Research Article Open Access
Fetal Magnetic Resonance Imaging for the Prenatal Assessment of the Extended Cardiovascular System by CASSEAL (Cardiovascular System Sonographic Evaluation Algorithm)
| Coral Bravo1,2, Yolanda Ruiz3, Luis Ortiz1, Teresa Álvarez4, Francisco Gámez1, Carlos Marín3, Ricardo Pérez1, Ángel Lancharro3 and Juan De León-Luis1* | |
| 1Department of Obstetrics and Gynecology. Hospital General Gregorio Marañón, Universidad Complutense de Madrid, Madrid, Spain | |
| 2Department of Obstetrics and Gynecology. Hospital Central de la Defensa Gómez Ulla. Universidad de Alcalá de Henares. Madrid, Spain | |
| 3Department of Radiology. Hospital General Gregorio Marañón, Universidad Complutense de Madrid, Madrid, Spain | |
| 4Department of Paediatric Cardiology. Hospital General Gregorio Marañón, Universidad Complutense de Madrid, Madrid, Spain | |
| Corresponding Author : | Juan De León-Luis Fetal Medicine Unit, Department of Obstetrics and Gynecology Hospital General Gregorio Marañón Universidad Complutense de Madrid O’Donnell, 48. 28009 Madrid, Spain Tel: + 34 (91) 5290218 E-mail: jdeleonluis@yahoo.es |
| Received: September 21, 2015 Accepted: November 09, 2015 Published: November 12, 2015 | |
| Citation:Bravo C, Ruiz Y, Ortiz L, Álvarez T, Gámez F, et al. (2015) Fetal Magnetic Resonance Imaging for the Prenatal Assessment of the Extended Cardiovascular System by CASSEAL (Cardiovascular System Sonographic Evaluation Algorithm) . OMICS J Radiol 4:209. doi:10.4172/2167-7964.1000209 | |
| Copyright: © 2015 Bravo C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Radiology
Abstract
Purpose: To compare axial view images obtained with fetal ultrasound (US) and magnetic resonance imaging (MRI) when applying the Cardiovascular System Sonographic Evaluation Algorithm (CASSEAL).
Materials and method: CASSEAL is an US algorithm consisting on the acquisition of 9 different axial views of the fetal abdomen and chest, from the umbilical vein to the subclavian arteries. It was designed for a thorough US assessment of the extended fetal cardiovascular system. Feasibility and reproducibility of CASSEAL have already been proven; however, its application in fetal MRI has yet to be established. A fetal MRI was performed to a 25 week-old fetus with ventriculomegaly (11 mm) in order to obtain the 9 axial views required by CASSEAL. Subsequently, a comparison between both imaging techniques was performed for each view.
Results: The comparison of the images obtained with these two imaging techniques showed a good correlation in the identification of cardiovascular anatomical structures.
Conclusion: CASSEAL US axial views can be obtained in fetal MRI and correlation between the 2 techniques is good. This finding suggests that MRI may be a useful complement to US in the assessment of fetal cardiovascular anomalies using the same views by which sonographers assess fetal cardiovascular structures.
| Keywords |
| Congenital heart disease; Fetal cardiovascular anomalies; Fetal magnetic resonance imaging; Prenatal ultrasound |
| Abbreviations |
| 3VT: Three Vessels View; CHD: Congenital Heart Disease; DA: Ductus Arteriosus; DV: Ductus Venosus; HP: Hepatic Veins; IVC: Inferior Vena Cava; fMRI: Fetal Magnetic Resonance Imaging; SVC: Superior Vena Cava; US: Ultrasound |
| Introduction |
| Fetal ultrasound (US) is the standard technique for the prenatal diagnosis of cardiovascular anomalies; however, in the last 20 years, magnetic resonance imaging (MRI) has become a complementary technique, during both prenatal and postnatal period [1-3]. In the prenatal period, MRI is used for the study of central nervous system, diaphragmatic hernia, lung diseases and placental anomalies [1]. In the postnatal period, when lung tissue interferes with US assessment of the heart and great vessels, MRI can better characterize these anomalies. Unfortunately, fetal MRI for the evaluation of congenital heart disease (CHD) is still limited [2]. |
| CHD is the most common major anomaly in the newborn, with an estimated incidence of 1/200 live births [4]. To increase its detection rate, several systematic protocols have been described, mainly based on the US acquisition of axial views of the heart [5] . Although CHD is the most common defect of the fetal cardiovascular system, other adjacent areas are also affected, albeit to a lesser extent. These areas, which include the portal system, the thymus, the supra-aortic vessels, and the heart itself, develop concomitantly during the embryonic period, as a unit, the extended fetal cardiovascular system. A new US algorithm (CASSEAL, Cardiovascular System Sonographic Evaluation Algorithm) combines the current recommendations for the screening of CHD with exploration of these areas adjacent to the heart in both a cranial and caudal direction [6]. The protocolized acquisition of systematic and reproducible views that are comparable in US and MRI can be useful in the prenatal and postnatal diagnosis of cardiovascular anomalies. The aim of this work is to determine whether the images of the extended fetal cardiovascular system obtained with the two imaging techniques are comparable and to discuss their benefits in terms of diagnostic accuracy. |
| Materials and Methods |
| A 28-year-old primigravida at 23 weeks of gestation was referred to our institution for further evaluation after a prenatal diagnosis of bilateral mild ventriculomegaly. The neurological findings were confirmed by US, so a fetal MRI was scheduled for the 25th week. The fetal cardiovascular system was assessed following the CASSEAL protocol which is our standard technique for cardiovascular anomaly screening in the second trimester of pregnancy (transabdominal 4–8 MHz transducer, Voluson E6, GE Medical Systems, Zipf, Austria). |
| CASSEAL consists of the sequential acquisition of 9 axial views of the main components of the extended fetal cardiovascular system [6], from caudal to cranial as follows: I, portal sinus; II, ductus venosus (DV); III, hepatic veins (HV); IV, four cardiac-chambers; V, left ventricle outflow tract; VI, right ventricle outflow tract; VII, three vessels and trachea (3VT); VIII, thy-box; and IX, subclavian arteries (Figures 1-3). All 9 views are obtained in B-mode, although color Doppler may be used when visualization is limited. No cardiovascular abnormality in the fetus was found with the CASSEAL assessment. |
| Subsequently, a fetal MRI was performed in order to confirm the ventriculomegaly and to detect any additional brain anomalies. A radiologist experienced in prenatal MRI was asked to reproduce the axial views included in CASSEAL to determine if it was achievable and to what extent both techniques were similar. The procedure was performed using an Intera 1.5 T scanner (Philips Medical Systems, Best, and The Netherlands) with a cardiac phased array coil. In addition to our standard MRI protocol for the fetal brain study, T2- weighted MR images of the fetal thorax and upper abdomen were acquired in a transverse plane using a Balanced Fast Field Echo (b- FFE) sequence in order to provide bright blood images to better visualized fetal heart and vessels. We obtained 25 sections of 4 mm thickness without gap, covering the region of interest with a total acquisition time of 37 seconds. MR settings were: repetition time 3.5 msec; effective echo time 1.74 msec; turbo factor 256; 1 signal acquired; matrix 192 × 256; specific absorption rate below 2.0 W per kg of body weight. |
| Results |
| After completion of both, the US and the MRI assessment, a set of 9 axial images was obtained for each imaging modality. This whole set was divided into 3 sections to better identify the anatomical structures involved in each axial view. |
| Infracardiac territory: CASSEAL views I to III |
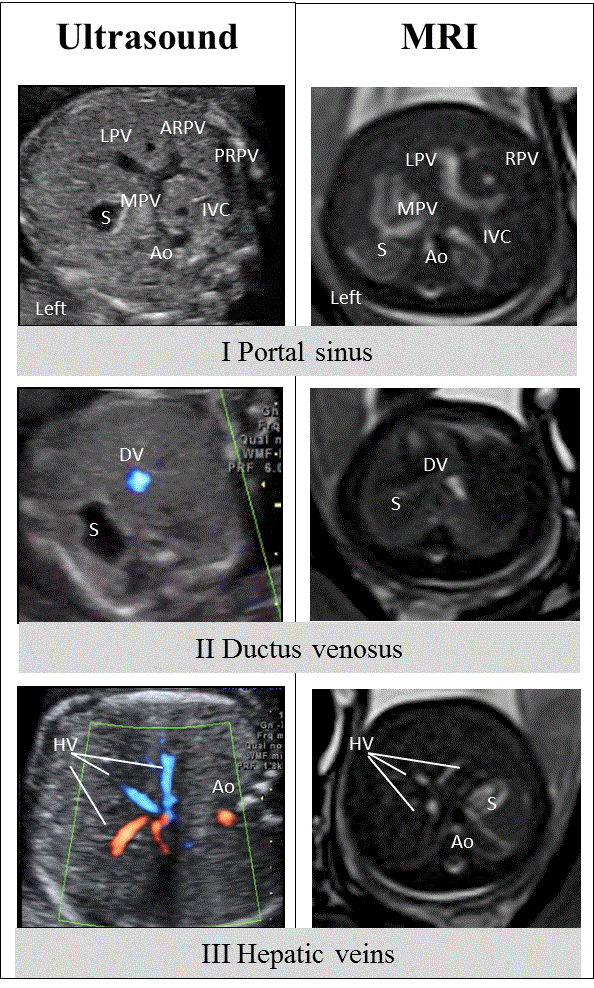
| View I is a transverse plane of the upper fetal abdomen at the level of the entrance of the umbilical vein. Visible frames of reference are the following: the spine in the back; the descending aorta to the left; the inferior vena cava (IVC) anterior and to the right; the stomach in the left abdomen; and the portal sinus on the right side of the abdomen. It may be possible to identify the left portal vein with all or some of its branches (superior, inferior, and medial), its confluence with the right portal vein and its branches (anterior and posterior), and the anastomosis of both vessels with the main portal vein (Figure 1) [7]. |
| View II is an axial view slightly cranial to view I that shows the DV. The DV is a thin vessel originating in the left portal vein and connecting this vessel with the IVC in a cranial, lateromedial, and anteroposterior direction. On its left, the stomach, the spine in the back, and cross sections of the descending aorta and the IVC can be identified (Figure 1) [7]. |
| View III is an axial plane of the fetal upper abdomen, at a slight oblique angle (less than 15º) above the DV. It allows the identification of the right, middle and left HV, which converge with the DV in the subdiaphragmatic portion of the IVC. The spine and the aorta can be visualized at the back of the abdomen; and the stomach is on the left (Figure 1) [7]. |
| For any of the views I to III, the images obtained by US and MRI are extremely similar and well correlated. All the features identified by US can also be visualized with MRI. |
| Heart area: CASSEAL views IV to VII |
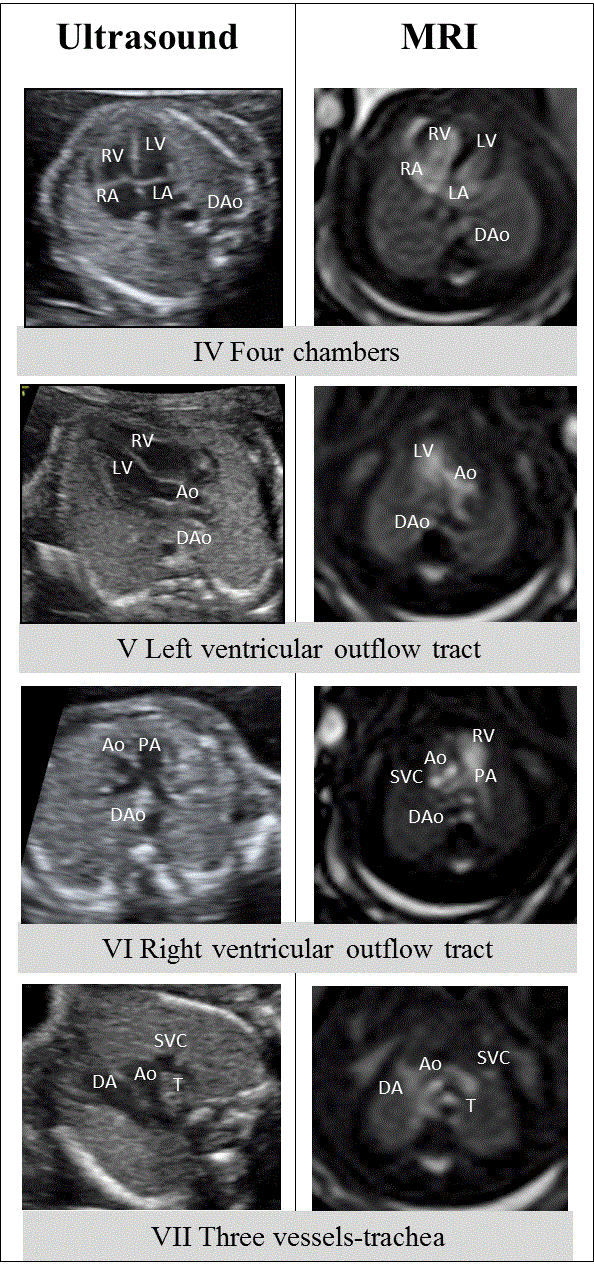
| View IV consists of the four-chamber view of the fetal heart. It is obtained from a transverse view of the fetal thorax, simultaneously showing the four main cavities, the spine in a posterior position, and at least 1 complete rib (Figure 2). A cross section of the descending aorta can be observed behind the left atrium. |
| View V shows the left ventricular outflow tract. It is viewed by angling the plane slightly from the position of the four-chamber view towards the fetal head and right shoulder (between 5°-15°), or by rotating the plane to visualize the left ventricular outflow tract and the aorta (Figure 2) [8]. |
| View VI shows the outflow tract of the right ventricle and the origin of the main pulmonary artery in a transverse view slightly cranial to view V. The methodology is similar to that used above, depending on the position of the interventricular septum. At this level, it is possible to observe the origin of the pulmonary trunk and its bifurcation into the right and left pulmonary arteries, as well as a cross section of the ascending and descending aorta and superior vena cava (SVC) (Figure 2) [8]. |
| View VII is a view of the 3VT. It is obtained by moving upwards from the previous view and in a slightly oblique plane with respect to the four-chamber cardiac view. The pulmonary artery connecting with the ductus arteriosus (DA) is identified, and to its right, a transverse section of the aortic arch, the SVC and the trachea are shown (Figure 2). The aorta and the DA are arranged in a V shape, which opens towards the anterior chest wall and has its vertex to the left of the trachea. To the right of the trachea, the azygos vein can be observed in its posteroanterior course to the SVC [9]. |
| As in the infracardiac territory, US and MRI images correlate fully and the heart and the great vessels are easily identifiable when images from the same views are compared. |
| Supracardiac territory: CASSEAL views VIII and IX |
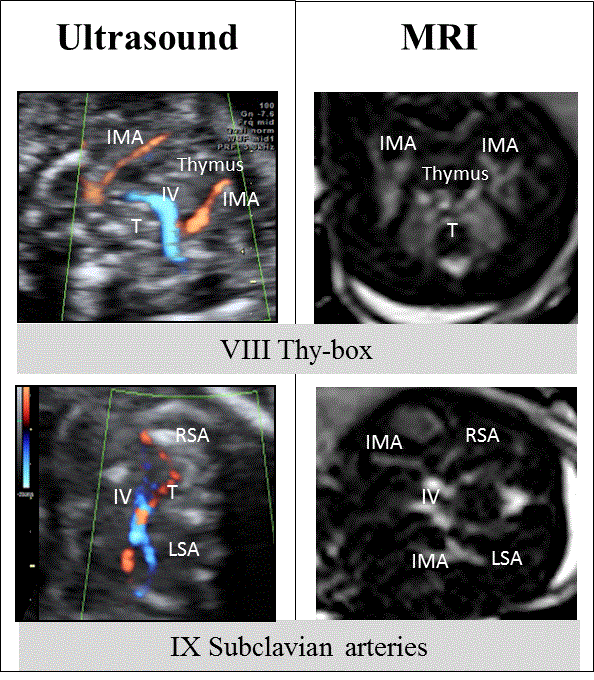
| View VIII includes the visualization of the fetal thymus in the thybox in a transverse section of the fetal thorax, slightly cranial to the 3VT view [10]. At this level, we can identify the thymus, located in the middle of the chest and limited anteriorly by the sternum, posteriorly by the origin of the great vessels, and laterally (on both sides) by the internal mammary arteries (Figure 3). View IX shows both subclavian arteries in a transverse section slightly cranial to view VIII with its typical S-shaped course anterior to the trachea towards the fetal arm (Figure 3). Again both imaging modalities provide similar images for these two upper views. Again both imaging modalities provide similar images for these two upper views. |
| Discussion |
| We report a case of prenatal ventriculomegaly evaluated by US and MRI to determine the feasibility and reproducibility of applying a US algorithm for assessing the fetal cardiovascular system to another modality, that of prenatal MRI. |
| Our main aim in this case was to reproduce CASSEAL protocol views used by sonographers in CHD screening in an evaluation conducted by fetal MRI, and to compare the images acquired with those obtained using echocardiography. As we have described in the previous section, the high degree of similarity of the images obtained with both modalities means that they can be transposed. This correlation may be very useful if MRI is used as a complementary study after detection of a cardiovascular anomaly in the fetus. |
| US is well established as the standard technique in the prenatal assessment of the fetal heart and vessels given its availability and costeffectiveness. In the evaluation of CHD, prenatal US has clear advantages: the fetus can be examined in real time, it is easily accepted by the patient, it is reproducible, and the vessels and their Doppler spectrum can be clearly visualized. However, the limitations of US include problematic visualization resulting from maternal body habitus, oligohydramnios and poor contrast resolution [11]. In contrast, MRI offers better resolution, it is not affected by maternal obesity, amniotic fluid volume or bone calcification, and enables visualization of the whole fetus independently of presentation [2]. Moreover, and to the best of our knowledge, no clinical or experimental evidence has indicated that MRI has any adverse effects on the human fetus [12]. |
| Recent studies have reported the benefits of MRI in the prenatal study of CHD and aortic arch anomalies [13-15]. Authors agree that fetal MRI has the potential to expand on the ability of US in imaging the fetal congenital cardiovascular abnormalities, and it would be indicated mainly in those cases in which US imaging is limited such as oligohydramnios, significant bone ossification or complex extracardiac anomalies with distortion of the fetal anatomy, such as heterotaxy syndromes [13,14,16]. |
| On the technical side, the most efficient technique for characterizing fetal cardiac anatomy appears to be SSFPE (single shot fast spin-echo) sequences used in conjunction with non-gated SSFPE cine sequences [13]. However, the temporal and spatial resolution of the images obtained with the non-gated cine SSFP sequence is usually not very clear [13]. In SSFPE images, blood is characterized by a high signal intensity, thereby improving the blood-to-tissue contrast at the endocardial surface, allowing the cardiac chambers and vessels to be imaged. In non-gated cine MR images, the movements of the atria and the ventricles are reproduced as a video, allowing the cardiac kinetics to be evaluated, especially cardiac valve regurgitation and shunt which are not seen in the static SSFPE images. Currently, cardiac contractility and valvular functionality cannot be reliably evaluated with fetal MRI. With advances in technology such as self-gating, real cardiac gating and metric optimized gating, both temporal and spatial resolution will improve [17]. |
| One of our concerns was whether fetal MRI could achieve the standard echocardiographic views by which sonographers evaluate fetal cardiovascular anatomy. Regarding US, a previous study on the feasibility of CASSEAL showed around 99% or higher feasibility for each view, being the View VIII the one with the lowest frequency of visualization (88.7%) [6]. According to the literature, in fetal MRI, overall feasibility for the four-chamber view is 98% whereas for ventricular outflow tracts it is close to 73%. The main limitation is fetal movements, which reduce feasibility to 50-54% for outflow tracts [16]. In the absence of fetal movements, the left and right outflow tracts are visible in more than 90% of fetuses. In the US application of CASSEAL, the feasibility for both the four chamber view and the ventricular outflow tracts is 99.5% [6]. The sensitivity of MRI in the four-chamber view is 88% (specificity of 96%), while sensitivity for the left and right outflow tract is 63% and 59%, respectively (specificity of 100% and 97%, respectively) [16]. |
| In aortic arch anomalies, transverse views of the aortic arch are recommended, both in echocardiography and MRI. The transverse aortic arch view is a transverse plane in the fetal upper mediastinum that simultaneously demonstrates the course of the aortic arch, in relation to the trachea and the superior vena cava [15]. However, we have demonstrated that the acquisition of a 3VT view is also achievable by MRI. This axial view in a steady-state free precession MRI provides clues to the diagnosis of cardiovascular anomalies by abnormal position, number, size, length, alignment and peripheral superfluous vessels of the aortic arch. Moreover, in the study of the fetal subclavian artery, high correlation has been demonstrated in the MRI assessment of the aberrant right subclavian artery after prenatal diagnosis by US [3] which could be of interest in the study of prenatal vascular rings. This view is feasible in the US application of the algorithm in 99.5% of the cases [6]. |
| Feasibility of the transverse aortic arch view in MRI is 77% and again, correlates positively with the absence of fetal movements. The sensitivity is 58%, with a specificity of 99% [16]. |
| In the fetal upper mediastinum, previous studies have demonstrated feasibility and reproducibility in the acquisition of images of the thymus and the subclavian arteries [3,18]. In the measurement of the fetal thymus transverse diameter and perimeter by both US and MRI, correlation coefficients of 0.91 and 0.88 (95% CI) have been described, respectively [18]. This result may be of interest in cases of thymus hypoplasia, mostly associated with conotruncal anomalies or fetal systemic inflammatory response syndrome [19,20]. In the particular case of thy-box measurements, a group has recently published the only US study describing thy-box diameters according to gestational age [21], so information in the correlation between US and MRI is limited. |
| Despite these promising results, not all technical difficulties have yet been fully resolved, including the effects of fetal blood flow, fetal cardiac motion and fetal body movements. In contrast to conventional US technology, fetal MRI requires large, expensive, less portable equipment, as well as specialized expertise in the conduct and interpretation of the procedure. |
| With this case, we show that US fetal echocardiographic views can be reproduced by fetal MRI and suggest that the acquisition of these images combines the advantages of both techniques and could be of great interest in improving the assessment of fetal cardiovascular anomalies. |
| In conclusion, the reproducibility of CASSEAL US axial views using fetal MRI seems to be high, and correlation between the images obtained by both modalities is good for each of the 9 views. This suggests that MRI may be a useful complement to US for assessment of the fetal cardiovascular system, both in cases of normality or abnormality, using axial views which are the most comprehensive and convenient for sonographers and radiologist. Despite the currently unresolved limitations of fetal cardiovascular MRI, this technique is indicated to complement US cardiovascular assessment in cases in which US is definitely limited. |
| Acknowledgements |
| The authors are grateful to Anne Marie Palma for assistance in English language. |
References
- Laifer-Narin S, Budorick NE, Simpson LL, and Platt LD (2007) Fetal magnetic resonance imaging: a review.CurrOpinObstetGynecol 19: 151-156.
- Manganaro L, Savelli S, Di Maurizio M, Perrone A, Francioso A, et al. (2009) Assessment of congenital heart disease (CHD): is there a role for fetal magnetic resonance imaging (MRI)? Eur J Radiol 72: 172-180.
- Bravo C, Ruiz Y, Ortiz L, Gamez F, and De Leon-Luis J (2013) Neonatal magnetic resonance imaging as a complementary technique after prenatal diagnosis of an aberrant right subclavian artery. J Ultrasound Med 32: 721-724.
- Ferencz C, Rubin JD, McCarter RJ, Brenner JI, Neill CA, et al. (1985) Congenital heart disease: prevalence at livebirth. The Baltimore-Washington Infant Study. Am J Epidemiol 121: 31-36.
- Li Y, Hua Y, Fang J, Wang C, Qiao L, et al. (2013) Performance of different scan protocols of fetal echocardiography in the diagnosis of fetal congenital heart disease: a systematic review and meta-analysis. PLoS One 8: e65484.
- De Leon-Luis J, Bravo C, Gamez F, and Ortiz-Quintana L (2015) Cardiovascular System Sonographic Evaluation Algorithm: A New Sonographic Algorithm for Evaluation of the Fetal Cardiovascular System in the Second Trimester. J Ultrasound Med 34: 1271-1282.
- Yagel S, Kivilevitch Z, Cohen SM, Valsky DV, Messing B, et al. (2010) The fetal venous system, part I: normal embryology, anatomy, hemodynamics, ultrasound evaluation and Doppler investigation. Ultrasound ObstetGynecol 35: 741-750.
- Achiron R, Glaser J, Gelernter I, Hegesh J, Yagel S (1992) Extended fetalecocardiographic examination for detecting cardiac malformations in low risk pregnancies. British Medical Journal 304: 671-674.
- Yagel S, Arbel R, Anteby EY, Raveh D, and Achiron R (2002) The three vessels and trachea view (3VT) in fetal cardiac scanning. Ultrasound ObstetGynecol 20: 340-345.
- Paladini D (2011) How to identify the thymus in the fetus: the thy-box. Ultrasound ObstetGynecol 37: 488-492.
- Levine D (2001) Ultrasound versus magnetic resonance imaging in fetal evaluation. Top MagnReson Imaging 12: 25-38.
- Ruckhaberle E, Nekolla SG, Ganter C, Schneider KT, Peter A, et al. (2008) In vivo intrauterine sound pressure and temperature measurements during magnetic resonance imaging (1.5 T) in pregnant ewes. FetalDiagnTher 24: 203-210.
- Dong SZ, Zhu M, Li F (2013) Preliminary experience with cardiovascular magnetic resonance in evaluation of fetal cardiovascular anomalies. J CardiovascMagnReson 15: 40.
- Manganaro L, Vinci V, Bernardo S, Sollazzo P, Sergi ME, et al. (2014) Magnetic resonance imaging of fetal heart: anatomical and pathological findings. J MaternFetal Neonatal Med 27: 1213-1219.
- Dong SZ, Zhu M (2015) Pattern-based approach to fetal congenital cardiovascular anomalies using the transverse aortic arch view on prenatal cardiac MRI. PediatrRadiol 45: 743-750.
- Votino C, Jani J, Damry N, Dessy H, Kang X, et al. (2012) Magnetic resonance imaging in the normal fetal heart and in congenital heart disease. Ultrasound ObstetGynecol 39 322-329.
- Yamamura J, Frisch M, Ecker H, Graessner J, Hecher K, et al. (2011) Self-gating MR imaging of the fetal heart: comparison with real cardiac triggering. EurRadiol 21: 142-149.
- De Leon-Luis J, Ruiz Y, Gamez F, Pintado P, Oyelese Y, et al. (2011) Comparison of measurements of the transverse diameter and perimeter of the fetal thymus obtained by magnetic resonance and ultrasound imaging. J MagnReson Imaging 33: 1100-1115.
- Chaoui R, Heling KS, Lopez AS, Thiel G, and Karl K (2011) The thymic-thoracic ratio in fetal heart defects: a simple way to identify fetuses at high risk for microdeletion 22q11. Ultrasound ObstetGynecol 37: 397-403.
- Santolya-Forgas J, De León J, Gamez F, Perez R, Antolin E, et al. (2008) 355: Fetalthymic involution can be used as an indicator of intrauterine infection in patients with preterm premature rupture of membranes (pPROM). Am JObstetGynecol 199: S109.
- Munoz-Chapuli M, Gamez F, Bravo C, Ortiz L, Perez R, et al. (2015) The thy-box for sonographic assessment of the fetal thymus: nomogram and review of the literature. J Ultrasound Med 34: 853-858.
Figures at a glance
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 |
Relevant Topics
- Abdominal Radiology
- AI in Radiology
- Breast Imaging
- Cardiovascular Radiology
- Chest Radiology
- Clinical Radiology
- CT Imaging
- Diagnostic Radiology
- Emergency Radiology
- Fluoroscopy Radiology
- General Radiology
- Genitourinary Radiology
- Interventional Radiology Techniques
- Mammography
- Minimal Invasive surgery
- Musculoskeletal Radiology
- Neuroradiology
- Neuroradiology Advances
- Oral and Maxillofacial Radiology
- Radiography
- Radiology Imaging
- Surgical Radiology
- Tele Radiology
- Therapeutic Radiology
Recommended Journals
Article Tools
Article Usage
- Total views: 11687
- [From(publication date):
December-2015 - Aug 17, 2025] - Breakdown by view type
- HTML page views : 10785
- PDF downloads : 902
