was admitted on November 2011 in our institution with history of severe and progressive disabling dorsal pain, low fever, chills, night sweating, adynamia, anorexia and a 20% height loss since April 2011. No history of trauma was disclosed and the patient was taking acetaminophen and nonsteroid anti-inflammatory drugs without pain or other symptoms relief. In July 2011 a fluctuant mass affecting all posterior left hemithorax was clinically detected, with progressive increase in dimension over time. The initial pain worsened and inability to walk developed in this context. In October 2011 spontaneous drainage started from the left hemithorax mass and in November 2011 the patient arrived to our institution. | |
| During the first evaluation at our institution provided by internal medicine and infectious diseases doctors, clinical history revealed no previous diseases, particularly HIV infection or other immunosuppressive conditions. The patient was in bed due to severe dorsal pain, extremely emaciated and not tolerating any orthostatic position. A bulky mass consistent with an abscess was observed in the left posterior hemithorax and spontaneous purulent drainage was also documented. Palpation and percussion was painful along all dorsal spine processes. No neurological deficit was documented. | |
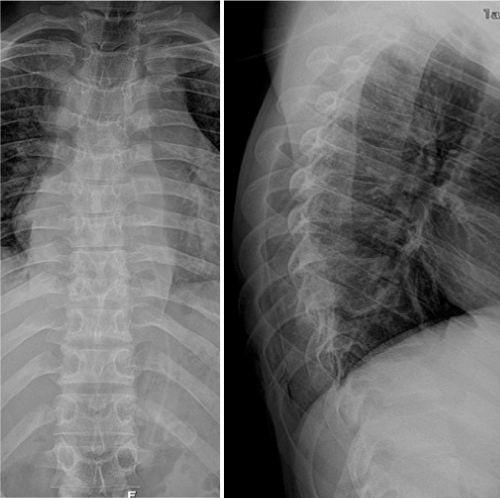
| Blood analysis revealed microcytic hypochromic anaemia, elevated ESR (erythrocyte sedimentation rate) and small increase in RCP (reactive C-Protein). HIV 1 and 2, HCV, HBV and syphilis serologies were all negative. Blood cultures, urine culture, purulent abscess drainage cultures were obtained. The patient was admitted in the infecciology department for clinical study. After orthopaedic consultation, spinal plain radiographs (Figure 1) and CT scans were also required. At the same time the dorsal abscess was surgically evacuated and a drain introduced. | |
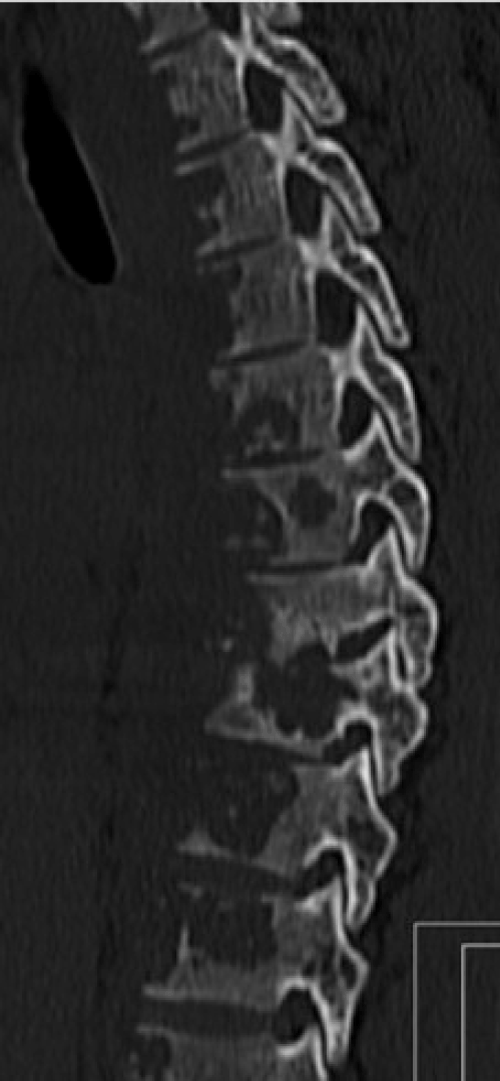
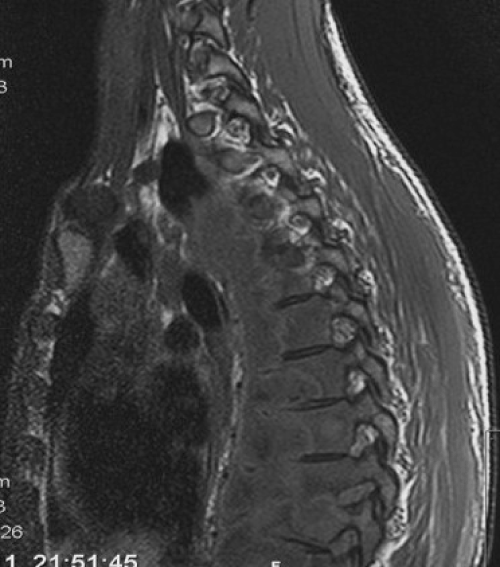
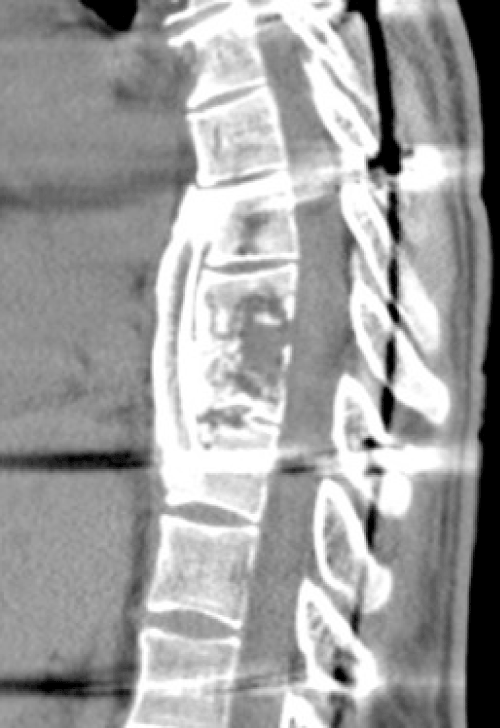
| The CT-scan showed extensive lytic lesions from T2 to T12 with gross instability in T8-T9 (Figure 2). Additional MRI confirmed the CT scan findings and also revealed an extensive paravertebral abscess, which had communication to the left posterior hemithorax abscess (Figure 3). Under suspicion of spinal tuberculosis the infectious disease department decided to initiate anti-tuberculosis chemotherapy. After proper investigation no other focus for tuberculous infection was disclosed. | |
| The culture of the pus obtained from the posterior thoracic abscess identified a Staphylococcus aureus susceptible to flucloxaciline, which was implemented. No other bacteria were identified in the first studies. | |
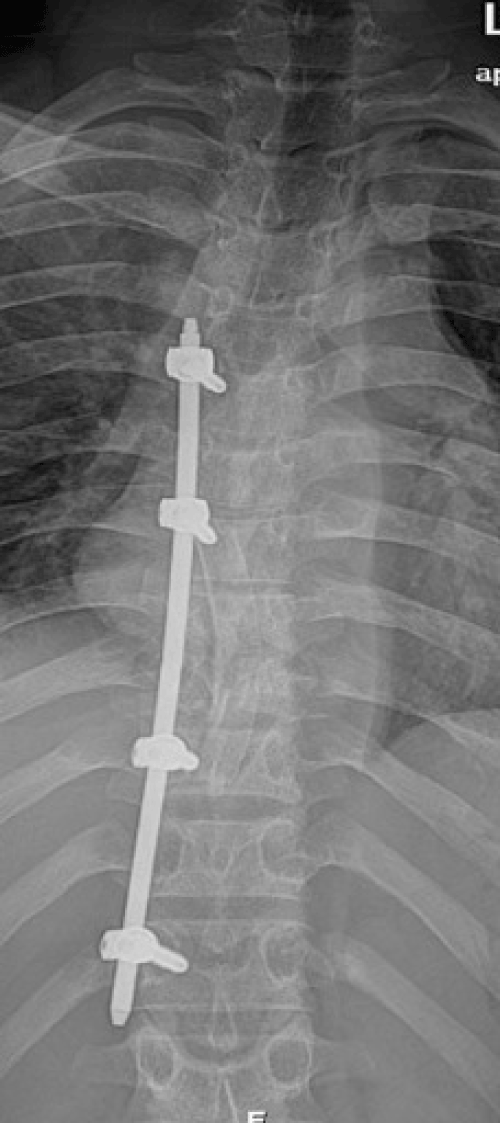
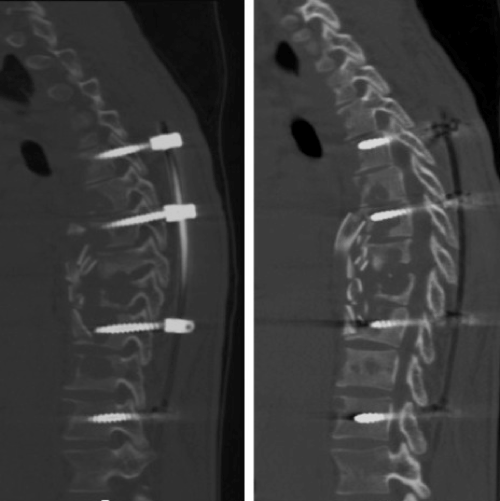
| Because of the uncontrolled disabling dorsal pain, spine instability and extensive paravertebral abscess, we decided to operate the patient after 15 days of anti-tuberculosis chemotherapy. In this occasion the patient maintained continuous drainage from left posterior hemithorax superinfected with Staphylococcus aureus. A posterior percutaneous unilateral T5-T12 pedicular instrumentation plus anterior debridement and T7-T10 arthrodesis with vascularized rib graft was performed (Figures 4-6). Left pedicular instrumentation was postponed to the third week to allow healing of the superinfected area over the left hemithorax where the skin was all detached from the rib cage. Intraoperatively were obtained pus samples for bacteriological studies, where we were able to identify Mycobacterium tuberculosis complex bacteria. The chemotherapy drugs susceptibility tests did not revealed resistant mycobacteria. Both anti-tuberculosis chemotherapy and flucloxaciline were maintained during all admission period. Anti-tuberculosis chemotherapy consisted in isoniazid, pyrazinamide, rifampicin and ethambutol for two months and isoniazid plus rifampicin for ten additional months. | |
| After surgery, the patient had immediate pain relieve starting rehabilitation two weeks after second surgery. The flucloxaciline therapy was interrupted after six weeks. | |
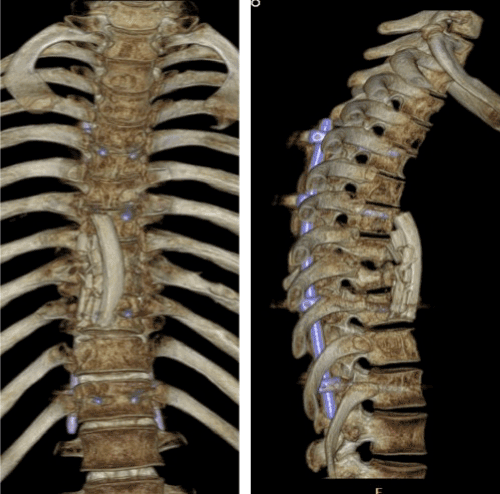
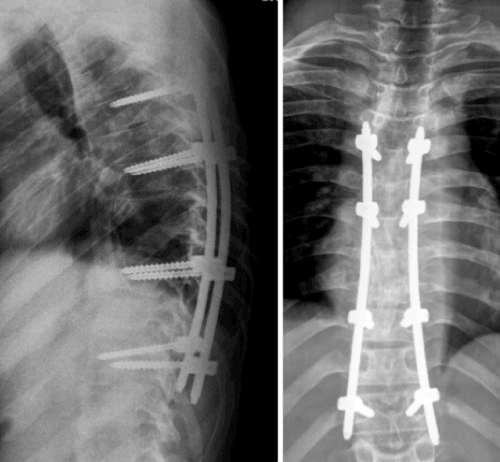
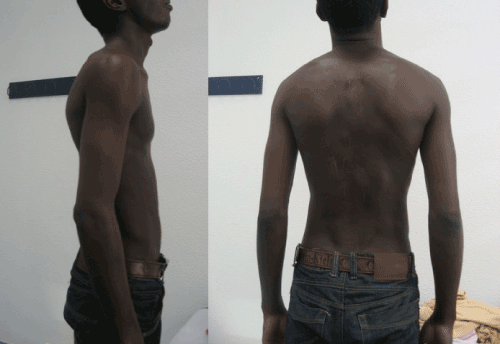
| At 24 months follow-up the patient regained complete and normal functional activity with no recurrence of infection, showing a solid fusion over the thoracic area with no significant deformity (Figures 7-9). | |
| Discussion | |
| Tuberculosis is an infection with worldwide impact and mortality rate accounting for two million deaths each year [1,2]. Additionally there are an estimated nine million new cases each year. Simultaneously, we are witnessing the emergence of antibiotic resistance to many drugs used as first-line drugs creating growing concern in western societies, turning tuberculosis into a global challenge [1,2]. | |
| Spinal tuberculosis, in the other hand, accounts for over 40% of all spine infections [1]. This clinical entity is socio-economic related, occurring more often in developing countries, although with a documented increased incidence in occidental countries [2]. About 10% of all tuberculosis cases present musculoskeletal involvement and 50% of the latest corresponds to cases of spinal tuberculosis [3]. The thoracic and lumbar spine is most commonly involved (90% of cases) and is relatively infrequent in the cervical spine (10% of cases) [3,4]. | |
| In the initial phase of the disease the diagnosis can be challenging. The cardinal symptoms in spinal tuberculosis are pain, mild fever, chills, kyphotic deformity, paravertebral abscess or even progressive neurological impairment. Clinical, laboratory and imaging studies are fundamental, and the definitive diagnosis is obtained with the isolation of Mycobacterium tuberculosis [2]. | |
| Antituberculosis chemotherapy is still the gold standard treatment for this condition, allowing spontaneous fusion in about 80% of cases [1,2]. There is great controversy in the international literature regarding the optimal duration of chemotherapy with these drugs. Suggested treatment programs can range from six to 18 months [3-7]. More recent literature supports shorter treatment programs, initially with four drugs (isoniazid, rifampicin, pyrazinamide and ethambutol) for two months, followed by isoniazid and rifampicin for additional four months [1]. This program had satisfactory results, although the treatment program for nine to twelve months continues to be the gold standard in specialized centres and followed in our institution [1,2,4]. | |
| The surgical procedure takes a preponderant role if there is vertebral instability, failure in medical treatment, progressive deformity, presence of paravertebral abscess or neurological injury, with or without the presence of epidural abscess [1]. It proved over time to be an extremely effective method for treating spinal tuberculosis [1,2,8]. This technique has high infection resolution rates, ability to eradicate paravertebral abscess and achieve vertebral fusion in 97% of cases [2]. Additionally, surgery has the advantage to control spinal deformity and limits or improves the neurological injury resulting from this disease [9,10]. | |
| The presented clinical case constitutes an unusual case of severe spinal tuberculosis condition. There was an extensive spinal involvement with paravertebral abscess and a left thoracic posterior wall abscess superinfected which complicated the treatment, making this case a significant therapeutic challenge. Surgery was decided based on severe instability and expected deformity as more than two vertebral bodies were involved [11]. Due to extensive disease and clinical conditions of the patient, percutaneous instrumentation seemed to be a good option to achieve stability. However, two problems had to be addressed: one was related to the absence of anterior wall in every vertebral bodies to be instrumented, increasing the risk of great vessel injury during the procedure; and the other being the need to postpone left side instrumentation. This was undertaken due to extensive soft tissue degloving over the left posterior hemithorax and superinfection with Staphylococcus aureus. We can also discuss the need to go anteriorly as the abscess could have been drain percutaneously. Our experience is a faster recovery and fusion by doing anterior debridement and grafting the spine through an anterior surgical approach. | |
| In our opinion, the two times staged surgical option associated with percutaneously instrumentation was truly beneficial to the excellent outcome we had without any complication reported despite the extensive dorsal spinal tuberculosis involvement seen in this patient. | |
References
- Guerado E, Cerván AM (2012) Surgical treatment of spondylodiscitis. An update. Int Orthop 36: 413-420.
- Luk KD (1999) Tuberculosis of the spine in the new millennium. Eur Spine J 8: 338-345.
- McLain RF, Isada C (2004) Spinal tuberculosis deserves a place on the radar screen. Cleve Clin J Med 71: 537-539, 543-9.
- Ferrer MF, Torres LG, Ramirez OA, Zarzuelo MR, Gonzalez NP; Tuberculosis of the spine. A systematic review of case series; International Orthopaedics (SICOT); Springer; 2011
- MRC Working party on tuberculosis of spine; A 10 year assessment of a controlled trials of in-patient and out-patient treatment of plaster-of Paris jackets for tuberculosis of the spine in children on standard chemotherapy; Journal of Bone and Joint Surgery B 1985; 67:103-110
- Tuli SM (1975) Results of treatment of spinal tuberculosis by "middle-path" regime. J Bone Joint Surg Br 57: 13-23.
- [No authors listed] (1993) Controlled trial of short-course regimens of chemotherapy in the ambulatory treatment of spinal tuberculosis. Results at three years of a study in Korea. Twelfth report of the Medical Research Council Working Party on Tuberculosis of the Spine. J Bone Joint Surg Br 75: 240-248.
- [No authors listed] (1982) A 10-year assessment of a controlled trial comparing debridement and anterior spinal fusion in the management of tuberculosis of the spine in patients on standard chemotherapy in Hong Kong. Eighth Report of the Medical Research Council Working Party on Tuberculosis of the Spine. J Bone Joint Surg Br 64: 393-398.
- Wang X, Li J, Lu G, Wang B, Lu C, Kang Y; Single-stage posterior instrumentation and anterior debridement for active tuberculosis of the thoracic and lumbar spine with kyphotic deformity; International Orthopaedics (SICOT); Springer; 2011
- Ma YZ, Cui X, li HW, Chen X, Cai XJ, Bai YB; Outcomes of anterior and posterior instrumentation under different surgical procedures for treating thoracic and lumbar spinal tuberculosis in adults; International Orthopaedics (SICOT); Springer; 2011
- Rajasekaran S, Shanmugasundaram TK (1987) Prediction of the angle of gibbus deformity in tuberculosis of the spine. J Bone Joint Surg Am 69: 503-509.
Figures at a glance
 |
 |
 |
 |
 |
||||
| Figure 1 | Figure 2 | Figure 3 | Figure 4 | Figure 5 |
 |
 |
 |
 |
|||
| Figure 6 | Figure 7 | Figure 8 | Figure 9 |
Relevant Topics
- Advanced Therapies
- Chicken Pox
- Ciprofloxacin
- Colon Infection
- Conjunctivitis
- Herpes Virus
- HIV and AIDS Research
- Human Papilloma Virus
- Infection
- Infection in Blood
- Infections Prevention
- Infectious Diseases in Children
- Influenza
- Liver Diseases
- Respiratory Tract Infections
- T Cell Lymphomatic Virus
- Treatment for Infectious Diseases
- Viral Encephalitis
- Yeast Infection
Recommended Journals
Article Tools
Article Usage
- Total views: 13681
- [From(publication date):
October-2014 - Aug 20, 2025] - Breakdown by view type
- HTML page views : 9079
- PDF downloads : 4602
